The Insulin-Glucose Tolerance Test. a Modified Procedure for the Detection of Hypoglycemia Unresponsiveness in Pituitary and Adrenal Insufficiency
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

WELLNESS SCREENING TEST EXPLANATION SHEET We Encourage You to Share All Lab Results with Your Primary Care Provider
WELLNESS SCREENING TEST EXPLANATION SHEET We encourage you to share all lab results with your primary care provider. EXPLANATION OF BLOOD TESTS HEMOGLOBIN A1C: A Hemoglobin A1c level is HEMATOLOGY WELLNESS: expressed as a percent and is used to evaluate the Blood counts are often used as a broad screening test average amount of glucose in the blood over the last to determine an individual’s general health status. 2 to 3 months. This test may be used to screen for and White blood cells are the cells that are part of the diagnose diabetes or risk of developing diabetes. body’s defense system against infections and cancer and also play a role in allergies and inflammation. ALT: This test is used to determine if a patient has Red blood cells are the cells that transport oxygen liver damage. In healthy individuals, ALT levels in the throughout the body. Hemoglobin measures the blood are low and they rise in various disease states. total amount of the oxygen-carrying protein in the blood, which generally reflects the number of red CALCIUM: A calcium test is ordered to screen for, blood cells in the blood. Hematocrit measures the diagnose and monitor a range of conditions percentage of a person’s total blood volume that relating to the bones, heart, nerves, kidneys and consists of red blood cells. Platelets are cell fragments teeth. The test may also be ordered if a person has that are vital for normal blood clotting. symptoms of parathyroid disorder, malabsorption or an overactive thyroid. FREE T4: Free T4 is used to help evaluate thyroid function, generally after determining the TSH is CREATININE: The creatinine blood test is used to abnormal. -

Metabolism Lectures Diabetes
Metabolism Lectures Diabetes Dalay Olson Ph.D. Integrative Biology and Physiology Email: [email protected] Office: 3-120 Jackson Hall Learning Objectives 1. Compare and contrast type 1 and type 2 diabetes. Identify the major similarities and differences (insulin level, insulin signaling events, treatment options, glucose tolerance test responses etc.) 2. How is diabetes diagnosed in the clinic? What tests are available and commonly used? What information does a glucose tolerance give you? What information does a hemoglobin A1C tell you? What are the limitations of these tests? 3. Explain how chronic elevation of blood glucose levels can result in AGE formation and AGE receptor (RAGE) activation. Explain the downstream effects of RAGE activation. 4. Identify the role of PKC (Protein Kinase C) in arteriolar vasoconstriction in type 2 diabetics. 5. List the common symptoms you might see in the clinic for a patient suffering from type 2 diabetes. 6. Explain why the plasma becomes acidic in a patient with uncontrolled diabetes. 7. Explain the mechanism of action (what is the point of the drug?) of insulin sensitizers, insulin mimetics, insulin secretagogues and SGLT2 inhibitors. Natural Progression of Type-2-Diabetes Pre-diabetes Lean Obese Henry, Am J Med 1998; 105 (1A):20S-6S Think about what is happening with Type 1 diabetics…how does their response differ from that of a normal person? Glucose Insulin is not present, Insulin binds to receptor therefore the signal transduction pathway is not initiated and glucose Glucose transporters remain in enters cell Exocytosis intracellular vesicles. Signal transduction cascade Plasma glucose remains high! GLUT4 Think about what is happening with Type-2-diabetics…how does their response differ from that of a Type-1- diabetic? Glucose Insulin is present but is not Insulin binds to receptor functional, therefore the signal transduction pathway is not initiated and glucose Glucose transporters remain in Exocytosis enters cell intracellular vesicles. -

Diagnosis of Insulinoma in a Maine Coon
JOR0010.1177/2055116919894782Journal of Feline Medicine and Surgery Open ReportsGifford et al 894782research-article2020 Case Report Journal of Feline Medicine and Surgery Open Reports Diagnosis of insulinoma in 1 –10 © The Author(s) 2020 Article reuse guidelines: a Maine Coon cat sagepub.com/journals-permissions DOI:https://doi.org/10.1177/2055116919894782 10.1177/2055116919894782 journals.sagepub.com/home/jfmsopenreports This paper was handled and processed by the American Editorial Office (AAFP) 1 2 3 Carol H Gifford , Anita P Morris , Kurt J Kenney and for publication in JFMS Open Reports J Scot Estep4 Abstract Case summary A 9-year-old male neutered Maine Coon cat presented with a 6-month history of polyphagia and one recent episode of tremors and weakness. Blood work revealed profound hypoglycemia and results of a paired insulin glucose test were consistent with an insulinoma. Abdominal ultrasound revealed a solitary pancreatic mass, and results of a fine-needle aspirate (FNA) gave further support for the location of the neuroendocrine tumor. After unsuccessful medical management of the hypoglycemia, the mass was surgically removed. Immunohistochemistry confirmed that it was an insulinoma. At the time of writing, the patient had been in clinical remission for 9 months. Relevance and novel information Feline insulinomas are rare and there is very little information on their behavior, clinical course and histologic characteristics. This is the first reported case of an insulinoma in a Maine Coon cat and the first to describe results of an ultrasound-guided FNA of the mass. In addition, the progression of disease, histopathology and immunohistochemistry results add to the currently minimal database for feline insulinomas. -

Levels of Serum Uric Acid in Patients with Impaired Glucose Tolerance
JOURNAL OF CRITICAL REVIEWS ISSN- 2394-5125 VOL 08, ISSUE 02, 2021 LEVELS OF SERUM URIC ACID IN PATIENTS WITH IMPAIRED GLUCOSE TOLERANCE 1,2Shahzad Ali Jiskani*, 1Lubna Naz, 3Ali Akbar Pirzado, 4Dolat Singh, 5Asadullah Hanif, 6Razia Bano 1Department of Pathology, Chandka Medical College, SMBBMU, Larkano 2Department of Pathology, Indus Medical College Hospital, Tando Muhammad Khan 3Department of Community Medicine and Public Health, Chadka Medical College, SMBBMU, Larkana 4Department of Medicine, Indus Medical College Hospital, Tando Muhammad Khan 5Health Department, Govt. of Sindh 6Department of Medicine, Liaquat University of Medical & Health Sciences Jamshoro *Corresponding Author: Shahzad Ali Jiskani Department of Pathology, Chandka Medical College, SMBBMU, Larkano ABSTRACT Objective: The main objective of this study is to see levels of serum uric acid in patients having impaired glucose tolerance as compared to normal glucose tolerant individuals. Patients and Methods: This was prospective study, conducted at Department of Medicine and Department of Pathology, Indus Medical College Hospital, Tando Muhammad Khan for the period of 8 months (March 2019 to October 2019). A total of 140 patients were included in this study. An oral glucose test was performed with load of 75g glucose in patients having impaired glucose in fasting. Both normal glucose tolerance and impaired glucose tolerance individuals were evaluated for their serum uric acid level. Serum glucose levels and serum uric acid levels were performed on COBAS C-111 Chemistry Analyzer ensuring procedures of quality control. Data was entered and analyzed using SPSS 21.0. Results: In patients having impaired glucose tolerance, the frequency of hyperuricemia was 62.35%. Analysis of both groups (patients with normal glucose tolerance and glucose intolerance), association was strong with p-value of <0.001. -

C-Reactive Protein and Gamma-Glutamyltransferase
Hindawi Publishing Corporation Experimental Diabetes Research Volume 2010, Article ID 761715, 8 pages doi:10.1155/2010/761715 Clinical Study C-Reactive Protein and Gamma-Glutamyltransferase Concentrations in Relation to the Prevalence of Type 2 Diabetes Diagnosed by Glucose or HbA1c Criteria in Chinese Adults in Qingdao, China J. Ren,1 Z. C. Pang,2 W. G. Gao,3, 4, 5 H. R. Nan,6 S. J. Wang,2 L. Zhang,3, 4, 5 and Q. Qiao3, 4 1 Department of Epidemiology and Health Statistics, Shandong University, Jinan 250012, China 2 Department of Non-Communicable Disease Prevention, Qingdao Municipal Centre for Disease Control and Prevention, no. 175, Shandong Road, Qingdao 266071, China 3 Department of Public Health, University of Helsinki, 00014 Helsinki, Finland 4 Diabetes Unit, Department of Chronic Disease Prevention, National Institute for Health and Welfare, 00014 Helsinki, Finland 5 Qingdao Endocrinology and Diabetes Hospital, 266071 Qingdao, China 6 Hong Kong Institute of Diabetes and Obesity, Hong Kong, China CorrespondenceshouldbeaddressedtoZ.C.Pang,[email protected] Received 13 August 2010; Revised 12 October 2010; Accepted 12 October 2010 Academic Editor: Giuseppe Paolisso Copyright © 2010 J. Ren et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. Aims. To investigate the association of C-reactive protein (CRP) and gamma glutamyltransferase (GGT) concentrations with newly diagnosed diabetes defined by either glucose or HbA1c criteria in Chinese adults. Methods. A population-based cross-sectional study was conducted in 2006. Data from 1167 men and 1607 women aged 35–74 years were analyzed. -
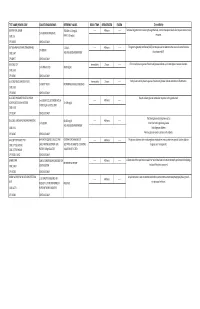
G's- Lab Test Menu
TEST NAME/ PSYCHE CODE COLLECTION GUIDELINES REFERENCE VALUES ROOM TEMP. REFRIGERATED FROZEN Clinical Utility GENTAMICIN, SERUM TROUGH: 0-2.0 mg/dL ------ 48 hours ------ Tests level of gentamicin circulating through the body. Certain therapeutic levels elicit require anti-microbial 2 ml SERUM. REFRIGERATE. CODE: GE PEAK: 5-10 mg/dL response. CPT: 81070 SCHEDULE: DAILY GGT (GAMMA GLUTAMYL TRANSFERASE) 5-31 IU/L ------ 48 hours ------ The gamma-glutamyl transferase (GGT) test may be used to determine the cause of elevated alkaline 1ml SERUM CODE: GGT AGE AND GENDER DEPENDENT phosphatase (ALP). CPT:82977 SCHEDULE: DAILY GLUCOSE, CSF Immediately 2 hours ------ CFS normally has no glucose. Presence of glucose indicates spinal meningitis or seizure disorders. 1 ml SPINAL FLUID 40-80 mg/mL CODE: GLFL CPT: 82947 SCHEDULE: DAILY GLUCOSE, MISCELLANEOUS FLUID Immediately 2 hours ------ Body fluids normally have no glucose. Presence of glucose indicates infection or inflammation. 1 ml BODY FLUID NO NORMAL RANGE ESTABLISHED CODE: GLFL CPT: 82945 SCHEDULE: DAILY GLUCOSE, PREGNANT RELATED 1 HOUR Results indicate glucose metabolism response to the glucola load. 1 ml SERUM COLLECTED ONE HOUR ------ 48 hours ------ LOADING (O'SULLIVAN SCREEN) 70-139 mg/dL AFTER 50 gm GLUCOSE LOAD CODE: GESC CPT: 82947 SCHEDULE: DAILY The blood glucose test may be used to: GLUCOSE, SERUM (FASTING AND RANDOM) 60-115 mg/dL ------ 48 hours ------ 1 ml SERUM Screen for both high blood glucose AGE AND GENDER DEPENDENT CODE: GLU Help diagnose diabetes CPT: 82947 SCHEDULE: DAILY Monitor glucose levels in persons with diabetes GLUCOSE TOLERANCE TEST 8HR FAST REQUIRED. COLLECT AND CRITERIA FOR DIAGNOSIS OF ------ 48 hours ------ The glucose tolerance test monitors glucose metabolism over a certain time period. -

Insulin Tolerance Test (ITT)
Insulin Tolerance Test (ITT) Indications: • This test is less frequently performed now but it is regarded as being the gold standard for the assessment of ACTH / Cortisol and Growth Hormone (GH) reserve in patients with pituitary/hypothalamic disease. • It is also sometimes used in the diagnosis of Cushing’s Syndrome. • The test may be combined with the GnRH or TRH tests although this is also rarely indicated. Contraindications: Ischaemic Heart Disease, Epilepsy or unexplained blackouts, severe long-standing; Hypoadrenalism and Glycogen Storage Disease. Precautions: ECG must be normal. Serum cortisol (09:00) must be > 100mmol/l. T4 must be normal - if abnormal or in doubt perform a Glucagon Test. Prior to test: • Give Lab. require prior warning (one weeks notice preferred) • Obtain accurate weight of patient. • Check patient has had recent ECG. • Give or send patient information letter at time of booking. • Arrange test for around 08:30am. • Ensure that the registrar on call is given prior warning of test date and time. Registrar should complete the prescription chart with the calculated Insulin dose. Registrar should remain in unit throughout test. • Insulin dose = 0.15u/kg body weight. Actrapid Insulin used. • Trolley prepared with : Dextrose 50% - 50ml syringe ; Hydrocortisone 100mg & syringes. • One Touch Glucose Meter. Minute minder required to time sample collection Procedure: • One nurse dedicated to test. • Patient fasting. • Patient supine throughout test. • Observation sheet to be completed (see example attached) Observations to include BP, pulse, sweating, cognitive function.. • IV cannula sited (green preferred) • Blood samples are collected at time 0 , IV bolus dose of insulin given and cannula flushed with 5mls 0.9% Normal Saline. -

Insulin Tolerance Test
ENDOCRINE TESTING UNIT Patient Information Sheet – Insulin Tolerance Test Your doctor has referred you to the Endocrine Testing Unit (ETU) for an Insulin Tolerance Test. What is an insulin tolerance test (ITT)? The insulin tolerance test or insulin stress test is designed to see how your pituitary gland (a small gland that lies just under the brain) functions under stress. Your pituitary gland normally produces several hormones, two of these are: ACTH (adreno-cortico-trophic hormone) which stimulates the adrenal glands (above the kidneys) to make the hormone cortisol. Cortisol is a steroid hormone that is vital for health. Its functions include: o Helping to regulate blood pressure o Helping to regulate the immune system o Helping to balance the effect of insulin and blood sugar levels o Helping the body respond to stress GH (growth hormone) effects childhood growth and adult body composition as well as the functioning of several body systems. The insulin tolerance test will assess how much ACTH, cortisol and growth hormone is produced when your body is under stress. This ‘stress’ will be induced by injecting a small amount of insulin to cause a lowering of your blood glucose (hypoglycaemia), under very controlled conditions. Your Endocrinologist will use the results of this test to determine if these hormones are being produced in sufficient quantities naturally or if they need to be replaced by medication. You should not have this test if you have epilepsy, ischaemic heart disease such as angina or previous heart attack or stroke. How do I prepare for this test? You must have nothing to eat or drink (except water) from midnight the night before the test If you are taking steroid medication, such as prednisone or cortisone, you should omit your dose 24 hours prior to the test. -

Clinical Performance of Flash Glucose Monitoring System in Patients With
www.nature.com/scientificreports OPEN Clinical Performance of Flash Glucose Monitoring System in Patients with Liver Cirrhosis and Diabetes Mellitus Dalila Costa1,2 ✉ , Joana Lourenço1, Ana Margarida Monteiro3, Beatriz Castro1, Patricia Oliveira3, Maria Carmo Tinoco3, Vera Fernandes3, Olinda Marques3, Raquel Gonçalves2 & Carla Rolanda1,2 Flash glucose monitoring system (FGMS) is an improved subset of continuous glucose monitoring with a recognized efectiveness on glycemic control, though validation in patients with Liver Cirrhosis (LC) is lacking. To evaluate the accuracy of FGMS in patients with Type 2 Diabetes Mellitus (DM) and LC, a prospective, case-control study was performed in 61 ambulatory patients with LC and DM (LC group, n = 31) or DM (Control group, n = 30). During 14 days, patients performed 4 assessments per day of self-monitoring of blood glucose (SMBG, reference value) followed by FGMS scanning. There were 2567 paired SMBG and FGMS values used in the accuracy analysis, with an overall mean absolute relative diference (MARD) of 12.68% in the LC group and 10.55% in the control group (p < 0,001). In patients with LC, the percentage of readings within Consensus Consensus Error Grid analysis Zone A and A + B were 80.36% and 99,26%, respectively. Sensor clinical accuracy was not afected by factors such as body mass index, age, gender, Child-Pugh score or edematoascitic decompensation. This is the frst study to approach FGMS clinical accuracy in LC, revealing a potential usability of this system to monitor glycemic control in this population. Type 2 Diabetes Mellitus (DM) has been considered a Public Health challenge due to its signifcant impact on mortality and morbidity worldwide1. -

Journal of Gynecology & Reproductive Medicine
Research Article Journal of Gynecology & Reproductive Medicine The Association Between Hyperuricemia in first Trimester and the Development of Gestational Diabetes Mounir Mohammed Fawzy, Mohamed El-Mandooh Mohamed, Alaa Sayed Hassanin and Mina Nashaat Ghally1* *Corresponding author Resident of Obstetrics and Gynecology, Al-Qussia central Hospital. Mina Nashaat Ghally, Resident of Obstetrics andGynecology, Al-Qussia central Hospital, Egypt. Submitted: 30 June 2017; Accepted: 03 July 2017; Published: 05 July 2017 Abstract Objective: This study aimed to assess the accuracy of the elevation of serum uric acid in the first trimester as a predictive test for development of gestational diabetes mellitus. Patientsand methods: It was a prospective observational study included 200 pregnant patients who were regularly attending the out-patient clinic for routine antenatal care to find if the elevated first trimester uric acid is associated with development of GDM or not. Results: The risk of developing GDM was higher if first-trimester uric acid was < 3.1 mg/dI. Women who developed GDM were significantly older when they compared to women who did not develop GDM [Normal with Mean + SD 24.53 + 4.40 years, Abnormal with Mean + SD 32.78 + 8.18 years, p-value 0.016]. It was found that, the mean BMI was significantly higher in women who developed GDM when compared to women who did not develop GDM [Normal 115 cases of total sample and no one developed GD with Mean + SD, 95.57 + 12.32, Overweight 59 cases, 56 cases (29.3%) were normal and 3 cases (33.3%) had GD with Mean + SD 106.29 + 26.62, Obese 26 cases, 20 cases (10.5%) were normal and 6 cases (66.7%) had GD with Mean + SD 124.27 + 39.78, p-value 0.000]. -
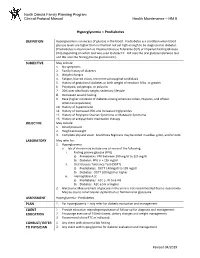
Hyperglycemia – Prediabetes
North Dakota Family Planning Program Clinical Protocol Manual Health Maintenance – HM 8 Hyperglycemia – Prediabetes DEFINITION Hyperglycemia is an excess of glucose in the blood. Prediabetes is a condition when blood glucose levels are higher than normal but not yet high enough to be diagnosed as diabetes. (Prediabetes is also known as Impaired Glucose Tolerance (IGT) or Impaired Fasting Glucose (IFG) depending on which test was used to detect it. IGT uses the oral glucose tolerance test and IFG uses the fasting plasma glucose test.) SUBJECTIVE May include: 1. No symptoms 2. Family history of diabetes 3. Weight changes 4. Fatigue, blurred vision, recurrent vulvovaginal candidiasis 5. History of gestational diabetes or birth weight of newborn 9 lbs. or greater 6. Polydipsia, polyphagia, or polyuria 7. 20% over ideal body weight; sedentary lifestyle 8. Decreased wound healing 9. Race (higher incidence of diabetes among American Indian, Hispanic, and African American population) 10. History of hypertension 11. History of decreased HDL and increased triglycerides 12. History of Polycystic Ovarian Syndrome or Metabolic Syndrome 13. History of antipsychotic medication therapy OBJECTIVE May include: 1. Blood pressure 2. Height and weight 3. Complete physical exam. Acanthosis Nigricans may be noted in axillae, groin, and/or neck LABORATORY May refer for: 1. Hyperglycemia a. lab of choice may include one or more of the following: i. Fasting plasma glucose (FPG) a) Prediabetes: FPG between 100 mg/dl to 125 mg/dl b) Diabetes: FPG is > 126 mg/dl ii. Oral Glucose Tolerance Test (OGTT) a) Prediabetes: OGTT 140mg/dl to 199 mg/dl b) Diabetes: OGTT 200mg/dl or higher iii. -

Standards of Medical Care for Patients with Diabetes Mellitus
POSITION STATEMENT Standards of Medical Care for Patients With Diabetes Mellitus iabetes is a chronic illness that requires contin- Dietary habits, nutritional status, and weight history; uing medical care and education to prevent acute growth and development in children complications and to reduce the risk of long- Details of previous treatment programs, including Dterm complications. People with diabetes should diabetes education receive their treatment and care from physicians with Current treatment of diabetes, including medications, expertise and a special interest in diabetes. The follow- diet, and results of glucose monitoring ing standards define basic (minimum) medical care for Exercise history people with diabetes. These standards are not intended Frequency, severity, and cause of acute complica- to preclude more extensive evaluation and management tions such as ketoacidosis and hypoglycemia of the patient. For more detailed information refer to Prior or current infections, particularly skin, foot, den- Physician's Guide to Insulin-Dependent (Type I) Dia- tal, and genitourinary betes: Diagnosis and Treatment and Physician's Guide Symptoms and treatment of chronic complications to Non-Insulin-Dependent (Type II) Diabetes: Diagnosis associated with diabetes: eye, heart, kidney, nerve, and Treatment. sexual function, peripheral vascular, and cerebral vascular Other medications that may affect blood glucose INITIAL VISIT concentration Risk factors for atherosclerosis: smoking, hyperten- Medical history. The comprehensive medical