Photoageing Skin of the Elderly
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Metastasizing Melanoma Formation Caused by Expression of Activated N-Rasq61k on an Ink4a-Deficient Background
Research Article Metastasizing Melanoma Formation Caused by Expression of Activated N-RasQ61K on an INK4a-Deficient Background Julien Ackermann,1 Manon Frutschi,1 Kostas Kaloulis,1 Thomas McKee,2 Andreas Trumpp,1 and Friedrich Beermann1 1ISREC, Swiss Institute for Experimental Cancer Research, National Center of Competence in Research Molecular Oncology, Epalinges, Switzerland and 2Institute of Pathology, University of Lausanne, Lausanne, Switzerland Abstract the most common factors predisposing to melanoma formation in humans is the INK4a/ARF locus (4), which is inactivated with high In human cutaneous malignant melanoma, a predominance of frequency in human melanoma. This locus encodes two distinct activated mutations in the N-ras gene has been documented. INK4a ARF ARF To obtain a mouse model most closely mimicking the human proteins by alternative exon usage, p16 and p14 (p19 in disease, a transgenic mouse line was generated by targeting mice), which function as tumor suppressor genes in the pRB and expression of dominant-active human N-ras (N-RasQ61K) to the p53 pathways, respectively (4, 5). Gene-targeted mice, where p16INK4a and p19ARF are deleted, develop a large variety of tumors melanocyte lineage by tyrosinase regulatory sequences INK4a Q61K but fail to develop melanoma (6). Mice deficient in p16 but (Tyr::N-Ras ). Transgenic mice show hyperpigmented skin ARF and develop cutaneous metastasizing melanoma. Consistent which retain one copy of p19 show carcinogen-induced with the tumor suppressor function of the INK4a locus that susceptibility to metastatic melanoma (7, 8). Transgenic mice that encodes p16INK4A and p19ARF, >90% of Tyr::N-RasQ61K INK4aÀ/À express a mutant form of H-ras specifically in melanocytes showed melanocytic hyperplasia with intense skin pigmentation (9), which transgenic mice develop melanoma at 6 months. -

Laser Treatment for Pigmentation
Laser treatment for pigmentation Sunspots and freckles In lesions such as solar lentigines (sun induced age spots), lentigo simplex and ephelides (freckles) the pigment (melanin) is in the top layers of the skin. Many lasers that selectively target melanin or simply remove the top layers will lead to improvement. One to two treatments will be necessary. There are many non-laser treatment approaches to treat such spots. However, if laser therapy is chosen, there are many different types of laser that can be used including Q-switched lasers [Q switched (QS) alexandrite, QS ruby (694nm)], long-pulsed, fractionated thulium (1927nm) and ablative lasers. IPL (filter 500-600nm) can also be very effective. However, it is common to see the pigmentation return over time. Treatments need to be avoided if the skin is tanned because this greatly increases the risk of complications. Seborrhoeic warts and dermatosis papulosa nigra Some conditions that present as dark spots are in fact wart-like and sit on the surface of the skin such as seborhoeic keratoses and dermatosis papulosa nigra and epidermal naevi. These conditions require physical removal. This is most commonly treated with a curette if thick or with fine wire diathermy particularly for the dermatosis papulosa nigra. Ablative lasers may also be used including CO2 in combination with a curette or an erbium YAG laser which reliably gives the best results. These lesions have a tendency to return over a number of years and maintenance treatments may be needed. Pigmented birth marks – Becker’s naevus Current lasers are unable to remove pigmented birthmarks without scarring. -

Dermatopathology
Dermatopathology Clay Cockerell • Martin C. Mihm Jr. • Brian J. Hall Cary Chisholm • Chad Jessup • Margaret Merola With contributions from: Jerad M. Gardner • Talley Whang Dermatopathology Clinicopathological Correlations Clay Cockerell Cary Chisholm Department of Dermatology Department of Pathology and Dermatopathology University of Texas Southwestern Medical Center Central Texas Pathology Laboratory Dallas , TX Waco , TX USA USA Martin C. Mihm Jr. Chad Jessup Department of Dermatology Department of Dermatology Brigham and Women’s Hospital Tufts Medical Center Boston , MA Boston , MA USA USA Brian J. Hall Margaret Merola Department of Dermatology Department of Pathology University of Texas Southwestern Medical Center Brigham and Women’s Hospital Dallas , TX Boston , MA USA USA With contributions from: Jerad M. Gardner Talley Whang Department of Pathology and Dermatology Harvard Vanguard Medical Associates University of Arkansas for Medical Sciences Boston, MA Little Rock, AR USA USA ISBN 978-1-4471-5447-1 ISBN 978-1-4471-5448-8 (eBook) DOI 10.1007/978-1-4471-5448-8 Springer London Heidelberg New York Dordrecht Library of Congress Control Number: 2013956345 © Springer-Verlag London 2014 This work is subject to copyright. All rights are reserved by the Publisher, whether the whole or part of the material is concerned, specifi cally the rights of translation, reprinting, reuse of illustrations, recitation, broadcasting, reproduction on microfi lms or in any other physical way, and transmission or information storage and retrieval, electronic adaptation, computer software, or by similar or dissimilar methodology now known or hereafter developed. Exempted from this legal reservation are brief excerpts in connection with reviews or scholarly analysis or material supplied specifi cally for the purpose of being entered and executed on a computer system, for exclusive use by the purchaser of the work. -
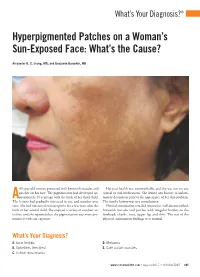
Hyperpigmented Patches on a Woman's Sun-Exposed Face
What’s Your Diagnosis?® Hyperpigmented Patches on a Woman’s Sun-Exposed Face: What’s the Cause? Alexander K. C. Leung, MD, and Benjamin Barankin, MD 45-year-old woman presented with brownish macules and Her past health was unremarkable, and she was not on any patches on her face. The pigmentation had developed ap- topical or oral medications. She denied any history of inflam- A proximately 10 years ago with the birth of her third child. matory dermatosis prior to the appearance of her skin problem. The lesions had gradually increased in size and number over The family history was not contributory. time. She had taken oral contraceptives for a few years after the Physical examination revealed symmetric, well-circumscribed, birth of her second child. She enjoyed a variety of outdoor ac- brownish macules and patches with irregular borders on the tivities, and she reported that the pigmentation was more pro- forehead, cheeks, nose, upper lip, and chin. The rest of the nounced with sun exposure. physical examination findings were normal. What’s Your Diagnosis? A. Solar lentigo D. Melasma B. Ephelides (freckles) E. Café au lait macules C. Actinic dyschromia www.consultant360.com • August 2017 • CONSULTANT 485 What’s Your Diagnosis?® Answer: Melasma A diagnosis of melasma was made. Wood lamp examination basement membrane disruption and dermal changes, indepen- showed accentuation of pigmentation suggestive of epidermal dent of UV radiation.1,17 pigmentation. The patient was treated with a series of trichlo- roacetic acid chemical peels, as well as a topical azelaic acid and HISTOPATHOLOGY a retinoid-hydroquinone-steroid (modified Kligman) formula- Three histologic patterns of pigmentation have been described: tion with significant, albeit incomplete, improvement. -

Quality of Life and Photodermatoses in People with Albinism in Benin City Nigeria
QUALITY OF LIFE AND PHOTODERMATOSES IN PEOPLE WITH ALBINISM IN BENIN CITY NIGERIA DISSERTATION SUBMITTED TO NATIONAL POSTGRADUATE MEDICAL COLLEGE OF NIGERIA IN PARTIAL FULFILMENT OF THE REQUIREMENTS FOR THE FELLOWSHIP IN INTERNAL MEDICINE (SUB-SPECIALTY: DERMATOLOGY) BY DR CYNTHIA ROLI MADUBUKO MB,BS (BENIN) DEPARTMENT OF MEDICINE UNIVERSITY OF BENIN TEACHING HOSPITAL, BENIN CITY, EDO STATE, NIGERIA NOVEMBER, 2016. i DECLARATION I hereby declare that this work is original and no part of it has been presented to any other college for a fellowship dissertation nor has it been submitted elsewhere for publication. Signature.................................... Date........................... Dr. Cynthia Roli Madubuko ii SUPERVISION We the undersigned have supervised the writing of this dissertation and the execution of this study. SIGNATURE: …………………………………… DATE: …………………………………………… YEAR OF FELLOWSHIP: ……………………… DR. B. OKWARA MBBS, FMCP Consultant Physician/ Dermatologist and Venereologist Department of Internal Medicine, University of Benin Teaching Hospital, Benin City, Nigeria. SIGNATURE: …………………………………… DATE: …………………………………………… YEAR OF FELLOWSHIP: ……………………… PROF. A.N. ONUNU MBBS, FWACP, FACP Consultant Physician/ Dermatologist and Venereologist Department of Internal Medicine, University of Benin Teaching Hospital, Benin City, Nigeria. SIGNATURE: …………………………………… DATE: …………………………………………… YEAR OF FELLOWSHIP: ……………………… PROF. E.P KUBEYINJE MBBS, FRCP (London), FWACP Consultant Physician Dermatologist and Venereologist Department of Internal Medicine, University of Benin Teaching Hospital, Benin City, Nigeria. iii CERTIFICATION I certify that this is a part 2 dissertation of the National postgraduate Medical College of Nigeria by Dr. Cynthia Roli Madubuko, of the Department of Internal Medicine, University of Benin Teaching Hospital, Benin City, under the supervision of Prof. A.N Onunu, Prof. E.P. Kubeyinje and Dr. B. Okwara Sign……………………………………. Date.............................................. DR OMUEMU, MBBS, FWACP. -

Actinic Cheilitis
ACTINIC CHEILITIS http://www.aocd.org Actinic cheilitis, also known as solar cheilosis, farmer’s lip, or sailor’s lip, is a reaction to long-term sun exposure on the lips, primarily the lower lip. The lip is especially susceptible to UV radiation because it has a thinner epithelium and less pigment. Some believe actinic cheilitis represents a type of actinic keratosis and is therefore premalignant. Others believe it is a form of in-situ squamous cell carcinoma. Regardless, the literature is in agreement that its presence indicates an increased risk for invasive squamous cell carcinoma. Risk factors for actinic cheilitis include fair complexion, everted lips, male sex, advanced age, living at high altitudes, living close to the equator, outdoor working, history of non-melanoma skin cancer, and any condition that increases photosensitivity. Clinically, patients commonly have other signs of sun damage such as poikiloderma of Civatte, solar lentigines, actinic keratoses, Favre-Racouchot Syndrome, cutis rhomboidalis nuchae, and solar elastosis. Patients often complain of persistent chapped lips or lip tightness. Early changes include atrophy and blurring of the vermilion border. The lips become scaly and rough; erosions or fissures may occasionally present. When palpated, it can have a sandpaper-like texture. Differential diagnosis can include chronic lip licking, granulomatous cheilitis, drug-induced cheilitis, contact dermatitis, cheilitis glandularis, lupus erythematosus, and lichen planus. An appropriate history can help elicit the proper diagnosis, such as inquiring about new medications or lip balms, lip-licking habits, and cumulative sun exposure. When actinic cheilitis is suspected, one must determine whether a biopsy is appropriate. -

Treatment of Poikiloderma of Civatte with Ablative Fractional Laser Resurfacing: Prospective Study and Review of the Literature Emily P
JUNE 2009 527 Vo l u m e 8 • Is s u e 6 CO P YR IGHT © 2009 ORIGINAL ARTICLES JOURN A L OF DRUGS IN DER MA TOLOGY Treatment of Poikiloderma of Civatte With Ablative Fractional Laser Resurfacing: Prospective Study and Review of the Literature emily P. Tierney MD and C. William Hanke MD MPH Laser and Skin Surgery Center of Indiana, Carmel, IN ABSTRACT Background: Previous laser treatments for Poikiloderma of Civatte (PC) (i.e., Pulsed dye, Intense Pulsed Light, KTP and Argon) are limited by side effect profiles and/or efficacy. Given the high degree of safety and efficacy of ablative fractional photothermolysis (AFP) for photoaging, we set out to assess the efficacy of PC with AFP. Design: A prospective pilot study for PC in 10 subjects with a series of 1−3 treatment sessions. Treatment sessions were adminis- tered at 6−8 week intervals with blinded physician photographic analysis of improvement at 2 months post-treatment. Evaluation was performed of five clinical indicators, erythema/telangiecatasia, dyschromia, skin texture, skin laxity and cosmetic outcome. Results: The number of treatments required for improvement of PC ranged from 1 to 3, with an average of 1.4. For erythema/te- langiecatasia, the mean score improved 65.0% (95% CI: 60.7%, 69.3%) dyschromia, 66.7% (95% CI: 61.8%, 71.6%), skin texture, 51.7% (95% CI: 48.3%, 55.1%) and skin laxity, 52.5% (95% CI: 49.6%, 55.4%). For cosmetic outcome, the mean score improved 66.7% (95% CI: 62.6%, 70.8%) at 2 months post treatment. -

Reticulate Dermatoses
[Downloaded free from http://www.e-ijd.org on Tuesday, April 08, 2014, IP: 111.93.251.154] || Click here to download free Android application for this journal CME Article Reticulate Dermatoses Keshavmurthy A Adya, Arun C Inamadar, Aparna Palit From the Department of Dermatology, Venereology and Leprosy, SBMP Medical College, Hospital and Research Center, BLDE University, Bijapur, Karnataka, India Abstract The term “reticulate” is used for clinical description of skin lesions that are configured in a net-like pattern. Many primary and secondary dermatoses present in such patterns involving specific body sites. Certain cutaneous manifestations of systemic diseases or genodermatoses also present in such manner. This review classifies and describes such conditions with reticulate lesions and briefly, their associated features. Key Words: Mottling, net-like, reticulate, retiform What was known? 3. Poikilodermatous Reticulate configuration of lesions is seen in many primary dermatoses and a. Inherited also as cutaneous reaction patterns consequent to internal pathology. • Rothmund–Thomson syndrome • Dyskeratosis congenita Reticulate Dermatoses • Xeroderma pigmentosum • Cockayne syndrome The term “reticulate” is commonly used for clinical • Fanconi anemia description of “net-like”, “sieve-like,” or “chicken wire” • Mendes da Costa syndrome configuration of the skin lesions. Various congenital • Kindler syndrome and acquired dermatoses present with this pattern of • Degos–Touraine syndrome skin lesions. Many systemic diseases also present with • Hereditary sclerosing poikiloderma of Weary such cutaneous manifestations providing useful clues to • Hereditary acrokeratotic poikiloderma of Weary diagnosis. • Werner’s syndrome (adult progeria) Classification • Chanarin–Dorfman syndrome • Diffuse and macular atrophic dermatosis 1. Vascular b. Acquired a. Cutis marmorata • Poikiloderma of Civatte b. -

Dermamelan ® Treatment for Melasma and Hyperpigmentation
Dermamelan ® treatment for melasma and hyperpigmentation Jean Luc Levy Expert Laser, Dermatologist Lausanne, Switzerland [email protected] Incidence of Melasma Caucasian Melasma is estimated to occur in 50%-70% of pregnancies among US women, usually during the 2nd or 3rd trimester of pregnancy. Asian In Asian countries, the estimated prevalence of melasma within skin type III-V is estimated to be as high as 40% in females and 20% in males. Hispanic Among Mexican women, the incidence is estimated to be about 80%, with more than one-third of these patients having the disease for life. Retrospective Study on the Clinical Presentation and Treatment Outcome of Melasma in a Tertiary Dermatolofical Referral Centre in Singapore C L Goh, C N Dlova, Singapore Med J 1999; Vol 40(07): Melasma in Orientals. Sivayathorn A. Clin Drug Invest 1995; 10 (Suppl 2):24-40. ‘Utilizing combination therapy to optimize melasma outcomes’, M, I, Rendon(2004), Journal of Drugs in Dermatology, Sept-Oct. Facial melasma : Sun history Majority of melasma are very sensitive to sun exposure and tanned during summer - Sunblock regurlaly applied are poorly effective - During winter quality of life is better Some of them are poorly sensitive to sun exposure and colour acquired is near from the surrounding skin - During winter color differences between melasma and surrounding skin is high and covermark required Upper forehead without due to the tissue Sun exposed and non sun exposed areas Facial melasma : locations Forehead : with commonly a lighten aspect if hair is used -
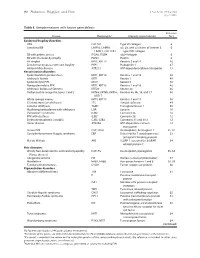

Table I. Genodermatoses with Known Gene Defects 92 Pulkkinen
92 Pulkkinen, Ringpfeil, and Uitto JAM ACAD DERMATOL JULY 2002 Table I. Genodermatoses with known gene defects Reference Disease Mutated gene* Affected protein/function No.† Epidermal fragility disorders DEB COL7A1 Type VII collagen 6 Junctional EB LAMA3, LAMB3, ␣3, 3, and ␥2 chains of laminin 5, 6 LAMC2, COL17A1 type XVII collagen EB with pyloric atresia ITGA6, ITGB4 ␣64 Integrin 6 EB with muscular dystrophy PLEC1 Plectin 6 EB simplex KRT5, KRT14 Keratins 5 and 14 46 Ectodermal dysplasia with skin fragility PKP1 Plakophilin 1 47 Hailey-Hailey disease ATP2C1 ATP-dependent calcium transporter 13 Keratinization disorders Epidermolytic hyperkeratosis KRT1, KRT10 Keratins 1 and 10 46 Ichthyosis hystrix KRT1 Keratin 1 48 Epidermolytic PPK KRT9 Keratin 9 46 Nonepidermolytic PPK KRT1, KRT16 Keratins 1 and 16 46 Ichthyosis bullosa of Siemens KRT2e Keratin 2e 46 Pachyonychia congenita, types 1 and 2 KRT6a, KRT6b, KRT16, Keratins 6a, 6b, 16, and 17 46 KRT17 White sponge naevus KRT4, KRT13 Keratins 4 and 13 46 X-linked recessive ichthyosis STS Steroid sulfatase 49 Lamellar ichthyosis TGM1 Transglutaminase 1 50 Mutilating keratoderma with ichthyosis LOR Loricrin 10 Vohwinkel’s syndrome GJB2 Connexin 26 12 PPK with deafness GJB2 Connexin 26 12 Erythrokeratodermia variabilis GJB3, GJB4 Connexins 31 and 30.3 12 Darier disease ATP2A2 ATP-dependent calcium 14 transporter Striate PPK DSP, DSG1 Desmoplakin, desmoglein 1 51, 52 Conradi-Hu¨nermann-Happle syndrome EBP Delta 8-delta 7 sterol isomerase 53 (emopamil binding protein) Mal de Meleda ARS SLURP-1 -

(12) United States Patent (10) Patent No.: US 7,359,748 B1 Drugge (45) Date of Patent: Apr
USOO7359748B1 (12) United States Patent (10) Patent No.: US 7,359,748 B1 Drugge (45) Date of Patent: Apr. 15, 2008 (54) APPARATUS FOR TOTAL IMMERSION 6,339,216 B1* 1/2002 Wake ..................... 250,214. A PHOTOGRAPHY 6,397,091 B2 * 5/2002 Diab et al. .................. 600,323 6,556,858 B1 * 4/2003 Zeman ............. ... 600,473 (76) Inventor: Rhett Drugge, 50 Glenbrook Rd., Suite 6,597,941 B2. T/2003 Fontenot et al. ............ 600/473 1C, Stamford, NH (US) 06902-2914 7,092,014 B1 8/2006 Li et al. .................. 348.218.1 (*) Notice: Subject to any disclaimer, the term of this k cited. by examiner patent is extended or adjusted under 35 Primary Examiner Daniel Robinson U.S.C. 154(b) by 802 days. (74) Attorney, Agent, or Firm—McCarter & English, LLP (21) Appl. No.: 09/625,712 (57) ABSTRACT (22) Filed: Jul. 26, 2000 Total Immersion Photography (TIP) is disclosed, preferably for the use of screening for various medical and cosmetic (51) Int. Cl. conditions. TIP, in a preferred embodiment, comprises an A6 IB 6/00 (2006.01) enclosed structure that may be sized in accordance with an (52) U.S. Cl. ....................................... 600/476; 600/477 entire person, or individual body parts. Disposed therein are (58) Field of Classification Search ................ 600/476, a plurality of imaging means which may gather a variety of 600/162,407, 477, 478,479, 480; A61 B 6/00 information, e.g., chemical, light, temperature, etc. In a See application file for complete search history. preferred embodiment, a computer and plurality of USB (56) References Cited hubs are used to remotely operate and control digital cam eras. -

Buffalo Medical Group, P.C. Robert E
Buffalo Medical Group, P.C. Robert E. Kalb, M.D. Phone: (716) 630-1102 Fax: (716) 633-6507 Department of Dermatology 325 Essjay Road Williamsville, New York 14221 2 FOOT- 1 HAND SYNDROME 2 foot - 1 hand syndrome is a superficial infection of the skin caused by the common athlete's foot fungus. It is quite common for people to have a minor amount of an athlete's foot condition. This would appear as slight scaling and/or itching between the toes. In addition, patients may have thickened toenails as part of the athlete's foot condition. Again the problem on the feet is very common and often patients are not even aware of it. In some patients, however, the athlete's foot fungus can spread to another area of the body. For some strange and unknown reason, it seems to affect only one hand. That is why the condition is called 2 foot - 1 hand syndrome. It is not clear why the problem develops in only one hand or why the right or left is involved in some patients. Fortunately there is very effective treatment to control this minor skin problem. If the problem with the superficial fungus infection is confined to the skin, then a short course of treatment with an oral antibiotic is all that is required. This antibiotic is very safe and normally clears the skin up fairly rapidly. It is often used with a topical cream to speed the healing process. If, however, the fingernails of the affected hand are also involved then a more prolonged course of the antibiotic will be necessary.