Partial Unilateral Lentiginoses
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Melanocytes and Their Diseases
Downloaded from http://perspectivesinmedicine.cshlp.org/ on October 2, 2021 - Published by Cold Spring Harbor Laboratory Press Melanocytes and Their Diseases Yuji Yamaguchi1 and Vincent J. Hearing2 1Medical, AbbVie GK, Mita, Tokyo 108-6302, Japan 2Laboratory of Cell Biology, National Cancer Institute, National Institutes of Health, Bethesda, Maryland 20892 Correspondence: [email protected] Human melanocytes are distributed not only in the epidermis and in hair follicles but also in mucosa, cochlea (ear), iris (eye), and mesencephalon (brain) among other tissues. Melano- cytes, which are derived from the neural crest, are unique in that they produce eu-/pheo- melanin pigments in unique membrane-bound organelles termed melanosomes, which can be divided into four stages depending on their degree of maturation. Pigmentation production is determined by three distinct elements: enzymes involved in melanin synthesis, proteins required for melanosome structure, and proteins required for their trafficking and distribution. Many genes are involved in regulating pigmentation at various levels, and mutations in many of them cause pigmentary disorders, which can be classified into three types: hyperpigmen- tation (including melasma), hypopigmentation (including oculocutaneous albinism [OCA]), and mixed hyper-/hypopigmentation (including dyschromatosis symmetrica hereditaria). We briefly review vitiligo as a representative of an acquired hypopigmentation disorder. igments that determine human skin colors somes can be divided into four stages depend- Pinclude melanin, hemoglobin (red), hemo- ing on their degree of maturation. Early mela- siderin (brown), carotene (yellow), and bilin nosomes, especially stage I melanosomes, are (yellow). Among those, melanins play key roles similar to lysosomes whereas late melanosomes in determining human skin (and hair) pigmen- contain a structured matrix and highly dense tation. -

Uniform Faint Reticulate Pigment Network - a Dermoscopic Hallmark of Nevus Depigmentosus
Our Dermatology Online Letter to the Editor UUniformniform ffaintaint rreticulateeticulate ppigmentigment nnetworketwork - A ddermoscopicermoscopic hhallmarkallmark ooff nnevusevus ddepigmentosusepigmentosus Surit Malakar1, Samipa Samir Mukherjee2,3, Subrata Malakar3 11st Year Post graduate, Department of Dermatology, SUM Hospital Bhubaneshwar, India, 2Department of Dermatology, Cloud nine Hospital, Bangalore, India, 3Department of Dermatology, Rita Skin Foundation, Kolkata, India Corresponding author: Dr. Samipa Samir Mukherjee, E-mail: [email protected] Sir, ND is a form of cutaneous mosaicism with functionally defective melanocytes and abnormal melanosomes. Nevus depigmentosus (ND) is a localized Histopathologic examination shows normal to hypopigmentation which most of the time is congenital decreased number of melanocytes with S-100 stain and and not uncommonly a diagnostic challenge. ND lesions less reactivity with 3,4-dihydroxyphenylalanine reaction are sometimes difficult to differentiate from other and no melanin incontinence [2]. Electron microscopic hypopigmented lesions like vitiligo, ash leaf macules and findings show stubby dendrites of melanocytes nevus anemicus. Among these naevus depigmentosus containing autophagosomes with aggregates of poses maximum difficulty in differentiating from ash melanosomes. leaf macules because of clinical as well as histological similarities [1]. Although the evolution of newer diagnostic For ease of understanding the pigmentary network techniques like dermoscopy has obviated the -

Skin Pigmentary Variants in Rana Nigromaculata
Original Article J. Clin. Biochem. Nutr., 38, 195–203, May 2006 Skin Pigmentary Variants in Rana Nigromaculata Ichiro Tazawa, Hitoshi Okumoto, and Akihiko Kashiwagi* Division of Embryology and Genetics, Institute for Amphibian Biology, Graduate School of Science, Hiroshima University, 1-3-1 Kagamiyama, Higashihiroshima, Hiroshima 739-8526, Japan Received 22 December, 2005; Accepted 26 January, 2006 Summary Because there is mounting evidence to suggest that oxidative stress is involved in the pathophysiology of albinism, albino amphibians are useful tools for studies on imbalances in the oxidant-antioxidant system. In the course of maintaining albino mutant frog strains it was found that crosses between albino males and heterozygous females of Rana nigromaculata sometimes produce offspring displaying pigmentary mosaicism. After hatching hypopigmented portions appear on the left or right side of the body, and this is accompanied by such abnormalities as poor viability, asymmetrical curvature of the body toward the hypopigmented side, and limb deformity. Histological examination of mosaics showed the cells of various tissues (except kidney) to be smaller on the hypopigmented side and larger on the pigmented side compared to corresponding cells in wild type offspring. Cytogenetic analysis of cultured skin cells revealed that wild type and albino individuals were diploidal with 26 chromosomes, the same as normal R. nigromaculata. In mosaics on the other hand, cells of hypopigmented portions were almost exclusively haploidal with 13 chromosomes, while pigmented portions were a mixture of roughly 75% triploidal, 39 chromosome cells and roughly 25% haploidal, 13 chromosome cells. Key Words: albino, unilateral pigmentation, pigmentary mosaicism, chromosomal mosaicism, mixoploidy, haploid, triploid, Rana one means of assessing the involvement of reactive oxygen Introduction species (ROS) in biological processes such as aging. -

Colocalized Nevus Depigmentosus and Lentigines Prashansa Jaiswal, Sundeep Chowdhry, Paschal D’ Souza
2XU'HUPDWRORJ\2QOLQH Case Report Colocalized nevus depigmentosus and lentigines Prashansa Jaiswal, Sundeep Chowdhry, Paschal D’ Souza Department of Dermatology, Venereology and Leprology, Employees’ State Insurance Corporation Post Graduate Institute of Medical Sciences & Research, Basaidarapur, New Delhi - 110 015, India Corresponding author: Assist. Prof. Sundeep Chowdhry, E-mail: [email protected] ABSTRACT Nevus depigmentosus (ND)is classically defined as a congenital nonprogressive hypopigmented macule, stable in size and distribution. A 17 year girl presented with hypopigmented patch with indented borders, present on the right side of face and neck since 3 years of age. Later on at the age of 5, numerous hyperpigmented punctiform spots appeared exclusively on the hyperpigmented area. On sun exposure, the hypopigmented area neither reddened nor burnt. On diascopy the margin of the hypopigmented lesion remained delineated. The dermoscopic examination showed 1-4 millimeters sized hyperpigmented lesions with a barely visible pseudonet, leading to the final diagnosis of colocalized nevus depigmentosus and lentigines. Key words: Nevus; Hypopigmentation; Reverse; Mutation; Pigmentation INTRODUCTION 25 X 8 centimeters was present at the angle of mouth on right side, further extending to lateral side of right ear, Nevus depigmentosus (ND)is a rare, congenital, right angle of jaw, lateral right side of neck to about 6 stable hypomelanosis first described by Lesser in centimeters below the clavicle. It was irregular in shape 1884 [1]. The lesions usually present as dermatomal with serrated irregular margins. The surface was smooth or quasidermatomal macules commonly on the trunk, and had multiple oval dark brown coloured macules of lower abdomen, or proximal extremities. They are off- 1 to 4 mm in size (Fig. -

Phacomatosis Spilorosea Versus Phacomatosis Melanorosea
Acta Dermatovenerologica 2021;30:27-30 Acta Dermatovenerol APA Alpina, Pannonica et Adriatica doi: 10.15570/actaapa.2021.6 Phacomatosis spilorosea versus phacomatosis melanorosea: a critical reappraisal of the worldwide literature with updated classification of phacomatosis pigmentovascularis Daniele Torchia1 ✉ 1Department of Dermatology, James Paget University Hospital, Gorleston-on-Sea, United Kingdom. Abstract Introduction: Phacomatosis pigmentovascularis is a term encompassing a group of disorders characterized by the coexistence of a segmental pigmented nevus of melanocytic origin and segmental capillary nevus. Over the past decades, confusion over the names and definitions of phacomatosis spilorosea, phacomatosis melanorosea, and their defining nevi, as well as of unclassifi- able phacomatosis pigmentovascularis cases, has led to several misplaced diagnoses in published cases. Methods: A systematic and critical review of the worldwide literature on phacomatosis spilorosea and phacomatosis melanorosea was carried out. Results: This study yielded 18 definite instances of phacomatosis spilorosea and 14 of phacomatosis melanorosea, with one and six previously unrecognized cases, respectively. Conclusions: Phacomatosis spilorosea predominantly involves the musculoskeletal system and can be complicated by neuro- logical manifestations. Phacomatosis melanorosea is sometimes associated with ancillary cutaneous lesions, displays a relevant association with vascular malformations of the brain, and in general appears to be a less severe syndrome. -

Metastasizing Melanoma Formation Caused by Expression of Activated N-Rasq61k on an Ink4a-Deficient Background
Research Article Metastasizing Melanoma Formation Caused by Expression of Activated N-RasQ61K on an INK4a-Deficient Background Julien Ackermann,1 Manon Frutschi,1 Kostas Kaloulis,1 Thomas McKee,2 Andreas Trumpp,1 and Friedrich Beermann1 1ISREC, Swiss Institute for Experimental Cancer Research, National Center of Competence in Research Molecular Oncology, Epalinges, Switzerland and 2Institute of Pathology, University of Lausanne, Lausanne, Switzerland Abstract the most common factors predisposing to melanoma formation in humans is the INK4a/ARF locus (4), which is inactivated with high In human cutaneous malignant melanoma, a predominance of frequency in human melanoma. This locus encodes two distinct activated mutations in the N-ras gene has been documented. INK4a ARF ARF To obtain a mouse model most closely mimicking the human proteins by alternative exon usage, p16 and p14 (p19 in disease, a transgenic mouse line was generated by targeting mice), which function as tumor suppressor genes in the pRB and expression of dominant-active human N-ras (N-RasQ61K) to the p53 pathways, respectively (4, 5). Gene-targeted mice, where p16INK4a and p19ARF are deleted, develop a large variety of tumors melanocyte lineage by tyrosinase regulatory sequences INK4a Q61K but fail to develop melanoma (6). Mice deficient in p16 but (Tyr::N-Ras ). Transgenic mice show hyperpigmented skin ARF and develop cutaneous metastasizing melanoma. Consistent which retain one copy of p19 show carcinogen-induced with the tumor suppressor function of the INK4a locus that susceptibility to metastatic melanoma (7, 8). Transgenic mice that encodes p16INK4A and p19ARF, >90% of Tyr::N-RasQ61K INK4aÀ/À express a mutant form of H-ras specifically in melanocytes showed melanocytic hyperplasia with intense skin pigmentation (9), which transgenic mice develop melanoma at 6 months. -

Preceded by Multiple Diagnostic. X-Rays One Year Prior to The
A Malformation Complex of Ectrodactyly, Clefting and Hypomelanosis of Ito (Incontinentia Pigmenti Achromians) RAY E. STEWART, D.M.D., M.S. STEVEN FUNDERBURK, M.D. YOSHIO SETOGUCHI, M.D. Torrance, California 90509 A case is described which, at birth, had a bizarre pattern of Aypopigmentation (incontinentia pigment achromians), ectrodactyly involving all four extremities, and unilateral cleft lip and palate. This patient does not have the seizures or other neurological and developmental anomalies previously described as associated with Aypopigmentation of Ito. This condition is also clearly different from the syndrome of ectrodactyly, ectodermal dysplasia, and clefting (EEC). We have recently observed four-month-old tone. The child has developed normally, Mexican-American female infant with an in- reaching all of her age-appropriate milestones teresting constellation of anomalies, including with no evidence of neurological or other _ unilateral complete clefts of the lip and pal- problems. The Denver Developmental Scales ate, ectrodactyly of the hands and feet, and yielded an intelligence quotient of 100 at 14 generalized abnormalities in skin pigmenta- months of age. tion. The association of ectodermal changes, Examination of the head and neck revealed ectrodactyly, and oralfacial clefting has been unilateral complete cleft of the lip and palate. well documented in the EEC syndrome (ec- There was mild hypoplasia of the right exter- trodactyly, ectodermal dysplasia, and clefting nal ear (Figure 1). syndrome). However, this patient clearly does Examination of the skin revealed a peculiar not fall into this classification. generalized pattern of hypopigmentation over the entire body, including the head, neck, and Clinical findings face. On the dorsum, the pigmentation as- The child was the product of a full-term, sumed a swirling pattern. -

Nevus Depigmentosus
Journal of Dermatology & Cosmetology Commentary Open Access Nevus depigmentosus Introduction Volume 1 Issue 1 - 2017 Nevus Depigmentosus (nevus achromicus) is a rare congenital pigmentary disorder. It is a depigmentation problem in skin which can Hayk S Arakelyan be easily differentiated from vitiligo. Nevus anemic us is a congenital General Medicine and Clinical Research, Armenian University of vascular anomaly that presents clinically as a hypo pigmented macule Integrative Medicine, Armenia or patch. Correspondence: Hayk S Arakelyan, Doctor of Medical The pathogenesis of ND is not fully understood. It is believed Sciences, PhD, Senior Expert of Interactive Clinical to be due to a functional defect of melanocytes with morphological Pharmacology, Drug Safety, Treatment Tactics, General Medicine abnormalities of melanosomes. It is also said to be a form of cutaneous and Clinical Research. Armenian University of Integrative mosaicism wherein an altered clone of melanocyte have a decreased Medicine, Armenia, Tel (37491)-40-94-97, Email [email protected] ability to synthesize melanin and transport to keratinocytes. Received: March 28, 2017 | Published: April 04, 2017 It can be found anywhere on the body but commonly it is seen on the trunk, neck, face, and proximal part of the extremities. Clinically, three types have been described: Localized Segmental, and Linear or Whorled. Localized variant is the most common compared to the others. It is a single well circumscribed lesion with serrated Acknowledgements borders. Segmental variant is larger in size and shape and also referred to as “segmental de-pigmentation disorder” with a sharp midline None. demarcation. Linear/whorled/systematized type may be extensive and have cutaneous lesions that overlap with HOI.( hypomelanosis of Ito ) Conflict of interest The systematized variant is very rare and may have extra cutaneous The author declares no conflict of interest. -

Laser Treatment for Pigmentation
Laser treatment for pigmentation Sunspots and freckles In lesions such as solar lentigines (sun induced age spots), lentigo simplex and ephelides (freckles) the pigment (melanin) is in the top layers of the skin. Many lasers that selectively target melanin or simply remove the top layers will lead to improvement. One to two treatments will be necessary. There are many non-laser treatment approaches to treat such spots. However, if laser therapy is chosen, there are many different types of laser that can be used including Q-switched lasers [Q switched (QS) alexandrite, QS ruby (694nm)], long-pulsed, fractionated thulium (1927nm) and ablative lasers. IPL (filter 500-600nm) can also be very effective. However, it is common to see the pigmentation return over time. Treatments need to be avoided if the skin is tanned because this greatly increases the risk of complications. Seborrhoeic warts and dermatosis papulosa nigra Some conditions that present as dark spots are in fact wart-like and sit on the surface of the skin such as seborhoeic keratoses and dermatosis papulosa nigra and epidermal naevi. These conditions require physical removal. This is most commonly treated with a curette if thick or with fine wire diathermy particularly for the dermatosis papulosa nigra. Ablative lasers may also be used including CO2 in combination with a curette or an erbium YAG laser which reliably gives the best results. These lesions have a tendency to return over a number of years and maintenance treatments may be needed. Pigmented birth marks – Becker’s naevus Current lasers are unable to remove pigmented birthmarks without scarring. -

Dermatopathology
Dermatopathology Clay Cockerell • Martin C. Mihm Jr. • Brian J. Hall Cary Chisholm • Chad Jessup • Margaret Merola With contributions from: Jerad M. Gardner • Talley Whang Dermatopathology Clinicopathological Correlations Clay Cockerell Cary Chisholm Department of Dermatology Department of Pathology and Dermatopathology University of Texas Southwestern Medical Center Central Texas Pathology Laboratory Dallas , TX Waco , TX USA USA Martin C. Mihm Jr. Chad Jessup Department of Dermatology Department of Dermatology Brigham and Women’s Hospital Tufts Medical Center Boston , MA Boston , MA USA USA Brian J. Hall Margaret Merola Department of Dermatology Department of Pathology University of Texas Southwestern Medical Center Brigham and Women’s Hospital Dallas , TX Boston , MA USA USA With contributions from: Jerad M. Gardner Talley Whang Department of Pathology and Dermatology Harvard Vanguard Medical Associates University of Arkansas for Medical Sciences Boston, MA Little Rock, AR USA USA ISBN 978-1-4471-5447-1 ISBN 978-1-4471-5448-8 (eBook) DOI 10.1007/978-1-4471-5448-8 Springer London Heidelberg New York Dordrecht Library of Congress Control Number: 2013956345 © Springer-Verlag London 2014 This work is subject to copyright. All rights are reserved by the Publisher, whether the whole or part of the material is concerned, specifi cally the rights of translation, reprinting, reuse of illustrations, recitation, broadcasting, reproduction on microfi lms or in any other physical way, and transmission or information storage and retrieval, electronic adaptation, computer software, or by similar or dissimilar methodology now known or hereafter developed. Exempted from this legal reservation are brief excerpts in connection with reviews or scholarly analysis or material supplied specifi cally for the purpose of being entered and executed on a computer system, for exclusive use by the purchaser of the work. -
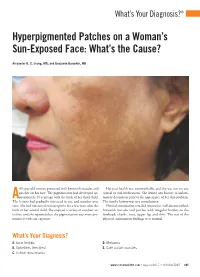
Hyperpigmented Patches on a Woman's Sun-Exposed Face
What’s Your Diagnosis?® Hyperpigmented Patches on a Woman’s Sun-Exposed Face: What’s the Cause? Alexander K. C. Leung, MD, and Benjamin Barankin, MD 45-year-old woman presented with brownish macules and Her past health was unremarkable, and she was not on any patches on her face. The pigmentation had developed ap- topical or oral medications. She denied any history of inflam- A proximately 10 years ago with the birth of her third child. matory dermatosis prior to the appearance of her skin problem. The lesions had gradually increased in size and number over The family history was not contributory. time. She had taken oral contraceptives for a few years after the Physical examination revealed symmetric, well-circumscribed, birth of her second child. She enjoyed a variety of outdoor ac- brownish macules and patches with irregular borders on the tivities, and she reported that the pigmentation was more pro- forehead, cheeks, nose, upper lip, and chin. The rest of the nounced with sun exposure. physical examination findings were normal. What’s Your Diagnosis? A. Solar lentigo D. Melasma B. Ephelides (freckles) E. Café au lait macules C. Actinic dyschromia www.consultant360.com • August 2017 • CONSULTANT 485 What’s Your Diagnosis?® Answer: Melasma A diagnosis of melasma was made. Wood lamp examination basement membrane disruption and dermal changes, indepen- showed accentuation of pigmentation suggestive of epidermal dent of UV radiation.1,17 pigmentation. The patient was treated with a series of trichlo- roacetic acid chemical peels, as well as a topical azelaic acid and HISTOPATHOLOGY a retinoid-hydroquinone-steroid (modified Kligman) formula- Three histologic patterns of pigmentation have been described: tion with significant, albeit incomplete, improvement. -

Cutaneous Manifestation of Β‑Thalassemic Patients Mohamed A
[Downloaded free from http://www.mmj.eg.net on Thursday, January 14, 2021, IP: 156.204.184.20] Original article 267 Cutaneous manifestation of β‑thalassemic patients Mohamed A. Gaber, Marwa Galal Departement of Dermatology and Venereology, Objective Menoufia University, Menoufia, Egypt The aim was to study the prevalence of common dermatological problems in patients with Correspondence to Marwa Galal, MBBCh, β‑thalassemia major to help rapid treatment and prevent complications. Shiben Elkom, Menoufia, Background Egypt β‑Thalassemia major affects multiple organs and is associated with considerable morbidity Tel: +20 100 276 8385; Postal code: 32511; and mortality. In β‑thalassemia, a wide spectrum of skin diseases was identified, which were e‑mail: [email protected] caused by both the hemoglobin disorder and the complications of treatment. Patients and methods Received 07 August 2018 Revised 10 September 2018 This cross‑sectional study included 105 Egyptian patients (50 female individuals and 55 male Accepted 23 September 2018 individuals) with transfusion‑dependent β‑thalassemia major in the period spanning from June Published 25 March 2020 2017 to February 2018. The study was performed on child and adult patients of β‑thalassemia Menoufia Medical Journal 2020, 33:267–271 who presented to the hematology clinic, Menoufia University hospital. Skin examination of each patient was carried out, and any skin disease present was recorded. Results The main skin disorders that were noticed in decreasing order of frequency were pruritus (34.4%), xerosis (24.8%), urticaria (21.1%), freckles (17.1%), tinea infections (11.6%), pitriasis alba reported in 10.5%, scars (10.5%), hypersensitivity to deferoxamine pump (9.5%), herpes simplex (9.5%), acne vulgaris (8.6%), miliaria (6.7%), contact dermatitis (4.8%).