Toxidromes: What's Your Poison
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-
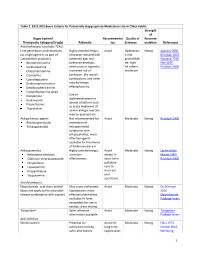
Table 2. 2012 AGS Beers Criteria for Potentially
Table 2. 2012 AGS Beers Criteria for Potentially Inappropriate Medication Use in Older Adults Strength of Organ System/ Recommendat Quality of Recomm Therapeutic Category/Drug(s) Rationale ion Evidence endation References Anticholinergics (excludes TCAs) First-generation antihistamines Highly anticholinergic; Avoid Hydroxyzin Strong Agostini 2001 (as single agent or as part of clearance reduced with e and Boustani 2007 combination products) advanced age, and promethazi Guaiana 2010 Brompheniramine tolerance develops ne: high; Han 2001 Carbinoxamine when used as hypnotic; All others: Rudolph 2008 Chlorpheniramine increased risk of moderate Clemastine confusion, dry mouth, Cyproheptadine constipation, and other Dexbrompheniramine anticholinergic Dexchlorpheniramine effects/toxicity. Diphenhydramine (oral) Doxylamine Use of diphenhydramine in Hydroxyzine special situations such Promethazine as acute treatment of Triprolidine severe allergic reaction may be appropriate. Antiparkinson agents Not recommended for Avoid Moderate Strong Rudolph 2008 Benztropine (oral) prevention of Trihexyphenidyl extrapyramidal symptoms with antipsychotics; more effective agents available for treatment of Parkinson disease. Antispasmodics Highly anticholinergic, Avoid Moderate Strong Lechevallier- Belladonna alkaloids uncertain except in Michel 2005 Clidinium-chlordiazepoxide effectiveness. short-term Rudolph 2008 Dicyclomine palliative Hyoscyamine care to Propantheline decrease Scopolamine oral secretions. Antithrombotics Dipyridamole, oral short-acting* May -

Blockade of Muscarinic Acetylcholine Receptors Facilitates Motivated Behaviour and Rescues a Model of Antipsychotic- Induced Amotivation
www.nature.com/npp ARTICLE Blockade of muscarinic acetylcholine receptors facilitates motivated behaviour and rescues a model of antipsychotic- induced amotivation Jonathan M. Hailwood 1, Christopher J. Heath2, Benjamin U. Phillips1, Trevor W. Robbins1, Lisa M. Saksida3,4 and Timothy J. Bussey1,3,4 Disruptions to motivated behaviour are a highly prevalent and severe symptom in a number of neuropsychiatric and neurodegenerative disorders. Current treatment options for these disorders have little or no effect upon motivational impairments. We assessed the contribution of muscarinic acetylcholine receptors to motivated behaviour in mice, as a novel pharmacological target for motivational impairments. Touchscreen progressive ratio (PR) performance was facilitated by the nonselective muscarinic receptor antagonist scopolamine as well as the more subtype-selective antagonists biperiden (M1) and tropicamide (M4). However, scopolamine and tropicamide also produced increases in non-specific activity levels, whereas biperiden did not. A series of control tests suggests the effects of the mAChR antagonists were sensitive to changes in reward value and not driven by changes in satiety, motor fatigue, appetite or perseveration. Subsequently, a sub-effective dose of biperiden was able to facilitate the effects of amphetamine upon PR performance, suggesting an ability to enhance dopaminergic function. Both biperiden and scopolamine were also able to reverse a haloperidol-induced deficit in PR performance, however only biperiden was able to rescue the deficit in effort-related choice (ERC) performance. Taken together, these data suggest that the M1 mAChR may be a novel target for the pharmacological enhancement of effort exertion and consequent rescue of motivational impairments. Conversely, M4 receptors may inadvertently modulate effort exertion through regulation of general locomotor activity levels. -

Severe Organophosphate Poisoning with Delayed Cholinergic Crisis, Intermediate Syndrome and Organophosphate Induced Delayed Polyneuropathy on Succession
Organophosphate Poisoning… Aklilu A 203 CASE REPORT SEVERE ORGANOPHOSPHATE POISONING WITH DELAYED CHOLINERGIC CRISIS, INTERMEDIATE SYNDROME AND ORGANOPHOSPHATE INDUCED DELAYED POLYNEUROPATHY ON SUCCESSION Aklilu Azazh ABSTRACT Organophosphate compounds are the organic derivatives of Phosphorous containing acids and their effect on neuromuscular junction and Autonomic Synapses is clinically important. After exposure these agents cause acute and sub acute manifestations depending on the type and severity of the agents like Acute Cholinergic Manifestations, Intermediate Syndrome with Nicotinic features and Delayed Central Nervous System Complications. The patient reported here had severe Organophosphate Poisoning with various rare complications on a succession. This is the first report of Organophosphates Poisoning complicated by Intermediate Syndrome and Organophosphate Induced Delayed Polyneuropathy in Ethiopia and it is reported to increase awareness of health care workers on these rare complications of a common problem. INTRODUCTION phosphorylated by the Phosphate end of Organophosphates; then the net result is Organophosphate compounds are the organic accumulation of excessive Acetyl Chlorine with derivatives of Phosphorous containing acids and resultant effect on Muscarinic, Nicotinic and their effect on Neuromuscular Junction and central nervous system (Figure 2). Autonomic synapses is clinically important. In the Neuromuscular Junction Acetylcholine is released Following classical OP poisoning, three well when a nerve impulse reaches -

Appendix A: Potentially Inappropriate Prescriptions (Pips) for Older People (Modified from ‘STOPP/START 2’ O’Mahony Et Al 2014)
Appendix A: Potentially Inappropriate Prescriptions (PIPs) for older people (modified from ‘STOPP/START 2’ O’Mahony et al 2014) Consider holding (or deprescribing - consult with patient): 1. Any drug prescribed without an evidence-based clinical indication 2. Any drug prescribed beyond the recommended duration, where well-defined 3. Any duplicate drug class (optimise monotherapy) Avoid hazardous combinations e.g.: 1. The Triple Whammy: NSAID + ACE/ARB + diuretic in all ≥ 65 year olds (NHS Scotland 2015) 2. Sick Day Rules drugs: Metformin or ACEi/ARB or a diuretic or NSAID in ≥ 65 year olds presenting with dehydration and/or acute kidney injury (AKI) (NHS Scotland 2015) 3. Anticholinergic Burden (ACB): Any additional medicine with anticholinergic properties when already on an Anticholinergic/antimuscarinic (listed overleaf) in > 65 year olds (risk of falls, increased anticholinergic toxicity: confusion, agitation, acute glaucoma, urinary retention, constipation). The following are known to contribute to the ACB: Amantadine Antidepressants, tricyclic: Amitriptyline, Clomipramine, Dosulepin, Doxepin, Imipramine, Nortriptyline, Trimipramine and SSRIs: Fluoxetine, Paroxetine Antihistamines, first generation (sedating): Clemastine, Chlorphenamine, Cyproheptadine, Diphenhydramine/-hydrinate, Hydroxyzine, Promethazine; also Cetirizine, Loratidine Antipsychotics: especially Clozapine, Fluphenazine, Haloperidol, Olanzepine, and phenothiazines e.g. Prochlorperazine, Trifluoperazine Baclofen Carbamazepine Disopyramide Loperamide Oxcarbazepine Pethidine -

Methamphetamine Presentations to an Emergency Department: Management and Complications
Isoardi Katherine (Orcid ID: 0000-0002-1176-7923) Abstract Objective: There is little recent published data characterising methamphetamine intoxication. This study aims to describe the clinical effects, management, complications and disposition of patients with methamphetamine exposure. Methods: This is a retrospective review of patients presenting with methamphetamine intoxication to an Emergency Department in 2016. All presentations were extracted from a relational database and each medical record reviewed. Demographics, clinical features, complications and disposition were extracted. Results: There were 378 presentations of 329 patients (234 males [71%]), median age 31 years (range 16-68 years). The commonest clinical effect was acute behavioural disturbance, occurring in 295 (78%) presentations. This was successfully managed with oral sedation alone in 180 (61%) patients with the remainder receiving parenteral sedation. Other effects included tachycardia in 212 (56%), hypertension in 160 (42%) and hyperthermia in 17 (4%) presentations. No antihypertensives were given. One patient was actively cooled. Complications included 21 (30%) presentations with rhabdomyolysis and 43 (11%) presentations with acute kidney injury. There were two seizures, three intracranial bleeds and one myocardial infarction. The majority of This is the author manuscript accepted for publication and has undergone full peer review but has not been through the copyediting, typesetting, pagination and proofreading process, which may lead to differences between this version and the Version of Record. Please cite this article as doi: 10.1111/1742-6723.13219 This article is protected by copyright. All rights reserved. patients (310 [82%]) were managed solely within the emergency department. The median length of stay was 14 hours. There were 41(11%) mental health admissions. -

Ketamine As a General Anesthesia Adjunct Michaela Wilcox, DNP
Ketamine as a General Anesthesia Adjunct Michaela Wilcox, DNP (c), RN Dept. of Nurse Anesthesia, Moffett & Sanders School of Nursing, Samford University Structured Abstract Background Ketamine is a unique anesthetic agent with both anesthetic and analgesic properties. Ketamine is primarily a N-Methyl-D-Aspartic acid (NMDA) antagonist that also works on glutamine, nicotinic, muscarinic, monoaminergic and opioid receptors. The uses of ketamine are numerous and include treatment of chronic pain, acute pain, depression, as a multimodal pain adjunct, opioid-sparing agent and as an adjunct in enhanced recovery after surgery (ERAS) protocols. A 49-year-old female presented for a lumbar lateral interbody fusion extreme, anterior lumbar spine arthrodesis L3/4 with revision and instrumentation. Based on the surgical need for both sensory and motor nerve monitoring intraoperatively, the anesthetic plan included minimal sevoflurane, succinylcholine for induction and a propofol intravenous (IV) infusion with boluses of ketamine to maintain unconsciousness. A bispectral index (BIS) monitor (Aspect Medical Systems, Natick, MA) was placed on the patient’s forehead prior to induction and utilized intraoperatively to maintain a goal of 40-60. General anesthesia was achieved with fentanyl 100 mcg, lidocaine 100 mg, propofol 200 mg, ketamine 50 mg and succinylcholine 160 mg IV. Laryngoscopy was successfully performed using a McGrath MAC video laryngoscope (Medtronic, Minneapolis, MN). Following induction, a propofol IV infusion was initiated and sevoflurane maintained at 0.3 minimum alveolar concentration. Ketamine 10 mg IV was administered every hour. Upon conclusion of the procedure, the patient was extubated and transported to postoperative recovery unit, where she had no complaints of nausea, vomiting or pain. -

Unintentional Fentanyl Overdoses Among Persons Who Thought They
Morbidity and Mortality Weekly Report Notes from the Field Unintentional Fentanyl Overdoses Among emergency departments; 2) holding a multiagency press Persons Who Thought They Were Snorting conference; 3) conducting media interviews; 4) informing Cocaine — Fresno, California, January 7, 2019 law enforcement, prehospital providers, and the public about Patil Armenian, MD1; Jeffrey D. Whitman, MD2; Adina Badea, PhD2; naloxone distribution and use; 5) educating persons on Whitney Johnson, MD1; Chelsea Drake, MS1; Simranjit Singh Dhillon3; the proper disposal of old or new but unused medications Michelle Rivera3; Nicklaus Brandehoff, MD1; Kara L. Lynch, PhD2 through the Fresno County Department of Behavioral Health/ California Health Collaborative drop-off containers§; and On January 7, 2019, three patients arrived at the Community 6) publicizing the California Central Valley Opioid Safety Regional Medical Center emergency department in Fresno, Coalition webpage,¶ which provides information about California, after snorting (i.e., nasally insufflating) white pow- naloxone and substance use disorders. der they thought was cocaine. One (patient A) was in cardiac On January 12, 2019, a similar drug overdose incident was arrest, and two (patients B and C) had opioid toxidrome reported in Chico, California, in which postmortem toxicol- (miosis, respiratory depression, and depressed mental status) ogy testing for one person confirmed fentanyl (1). Fourteen (Table). After spontaneous circulation was reestablished in other persons at the same event were hospitalized with opioid patient A, he was admitted to the intensive care unit, where toxidrome and later released. They reported thinking they he was pronounced brain-dead 3 days later. Patients B and C were snorting cocaine,** but confirmatory toxicology results responded to naloxone, but repeated dosing was required to are unavailable. -

The Influence of a Muscarinic M1 Receptor Antagonist on Brain Choline Levels in Patients with a Psychotic Disorder and Healthy Controls
MHENS School for Mental Health and Neuroscience The influence of a muscarinic M1 receptor antagonist on brain choline levels in patients with a psychotic disorder and healthy controls. W.A.M. VingerhoetsA,B, G. BakkerA,B, O. BloemenA,C, M. CaanD, J. BooijB, T.A.M.J. van AmelsvoortA. A Department of Psychiatry & Psychology, Maastricht University, Maastricht, The Netherlands.. B Department of Nuclear Medicine, Academic Medical Center, Amsterdam, The Netherlands. C GGZ Centraal, Center for Mental Health Care, Hilversum, The Netherlands D Department of Radiology, Academic Medical Center, Amsterdam, The Netherlands Background • The majority of the patients with a psychotic disorder report cognitive impairments in addition to positive and negative symptoms. • It is well known that the neurotransmitter acetylcholine plays an important role in cognition. • A post-mortem study of chronic schizophrenia patients demonstrated a reduction of up to 75% in the number of the acetylcholine muscarinic M1 receptors (1). • Research has shown that muscarinic cholinergic receptors play a major role in cognitive processes. Objective • To investigate in-vivo whether there are differences in baseline choline levels in the anterior cingulate cortex (ACC) and striatum between recent onset medication-free patients with a psychotic disorder and healthy control subjects. • To investigate in-vivo the influence of a muscarinic antagonist on choline levels in the ACC and striatum in recent onset medication-free patients with Figure 2. Example of a striatal spectrum. a psychotic disorder and healthy control subjects. Results Methods • No significant differences were found in baseline choline levels between the two groups in both the striatum (p=0.336) and the ACC (p=0.479). -

Muscarinic Acetylcholine Receptor
mAChR Muscarinic acetylcholine receptor mAChRs (muscarinic acetylcholine receptors) are acetylcholine receptors that form G protein-receptor complexes in the cell membranes of certainneurons and other cells. They play several roles, including acting as the main end-receptor stimulated by acetylcholine released from postganglionic fibersin the parasympathetic nervous system. mAChRs are named as such because they are more sensitive to muscarine than to nicotine. Their counterparts are nicotinic acetylcholine receptors (nAChRs), receptor ion channels that are also important in the autonomic nervous system. Many drugs and other substances (for example pilocarpineand scopolamine) manipulate these two distinct receptors by acting as selective agonists or antagonists. Acetylcholine (ACh) is a neurotransmitter found extensively in the brain and the autonomic ganglia. www.MedChemExpress.com 1 mAChR Inhibitors & Modulators (+)-Cevimeline hydrochloride hemihydrate (-)-Cevimeline hydrochloride hemihydrate Cat. No.: HY-76772A Cat. No.: HY-76772B Bioactivity: Cevimeline hydrochloride hemihydrate, a novel muscarinic Bioactivity: Cevimeline hydrochloride hemihydrate, a novel muscarinic receptor agonist, is a candidate therapeutic drug for receptor agonist, is a candidate therapeutic drug for xerostomia in Sjogren's syndrome. IC50 value: Target: mAChR xerostomia in Sjogren's syndrome. IC50 value: Target: mAChR The general pharmacol. properties of this drug on the The general pharmacol. properties of this drug on the gastrointestinal, urinary, and reproductive systems and other… gastrointestinal, urinary, and reproductive systems and other… Purity: >98% Purity: >98% Clinical Data: No Development Reported Clinical Data: No Development Reported Size: 10mM x 1mL in DMSO, Size: 10mM x 1mL in DMSO, 1 mg, 5 mg 1 mg, 5 mg AC260584 Aclidinium Bromide Cat. No.: HY-100336 (LAS 34273; LAS-W 330) Cat. -

Approach to the Poisoned Patient
PED-1407 Chocolate to Crystal Methamphetamine to the Cinnamon Challenge - Emergency Approach to the Intoxicated Child BLS 08 / ALS 75 / 1.5 CEU Target Audience: All Pediatric and adolescent ingestions are common reasons for 911 dispatches and emergency department visits. With greater availability of medications and drugs, healthcare professionals need to stay sharp on current trends in medical toxicology. This lecture examines mind altering substances, initial prehospital approach to toxicology and stabilization for transport, poison control center resources, and ultimate emergency department and intensive care management. Pediatric Toxicology Dr. James Burhop Pediatric Emergency Medicine Children’s Hospital of the Kings Daughters Objectives • Epidemiology • History of Poisoning • Review initial assessment of the child with a possible ingestion • General management principles for toxic exposures • Case Based (12 common pediatric cases) • Emerging drugs of abuse • Cathinones, Synthetics, Salvia, Maxy/MCAT, 25I, Kratom Epidemiology • 55 Poison Centers serving 295 million people • 2.3 million exposures in 2011 – 39% are children younger than 3 years – 52% in children younger than 6 years • 1-800-222-1222 2011 Annual report of the American Association of Poison Control Centers Toxic Exposure Surveillance System Introduction • 95% decline in the number of pediatric poisoning deaths since 1960 – child resistant packaging – heightened parental awareness – more sophisticated interventions – poison control centers Epidemiology • Unintentional (1-2 -

A Comparison of Scopolamine and Biperiden As a Rodent Model for Cholinergic Cognitive Impairment
Psychopharmacology (2011) 215:549–566 DOI 10.1007/s00213-011-2171-1 ORIGINAL INVESTIGATION A comparison of scopolamine and biperiden as a rodent model for cholinergic cognitive impairment Inge Klinkenberg & Arjan Blokland Received: 30 June 2010 /Accepted: 9 January 2011 /Published online: 19 February 2011 # The Author(s) 2011. This article is published with open access at Springerlink.com Abstract Keywords Sensorimotor . Motivation . Attention . Rationale The nonselective muscarinic antagonist scopol- Memory. Animal model . Fixed ratio . Progressive ratio . amine hydrobromide (SCOP) is employed as the gold Delayed nonmatching to position . Muscarinic . standard for inducing memory impairments in healthy Acetylcholine humans and animals. However, its use remains controversial due to the wide spectrum of behavioral effects of this drug. Objective The present study investigated whether biperiden Introduction (BIP), a muscarinic m1 receptor antagonist, is to be preferred over SCOP as a pharmacological model for The muscarinic antagonist scopolamine hydrobromide cholinergic memory deficits in rats. This was done by (SCOP) is used as the gold standard for inducing deficits comparing the effects of SCOP and BIP using a battery of in human and animal models of memory dysfunction. operant tasks: fixed ratio (FR5) and progressive ratio Justification for this purpose has been provided by the (PR10) schedules of reinforcement, an attention paradigm cholinergic hypothesis of geriatric memory dysfunction and delayed nonmatching to position task. proposed in the early 1980s by Bartus et al. (1982). The Results SCOP induced diffuse behavioral disruption, which SCOP model is still used extensively for preclinical testing included sensorimotor responding (FR5, 0.3 and 1 mg/kg), of new substances designed to treat cognitive impairment food motivation (PR10, 1 mg/kg), attention (0.3 mg/kg, (e.g., Barak and Weiner 2009; Buccafusco et al. -

Protocol for a Randomised Controlled Trial: Efficacy of Donepezil Against
BMJ Open: first published as 10.1136/bmjopen-2013-003533 on 25 September 2013. Downloaded from Open Access Protocol Protocol for a randomised controlled trial: efficacy of donepezil against psychosis in Parkinson’s disease (EDAP) Hideyuki Sawada, Tomoko Oeda To cite: Sawada H, Oeda T. ABSTRACT ARTICLE SUMMARY Protocol for a randomised Introduction: Psychosis, including hallucinations and controlled trial: efficacy of delusions, is one of the important non-motor problems donepezil against psychosis Strengths and limitations of this study in patients with Parkinson’s disease (PD) and is in Parkinson’s disease ▪ In previous randomised controlled trials for (EDAP). BMJ Open 2013;3: possibly associated with cholinergic neuronal psychosis the efficacy was investigated in patients e003533. doi:10.1136/ degeneration. The EDAP (Efficacy of Donepezil against who presented with psychosis and the primary bmjopen-2013-003533 Psychosis in PD) study will evaluate the efficacy of endpoint was improvement of psychotic symp- donepezil, a brain acetylcholine esterase inhibitor, for toms. By comparison, this study is designed to prevention of psychosis in PD. ▸ Prepublication history for evaluate the prophylactic effect in patients this paper is available online. Methods and analysis: Psychosis is assessed every without current psychosis. Because psychosis To view these files please 4 weeks using the Parkinson Psychosis Questionnaire may be overlooked and underestimated it is visit the journal online (PPQ) and patients with PD whose PPQ-B score assessed using a questionnaire, Parkinson (http://dx.doi.org/10.1136/ (hallucinations) and PPQ-C score (delusions) have Psychosis Questionnaire (PPQ) every 4 weeks. bmjopen-2013-003533). been zero for 8 weeks before enrolment are ▪ The strength of this study is its prospective randomised to two arms: patients receiving donepezil design using the preset definition of psychosis Received 3 July 2013 hydrochloride or patients receiving placebo.