Appendix A: Potentially Inappropriate Prescriptions (Pips) for Older People (Modified from ‘STOPP/START 2’ O’Mahony Et Al 2014)
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-
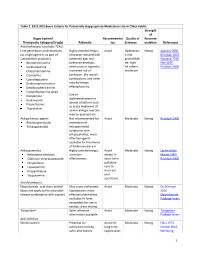
Table 2. 2012 AGS Beers Criteria for Potentially
Table 2. 2012 AGS Beers Criteria for Potentially Inappropriate Medication Use in Older Adults Strength of Organ System/ Recommendat Quality of Recomm Therapeutic Category/Drug(s) Rationale ion Evidence endation References Anticholinergics (excludes TCAs) First-generation antihistamines Highly anticholinergic; Avoid Hydroxyzin Strong Agostini 2001 (as single agent or as part of clearance reduced with e and Boustani 2007 combination products) advanced age, and promethazi Guaiana 2010 Brompheniramine tolerance develops ne: high; Han 2001 Carbinoxamine when used as hypnotic; All others: Rudolph 2008 Chlorpheniramine increased risk of moderate Clemastine confusion, dry mouth, Cyproheptadine constipation, and other Dexbrompheniramine anticholinergic Dexchlorpheniramine effects/toxicity. Diphenhydramine (oral) Doxylamine Use of diphenhydramine in Hydroxyzine special situations such Promethazine as acute treatment of Triprolidine severe allergic reaction may be appropriate. Antiparkinson agents Not recommended for Avoid Moderate Strong Rudolph 2008 Benztropine (oral) prevention of Trihexyphenidyl extrapyramidal symptoms with antipsychotics; more effective agents available for treatment of Parkinson disease. Antispasmodics Highly anticholinergic, Avoid Moderate Strong Lechevallier- Belladonna alkaloids uncertain except in Michel 2005 Clidinium-chlordiazepoxide effectiveness. short-term Rudolph 2008 Dicyclomine palliative Hyoscyamine care to Propantheline decrease Scopolamine oral secretions. Antithrombotics Dipyridamole, oral short-acting* May -

Dosulepin Prescribing
SAFETY BULLETIN: DOSULEPIN PRESCRIBING In December 2007, the Medicines and Healthcare Regulatory Agency (MHRA) issued safety advice around prescribing of dosulepin, related to the narrow margin between therapeutic doses and potentially fatal doses. Nevertheless, dosulepin continues to be prescribed widely. Over eight years after the safety advice was published, prescribing of dosulepin in the Dorset area remains high. In the South West area, Dorset CCG was the highest prescriber of dosulepin for the 2015/16 financial year (3.238% of all antidepressant items). Of the 209 CCGs in the UK, Dorset is the fourteenth highest prescriber of dosulepin, and well above the national average of 2.111%. The following points summarise the reasons that dosulepin is not recommended for prescribing nationally, and in Dorset: Dosulepin has a small margin of safety between the (maximum) therapeutic dose and potentially fatal doses. The NICE guideline on depression in adults recommends that dosulepin should not be prescribed for adults with depression because evidence supporting its tolerability relative to other antidepressants is outweighed by the increased cardiac risk and toxicity in overdose. Dosulepin has also been used ‘off label’ in other indications such as fibromyalgia and neuropathic pain. However the evidence for use in in this way is weak, and is not recommended. The lethal dose of dosulepin is relatively low and can be potentiated by alcohol and other CNS depressants. Dosulepin overdose is associated with high mortality and can occur rapidly, even before hospital treatment can be received. Onset of toxicity occurs within 4-6 hours. Every year, up to 200 people in England and Wales fatally overdose with dosulepin. -

Dose Equivalents of Antidepressants Evidence-Based Recommendations
Journal of Affective Disorders 180 (2015) 179–184 Contents lists available at ScienceDirect Journal of Affective Disorders journal homepage: www.elsevier.com/locate/jad Research report Dose equivalents of antidepressants: Evidence-based recommendations from randomized controlled trials Yu Hayasaka a,n, Marianna Purgato b, Laura R Magni c, Yusuke Ogawa a, Nozomi Takeshima a, Andrea Cipriani b,d, Corrado Barbui b, Stefan Leucht e, Toshi A Furukawa a a Department of Health Promotion and Human Behavior, Kyoto University Graduate School of Medicine/School of Public Health, Yoshida Konoe-cho, Sakyo- ku, Kyoto 606-8501, Japan b Department of Public Health and Community Medicine, Section of Psychiatry, University of Verona, Policlinico “G.B.Rossi”, Pzz.le L.A. Scuro, 10, Verona 37134, Italy c Psychiatric Unit, Istituto di Ricovero e Cura a Carattere Scientifico, Centro San Giovanni di Dio, Fatebenefratelli, Brescia, Italy d Department of Psychiatry, University of Oxford, Oxford, UK e Department of Psychiatry and Psychotherapy, Technische Universität München, Klinikum rechts der Isar, Ismaningerstr. 22, 81675 Munich, Germany article info abstract Article history: Background: Dose equivalence of antidepressants is critically important for clinical practice and for Received 4 February 2015 research. There are several methods to define and calculate dose equivalence but for antidepressants, Received in revised form only daily defined dose and consensus methods have been applied to date. The purpose of the present 10 March 2015 study is to examine dose equivalence of antidepressants by a less arbitrary and more systematic method. Accepted 12 March 2015 Methods: We used data from all randomized, double-blind, flexible-dose trials comparing fluoxetine or Available online 31 March 2015 paroxetine as standard drugs with any other active antidepressants as monotherapy in the acute phase Keywords: treatment of unipolar depression. -

Chlorphenamine Maleate)
Package leaflet: Information for the patient Chlorphenamine 10 mg/ml Solution for Injection (Chlorphenamine Maleate) Read all of this leaflet carefully before you start taking this medicine because it contains important information for you. − Keep this leaflet. You may need to read it again. − If you have any further questions, ask your doctor or nurse. − If you get any side effects, talk to your doctor or nurse. This includes any possible side effects not listed in this leaflet. See section 4. What is in this leaflet: 1. What Chlorphenamine is and what it is used for 2. What you need to know before Chlorphenamine is given 3. How Chlorphenamine is given 4. Possible side effects 5. How to store Chlorphenamine 6. Contents of the pack and other information 1. What Chlorphenamine is and what it is used for Chlorphenamine 10 mg/ml Solution for Injection contains the active ingredient chlorphenamine maleate which is an antihistamine. Chlorphenamine is indicated in adults and children (aged 1 month to 18 years) for the treatment of acute allergic reactions. These medicines inhibit the release of histamine into the body that occurs during an allergic reaction. This product relieves some of the main symptoms of a severe allergic reaction. 2. What you need to know before Chlorphenamine is given You MUST NOT be given Chlorphenamine: if you are allergic to chlorphenamine maleate or any of the other ingredients of this medicine (listed in section 6) if you have had monoamine oxidase inhibitor (MAOI) antidepressive treatment within the past 14 days. Warnings and precautions Talk to your doctor or nurse before you are given this medicine if you: are being treated for an overactive thyroid or enlarged prostate gland have epilepsy, raised blood pressure within the eye or glaucoma, very high blood pressure, heart, liver, asthma or other chest diseases. -

Prescribing Trends of Antihistamines in the Outpatient Setting in Al-Kharj
Prescribing Trends of Antihistamines in the Outpatient Setting in Al-Kharj Nehad J. Ahmed1*, Menshawy A. Menshawy2 1Department of Clinical Pharmacy, College of Pharmacy, Prince Sattam Bin Abdulaziz University, Al-Kharj, Saudi Arabia, 2Department of Medicinal chemistry, College of Pharmacy, Prince Sattam Bin Abdulaziz University, Al-Kharj, Saudi Arabia Abstract Aim: This study aims to illustrate the prescribing trends of antihistamines in the outpatient setting in Al-Kharj. Materials and Methods: This is a retrospective study that included the evaluation of antihistamines in the outpatient setting in a public hospital in Al-Kharj. The data were collected from the pharmacy-based computer system. Results: The total number of prescriptions that included antihistamines was 799. Most of the prescribed ORIGINAL ARTICLE ARTICLE ORIGINAL antihistamines were first-generation sedating antihistamines (chlorphenamine and diphenhydramine) (66.33%). About 63.20% of the prescribed antihistamines included chlorpheniramine followed by cetirizine (19.27%) and loratadine (14.39%). Conclusion: Antihistamines were prescribed commonly in the outpatient setting mainly first-generation sedating antihistamines. It is recommended to increase the awareness of health- care providers about the efficacy and the side effects of antihistamines and to encourage them to use these agents wisely. Key words: Antihistamines, outpatient, prescribing, trends INTRODUCTION In addition, antihistamines have been classified as sedating antihistamines (first-generation antihistamines) and non- ntihistamines are used in the sedating antihistamines (second-generation antihistamines).[4] management of allergic conditions. Sedating antihistamines include chlorphenamine, clemastine, They are useful for treating the itching hydroxyzine, alimemazine, cyproheptadine, promethazine, A [1] and ketotifen.[4] Non-sedating antihistamines include that results from the release of histamine. -

Ketamine As a General Anesthesia Adjunct Michaela Wilcox, DNP
Ketamine as a General Anesthesia Adjunct Michaela Wilcox, DNP (c), RN Dept. of Nurse Anesthesia, Moffett & Sanders School of Nursing, Samford University Structured Abstract Background Ketamine is a unique anesthetic agent with both anesthetic and analgesic properties. Ketamine is primarily a N-Methyl-D-Aspartic acid (NMDA) antagonist that also works on glutamine, nicotinic, muscarinic, monoaminergic and opioid receptors. The uses of ketamine are numerous and include treatment of chronic pain, acute pain, depression, as a multimodal pain adjunct, opioid-sparing agent and as an adjunct in enhanced recovery after surgery (ERAS) protocols. A 49-year-old female presented for a lumbar lateral interbody fusion extreme, anterior lumbar spine arthrodesis L3/4 with revision and instrumentation. Based on the surgical need for both sensory and motor nerve monitoring intraoperatively, the anesthetic plan included minimal sevoflurane, succinylcholine for induction and a propofol intravenous (IV) infusion with boluses of ketamine to maintain unconsciousness. A bispectral index (BIS) monitor (Aspect Medical Systems, Natick, MA) was placed on the patient’s forehead prior to induction and utilized intraoperatively to maintain a goal of 40-60. General anesthesia was achieved with fentanyl 100 mcg, lidocaine 100 mg, propofol 200 mg, ketamine 50 mg and succinylcholine 160 mg IV. Laryngoscopy was successfully performed using a McGrath MAC video laryngoscope (Medtronic, Minneapolis, MN). Following induction, a propofol IV infusion was initiated and sevoflurane maintained at 0.3 minimum alveolar concentration. Ketamine 10 mg IV was administered every hour. Upon conclusion of the procedure, the patient was extubated and transported to postoperative recovery unit, where she had no complaints of nausea, vomiting or pain. -

Inhibitory Effect of Eslicarbazepine Acetate and S-Licarbazepine on 2 Nav1.5 Channels
bioRxiv preprint doi: https://doi.org/10.1101/2020.04.24.059188; this version posted August 14, 2020. The copyright holder for this preprint (which was not certified by peer review) is the author/funder, who has granted bioRxiv a license to display the preprint in perpetuity. It is made available under aCC-BY 4.0 International license. 1 Inhibitory effect of eslicarbazepine acetate and S-licarbazepine on 2 Nav1.5 channels 3 Theresa K. Leslie1, Lotte Brückner 1, Sangeeta Chawla1,2, William J. Brackenbury1,2* 4 1Department of Biology, University of York, Heslington, York, YO10 5DD, UK 5 2York Biomedical Research Institute, University of York, Heslington, York, YO10 5DD, UK 6 * Correspondence: Dr William J. Brackenbury, Department of Biology and York Biomedical 7 Research Institute, University of York, Wentworth Way, Heslington, York YO10 5DD, UK. Email: 8 [email protected]. Tel: +44 1904 328284. 9 Keywords: Anticonvulsant, cancer, epilepsy, eslicarbazepine acetate, Nav1.5, S-licarbazepine, 10 voltage-gated Na+ channel. 11 Abstract 12 Eslicarbazepine acetate (ESL) is a dibenzazepine anticonvulsant approved as adjunctive treatment for 13 partial-onset epileptic seizures. Following first pass hydrolysis of ESL, S-licarbazepine (S-Lic) 14 represents around 95 % of circulating active metabolites. S-Lic is the main enantiomer responsible 15 for anticonvulsant activity and this is proposed to be through the blockade of voltage-gated Na+ 16 channels (VGSCs). ESL and S-Lic both have a voltage-dependent inhibitory effect on the Na+ current 17 in N1E-115 neuroblastoma cells expressing neuronal VGSC subtypes including Nav1.1, Nav1.2, 18 Nav1.3, Nav1.6 and Nav1.7. -

Commonly Prescribed Psychotropic Medications
COMMONLY PRESCRIBED PSYCHOTROPIC MEDICATIONS NAME Generic (Trade) DOSAGE KEY CLINICAL INFORMATION Antidepressant Medications* Start: IR-100 mg bid X 4d then ↑ to 100 mg tid; SR-150 mg qam X 4d then ↑ to 150 mg Contraindicated in seizure disorder because it decreases seizure threshold; stimulating; not good for treating anxiety disorders; second Bupropion (Wellbutrin) bid; XL-150 mg qam X 4d, then ↑ to 300 mg qam. Range: 300-450 mg/d. line TX for ADHD; abuse potential. ¢ (IR/SR), $ (XL) Citalopram (Celexa) Start: 10-20 mg qday,↑10-20 mg q4-7d to 30-40 mg qday. Range: 20-60 mg/d. Best tolerated of SSRIs; very few and limited CYP 450 interactions; good choice for anxious pt. ¢ Duloxetine (Cymbalta) Start: 30 mg qday X 1 wk, then ↑ to 60 mg qday. Range: 60-120 mg/d. More GI side effects than SSRIs; tx neuropathic pain; need to monitor BP; 2nd line tx for ADHD. $ Escitalopram (Lexapro) Start: 5 mg qday X 4-7d then ↑ to 10 mg qday. Range 10-30 mg/d (3X potent vs. Celexa). Best tolerated of SSRIs, very few and limited CYP 450 interactions. Good choice for anxious pt. $ Fluoxetine (Prozac) Start: 10 mg qam X 4-7d then ↑ to 20 mg qday. Range: 20-60 mg/d. More activating than other SSRIs; long half-life reduces withdrawal (t ½ = 4-6 d). ¢ Mirtazapine (Remeron) Start: 15 mg qhs. X 4-7d then ↑ to 30 mg qhs. Range: 30-60 mg/qhs. Sedating and appetite promoting; Neutropenia risk (1 in 1000) so avoid in immunosupressed patients. -

The In¯Uence of Medication on Erectile Function
International Journal of Impotence Research (1997) 9, 17±26 ß 1997 Stockton Press All rights reserved 0955-9930/97 $12.00 The in¯uence of medication on erectile function W Meinhardt1, RF Kropman2, P Vermeij3, AAB Lycklama aÁ Nijeholt4 and J Zwartendijk4 1Department of Urology, Netherlands Cancer Institute/Antoni van Leeuwenhoek Hospital, Plesmanlaan 121, 1066 CX Amsterdam, The Netherlands; 2Department of Urology, Leyenburg Hospital, Leyweg 275, 2545 CH The Hague, The Netherlands; 3Pharmacy; and 4Department of Urology, Leiden University Hospital, P.O. Box 9600, 2300 RC Leiden, The Netherlands Keywords: impotence; side-effect; antipsychotic; antihypertensive; physiology; erectile function Introduction stopped their antihypertensive treatment over a ®ve year period, because of side-effects on sexual function.5 In the drug registration procedures sexual Several physiological mechanisms are involved in function is not a major issue. This means that erectile function. A negative in¯uence of prescrip- knowledge of the problem is mainly dependent on tion-drugs on these mechanisms will not always case reports and the lists from side effect registries.6±8 come to the attention of the clinician, whereas a Another way of looking at the problem is drug causing priapism will rarely escape the atten- combining available data on mechanisms of action tion. of drugs with the knowledge of the physiological When erectile function is in¯uenced in a negative mechanisms involved in erectile function. The way compensation may occur. For example, age- advantage of this approach is that remedies may related penile sensory disorders may be compen- evolve from it. sated for by extra stimulation.1 Diminished in¯ux of In this paper we will discuss the subject in the blood will lead to a slower onset of the erection, but following order: may be accepted. -

(Antimuscarinic) Drugs?
© July - August 2018 How well do you know your anticholinergic (antimuscarinic) drugs? nticholinergic drugs, prescribed for a variety of clini- Acal conditions, are amongst the most frequently used prescription drugs in BC (Table 1). Also referred to as “an- timuscarinics,” such drugs specifically block muscarinic receptors for acetylcholine (ACh).1 Muscarinic ACh recep- tors are important in the parasympathetic nervous system that governs heart rate, exocrine glands, smooth muscles, clude drugs whose active metabolites are potent- as well as brain function. In contrast, nicotinic ACh recep- ly antimuscarinic,5 or which often cause typical tors stimulate contraction of striated muscles. This Letter is AC adverse effects such as dry mouth or urinary intended to remind clinicians of commonly used drugs that retention.6 People taking antihistamines, antide- have anticholinergic (AC), or technically, antimuscarinic pressants, antipsychotics, opioids, antimuscarinic properties, and of their potential adverse effects. inhalers, or many other drugs need to know that Beneficial and harmful effects of anticholinergic drugs have blockade of ACh receptors can cause bothersome been known for centuries. In Homer’s Odyssey, the nymph or even dangerous adverse effects (Table 3). pharmacologist Circe utilized central effects of atropinics Subtle and not-so-subtle toxicity in the common plant jimson weed (Datura stramonium) to cause delusions in the crew of Odysseus. Believing they Students often learn the adverse effects of anticho- had been turned into pigs, they could be herded.2 linergics from a mnemonic, e.g.: “Blind as a bat, Sometimes a drug is recommended specifically for its an- mad as a hatter, red as a beet, hot as a hare, dry as ticholinergic potency. -

Pain Management 101
PAIN MANAGEMENT 101 By: Vicki McCulloch RN, NP & DeAnna Looper RN, CHPN, CHPCA Expect more from us. We do. Objectives • Identify a step-wise approach to pain management. • Identify the WHO Pain Ladder. • Identify non-pharmacological pain control measures. • Identify adjuvant treatment measures. • Identify common myths and truths • Identify common side effects and treatment options. Expect more from us. We do. Pain Management Principles • Use Multi-Treatment and Multi-Discipline Approach • Combine opioids with non-opioid medications • Non-pharmaceutical approaches • Include family and caregiver in planning • Include the patient! • Coordinate with facility • Coordinate with all providers- • Primary Care Provider • Nursing Home Physician • Hospice IDG Members Expect more from us. We do. Utilize the WHO Ladder World Health Organization • (WHO) “analgesic ladder” • Follow the steps as indicated. • Determine if adjuvants are necessary. Expect more from us. We do. WHO Pain Ladder STEP 3 “Strong” opioid for severe pain +/- non-opioid +/- adjuvant STEP 2 “Mild” opioid for mild- moderate pain +/- non- opioid +/- adjuvant STEP 1 Non-opioid + / - adjuvant Expect more from us. We do. Step 1-Mild Pain NON-OPIOID MEDICATION OPTIONS • Acetaminophen (Tylenol)-(Paracetamol)-(Panadol) • Non-steroidal anti-inflammatory drugs (NSAIDs) Traditional NSAIDS Ibuprofen-(Motrin) Aspirin-(Bayer) Naproxen- (Aleve) Nabumetone-(Relafen) Cox-2 Inhibitors Celecoxib-(Celebrex) Rofecoxib-(Vioxx) Valdecoxib-(Bextra) Expect more from us. We do. Adjuvants • Antidepressants -

Headache in Primary Care *
HeadacHe IN PRIMARY CARE * Dr Neil Whittaker - GP, Nelson Key Advisers: Dr Alistair Dunn - GP, Whangarei Dr Alan Wright - Neurologist, Dunedin Expert Reviewer: Every headache presentation is unique and challenging, requiring a flexible and individualised approach to headache management. - Most headaches are benign primary headaches - A few headaches are secondary to underlying pathology, which may be life threatening Primary headaches can be difficult to diagnose and manage. People, who experience severe or recurrent primary headache, can be subject to significant social, financial and disability burden. We cannot cover all the issues associated with headache presentation in primary care; instead, our focus is on assisting clinicians to: - Recognise presentations of secondary headaches - Effectively diagnose primary headaches - Manage primary headaches, in particular tension-type headache, migraine and cluster headache - Avoid, recognise and manage medication overuse headache 10 I BPJ I Issue 7 www.bpac.org.nz keyword: “Headache” DIAGNOSIS OF HEADACHE IN PRIMARY CARE The keys to headache diagnosis in primary care are: - Ensuring occasional presentations of secondary headache do not escape notice - Differentiating between the causes of primary headache - Addressing patient concerns about serious pathology RECOGNISE SERIOUS SECONDARY HEADACHES BY BEING ALERT FOR RED FLAGS AND PERFORMING FUNDOSCOPY Although primary care clinicians worry about Red Flags in headache presentation missing serious secondary headaches, most Red Flags in headache presentation include: people presenting with secondary headache will have alerting clinical features. These Age clinical features, red flags, are not highly - Over 50 years at onset of new headache specific but do alert clinicians to the need for - Under 10 years at onset particular care in the history, examination and Characteristics investigation.