Cleft Lip and Palate (Let's Talk About... Pediatric
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Angina Bullosa Haemorrhagica (Oral Blood Blister) (PDF)
Patient Information Maxillo-facial Angina Bullosa Haemorrhagica (Oral Blood Blister) What is Angina Bullosa Haemorrhagica? Angina Bullosa Hemorrhagica (ABH) is a condition where an often painful, but benign blood-filled blister suddenly develops in the mouth. The blisters are generally not due to a blood clotting disorder or any other medical disorder. It is a fairly common, sudden onset and benign blood blistering oral (mouth) disorder. It mainly affects people over 45 years and both males and females are equally affected. Usually there is no family history of the condition. It may be associated with Type 2 Diabetes, a family history of diabetes or Hyperglycaemia. What are the signs and symptoms of ABH? The first indication is a stinging pain or burning sensation just before the appearance of a blood blister The blisters last only a few minutes and then spontaneously rupture (burst), leaving a shallow ulcer that heals without scarring, discomfort or pain They can reach an average size of one to three centimetres in diameter The Soft Palate (back of the mouth) is the most affected site If they occur on the palate and are relatively big, they may need to be de-roofed (cut and drained) to ease the sensation of choking Patient Information Occasionally blisters can occur in the buccal mucosa (cheek) and tongue Approximately one third of the patients have blood blisters in more than one location. What are the causes of ABH? More than 50% of cases are related to minor trauma caused by: hot foods, restorative dentistry (fillings, crowns etc) or Periodontal Therapy (treatment of gum disease). -

Vestibule Lingual Frenulum Tongue Hyoid Bone Trachea (A) Soft Palate
Mouth (oral cavity) Parotid gland Tongue Sublingual gland Salivary Submandibular glands gland Esophagus Pharynx Stomach Pancreas (Spleen) Liver Gallbladder Transverse colon Duodenum Descending colon Small Jejunum Ascending colon intestine Ileum Large Cecum intestine Sigmoid colon Rectum Appendix Anus Anal canal © 2018 Pearson Education, Inc. 1 Nasopharynx Hard palate Soft palate Oral cavity Uvula Lips (labia) Palatine tonsil Vestibule Lingual tonsil Oropharynx Lingual frenulum Epiglottis Tongue Laryngopharynx Hyoid bone Esophagus Trachea (a) © 2018 Pearson Education, Inc. 2 Upper lip Gingivae Hard palate (gums) Soft palate Uvula Palatine tonsil Oropharynx Tongue (b) © 2018 Pearson Education, Inc. 3 Nasopharynx Hard palate Soft palate Oral cavity Uvula Lips (labia) Palatine tonsil Vestibule Lingual tonsil Oropharynx Lingual frenulum Epiglottis Tongue Laryngopharynx Hyoid bone Esophagus Trachea (a) © 2018 Pearson Education, Inc. 4 Visceral peritoneum Intrinsic nerve plexuses • Myenteric nerve plexus • Submucosal nerve plexus Submucosal glands Mucosa • Surface epithelium • Lamina propria • Muscle layer Submucosa Muscularis externa • Longitudinal muscle layer • Circular muscle layer Serosa (visceral peritoneum) Nerve Gland in Lumen Artery mucosa Mesentery Vein Duct oF gland Lymphoid tissue outside alimentary canal © 2018 Pearson Education, Inc. 5 Diaphragm Falciform ligament Lesser Liver omentum Spleen Pancreas Gallbladder Stomach Duodenum Visceral peritoneum Transverse colon Greater omentum Mesenteries Parietal peritoneum Small intestine Peritoneal cavity Uterus Large intestine Cecum Rectum Anus Urinary bladder (a) (b) © 2018 Pearson Education, Inc. 6 Cardia Fundus Esophagus Muscularis Serosa externa • Longitudinal layer • Circular layer • Oblique layer Body Lesser Rugae curvature of Pylorus mucosa Greater curvature Duodenum Pyloric Pyloric sphincter antrum (a) (valve) © 2018 Pearson Education, Inc. 7 Fundus Body Rugae of mucosa Pyloric Pyloric (b) sphincter antrum © 2018 Pearson Education, Inc. -

Head and Neck
DEFINITION OF ANATOMIC SITES WITHIN THE HEAD AND NECK adapted from the Summary Staging Guide 1977 published by the SEER Program, and the AJCC Cancer Staging Manual Fifth Edition published by the American Joint Committee on Cancer Staging. Note: Not all sites in the lip, oral cavity, pharynx and salivary glands are listed below. All sites to which a Summary Stage scheme applies are listed at the begining of the scheme. ORAL CAVITY AND ORAL PHARYNX (in ICD-O-3 sequence) The oral cavity extends from the skin-vermilion junction of the lips to the junction of the hard and soft palate above and to the line of circumvallate papillae below. The oral pharynx (oropharynx) is that portion of the continuity of the pharynx extending from the plane of the inferior surface of the soft palate to the plane of the superior surface of the hyoid bone (or floor of the vallecula) and includes the base of tongue, inferior surface of the soft palate and the uvula, the anterior and posterior tonsillar pillars, the glossotonsillar sulci, the pharyngeal tonsils, and the lateral and posterior walls. The oral cavity and oral pharynx are divided into the following specific areas: LIPS (C00._; vermilion surface, mucosal lip, labial mucosa) upper and lower, form the upper and lower anterior wall of the oral cavity. They consist of an exposed surface of modified epider- mis beginning at the junction of the vermilion border with the skin and including only the vermilion surface or that portion of the lip that comes into contact with the opposing lip. -

Cleft Palate/Lip
CLEFT PALATE/LIP WHAT IS A CLEFT? A cleft is a separation in the skin, tissue lining of the mouth, muscle, and bone that is normally fused together; however, no structures are missing. Clefts can be either unilateral (one side) or bilateral (both sides) and may include the lip, soft palate and/or hard palate or any of the structures in isolation. TYPES OF CLEFTS Cleft Lip – separation in the lip and may include the bottom of the nose Cleft Palate – separation in the hard palate and/or soft palate Submucous Cleft – separation in the muscle of the soft palate with the tissue lining of the mouth intact. Often, it is not easily viewed. WHEN DID CLEFTING HAPPEN? During the 4th week of fetal development, the primary palate (line from nostril to upper lip and mucosa behind upper teeth) fuse together. By the 8th week, the tongue drops in the mouth and the secondary palate (hard palate and soft palate) fuse together with the nasal septum. By the 12th week, if the process is not complete, a cleft (separation) will develop. WHAT CAUSED MY CHILD’S CLEFT? The exact cause is not known but theories include: Low intake of Folic Acid (Vitamin B) Large intake of Vitamin A Genetic disposition Syndromes or Sequences (Pierre Robin, Treacher Collins) Drugs, alcohol, medication, and smoking CLEFT PALATE MANAGEMENT You and your child will be in contact with many different healthcare professionals who need to work together. Every case is individualized, therefore your child will need a thorough assessment to the appropriate treatment plan. -

Oral-Peripheral Examination
Oral-Peripheral Examination SCSD 632 Week 2 Phonological Disorders 3. General Cautions Relating to the Oral-Peripheral Examination a. Use your initial impressions of the child’s speech and facial characteristics to guide your examination. b. Remember that one facial or oral abnormality may be associated with others. c. If you suspect an abnormality in structure or function you may want to get a second opinion from a more experienced SLP or an SLP who specializes in craniofacial or motor-speech disorders before initiating referrals to other professionals. d. Remember that in the case of most “special” conditions, it is not your role to diagnose the condition; rather it is your responsibility to make appropriate referrals. e. Remember that in Canada you cannot usually refer directly to a specialist; be sensitive in your approach to the family doctor or referring physician. f. Be sensitive about how you present your results to parents, especially when you are recommending referrals to other professionals. The parents have the right to refuse the referral. g. An oral-peripheral examination is at least as important for your young patients as for your older patients. 1 Oral-Peripheral Examination | Oral and Facial Structure z Face z Lips z Teeth z Hard palate z Soft palate z Tongue When you perform an oral-peripheral examination what are you looking for when you examine each of the following structures? a. Facial Characteristics: overall expression and appearance, size, shape and overall symmetry of the head and facial structures b. Teeth: maxillary central incisors should extend just slightly over the mandibular central incisors; the lower canine tooth should be half-way between the upper lateral incisor and the upper canine tooth c. -

The Effectiveness of Frenotomy on Speech in Adults
applied sciences Article The Effectiveness of Frenotomy on Speech in Adults Anna Lichnowska * and Marcin Kozakiewicz Department of Maxillofacial Surgery, Medical University of Lodz, 113th S. Zeromskiego,˙ 90-549 Lodz, Poland; [email protected] * Correspondence: [email protected] Featured Application: The impact of tongue frenulum status in malocclusion is neglected in adults. Orthodontic and/or orthognathic treatment leads to a dental and visual correction of the face but leaves a functional deficiency in the form of a speech disorder. This study highlights the important functional role of the tongue frenulum not only in children but also in adult patients. Evaluation and correction of ankyloglossia should be part of the team treatment of malocclusion and facial skeletal deformities. Abstract: There is no publication concerning tongue-tie (TT) in adults, surprisingly. It is generally known that TT is mainly diagnosed in newborns and infants. It seems unlikely that TT does not cause functional disorders in adults, especially considering that TT has been present in organism since childhood. Thus, there is insufficient information about the influence of TT on adults0 speech production. The purpose of this study was the functional evaluation of lingual frenotomy on tongue mobility and speech in the adult Polish population. Methods: Methods were based on visual observation and examination of the oral cavity accompanied by visual and auditory examination 2 of articulation. X test, Kruskal–Wallis, analysis of variance (ANOVA), and Student’s t-test were used for statistical analyses. Conclusions: Tongue-tie is a serious condition in adults. Implementing 0 Citation: Lichnowska, A.; surgical procedures to treat it improves the tongue s mobility in every direction and improves speech Kozakiewicz, M. -

Uvula in Snoring and Obstructive Sleep Apnea: Role and Surgical Intervention
Opinion American Journal of Otolaryngology and Head and Neck Surgery Published: 13 Apr, 2020 Uvula in Snoring and Obstructive Sleep Apnea: Role and Surgical Intervention Elbassiouny AM* Department of Otolaryngology, Cairo University, Egypt Abstract Objective: Currently, the consideration of the enlarged uvula as a cause of snoring and Obstructive Sleep Apnea (OSA) lacks data for objective interpretation. This article focused on some concepts on how we can manage the enlarged uvula in cases of snoring and OSA. The purpose of the present article is to discuss the cost benefits of uvular surgery versus its preservation. Conclusion: The direct correlation between the uvula and OSA needs to be reevaluated to maintain a balance between reserving its anatomical and physiological functions and surgically manipulating it as a part of palatopharyngeal surgery, yet further objective studies are needed to reach optimal results. Keywords: Uvula; Snoring; Obstructive sleep apnea Introduction The palatine uvula, usually referred to as simply the uvula, is that part of the soft palate that has an anatomical structure and serves some functions. Anatomically, the uvula, a conic projection from the back edge of the middle of the soft palate, is composed of connective tissue containing several racemose glands, and some muscular fibers, musculus uvulae muscle; arises from the posterior nasal spine and the palatine aponeurosis and inserts into the mucous membrane of the uvula. It contains many serous glands, which produce thin saliva [1]. Physiologically, the uvula serves several functions. First during swallowing, the soft palate and the uvula move together to close off the nasopharynx OPEN ACCESS and prevent food from entering the nasal cavity. -

The Main Criteria for Determining Disability in Children With
Sys Rev Pharm 2020; 11(4): 413 418 A multifaceted review journal in the field of pharmacy E-ISSN 0976-2779 P-ISSN 0975-8453 The Main Criteria for Determining Disability in Children with Congenital Cleft Upper Lip and Palate according to the International Classification of Functioning (ICF) Alma Zamurayeva, Taurzhan Aldabergenova*, Bibi-Aisha Orynbayeva, Violetta Detochkina Astana Medical University, Nur-Sultan, Kazakhstan Article History: Submitted: 15.01.2020 Revised: 16.03.2020 Accepted: 20.04.2020 ABSTRACT The role of social rehabilitation of children with congenital facial clinical condition of the child according to the criteria for the severity of pathology is very large. Children with this pathology undoubtedly cleft upper lip and palate, followed by their calculation. belong to the disabling group and are in urgent need of medical and Keywords: face pathology, cleft, disability in children, lip, palate social protection based on a multidisciplinary approach, involving a Correspondence: neonatologist, a pediatrician, an orthodontist, a maxillofacial surgeon, Taurzhan Aldabergenova an ENT doctor, a speech therapist, a teacher, a psychologist, and a Astana Medical University, Nur – Sultan, Kazakhstan social worker. When determining disability for children with congenital DOI: 10.31838/srp.2020.4.62 cleft upper lip and palate by ICF, it is very important to assess the @Advanced Scientific Research. All rights reserved INTRODUCTION children with congenital cleft upper lip and palate according Medical and social rehabilitation of children -
PE1706 Early Speech Development in Children with Cleft Palate
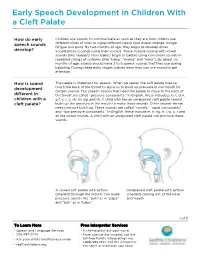
Early Speech Development in Children With a Cleft Palate How do early Children use sounds to communicate as soon as they are born. Infants use speech sounds different kinds of cries to signal different needs (like diaper change, hunger, fatigue and pain). By two months of age, they begin to develop other develop? vocalizations (sounds using their voices). These include cooing with vowel sounds (like “aaaaa”). Next babies begin to babble using consonant sounds in repeated strings of syllables (like “baba,” “mama” and “nana”). By about six months of age, a baby should have 2 to 5 speech sounds that they use during babbling. During these early stages, babies learn they can use sound to get attention. How is sound The palate is important for speech. When we speak, the soft palate rises to development touch the back of the throat to allow us to build up pressure in our mouth for certain sounds. The speech sounds that need the palate to close to the back of different in the throat are called “pressure consonants.” In English, these include p, b, t, d, k, children with a g f, v, s, z, sh, ch, dg, and th. A child who has an unrepaired cleft palate cannot cleft palate? build up the pressure in the mouth to make these sounds. Other sounds do not need pressure build-up. These sounds are called “vowels,” “nasal consonants” and “low pressure consonants.” In English, these include m, n, ng, h, l, w, y, r and all the vowel sounds. A child with an unrepaired cleft palate can produce these sounds. -

Soft Palate and Its Motor Innervation: a Brief Review
Review Article Anatomy Physiol Biochem Int J Volume 5 Issue 4 - April 2019 Copyright © All rights are reserved by Liancai Mu DOI: 10.19080/APBIJ.2019.05.555672 Soft Palate and Its Motor Innervation: A Brief Review Liancai Mu1*, Jingming Chen1, Jing Li1, Stanislaw Sobotka1,2 and Mary Fowkes3 1Department of Biomedical Research, Upper Airway Research Laboratory, Hackensack University Medical Center, USA 2Department of Neurosurgery, Icahn School of Medicine at Mount Sinai, USA 3Department of Pathology, Icahn School of Medicine at Mount Sinai, USA Submission: March 29, 2019; Published: April 18, 2019 *Corresponding author: Liancai Mu, MD, Ph.D, Upper Airway Research Laboratory, Department of Biomedical Research, Hackensack University Medical Center, 40 Prospect Avenue, Hackensack, NJ, 07601, USA Abstract Human soft palate plays an important role in upper airway functions such as speech, swallowing and respiration. However, neural control of the soft palate is poorly understood because innervation of this structure has long been controversial. In this review, the inconsistent and even contradictory observations regarding the motor innervation of the palatal muscles are summarized. We emphasize to use Sihler’s stain for documenting the nerves and their supply patterns within individual palatal muscles as studies have demonstrated that Sihler’s stain permits mapping of entire nerve supply within organs, skeletal muscles, mucosa, skin, and other structures. This wholemount nerve staining has unique advantage over other anatomical methods as all the nerves within the muscles processed with Sihler’s stain can be visualized in their 3-dimensional positions. Advanced knowledge of the neural organization of the soft palate is critical for a better understanding of its functions and for the development of novel neuromodulation therapies to treat soft palate-related upper airway disorders such as obstructive sleep apnea. -

Cleft Lip and Cleft Palate
Cleft Lip and Cleft Palate How do cleft lip and cleft palate occur? Each of us has a cleft or gap of the lip and palate during the early weeks of development in our mother’s womb. Normally, the tissues that form the palate (the roof of your mouth) and the upper lip come together in the middle and join (fuse). You can see the lines of fusion in the “Cupid’s bow” under your own nose, and feel the ridge and line in the middle of your palate. If your baby has a cleft, this fusion did not happen when he or she was developing. Why does fusion of the palate fail to happen? In most cases we simply don’t know why lip and palate do not fuse. About 1 in 700 babies has a cleft lip or cleft palate. In some families, clefts appear in several family members, so heredity is important. Sometimes substances in the environment, called teratogens, may be associated with clefts. But most babies with clefts have no known relatives with clefts and no known exposure to teratogens. A few babies with clefts also have other abnormalities. Unilateral incomplete cleft lip Unilateral complete cleft lip Bilateral cleft lip Cleft palate Revised: 26. 03.14 Page 1 Did we do anything wrong? We don’t know what causes most clefts. Even if it is hereditary in your family, it is still not your fault. What happens now? Remember that cleft lip and palate are not dangerous to your child. The surgery to repair the cleft can be done when the child is the right size and in good enough general health to tolerate surgery. -

Information for Parents Whose Baby Has Been Born with a Cleft Palate
Patient Information Service Cleft information Information for parents whose baby has been born with a cleft palate Respecting everyone Embracing change Recognising success Working together Our hospitals. Contents Page Adjusting to the birth of your baby 3 Background information 5 Feeding your baby 8 Surgery for your baby’s cleft palate 10 Looking after your child’s teeth 13 Hearing – what to watch for 15 Supporting your baby’s speech and language development 17 Psychological support 21 CLAPA: The Cleft Lip and Palate Association 24 Glossary 27 List of contacts 34 2 Adjusting to the birth of your baby The birth of your baby is a wonderful event – an event you have waited for with a mixture of excitement and happiness. Naturally, all parents hope and expect that their child will be perfectly formed. To you, particularly if you have never seen this condition before, your baby may look very different and part of you may feel this isn’t the child you expected. All sorts of feelings may arise and many thoughts race through your head, possibly most of all “why us?” You are not alone. All parents whose babies have this condition can feel like this and can find adjusting to the realisation that their baby is not “perfect” very difficult. These are all very normal reactions and are understood by all those people involved with your care and the care of your baby. You may have lots of questions from the start, or these may take a while to become clear to you. You may find that the information given to you at and around the time of the birth of your baby is confusing and just too much.