Leveraging Allele-Specific Expression for Therapeutic Response Gene Discovery in Glioblastoma
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Using Cellminer 1.6 for Systems Pharmacology and Genomic Analysis of the NCI-60 William C. Reinhold1, Margot Sunshine1,2, Sudhir
Author Manuscript Published OnlineFirst on June 5, 2015; DOI: 10.1158/1078-0432.CCR-15-0335 Author manuscripts have been peer reviewed and accepted for publication but have not yet been edited. Using CellMiner 1.6 for Systems Pharmacology and Genomic Analysis of the NCI-60 William C. Reinhold1, Margot Sunshine1,2, Sudhir Varma1,2,3, James H. Doroshow1,4, and Yves Pommier1 1Developmental Therapeutics Branch and Laboratory of Molecular Pharmacology, Center for Cancer Research, NCI, NIH, Bethesda, Maryland; 2Systems Research and Applications Corp., Fairfax, Virginia; 3HiThru Analytics LLC, Laurel, Maryland; 4Developmental Therapeutics Program, DCTD, NCI, NIH, Bethesda, Maryland. Note: Supplementary data for this article are available at Clinical Cancer Research Online (http://clincancerres.aacrjournals.org/). W.C. Reinhold and Y. Pommier share senior authorship. Corresponding Authors: William C. Reinhold, NIH, 9000 Rockville Pike, Building 37, Room 5041, Bethesda, MD 20892; E-mail: [email protected], and Yves Pommier, NIH, 9000 Rockville Pike, Building 37, Room 5068, Bethesda, MD 20892; E-mail [email protected] Running Title: CellMiner for Systems Pharmacology Disclosure of Potential Conflicts of Interest No potential conflicts of interest were disclosed. Downloaded from clincancerres.aacrjournals.org on September 27, 2021. © 2015 American Association for Cancer Research. Author Manuscript Published OnlineFirst on June 5, 2015; DOI: 10.1158/1078-0432.CCR-15-0335 Author manuscripts have been peer reviewed and accepted for publication but have not yet been edited. Abstract The NCI-60 cancer cell line panel provides a premier model for data integration and systems pharmacology being the largest publicly available database of anticancer drug activity, , genomic, molecular, and phenotypic data. -

SLFN11 Promotes CDT1 Degradation by CUL4 in Response to Replicative DNA Damage, While Its Absence Leads to Synthetic Lethality with ATR/CHK1 Inhibitors
SLFN11 promotes CDT1 degradation by CUL4 in response to replicative DNA damage, while its absence leads to synthetic lethality with ATR/CHK1 inhibitors Ukhyun Joa,1, Yasuhisa Muraia, Sirisha Chakkab, Lu Chenb, Ken Chengb, Junko Muraic, Liton Kumar Sahaa, Lisa M. Miller Jenkinsd, and Yves Pommiera,1 aDevelopmental Therapeutics Branch, Laboratory of Molecular Pharmacology, Center for Cancer Research, National Cancer Institute, Bethesda, MD 20814; bNational Center for Advancing Translational Sciences, Functional Genomics Laboratory, NIH, Rockville, MD 20850; cInstitute for Advanced Biosciences, Keio University, 997-0052 Yamagata, Japan; and dLaboratory of Cell Biology, Center for Cancer Research, National Cancer Institute, NIH, Bethesda, MD 20892 Edited by Richard D. Kolodner, Ludwig Institute for Cancer Research, La Jolla, CA, and approved December 8, 2020 (received for review July 29, 2020) Schlafen-11 (SLFN11) inactivation in ∼50% of cancer cells confers condensation related to deposition of H3K27me3 in the gene broad chemoresistance. To identify therapeutic targets and under- body of SLFN11 by EZH2, a histone methyltransferase (11). lying molecular mechanisms for overcoming chemoresistance, we Targeting epigenetic regulators is therefore an attractive com- performed an unbiased genome-wide RNAi screen in SLFN11-WT bination strategy to overcome chemoresistance of SLFN11- and -knockout (KO) cells. We found that inactivation of Ataxia deficient cancers (10, 25, 26). An alternative approach is to at- Telangiectasia- and Rad3-related (ATR), CHK1, BRCA2, and RPA1 tack SLFN11-negative cancer cells by targeting the essential SLFN11 overcome chemoresistance to camptothecin (CPT) in -KO pathways that cells use to overcome replicative damage and cells. Accordingly, we validate that clinical inhibitors of ATR replication stress. -

CD29 Identifies IFN-Γ–Producing Human CD8+ T Cells with an Increased Cytotoxic Potential
+ CD29 identifies IFN-γ–producing human CD8 T cells with an increased cytotoxic potential Benoît P. Nicoleta,b, Aurélie Guislaina,b, Floris P. J. van Alphenc, Raquel Gomez-Eerlandd, Ton N. M. Schumacherd, Maartje van den Biggelaarc,e, and Monika C. Wolkersa,b,1 aDepartment of Hematopoiesis, Sanquin Research, 1066 CX Amsterdam, The Netherlands; bLandsteiner Laboratory, Oncode Institute, Amsterdam University Medical Center, University of Amsterdam, 1105 AZ Amsterdam, The Netherlands; cDepartment of Research Facilities, Sanquin Research, 1066 CX Amsterdam, The Netherlands; dDivision of Molecular Oncology and Immunology, Oncode Institute, The Netherlands Cancer Institute, 1066 CX Amsterdam, The Netherlands; and eDepartment of Molecular and Cellular Haemostasis, Sanquin Research, 1066 CX Amsterdam, The Netherlands Edited by Anjana Rao, La Jolla Institute for Allergy and Immunology, La Jolla, CA, and approved February 12, 2020 (received for review August 12, 2019) Cytotoxic CD8+ T cells can effectively kill target cells by producing therefore developed a protocol that allowed for efficient iso- cytokines, chemokines, and granzymes. Expression of these effector lation of RNA and protein from fluorescence-activated cell molecules is however highly divergent, and tools that identify and sorting (FACS)-sorted fixed T cells after intracellular cytokine + preselect CD8 T cells with a cytotoxic expression profile are lacking. staining. With this top-down approach, we performed an un- + Human CD8 T cells can be divided into IFN-γ– and IL-2–producing biased RNA-sequencing (RNA-seq) and mass spectrometry cells. Unbiased transcriptomics and proteomics analysis on cytokine- γ– – + + (MS) analyses on IFN- and IL-2 producing primary human producing fixed CD8 T cells revealed that IL-2 cells produce helper + + + CD8 Tcells. -

Integrated Genomics and Therapeutics Predictors of Small
bioRxiv preprint doi: https://doi.org/10.1101/2020.03.09.980623; this version posted April 7, 2020. The copyright holder for this preprint (which was not certified by peer review) is the author/funder. This article is a US Government work. It is not subject to copyright under 17 USC 105 and is also made available for use under a CC0 license. 1 SCLC_CellMiner: Integrated Genomics and Therapeutics Predictors of Small Cell Lung 2 Cancer Cell Lines based on their genomic signatures 3 4 Camille Tlemsani1,†,*, Lorinc Pongor1,†, Luc Girard4, Nitin Roper1, Fathi Elloumi1, Sudhir 5 Varma1, Augustin Luna5, Vinodh N. Rajapakse1, Robin Sebastian1, Kurt W. Kohn1, Julia 6 Krushkal2, Mirit Aladjem1, Beverly A. Teicher2, Paul S. Meltzer3, William C. Reinhold1, John D. 7 Minna4, Anish Thomas1 and Yves Pommier1, 6 8 9 1 Developmental Therapeutics Branch and Laboratory of Molecular Pharmacology, Center for 10 Cancer Research, National Cancer Institute, NIH, Bethesda, MD 20892, USA 11 12 2 Biometric Research Program, Division of Cancer Treatment and Diagnosis, National Cancer 13 Institute, NIH, 9609 Medical Center Dr., Rockville, MD 20850, USA 14 15 3 Genetics Branch, Center for Cancer Research, National Cancer Institute, Bethesda, MD 20892, 16 USA 17 18 4 Hamon Center for Therapeutic Oncology Research, UT Southwestern Medical Center, Dallas, 19 TX 75390, USA 20 21 5 cBio Center, Division of Biostatistics, Department of Data Sciences, Dana-Farber Cancer 22 Institute, Boston, MA 02115, USA 23 24 6 To whom correspondence should be addressed: 25 [email protected] 26 27 * present address, INSERM U1016, Cochin Institute, Paris Descartes University, 75014 Paris 28 29 † Contributed equally to the study 30 31 32 1 bioRxiv preprint doi: https://doi.org/10.1101/2020.03.09.980623; this version posted April 7, 2020. -

HHS Public Access Author Manuscript
HHS Public Access Author manuscript Author Manuscript Author ManuscriptClin Cancer Author Manuscript Res. Author Author Manuscript manuscript; available in PMC 2016 September 15. Published in final edited form as: Clin Cancer Res. 2015 September 15; 21(18): 4184–4193. doi:10.1158/1078-0432.CCR-14-2112. SLFN11 is a transcriptional target of EWS-FLI1 and a determinant of drug response in Ewing’s sarcoma Sai-Wen Tang1, Sven Bilke2, Liang Cao2, Junko Murai1, Fabricio G. Sousa1,4, Mihoko Yamade1, Vinodh Rajapakse1, Sudhir Varma1, Lee J. Helman3, Javed Khan2, Paul S. Meltzer2, and Yves Pommier1 1Laboratory of Molecular Pharmacology, Developmental Therapeutics Branch, National Institutes of Health, Bethesda, MD 20892 2Genetics Branch, National Institutes of Health, Bethesda, MD 20892 3Pediatric Oncology Branch, Center for Cancer Research, National Cancer Institute, National Institutes of Health, Bethesda, MD 20892 4CETROGEN, PPGFARM, UFMS, Campo Grande, MS 79070-900, Brazil Abstract Purpose—SLFN11 was identified as a critical determinant of response to DNA targeted therapies by analyzing gene expression and drug sensitivity of NCI-60 and CCLE datasets. However, how SLFN11 is regulated in cancer cells remained unknown. Ewing’s sarcoma (ES), which is characterized by the chimeric transcription factor EWS-FLI1, has notably high SLFN11 expression, leading us to investigate whether EWS-FLI1 drives SLFN11 expression and the role of SLFN11 in the drug response of ES cells. Experimental Design—Binding sites of EWS-FLI1 on the SLFN11 promoter were analyzed by chromatin immunoprecipitation-DNA sequence (ChIP-Seq) and promoter-luciferase reporter analyses. The relationship between SLFN11 and EWS-FLI1 were further examined in EWS-FLI1- knockdown or -overexpressing cells and in clinical tumor samples. -

The Role of SMARCAD1 During Replication Stress Sarah Joseph
The role of SMARCAD1 during replication stress Sarah Joseph Submitted in partial fulfillment of the requirements for the degree of Doctor of Philosophy under the Executive Committee of the Graduate School of Arts and Sciences COLUMBIA UNIVERSITY 2020 © 2020 Sarah Joseph All Rights Reserved Abstract The role of SMARCAD1 during replication stress Sarah Joseph Heterozygous mutations in BRCA1 or BRCA2 predispose carriers to an increased risk for breast or ovarian cancer. Both BRCA1 and BRCA2 (BRCA1/2) play an integral role in promoting genomic stability through their respective actions during homologous recombination (HR) mediated repair and stalled replication fork protection from nucleolytic degradation. SMARCAD1 (SD1) is a SWI/SNF chromatin remodeler that has been implicated in promoting long-range end resection and contributes to HR. Using human cell lines, we show that SMARCAD1 promotes nucleolytic degradation in BRCA1/2-deficient cells dependent on its chromatin remodeling activity. Moreover, SMARCAD1 prevents DNA break formation and promotes fork restart at stalled replication forks. These studies identify a new role for SMARCAD1 at the replication fork. In addition to the work presented here, I discuss a method for introducing stop codons (nonsense mutations) into genes using CRISPR-mediated base editing, called iSTOP, and provide an online resource for accessing the sequence of iSTOP sgRNASs (sgSTOPs) for five base editor variants (VQR-BE3, EQR-BE3, VRER-BE3, SaBE3, and SaKKH-BE3) in humans and over 3 million targetable gene coordinates for eight eukaryotic species. Ultimately, with improvements to CRISPR base editors this method can help model and study nonsense mutations in human disease. Table of Contents List of Figures ................................................................................................................. -

34858 SLFN11 (D8W1B) Rabbit Mab
Revision 1 C 0 2 - t SLFN11 (D8W1B) Rabbit mAb a e r o t S Orders: 877-616-CELL (2355) [email protected] 8 Support: 877-678-TECH (8324) 5 8 Web: [email protected] 4 www.cellsignal.com 3 # 3 Trask Lane Danvers Massachusetts 01923 USA For Research Use Only. Not For Use In Diagnostic Procedures. Applications: Reactivity: Sensitivity: MW (kDa): Source/Isotype: UniProt ID: Entrez-Gene Id: WB, IP, IHC-Bond, IHC-P, F H Endogenous 100 Rabbit IgG Q7Z7L1 91607 Product Usage Information Application Dilution Western Blotting 1:1000 Immunoprecipitation 1:100 IHC-Leica® Bond™ 1:200 Immunohistochemistry (Paraffin) 1:200 Flow Cytometry 1:400 Storage Supplied in 10 mM sodium HEPES (pH 7.5), 150 mM NaCl, 100 µg/ml BSA, 50% glycerol and less than 0.02% sodium azide. Store at –20°C. Do not aliquot the antibody. Specificity / Sensitivity SLFN11 (D8W1B) Rabbit mAb recognizes endogenous levels of total SLFN11 protein. Non-specific staining was observed in skeletal muscle. Species Reactivity: Human Source / Purification Monoclonal antibody is produced by immunizing animals with recombinant protein specific to human SLFN11 protein. Background SLFN11 is a nuclear protein that belongs to the Schlafen (SLFN) family of genes involved in cell cycle regulation and growth inhibition (1, 2). Expression of SLFN11 predicts sensitivity of cancer cell lines to DNA-damaging agents (1, 3). Evidence suggests that in the presence of DNA-targeted therapies, SLFN11 is recruited to stressed replication forks where it blocks replication leading to cell death (4). SLFN11 is being explored as a predictive biomarker for response to DNA-targeted therapies (5). -

Regulation of Schlafen 11 Expression
University of Texas at El Paso ScholarWorks@UTEP Open Access Theses & Dissertations 2020-01-01 Regulation Of Schlafen 11 Expression Christian Waldemar Corona Ayala University of Texas at El Paso Follow this and additional works at: https://scholarworks.utep.edu/open_etd Part of the Biomedical Commons Recommended Citation Corona Ayala, Christian Waldemar, "Regulation Of Schlafen 11 Expression" (2020). Open Access Theses & Dissertations. 2952. https://scholarworks.utep.edu/open_etd/2952 This is brought to you for free and open access by ScholarWorks@UTEP. It has been accepted for inclusion in Open Access Theses & Dissertations by an authorized administrator of ScholarWorks@UTEP. For more information, please contact [email protected]. REGULATION OF SCHLAFEN 11 EXPRESSION CHRISTIAN WALDEMAR CORONA AYALA Master’s Program in Biomedical Engineering APPROVED: Manuel Llano, Ph.D., M.D., Chair Thomas Boland, Ph.D. Delfina Dominguez, Ph.D. Stephen L. Crites, Jr., Ph.D. Dean of the Graduate School Copyright © by Christian Waldemar Corona Ayala 2020 DEDICATION I would like to dedicate this work to my family, specially my mother that always gave me her support and love, I also want to dedicate this to my girlfriend that always believed in me, and last but not least to all my friends that always helped me during this processes. REGULATION OF SCHLAFEN 11 EXPRESSION by CHRISTIAN WALDEMAR CORONA AYALA M.D. THESIS Presented to the Faculty of the Graduate School of The University of Texas at El Paso in Partial Fulfillment of the Requirements for the Degree of MASTER OF SCIENCE Department of Metallurgical, Materials and Biomedical Engineering THE UNIVERSITY OF TEXAS AT EL PASO May 2020 ACKNOWLEDGEMENT I wish to express my sincere gratitude to my mentor, Dr. -

The NCI-60 Methylome and Its Integration Into Cellminer William C
Published OnlineFirst December 6, 2016; DOI: 10.1158/0008-5472.CAN-16-0655 Cancer Integrated Systems and Technologies Research The NCI-60 Methylome and Its Integration into CellMiner William C. Reinhold1, Sudhir Varma1,2,3, Margot Sunshine1,2, Vinodh Rajapakse1, Augustin Luna1,4,5, Kurt W. Kohn1, Holly Stevenson6, Yonghong Wang6, Holger Heyn7, Vanesa Nogales7, Sebastian Moran7, David J. Goldstein8, James H. Doroshow1,10, Paul S. Meltzer6, Manel Esteller6,9,11,12, and Yves Pommier1 Abstract A unique resource for systems pharmacology and genomic with transcript levels yielded an assessment of their relative studies is the NCI-60 cancer cell line panel, which provides data influence for 15,798 genes, including tumor suppressor, mito- for the largest publicly available library of compounds with chondrial, and mismatch repair genes. Four forms of molecular cytotoxic activity (21,000 compounds), including 108 FDA- data were combined, providing rationale for microsatellite approved and 70 clinical trial drugs as well as genomic data, instability for 8 of the 9 cell lines in which it occurred. including whole-exome sequencing, gene and miRNA tran- Individual cell line analyses showed global methylome patterns scripts, DNA copy number, and protein levels. Here, we provide with overall methylation levels ranging from 17% to 84%. A the first readily usable genome-wide DNA methylation data- six-gene model, including PARP1, EP300, KDM5C, SMARCB1, base for the NCI-60, including 485,577 probes from the Infi- and UHRF1 matched this pattern. In addition, promoter meth- nium HumanMethylation450k BeadChip array, which yielded ylation of two translationally relevant genes, Schlafen 11 DNA methylation signatures for 17,559 genes integrated into (SLFN11) and methylguanine methyltransferase (MGMT), our open access CellMiner version 2.0 (https://discover.nci.nih. -
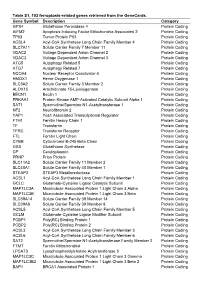
Table S1. 103 Ferroptosis-Related Genes Retrieved from the Genecards
Table S1. 103 ferroptosis-related genes retrieved from the GeneCards. Gene Symbol Description Category GPX4 Glutathione Peroxidase 4 Protein Coding AIFM2 Apoptosis Inducing Factor Mitochondria Associated 2 Protein Coding TP53 Tumor Protein P53 Protein Coding ACSL4 Acyl-CoA Synthetase Long Chain Family Member 4 Protein Coding SLC7A11 Solute Carrier Family 7 Member 11 Protein Coding VDAC2 Voltage Dependent Anion Channel 2 Protein Coding VDAC3 Voltage Dependent Anion Channel 3 Protein Coding ATG5 Autophagy Related 5 Protein Coding ATG7 Autophagy Related 7 Protein Coding NCOA4 Nuclear Receptor Coactivator 4 Protein Coding HMOX1 Heme Oxygenase 1 Protein Coding SLC3A2 Solute Carrier Family 3 Member 2 Protein Coding ALOX15 Arachidonate 15-Lipoxygenase Protein Coding BECN1 Beclin 1 Protein Coding PRKAA1 Protein Kinase AMP-Activated Catalytic Subunit Alpha 1 Protein Coding SAT1 Spermidine/Spermine N1-Acetyltransferase 1 Protein Coding NF2 Neurofibromin 2 Protein Coding YAP1 Yes1 Associated Transcriptional Regulator Protein Coding FTH1 Ferritin Heavy Chain 1 Protein Coding TF Transferrin Protein Coding TFRC Transferrin Receptor Protein Coding FTL Ferritin Light Chain Protein Coding CYBB Cytochrome B-245 Beta Chain Protein Coding GSS Glutathione Synthetase Protein Coding CP Ceruloplasmin Protein Coding PRNP Prion Protein Protein Coding SLC11A2 Solute Carrier Family 11 Member 2 Protein Coding SLC40A1 Solute Carrier Family 40 Member 1 Protein Coding STEAP3 STEAP3 Metalloreductase Protein Coding ACSL1 Acyl-CoA Synthetase Long Chain Family Member 1 Protein -

Characterization of the Anti-Viral Activity of Schlafen13
University of Texas at El Paso ScholarWorks@UTEP Open Access Theses & Dissertations 2020-01-01 Characterization Of The Anti-Viral Activity Of Schlafen13 Jordan Winfield University of Texas at El Paso Follow this and additional works at: https://scholarworks.utep.edu/open_etd Part of the Virology Commons Recommended Citation Winfield, Jordan, "Characterization Of The Anti-Viral Activity Of Schlafen13" (2020). Open Access Theses & Dissertations. 3061. https://scholarworks.utep.edu/open_etd/3061 This is brought to you for free and open access by ScholarWorks@UTEP. It has been accepted for inclusion in Open Access Theses & Dissertations by an authorized administrator of ScholarWorks@UTEP. For more information, please contact [email protected]. CHARACTERIZATION OF THE ANTI-VIRAL ACTIVITY OF SCHLAFEN13 JORDAN WILLIAM WINFIELD Master’s Program in Biological Sciences APPROVED: Manuel Llano, M.D., Ph.D., Chair Ricardo Bernal, Ph.D. Immo A. Hansen, Ph.D. Stephen L. Crites, Jr., Ph.D. Dean of the Graduate School Copyright © by Jordan Winfield 2020 CHARACTERIZATION OF THE ANTI-VIRAL ACTIVITY OF SCHLAFEN13 by JORDAN WILLIAM WINFIELD, B.S. THESIS Presented to the Faculty of the Graduate School of The University of Texas at El Paso in Partial Fulfillment of the Requirements for the Degree of MASTER OF SCIENCE Department of Biological Sciences THE UNIVERSITY OF TEXAS AT EL PASO May 2020 ACKNOWLEDGEMENTS First and foremost, I would like to thank my family and friends who have supported me throughout my journey to arrive at this point. Particularly, my mother who has sacrificed so much to ensure that I am able to be successful in life. -

Gene Expression Signature Based Screening Identifies Ribonucleotide Reductase As a Candidate Therapeutic Target in Ewing Sarcoma
www.impactjournals.com/oncotarget/ Oncotarget, Vol. 7, No. 39 Research Paper Gene expression signature based screening identifies ribonucleotide reductase as a candidate therapeutic target in Ewing sarcoma Kelli L. Goss1 and David J. Gordon1 1 Department of Pediatrics, Division of Pediatric Hematology/Oncology, University of Iowa, Iowa City, Iowa, USA Correspondence to: David J. Gordon , email: [email protected] Keywords: Ewing sarcoma, ribonucleotide reductase, ciclopirox, iron chelator Received: June 28, 2016 Accepted: August 13, 2016 Published: August 19, 2016 ABSTRACT There is a critical need in cancer therapeutics to identify targeted therapies that will improve outcomes and decrease toxicities compared to conventional, cytotoxic chemotherapy. Ewing sarcoma is a highly aggressive bone and soft tissue cancer that is caused by the EWS-FLI1 fusion protein. Although EWS-FLI1 is specific for cancer cells, and required for tumorigenesis, directly targeting this transcription factor has proven challenging. Consequently, targeting unique dependencies or key downstream mediators of EWS-FLI1 represent important alternative strategies. We used gene expression data derived from a genetically defined model of Ewing sarcoma to interrogate the Connectivity Map and identify a class of drugs, iron chelators, that downregulate a significant number of EWS-FLI1 target genes. We then identified ribonucleotide reductase M2 (RRM2), the iron-dependent subunit of ribonucleotide reductase (RNR), as one mediator of iron chelator toxicity in Ewing sarcoma cells. Inhibition of RNR in Ewing sarcoma cells caused apoptosis in vitro and attenuated tumor growth in an in vivo, xenograft model. Additionally, we discovered that the sensitivity of Ewing sarcoma cells to inhibition or suppression of RNR is mediated, in part, by high levels of SLFN11, a protein that sensitizes cells to DNA damage.