General Principles the Acetabular Index and Center-Edge Angles
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Pelvic Anatomyanatomy
PelvicPelvic AnatomyAnatomy RobertRobert E.E. Gutman,Gutman, MDMD ObjectivesObjectives UnderstandUnderstand pelvicpelvic anatomyanatomy Organs and structures of the female pelvis Vascular Supply Neurologic supply Pelvic and retroperitoneal contents and spaces Bony structures Connective tissue (fascia, ligaments) Pelvic floor and abdominal musculature DescribeDescribe functionalfunctional anatomyanatomy andand relevantrelevant pathophysiologypathophysiology Pelvic support Urinary continence Fecal continence AbdominalAbdominal WallWall RectusRectus FasciaFascia LayersLayers WhatWhat areare thethe layerslayers ofof thethe rectusrectus fasciafascia AboveAbove thethe arcuatearcuate line?line? BelowBelow thethe arcuatearcuate line?line? MedianMedial umbilicalumbilical fold Lateralligaments umbilical & folds folds BonyBony AnatomyAnatomy andand LigamentsLigaments BonyBony PelvisPelvis TheThe bonybony pelvispelvis isis comprisedcomprised ofof 22 innominateinnominate bones,bones, thethe sacrum,sacrum, andand thethe coccyx.coccyx. WhatWhat 33 piecespieces fusefuse toto makemake thethe InnominateInnominate bone?bone? PubisPubis IschiumIschium IliumIlium ClinicalClinical PelvimetryPelvimetry WhichWhich measurementsmeasurements thatthat cancan bebe mademade onon exam?exam? InletInlet DiagonalDiagonal ConjugateConjugate MidplaneMidplane InterspinousInterspinous diameterdiameter OutletOutlet TransverseTransverse diameterdiameter ((intertuberousintertuberous)) andand APAP diameterdiameter ((symphysissymphysis toto coccyx)coccyx) -

Evaluation and Treatment of Selected Sacral Somatic Dysfunctions
Evaluation and Treatment of Selected Sacral Somatic Dysfunctions Using Direct and HVLA Techniques including Counterstrain and Muscle Energy AND Counterstrain Treatment of the Pelvis and Sacrum F. P. Wedel, D.O. Associate Adjunct Professor in Osteopathic Principles and Practice A.T. Still University School of Osteopathic Medicine in Arizona, and private practice in Family Medicine in Tucson, Arizona Learning Objectives HOURS 1 AND 2 Review the following diagnostic and treatment techniques related to sacral torsion Lumbosacral spring test Sacral palpation Seated flexion test HOURS 3 AND 4 Counterstrain treatments of various low back pathologies Sacral Techniques Covered : 1. Prone, direct, muscle energy, for sacral rotation on both same and opposite axes 2. HVLA treatment for sacral rotation on both same and opposite axes 3. Counterstain treatment of sacral tender points and of sacral torsion Counterstrain Multifidi and Rotatores : UP5L Gluteii – maximus: HFO-SI, HI, P 3L- P 4L ,medius, minimus Piriformis Background and Basis The 4 Osteopathic Tenets (Principles) 1. The body is a unit; the person is a unit of body, mind, and spirit. 2. Structure and function are reciprocally inter-related. 3. The body is capable of self- regulation, self-healing, and health maintenance. 4. Rational treatment is based upon an understanding of these basic principles. Somatic Dysfunction - Defined • “Impaired or altered function of related components of the somatic (body framework) system: • Skeletal, arthrodial, and myofascial structures, • And… • Related vascular, lymphatic, and neural elements” Treatment Options for Somatic Dysfunctions All somatic dysfunctions have a restrictive barrier which are considered “pathologic” This restriction inhibits movement in one direction which causes asymmetry within the joint: The goal of osteopathic treament is to eliminate the restrictive barrier thus restoring symmetry…. -

Hybrid Solution Combining Osteosynthesis and Endoprosthesis for Double Column Acetabular Fractures in the Elderly Provide More Stability with Finite Element Model
Eklem Hastalıkları ve Eklem Hastalik Cerrahisi Cerrahisi 2019;30(2):106-111 Joint Diseases and Related Surgery Original Article / Özgün Makale doi: 10.5606/ehc.2019.66592 Hybrid solution combining osteosynthesis and endoprosthesis for double column acetabular fractures in the elderly provide more stability with finite element model Yaşlılarda çift kolon asetabuler kırıklar için osteosentez ve endoprotez hibrid kombinasyonu “finite element” yöntemi ile daha çok stabilite sağlar András Kocsis, MD1, Károly Váradi, MD2, Gábor Szalai2, Tamás Kovács, MD1, Tamás Bodzay, MD, PhD1 1Jenő Manninger National Institute of Traumatology, Budapest, Hungary 2Budapest University of Technology and Economics, Faculty of Mechanical Engineering, Department of Machine and Product Design, Hungary ABSTRACT ÖZ Objectives: This study aims to compare mechanical Amaç: Bu çalışmada yaşlılarda çift kolon kırıklarında stability of osteosynthesis (plate and screw fixation) alone osteosenteze (plak ve vida tespiti) kıyasla kalça artroplastisi ile versus the same method supplemented with hip arthroplasty desteklenen aynı yöntemin (hibrid çözüm) mekanik stabilitesi (hybrid solution) for double column fractures in elderly. karşılaştırıldı. Patients and methods: Mechanical investigations were Hastalar ve yöntemler: Çift kolon kırıkları için geliştirilen performed on an advanced finite element pelvis model ileri sonlu eleman pelvis modelinde mekanik araştırmalar developed for double column fractures. The following yapıldı. İncelenen simüle edilen implant kombinasyonları simulated -

Lab #23 Anal Triangle
THE BONY PELVIS AND ANAL TRIANGLE (Grant's Dissector [16th Ed.] pp. 141-145) TODAY’S GOALS: 1. Identify relevant bony features/landmarks on skeletal materials or pelvic models. 2. Identify the sacrotuberous and sacrospinous ligaments. 3. Describe the organization and divisions of the perineum into two triangles: anal triangle and urogenital triangle 4. Dissect the ischiorectal (ischioanal) fossa and define its boundaries. 5. Identify the inferior rectal nerve and artery, the pudendal (Alcock’s) canal and the external anal sphincter. DISSECTION NOTES: The perineum is the diamond-shaped area between the upper thighs and below the inferior pelvic aperture and pelvic diaphragm. It is divided anatomically into 2 triangles: the anal triangle and the urogenital (UG) triangle (Dissector p. 142, Fig. 5.2). The anal triangle is bounded by the tip of the coccyx, sacrotuberous ligaments, and a line connecting the right and left ischial tuberosities. It contains the anal canal, which pierced the levator ani muscle portion of the pelvic diaphragm. The urogenital triangle is bounded by the ischiopubic rami to the inferior surface of the pubic symphysis and a line connecting the right and left ischial tuberosities. This triangular space contains the urogenital (UG) diaphragm that transmits the urethra (in male) and urethra and vagina (in female). A. Anal Triangle Turn the cadaver into the prone position. Make skin incisions as on page 144, Fig. 5.4 of the Dissector. Reflect skin and superficial fascia of the gluteal region in one flap to expose the large gluteus maximus muscle. This muscle has proximal attachments to the posteromedial surface of the ilium, posterior surfaces of the sacrum and coccyx, and the sacrotuberous ligament. -

Approach to the Anterior Pelvis (Enneking Type III Resection) Bruno Fuchs, MD Phd & Franklin H.Sim, MD Indication 1
Approach to the Anterior Pelvis (Enneking Type III Resection) Bruno Fuchs, MD PhD & Franklin H.Sim, MD Indication 1. Tumors of the pubis 2. part of internal and external hemipelvectomy 3. pelvic fractures Technique 1. Positioning: Type III resections involve the excision of a portion of the symphysis or the whole pubis from the pubic symphysis to the lateral margin of the obturator foramen. The best position for these patients is the lithotomy or supine position. The patient is widely prepared and draped in the lithotomy position with the affected leg free to allow manipulation during the procedure. This allows the hip to be flexed, adducted, and externally rotated to facilitate exposure. 2. Landmarks: One should palpate the ASIS, the symphysis with the pubic tubercles, and the ischial tuberosity. 3. Incision: The incision may be Pfannenstiel like with vertical limbs set laterally along the horizontal incision depending on whether the pubic bones on both sides are resected or not. Alternatively, if only one side is resected, a curved incision following the root of the thigh may be used. This incision begins below the inguinal ligament along the medial border of the femoral triangle and extends across the medial thigh a centimeter distal to the inguinal crease and perineum, to curve distally below the ischium several centimeters (Fig.1). 4. Full thickness flaps are raised so that the anterior inferior pubic ramus is shown in its entire length, from the pubic tubercle to the ischial spine. Laterally, the adductor muscles are visualized, cranially the pectineus muscle and the pubic tubercle with the insertion of the inguinal ligament (Fig.2). -
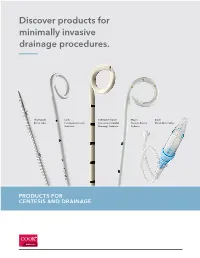
Discover Products for Minimally Invasive Drainage Procedures
Discover products for minimally invasive drainage procedures. Thal-Quick Lock Fuhrman Pleural/ Wayne Cook Chest Tube Pericardiocentesis Pneumopericardial Pneumothorax Chest Drain Valve Catheter Drainage Catheter Catheter MEDICAL Contents Pneumothorax catheters Wayne Pneumothorax Catheter Set and Tray – Seldinger ......................................................................................... 4 Wayne Pneumothorax Catheter Set – Trocar ............................................................................................................... 5 Cook Emergency Pneumothorax Set ........................................................................................................................... 6 Pneumothorax Set and Tray ........................................................................................................................................... 7 Richli Pneumothorax Catheter Set ................................................................................................................................ 8 Catheter Aspiration Set for Simple Pneumothorax .................................................................................................... 9 Multipurpose catheters Thal-Quick Chest Tube Set .......................................................................................................................................... 10 Thal-Quick Chest Tube Tray ......................................................................................................................................... 11 -

Intrapelvic Causes of Sciatica: a Systematic Review
DOI: 10.14744/scie.2020.59354 Review South. Clin. Ist. Euras. 2021;32(1):86-94 Intrapelvic Causes of Sciatica: A Systematic Review 1 1 1 1 Ahmet Kale, Betül Kuru, Gülfem Başol, Elif Cansu Gündoğdu, 1 1 2 3 Emre Mat, Gazi Yıldız, Navdar Doğuş Uzun, Taner A Usta 1Department of Gynecology and Obstetrics, University of Health Sciences, Kartal Dr. Lütfi Kırdar Training and Research Hospital, İstanbul, Turkey 2Department of Gynecology and Obstetrics, Midyat State Hospital, Mardin, Turkey 3Department of Gynecology and Obstetrics, Acıbadem University, Altunizade Hospital, İstanbul, Turkey ABSTRACT Submitted: 09.09.2020 The sciatic nerve is the nerve of the lower limb. It is derived from spinal nerves, fourth Accepted: 27.11.2020 Lumbar (L4) to third Sacral (S3). The sciatic nerve innervates the muscles of the posterior Correspondence: Ahmet Kale, thigh and additionally has sensory functions. Sciatica is the given name to the pain sourced by SBÜ Kartal Dr. Lütfi Kırdar Eğitim irritation of the sciatic nerve. Sciatica is most commonly induced by compression of a lower ve Araştırma Hastanesi, Kadın lumbar nerve root (L4, L5, or S1). Various intrapelvic pathologies include gynecological, Hastalıkları ve Doğum Kliniği, İstanbul, Turkey vascular, traumatic, inflammatory, and tumoral disorders that may cause sciatica. Intrapelvic E-mail: [email protected] pathologies that mimic disc herniation are quite always ignored. Surgical approach and a functional exploration by laparoscopy or robotic surgery have significantly increased the intrapelvic pathology’s awareness, resulting in sciatica. After a detailed assessment of the patient, which causes intrapelvic pathologies, deciding whether surgical or medical therapy is needed, notable results in sciatic pain remission can be done. -

A Novel Wound and Soft Tissue Flap Negative Pressure Drain System - a Pilot Study Steven D
Archives of Health Science Research Article A Novel Wound and Soft Tissue Flap Negative Pressure Drain System - a Pilot Study Steven D. Jones Jr MD*1, Parker J. Prusick MD1, Bennie G. Lindeque MD PhD1 1Department of Orthopedic Surgery, University of Colorado Denver, 12631 E 17th Ave, Aurora, CO 80045, USA *Corresponding Author: Steven D. Jones Jr MD, Department of Orthopedic Surgery, University of Colorado Denver, 12631 E 17th Ave, Aurora, CO 80045, USA Abstract Background: Negative-pressure wound-therapy (NPWT) has become a mainstay of treatment for high-risk surgical wounds. In closed wounds, traditional NPWT utilizes surface level sponges alone to provide negative pressure. A technique that allows for deep dead-space management, while maintaining superficial negative pressure over a closed wound, may prove beneficial inhigh-risk patients. Purpose: A novel technique and prospective case series are described which incorporate deep hemovac drain tubings into a traditional NPWT device (Deep Inside-Out Vac; DIOV). Pilot data is needed to begin evaluating the efficacy of this technique. Methods: Fourteen patients were stratified by initial indication for DIOV placement. Group 1 patients underwent wide tumor resection, while Group 2 patients underwent extensive debridement for infection. Demographic, surgical, and microbiological data were recorded. Results: Eight patients were identified in Group 1. Six were identified in Group 2. Both demonstrated 50% positive culture rates at time of drain removal. Most common organisms were coagulase negative staphylococcus species. At final follow-up, all wounds were clinically healed. Conclusions: NPWT is an established augment in post-operative wound care. The DIOV may provide added benefit in wounds at high-risk for dead-space related complications. -

Curvature of the Greater Sciatic Notch in Sexing the Human Pelvis HIDEO TAKAHASHI1*
ANTHROPOLOGICAL SCIENCE Vol. 000, 000–000, 2006 Curvature of the greater sciatic notch in sexing the human pelvis HIDEO TAKAHASHI1* 1Department of Anatomy, Dokkyo University School of Medicine, 880 Kitakobayashi, Mibu-machi, Shimotuga-gun, Tochigi, 321-0293 Japan Received 11 November 2005; accepted 26 January 2006 Abstract The maximum curvature of the greater sciatic notch and two standardized indices were cal- culated for use in the sexing of human hip bones. This was done by means of quadratic regression of the contour points of the greater sciatic notch. The new variables are not directly affected by the osteo- metric landmarks (e.g. ischial spine, tubercle of the piriformis, and posterior inferior iliac spine) which determine the greatest width of the notch. These landmarks are, however, known to be ill-defined on occasion, but nevertheless have been used to derive the conventional depth-to-width index and angles of the sciatic notch. The curvature parameter and its new indices were applied to the sciatic notch of 164 Japanese hip bones of known sex (104 males and 61 females). The accuracy of the new variables in the determination of sex was assessed and compared with that of the conventional indices and angles of the sciatic notch. The best discriminating variable was found to be the posterior angle with an accu- racy of 91%. The new parameters of the present study that represent localized shape of the sharply curved edge of the notch diagnosed sex with an accuracy of 88%. In paleoanthropological or forensic cases, using the maximum curvature of the sciatic notch and its indices may be applicable to sexing the hip bones of specimens with postmortem damage. -

Wound Drain Tube Management
CLINICAL PROCEDURE WOUND DRAIN TUBE MANAGEMENT TARGET AUDIENCE All Peter Mac medical and nursing staff. STATE ANY RELATED PETER MAC POLICIES, PROCEDURES OR GUIDELINES Clinical Handover Policy Wound Management Guideline Hand Hygiene Procedure Aseptic Technique Procedure Care of Underwater Drainage Procedure Care of Percutaneous Nephrostomy Catheters Procedure Nursing Services Patient Health Assessment Guideline Patient Identification and Procedure Matching Procedure Observation and Response Chart Procedure PURPOSE This procedure aims to provide the target audience with best practice based evidence available, along with expert opinion, in regards to the management of drain tubes within the hospital setting. PROCEDURE Indication Drain tubes can be inserted prophylactically to either prevent or remove the accumulation of fluid in a wound. They can also be therapeutically inserted to evacuate an existing collection of fluid in a wound. Fluid is removed in order to treat or prevent infection and promote wound healing and patient comfort. Drain tubes can also be used to diagnose postoperative complications such as an anastomotic leak or haemorrhage. Types of Drainage Tubes ExudrainTM A closed, active drain system, with a negative pressure of approximately 75mmHg and a reservoir of 100mL. http://vitalmedikal.com.tr/yeni/index.php?option=com_content&task=view&id=9&Itemid=3 BellovacTM A closed, active drain system, with a negative pressure of approximately 90mmHg and a reservoir of 220mL. http://surgery.astratech.com.au/Main.aspx/Item/459337/navt/68686/navl/83954/nava/83974 Surimex Fixvac A closed, active drain system, with a negative pressure of approximately Vacuum System 338mmHg. It has a resevoir of 600mL. Please note: the bottle will only half fill and therefore will need to be changed when half filled. -

The Association of Iliac and Sacral Insufficiency Fractures and Implications for Treatment: the Role of Bone Scans in Three Different Cases
Open Access Case Report DOI: 10.7759/cureus.3861 The Association of Iliac and Sacral Insufficiency Fractures and Implications for Treatment: The Role of Bone Scans in Three Different Cases Sandeep Kola 1 , Michelle Granville 2 , Robert E. Jacobson 2 1. Physical Medicine and Rehabilitation, Larkin Community Hospital, Miami, USA 2. Neurological Surgery, University of Miami Hospital, Miami, USA Corresponding author: Michelle Granville, [email protected] Abstract Iliac wing fractures are under-diagnosed fractures often associated with sacral insufficiency fractures in osteoporotic patients. They are rarely seen alone. Insufficiency fractures of the iliac bone can often be missed on computerized tomography (CT) and magnetic resonance imaging (MRI) yet identified on radioisotope bone scans. Symptomatic iliac fractures present with more lateralized pain in the hip and groin compared to patients with only sacral insufficiency fractures. Since the acetabulum is the key weight- bearing articulation between the sacrum and pelvis and the femoral head and leg, worsening of iliac stress fractures can have major effects on weight bearing and should be a consideration in patients with persistent pain in this area. The anatomy of the ilium and relationship to other pelvic insufficiency fractures is reviewed as well as treatment options. Typical cases are presented where the iliac fractures were found on bone scan either in addition to the more common sacral fracture or due to the persistence of symptoms of hip and thigh pain. Categories: Physical Medicine & Rehabilitation, Radiology, Neurosurgery Keywords: insufficency fractures, ilium, sacral fractures, sacroplasty, acetabulum rim fractures, osteoporosis Introduction The iliac bone composes part of the pelvic ring and can be affected by both traumatic and osteoporotic sacral and pelvic fractures [1-2]. -

Chronic Non Congestive Glaucoma: with Special Emphasis on Therapy
University of Nebraska Medical Center DigitalCommons@UNMC MD Theses Special Collections 5-1-1934 Chronic non congestive glaucoma: with special emphasis on therapy W. Morrison University of Nebraska Medical Center This manuscript is historical in nature and may not reflect current medical research and practice. Search PubMed for current research. Follow this and additional works at: https://digitalcommons.unmc.edu/mdtheses Part of the Medical Education Commons Recommended Citation Morrison, W., "Chronic non congestive glaucoma: with special emphasis on therapy" (1934). MD Theses. 339. https://digitalcommons.unmc.edu/mdtheses/339 This Thesis is brought to you for free and open access by the Special Collections at DigitalCommons@UNMC. It has been accepted for inclusion in MD Theses by an authorized administrator of DigitalCommons@UNMC. For more information, please contact [email protected]. CHRONIC NON-CONGESTIVE GLAUCOMA: WITH ESPECIAL EMPHASIS ON THERAPY -. w. HOWARD MORRISON CHRONIC NON CONGESTIVE GLAUCOMA: with especial emphasis on therapy INTRODUCTION AND HISTORY It is my intention herein to discuss chronic non congestive glaucoma only briefly as an entirety, so that a suitable back ground may be constructed for the more exhaustive perusal of the recent literature on the therapy in that particular type of glaucoma. Throughout this paper the terms chronic non-congestive glaucoma, Simple glaucoma and glaucoma simplex will all refer to the same condition. The term glaucoma is not the title of anyone Single disease but is a clinical label for a complex of symptoms. Over four centuries before the Christian era, Hippocrates described glaukos as among the known affections of the eye. The Greek word, glaukos, he used to describe the disease because he saw a gray green reflex from the pupil.