Diffusion of Innovations in Service Organizations: Systematic Review and Recommendations
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Diffusion of Innovations in Service Organizations: Systematic Review and Recommendations
Diffusion of Innovations in Service Organizations: Systematic Review and Recommendations TRISHA GREENHALGH, GLENN ROBERT, FRASER MACFARLANE∗,PAULBATE, and OLIVIA KYRIAKIDOU∗ University College London; ∗University of Surrey This article summarizes an extensive literature review addressing the question, How can we spread and sustain innovations in health service delivery and or- ganization? It considers both content (defining and measuring the diffusion of innovation in organizations) and process (reviewing the literature in a sys- tematic and reproducible way). This article discusses (1) a parsimonious and evidence-based model for considering the diffusion of innovations in health service organizations, (2) clear knowledge gaps where further research should be focused, and (3) a robust and transferable methodology for systematically re- viewing health service policy and management. Both the model and the method should be tested more widely in a range of contexts. Key Words: Diffusion of innovation, systematic review, implementation. his article summarizes the findings of a systematic literature review of the diffusion of service inno- T vations. The United Kingdom Department of Health explic- itly commissioned this work, which was carried out between October 2002 and December 2003, for its National Health Service’s exten- sive modernization agenda (UK Department of Health 2001). Our review, which supplements and extends previous overviews and meta- analyses (Damanpour 1991, 1992, 1996; Granados et al. 1997; Meyers, Sivakumar, and Nakata 1999; Rogers 1995; Tornatsky and Klein 1982; Address correspondence to: Trisha Greenhalgh, University College London, Room 403, Holborn Union Building, Highgate Hill, London N19 5LW, United Kingdom (e-mail: [email protected]). The Milbank Quarterly, Vol. -

Diffusion of P2 Innovations Pollution Prevention Review / Winter 1998 / 3 Exhibit 1
,+ I. P r, c DIFFUSION OF P2 INNOVATIOHS How does pollution prevention While most private belts, buying insur- and public sector compare with other innovative ance, and emergency agencies agree that planning may be un- preventing pollution ideas? pleasant and theirre- makes much more sults may not be eas- sense than alterna- ily observed. They tive waste management strategies, most would also also tend to have a relatively slow rate of adoption. agree that pollution prevention technology is dif- fusing at a rate far slower than would be expected. Rogers (1995) states: This is particularly true given the advantages and benefits that P2 offers. mhe relative advantage of preventive in- This article, through comparison of pertinent novations is difficult for change agents to literature regarding the diffusion of innovations, demonstrate to their clients, because it attempts to offer some explanations for this rela- occurs at some future, unknown time. tively slow rate and some insights on speeding up Individuals have difficulties in perceiving the P2 diffusion process. the relative advantage of preventive in- novations because the sought-after con- Prevention Is Hard to Sell sequence is distant in time, and so the rela- According to Rogers (1995), a preventive inno- tive advantage of a preventive innovation vation is an idea that an individual adopts at one is a delayed reward. In contrast, point in time in order to lower the probability that nonpreventive innovations tend to pro- some future unwanted event will occur. The un- vide a desired outcome in the near future. wanted future event might not have happened any- way, even without adoption of the preventive inno- P2 innovations have been diffusing relatively vation, so the benefits of adoption may not be clear slowly, in part because they are frequently per- cut. -

18. Innovation and Diffusion
Hall on Diffusion 8 October 2003 18. Innovation and Diffusion Bronwyn H. Hall1 1 Hall on Diffusion 8 October 2003 18.1. Introduction In 1953, a young female Macaque monkey in the south of Japan washed a muddy sweet potato in a stream before eating it. This obvious improvement in food preparation was imitated quickly by other monkeys and in less than 10 years it became the norm in her immediate group; by 1983, the method had diffused completely. In 1956, the same monkey innovated again, inventing a technique in which handfuls of mixed sand and wheat grains were cast upon the sea, so that the floating cereal could be skimmed from the surface. Again, by 1983, this method of gleaning wheat had diffused almost completely throughout the local populations of Macaques.2 Besides the obvious fact that humankind does not have a monopoly on innovation, these examples illustrate a couple of things about the diffusion of innovations: first, when they are clearly better than what went before, new ideas of how to do things will usually spread via a “learning by observing” process, and second, the process can take some time; in these cases it took thirty years, and the life cycle of the Macaque monkey is somewhat shorter than ours (Kawai, Watanabe, and Mori 1992). Turning to the world of humans, it is safe to say that without diffusion, innovation would have little social or economic impact. In the study of innovation, the word diffusion is commonly used to describe the process by which individuals and firms in a society/economy adopt a new technology, or replace an older technology with a newer. -

An Empirical Analysis of the Factors Affecting the Adoption and Diffusion of GBTS in the Construction Market
sustainability Article An Empirical Analysis of the Factors Affecting the Adoption and Diffusion of GBTS in the Construction Market Wei Wang 1, Shoujian Zhang 2 , Yikun Su 3,* and Xinyang Deng 4 1 School of Management, Harbin Institute of Technology, Harbin 150001, China; [email protected] 2 School of Civil Engineering, Harbin Institute of Technology, Harbin 150001, China; [email protected] 3 School of Civil Engineering, Northeast Forestry University, Harbin 150040, China 4 State Grid Liaoning Electric Power Company Limited Economic Research Institute, Shenyang 110015, China; [email protected] * Correspondence: [email protected] Received: 25 February 2019; Accepted: 21 March 2019; Published: 25 March 2019 Abstract: This study focuses on better development of green buildings. The key to the sustainable development of the construction industry is to popularize and promote the spread of green building technologies (GBTS) in the construction market. This study integrates the technology acceptance model (TAM) and the innovation diffusion theory (IDT) to analyze and construct the theoretical model of developers’ GBTS adoption behavior from three dimensions, including the individual factor, product factor and interface factor. This paper discusses the mechanism of GBTS adoption and diffusion in the construction market. The data are collected by questionnaire, and the structural equation model (SEM) is used for empirical analysis. The results show that the developers’ perceived usefulness (PU) and perceived ease of use (PEOU) of GBTS, developers’ innovativeness and sense of community at the individual level, competitive advantage at the product level, as well as government structural guarantees and relevant stakeholders at the interface level have a significant positive impact on the adoption of GBTS by developers. -

A Summary of Diffusion of Innovations
Les Robinson | Phone 0414 674 676 | Email [email protected] Web www.enablingchange.com.au | Blog http://enablingchange.posterous.com A summary of Diffusion of Innovations Les Robinson Fully revised and rewritten Jan 2009 Diffusion of Innovations seeks to explain how innovations are taken up in a population. An innovation is an idea, behaviour, or object that is perceived as new by its audience. Diffusion of Innovations offers three valuable insights into the process of social change: - What qualities make an innovation spread successfully. - The importance of peer-peer conversations and peer networks. - Understanding the needs of different user segments. These insights have been tested in more than 6000 research studies and field tests, so they are amongst the most reliable in the social sciences. What qualities make innovations spread? Diffusion of Innovations takes a radically different approach to most other theories of change. Instead of focusing on persuading individuals to change, it sees change as being primarily about the evolution or “reinvention” of products and behaviours so they become better fits for the needs of individuals and groups. In Diffusion of Innovations it is not people who change, but the innovations themselves. Why do certain innovations spread more quickly than others? And why do others fail? Diffusion scholars recognise five qualities that determine the success of an innovation. This work is licensed under the Creative Commons Attribution-Noncommercial-No Derivative Works 2.5 Australia License. To view a copy of this license visit http://creativecommons.org/licenses/by-nc-nd/2.5/au/deed.en Attribution should be made to “Les Robinson www.enablingchange.com.au”. -

Linking Resilience Theory and Diffusion of Innovations Theory to Understand the Potential for Perennials in the U.S
View metadata, citation and similar papers at core.ac.uk brought to you by CORE provided by Digital Repository @ Iowa State University Natural Resource Ecology and Management Natural Resource Ecology and Management Publications 2009 Linking Resilience Theory and Diffusion of Innovations Theory to Understand the Potential for Perennials in the U.S. Corn Belt Ryan C. Atwell Iowa State University Lisa A. Schulte Iowa State University, [email protected] Lynne M. Westphal United States Forest Service Follow this and additional works at: http://lib.dr.iastate.edu/nrem_pubs Part of the Agriculture Commons, Forest Sciences Commons, and the Natural Resources Management and Policy Commons The ompc lete bibliographic information for this item can be found at http://lib.dr.iastate.edu/ nrem_pubs/8. For information on how to cite this item, please visit http://lib.dr.iastate.edu/ howtocite.html. This Article is brought to you for free and open access by the Natural Resource Ecology and Management at Iowa State University Digital Repository. It has been accepted for inclusion in Natural Resource Ecology and Management Publications by an authorized administrator of Iowa State University Digital Repository. For more information, please contact [email protected]. Linking Resilience Theory and Diffusion of Innovations Theory to Understand the Potential for Perennials in the U.S. Corn Belt Abstract In the last 200 yr, more than 80% of the land in the U.S. Corn Belt agro-ecosystem has been converted from natural perennial vegetation to intensive agricultural production of row crops. Despite research showing how re-integration of perennial vegetation, e.g., cover crops, pasture, riparian buffers, and restored wetlands, at strategic landscape positions can bolster declining regional ecosystem functions, the amount of land area devoted to row crop production in the Corn Belt continues to increase. -

The Intellectual Structure and Substance of the Knowledge
Implementation Science BioMed Central Research article Open Access The intellectual structure and substance of the knowledge utilization field: A longitudinal author co-citation analysis, 1945 to 2004 Carole A Estabrooks*1, Linda Derksen2, Connie Winther3, John N Lavis4, Shannon D Scott5, Lars Wallin6 and Joanne Profetto-McGrath7 Address: 1Faculty of Nursing, Third Floor Clinical Sciences Building, University of Alberta, Edmonton, Alberta, Canada, 2Department of Sociology, Vancouver Island University, Nanaimo, British Columbia, Canada, 3Department of Pediatrics, Faculty of Medicine, University of Alberta, Edmonton, Alberta, Canada, 4Department of Clinical Epidemiology and Biostatistics and Department of Political Science, McMaster University, Hamilton, Ontario, Canada, 5Faculty of Nursing, University of Alberta, Edmonton, Alberta, Canada, 6Department of Neurobiology, Care Sciences and Society, Division of Nursing, Karolinska Institute and Clinical Research Utilization (CRU), Karolinska University Hospital, Stockholm, Sweden and 7Faculty of Nursing, University of Alberta, Edmonton, Alberta, Canada Email: Carole A Estabrooks* - [email protected]; Linda Derksen - [email protected]; Connie Winther - [email protected]; John N Lavis - [email protected]; Shannon D Scott - [email protected]; Lars Wallin - [email protected]; Joanne Profetto-McGrath - [email protected] * Corresponding author Published: 13 November 2008 Received: 19 December 2007 Accepted: 13 November 2008 Implementation Science 2008, 3:49 doi:10.1186/1748-5908-3-49 This article is available from: http://www.implementationscience.com/content/3/1/49 © 2008 Estabrooks et al; licensee BioMed Central Ltd. This is an Open Access article distributed under the terms of the Creative Commons Attribution License (http://creativecommons.org/licenses/by/2.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. -

Measuring the Perceived Attributes of Innovation: a Study of Capacitive Switch Technology in Industrially Designed User Interface Controls Aaron B
Eastern Michigan University DigitalCommons@EMU Master's Theses, and Doctoral Dissertations, and Master's Theses and Doctoral Dissertations Graduate Capstone Projects 7-19-2011 Measuring the perceived attributes of innovation: A study of capacitive switch technology in industrially designed user interface controls Aaron B. Stachewicz Follow this and additional works at: http://commons.emich.edu/theses Part of the Science and Technology Studies Commons Recommended Citation Stachewicz, Aaron B., "Measuring the perceived attributes of innovation: A study of capacitive switch technology in industrially designed user interface controls" (2011). Master's Theses and Doctoral Dissertations. 359. http://commons.emich.edu/theses/359 This Open Access Dissertation is brought to you for free and open access by the Master's Theses, and Doctoral Dissertations, and Graduate Capstone Projects at DigitalCommons@EMU. It has been accepted for inclusion in Master's Theses and Doctoral Dissertations by an authorized administrator of DigitalCommons@EMU. For more information, please contact [email protected]. Measuring the Perceived Attributes of Innovation: A Study of Capacitive Switch Technology in Industrially Designed User Interface Controls by Aaron B. Stachewicz, PMP, CMfgE Dissertation Submitted to the College of Technology Eastern Michigan University in partial fulfillment of the requirements for the degree of DOCTOR OF PHILOSOPHY Area of Concentration: Engineering Management Dissertation Committee: Polly Buchanan, PhD - Chair Daniel Fields, PhD - Member Phillip Cardon, PhD - Member Thomas A. Schmitt, PhD - Member July 19, 2011 Ypsilanti, Michigan ii Dedication I dedicate this work to those who are still trying to answer the hardest question in the academic community: What do you want to be when you “grow up”? This age-old question perplexes the young and old. -
Diffusion of Innovations 1 Diffusion of Innovations
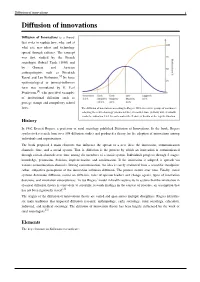
Diffusion of innovations 1 Diffusion of innovations Diffusion of Innovations is a theory that seeks to explain how, why, and at what rate new ideas and technology spread through cultures. The concept was first studied by the French sociologist Gabriel Tarde (1890) and by German and Austrian anthropologists such as Friedrich Ratzel and Leo Frobenius.[1] Its basic epidemiological or internal-influence form was formulated by H. Earl Pemberton,[2] who provided examples of institutional diffusion such as postage stamps and compulsory school laws. The diffusion of innovations according to Rogers. With successive groups of consumers adopting the new technology (shown in blue), its market share (yellow) will eventually reach the saturation level. In mathematics the S curve is known as the logistic function. History In 1962 Everett Rogers, a professor of rural sociology published Diffusion of Innovations. In the book, Rogers synthesized research from over 508 diffusion studies and produced a theory for the adoption of innovations among individuals and organizations. The book proposed 4 main elements that influence the spread of a new idea: the innovation, communication channels, time, and a social system. That is, diffusion is the process by which an innovation is communicated through certain channels over time among the members of a social system. Individuals progress through 5 stages: knowledge, persuasion, decision, implementation, and confirmation. If the innovation is adopted, it spreads via various communication channels. During communication, the idea is rarely evaluated from a scientific standpoint; rather, subjective perceptions of the innovation influence diffusion. The process occurs over time. Finally, social systems determine diffusion, norms on diffusion, roles of opinion leaders and change agents, types of innovation decisions, and innovation consequences. -

The Chasm We Must Cross in Japan for Re-Promotion of the HPV Vaccine a C Yutaka Ueda1, Kayoko Katayama2, Asami Yagi1, and Tadashi Kimura1
CANCER PREVENTION RESEARCH | COMMENTARY The Chasm We Must Cross in Japan for Re-promotion of the HPV Vaccine A C Yutaka Ueda1, Kayoko Katayama2, Asami Yagi1, and Tadashi Kimura1 ABSTRACT ◥ In Japan, the human papillomavirus (HPV) vaccination an important determinate of whether a new product will rate has decreased from around 70% to less than 1% due to penetrate the market. By various initiatives, vaccination repeated media reports of diverse symptoms after HPV coverage has recently risen to about 10%; however, there is vaccination, and to suspension of the governmental recom- still a large chasm difficult to cross before reaching the mendation. The challenges for re-promotion of the vaccine majority of individuals. To cross that chasm, peer education will be discussed from a marketing perspective. The adopter will be essential. First, community health workers will need to categories by which a new product penetrates the market can be educated so that they have a firm understanding of HPV be divided into five groups, including Innovators, Early vaccine and can confidently recommend vaccination to the adopters, Early majority, Late majority, and Laggards. The targeted population. That population will be expected to pass 16.0% line, which is the sum of the percentages of the on that recommendation to their acquaintances, resulting in innovators and the early adopters, is thought to be widening dissemination of HPV vaccine among the majority. In recent years, the incidence of cervical cancer has been gorizes the process by which a new service or product pene- decreasing in developed countries; the same downward trend in trates the market into five groups (Fig. -

Barriers to Innovation in the Field of Medical Devices
WH0/HSS/EHT/DIM/10.6 MedicAl devices: MAnAging the Mismatch An outcome of the Priority Medical Devices project Barriers to innovation in the field of medical devices Background Paper 6 August 2010 Contents Preface 2 Introduction 3 Literature review of innovation diffusion: nature, stages, trends 4 Diffusion of innovation in health care 4 Unpacking the concept of innovation diffusion 5 Critique of the linear model of innovation diffusion 7 The changing composition of the users of new medical devices 8 Trends in medical device development and barriers to innovation 10 Imported versus locally produced medical devices 11 Barriers to medical devices 11 Barriers to innovation in high-resource countries 14 Model for the analysis of barriers to innovation in priority medical devices 16 Several perspectives from the literature 16 Outcomes of the literature review 19 Towards a new model of medical device innovation 21 References 22 2 Medical devices: managing the mismatch—An outcome of the Priority Medical Devices project Preface In 2007, at the request of the Government • projections of future burdens of These problems, challenges, and failures of the Netherlands, the World Health disease and disability in the context of amount to a mismatch, rather than a Organization launched the Priority Medical demographic trends; gap, that prevents medical devices from Devices (PMD) project to determine • cross-cutting issues, such as the training achieving their full public health potential. whether medical devices currently on of medical device users, medical device the global market are meeting the needs design, contextual appropriateness The PMD project also produced a report of health-care providers and patients of medical devices, and regulatory Medical Devices: Managing the Mismatch throughout the world and, if not, to propose oversight; aimed at achieving two objectives: the fi rst, remedial action based on sound research. -

Diffusion of Innovation Theory: a Bridge for the Research–Practice Gap in Counseling Christine E
Reprinted from Journal of Counseling and Development, Winter, Vol. 87 p. 108-116 © (2009) The American Counseling Association. Reprinted with permission. No further reproduction authorized without written permission from the American Counseling Association Diffusion of Innovation Theory: A Bridge for the Research–Practice Gap in Counseling Christine E. Murray This article presents a diffusion of innovation theory–based framework for addressing the gap between research and practice in the counseling profession. The author describes the nature of the research–practice gap and presents an overview of diffusion of innovation theory. On the basis of the application of several major postulates of diffusion of in- novation theory to the research–practice gap, several theory-based research practices and questions are proposed. Getting a new idea adopted, even when it has obvious The Research–Practice Gap advantages, is difficult. —Everett M. Rogers (2003, p. 1) in Counseling Evidence-based counseling practices are necessary to establish Counseling researchers face the challenge of translating their the credibility and effectiveness of counseling interventions findings into meaningful strategies for practice. Scholars have (Bradley et al., 2005), and many external funding agencies identified a major gap between research findings and clinical have begun to mandate an increased use of evidence-based practice (Froehle & Rominger, 1993; Martin & Martin, 1989; practices (Rawson et al., 2002). Researchers have demonstrated Proctor, 2004; Rawson, Marinelli-Casey, & Ling, 2002; D. the effectiveness and efficacy of many counseling-related prac- I. Williams & Irving, 1999). This gap reflects the tendency tices (Proctor, 2004). For decades, however, the counseling for many research findings to go unused, perhaps even un- profession has demonstrated a chasm between the knowledge noticed, by practitioners.