T5 Spinal Cord Injuries
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Spinal Cord Injury and Traumatic Brain Injury Research Grant Program Report 2020
This document is made available electronically by the Minnesota Legislative Reference Library as part of an ongoing digital archiving project. http://www.leg.state.mn.us/lrl/lrl.asp Spinal Cord Injury and Traumatic Brain Injury Research Grant Program Report January 15, 2020 Author About the Minnesota Office of Higher Education Alaina DeSalvo The Minnesota Office of Higher Education is a Competitive Grants Administrator cabinet-level state agency providing students with Tel: 651-259-3988 financial aid programs and information to help [email protected] them gain access to postsecondary education. The agency also serves as the state’s clearinghouse for data, research and analysis on postsecondary enrollment, financial aid, finance and trends. The Minnesota State Grant Program is the largest financial aid program administered by the Office of Higher Education, awarding up to $207 million in need-based grants to Minnesota residents attending eligible colleges, universities and career schools in Minnesota. The agency oversees other state scholarship programs, tuition reciprocity programs, a student loan program, Minnesota’s 529 College Savings Plan, licensing and early college awareness programs for youth. Minnesota Office of Higher Education 1450 Energy Park Drive, Suite 350 Saint Paul, MN 55108-5227 Tel: 651.642.0567 or 800.657.3866 TTY Relay: 800.627.3529 Fax: 651.642.0675 Email: [email protected] Table of Contents Introduction 1 Spinal Cord Injury and Traumatic Brain Injury Advisory Council 1 FY 2020 Proposal Solicitation Schedule -

A Young Adult with Post-Traumatic Breathlessness, Unconsciousness and Rash
Shihan Mahmud Redwanul Huq 1, Ahmad Mursel Anam1, Nayeema Joarder1, Mohammed Momrezul Islam1, Raihan Rabbani2, Abdul Kader Shaikh3,4 [email protected] Case report A young adult with post-traumatic breathlessness, unconsciousness and rash Cite as: Huq SMR, A 23-year-old Bangladeshi male was referred to our with back slab at the previous healthcare facility. Anam AM, Joarder N, et al. hospital for gradual worsening of breathlessness During presentation at the emergency department, A young adult with post- over 3 h, developed following a road-accident he was conscious and oriented (Glasgow coma scale traumatic breathlessness, about 14 h previously. He had a close fracture of 15/15), tachycardic (heart rate 132 per min), blood unconsciousness and rash. mid-shaft of his right tibia, which was immobilised pressure 100/70 mmHg, tachypnoeic (respiratory Breathe 2019; 15: e126–e130. rate 34 per min) with oxygen saturation 89% on room air, and afebrile. Chest examination revealed a) b) restricted chest movement, hyper-resonant percussion notes and reduced breath sound on the left, and diffuse crackles on both sides. He was fit before the accident with no known medical illness. Oxygen supplementation (up to 8 L·min−1) and intravenous fluids were provided as required. Simultaneously, a portable anteroposterior radiograph of chest was performed (figure 1). Task 1 Analyse the chest radiograph. Figure 1 Chest radiography: a) anteroposterior view; b) magnified view of same image showing the clear margin of a pneumothorax on the left-hand side (dots and arrow). @ERSpublications Can you diagnose this young adult with post-traumatic breathlessness, unconsciousness and rash? http://bit.ly/2LlpkiV e126 Breathe | September 2019 | Volume 15 | No 3 https://doi.org/10.1183/20734735.0212-2019 A young adult with post-traumatic breathlessness Answer 1 a) b) The bilateral patchy opacities are likely due to pulmonary contusion or acute respiratory distress syndrome (ARDS) along with the left- sided traumatic pneumothorax. -

Fat Embolism Syndrome
Crit Care & Shock (2008) 11 : 83-93 Fat Embolism Syndrome Gavin M. Joynt, Thomas ST Li, Joey KM Wai, Florence HY Yap Abstract The classical syndrome of fat embolism is recognition as well as the development of preventive characterized by the triad of respiratory failure, and therapeutic strategies. Early fracture fi xation neurologic dysfunction and the presence of a is likely to reduce the incidence of fat embolism petechial rash. Fat embolism syndrome (FES) syndrome and pulmonary complications; however occurs most commonly following orthopedic the best fi xation technique remains controversial. trauma, particularly fractures of the pelvis or long The use of prophylactic corticosteroids may be bones, however non-traumatic fat embolism has considered to reduce the incidence of FES and in also been known to occur on rare occasions. Because selected high-risk trauma patients but effects on no defi nitive consensus on diagnostic criteria exist, outcome are not proved. New reaming and venting the accurate assessment of incidence, comparative techniques have potential to reduce the incidence research and outcome assessment is diffi cult. A of FES during arthroplasty. Unfortunately, no reasonable estimate of incidence in patients after specifi c therapies have been proven to be of benefi t long bone or pelvic fractures appears to be about in FES and treatment remains supportive with 3-5%. The FES therefore remains an important priority being given to the maintenance of adequate cause of morbidity and mortality and warrants oxygenation. further investigation and research to allow proper Key words: respiratory failure, petechiae, rash, trauma, orthopedic, fracture Introduction The classical syndrome of fat embolism is characterized following orthopedic trauma, particularly fractures of by the triad of respiratory failure, neurologic the pelvis or long bones, however non-traumatic fat dysfunction and the presence of a petechial rash [1,2]. -

Neurologic Deterioration Secondary to Unrecognized Spinal Instability Following Trauma–A Multicenter Study
SPINE Volume 31, Number 4, pp 451–458 ©2006, Lippincott Williams & Wilkins, Inc. Neurologic Deterioration Secondary to Unrecognized Spinal Instability Following Trauma–A Multicenter Study Allan D. Levi, MD, PhD,* R. John Hurlbert, MD, PhD,† Paul Anderson, MD,‡ Michael Fehlings, MD, PhD,§ Raj Rampersaud, MD,§ Eric M. Massicotte, MD,§ John C. France, MD, Jean Charles Le Huec, MD, PhD,¶ Rune Hedlund, MD,** and Paul Arnold, MD†† Study Design. A retrospective study was undertaken their neurologic injury. The most common reason for the that evaluated the medical records and imaging studies of missed injury was insufficient imaging studies (58.3%), a subset of patients with spinal injury from large level I while only 33.3% were a result of misread radiographs or trauma centers. 8.3% poor quality radiographs. The incidence of missed Objective. To characterize patients with spinal injuries injuries resulting in neurologic injury in patients with who had neurologic deterioration due to unrecognized spine fractures or strains was 0.21%, and the incidence as instability. a percentage of all trauma patients evaluated was 0.025%. Summary of Background Data. Controversy exists re- Conclusions. This multicenter study establishes that garding the most appropriate imaging studies required to missed spinal injuries resulting in a neurologic deficit “clear” the spine in patients suspected of having a spinal continue to occur in major trauma centers despite the column injury. Although most bony and/or ligamentous presence of experienced personnel and sophisticated im- spine injuries are detected early, an occasional patient aging techniques. Older age, high impact accidents, and has an occult injury, which is not detected, and a poten- patients with insufficient imaging are at highest risk. -

Update on Critical Care for Acute Spinal Cord Injury in the Setting of Polytrauma
NEUROSURGICAL FOCUS Neurosurg Focus 43 (5):E19, 2017 Update on critical care for acute spinal cord injury in the setting of polytrauma *John K. Yue, BA,1,2 Ethan A. Winkler, MD, PhD,1,2 Jonathan W. Rick, BS,1,2 Hansen Deng, BA,1,2 Carlene P. Partow, BS,1,2 Pavan S. Upadhyayula, BA,3 Harjus S. Birk, MD,3 Andrew K. Chan, MD,1,2 and Sanjay S. Dhall, MD1,2 1Department of Neurological Surgery, University of California, San Francisco; 2Brain and Spinal Injury Center, Zuckerberg San Francisco General Hospital, San Francisco; and 3Department of Neurological Surgery, University of California, San Diego, California Traumatic spinal cord injury (SCI) often occurs in patients with concurrent traumatic injuries in other body systems. These patients with polytrauma pose unique challenges to clinicians. The current review evaluates existing guidelines and updates the evidence for prehospital transport, immobilization, initial resuscitation, critical care, hemodynamic stabil- ity, diagnostic imaging, surgical techniques, and timing appropriate for the patient with SCI who has multisystem trauma. Initial management should be systematic, with focus on spinal immobilization, timely transport, and optimizing perfusion to the spinal cord. There is general evidence for the maintenance of mean arterial pressure of > 85 mm Hg during imme- diate and acute care to optimize neurological outcome; however, the selection of vasopressor type and duration should be judicious, with considerations for level of injury and risks of increased cardiogenic complications in the elderly. Level II recommendations exist for early decompression, and additional time points of neurological assessment within the first 24 hours and during acute care are warranted to determine the temporality of benefits attributable to early surgery. -

Posttraumatic Stress Following Spinal Cord Injury: a Systematic Review of Risk and Vulnerability Factors
Spinal Cord (2017) 55, 800–811 & 2017 International Spinal Cord Society All rights reserved 1362-4393/17 www.nature.com/sc REVIEW Posttraumatic stress following spinal cord injury: a systematic review of risk and vulnerability factors K Pollock1,3, D Dorstyn1,3, L Butt2 and S Prentice1 Objectives: To summarise quantitatively the available evidence relating to pretraumatic, peritraumatic and posttraumatic characteristics that may increase or decrease the risk of developing posttraumatic stress disorder (PTSD) following spinal cord injury (SCI). Study design: Systematic review. Methods: Seventeen studies were identified from the PubMed, PsycInfo, Embase, Scopus, CINAHL, Web of Science and PILOTS databases. Effect size estimates (r) with associated 95% confidence intervals (CIs), P-values and fail-safe Ns were calculated. Results: Individual studies reported medium-to-large associations between factors that occurred before (psychiatric history r = 0.48 (95% CI, 0.23–0.79) P = 0.01) or at the time of injury (tetraplegia r = − 0.36 (95% CI, − 0.50 to − 0.19) Po0.01). Postinjury factors had the strongest pooled effects: depressed mood (rw = 0.64, (95% CI, 0.54–0.72)), negative appraisals (rw = 0.63 (95% CI, 0.52– 0.72)), distress (rw = 0.57 (95% CI, 0.50–0.62)), anxiety (rw = 0.56 (95% CI, 0.49–0.61)) and pain severity (rw = 0.35 (95% CI, 0.27– 0.43)) were consistently related to worsening PTSD symptoms (Po0.01). Level of injury significantly correlated with current PTSD severity for veteran populations (QB (1) = 18.25, Po0.001), although this was based on limited data. -

Femoral Shaft Fracture Fixation and Chest Injury After Polytrauma
This is an enhanced PDF from The Journal of Bone and Joint Surgery The PDF of the article you requested follows this cover page. Femoral Shaft Fracture Fixation and Chest Injury After Polytrauma Lawrence B. Bone and Peter Giannoudis J Bone Joint Surg Am. 2011;93:311-317. doi:10.2106/JBJS.J.00334 This information is current as of January 25, 2011 Reprints and Permissions Click here to order reprints or request permission to use material from this article, or locate the article citation on jbjs.org and click on the [Reprints and Permissions] link. Publisher Information The Journal of Bone and Joint Surgery 20 Pickering Street, Needham, MA 02492-3157 www.jbjs.org 311 COPYRIGHT Ó 2011 BY THE JOURNAL OF BONE AND JOINT SURGERY,INCORPORATED Current Concepts Review Femoral Shaft Fracture Fixation and Chest Injury After Polytrauma By Lawrence B. Bone, MD, and Peter Giannoudis, MD, FRCS Thirty years ago, the standard of care for the multiply injured tients with multiple injuries, defined as an ISS of ‡18, and patient with fractures was placement of the fractured limb in a patients with essentially an isolated femoral fracture and an splint or skeletal traction, until the patient was considered stable ISS of <18. Pulmonary complications consisting of ARDS, enough to undergo surgery for fracture fixation1. This led to a pulmonary dysfunction, fat emboli, pulmonary emboli, and number of complications2, such as adult respiratory distress pneumonia were present in 38% (fourteen) of thirty-seven syndrome (ARDS), infection, pneumonia, malunion, non- patients in the late fixation/multiple injuries group and 4% union, and death, particularly when the patient had a high (two) of forty-six in the early fixation/multiple injuries group; Injury Severity Score (ISS)3. -

Amc Trauma Practice Management Guidelines: Traumatic Brian Injury
AMC TRAUMA PRACTICE MANAGEMENT GUIDELINES: TRAUMATIC BRIAN INJURY Original 10/2018 Revised 1/2020 AMC TRAUMA PRACTICE MANAGEMENT GUIDELINES: TRAUMATIC BRIAN INJURY Purpose: Neurotrauma care must be continuously available for all TRAUMATIC BRIAN INJURY (TBI) and Spinal Cord Injury patients. SUPPORTIVE DATA Policy Statements: Neurosurgical providers must respond and be present for consultation and management decisions for patients with TBI or spinal cord injury within 30 minutes of consultation by the Trauma Service based on institution specific criteria. Neurosurgery Attending will arrive within 30 minutes for decreasing GCS with midline shift requiring operative decompression. Institution Specific Criteria and Definitions: TBI Initial Encounter Codes S06.1 Traumatic Cerebral Edema S06.2 Diffuse Traumatic Brain Injury S06.3 Focal Traumatic Brain Injury S06.4 Epidural Hemorrhage S06.5 Traumatic Subdural Hemorrhage S06.6 Traumatic Subarachnoid Hemorrhage S06.8 Other Specified Intracranial Injuries S06.9 Unspecified Intracranial Injury Spinal Cord Injury Cervical Initial Encounter Codes S14.0xxa Concussion and Edema of Cervical Spinal Cord, Initial Encounter S14.1 Other and Unspecified Injuries of Cervical Spinal Cord Spinal Cord Injury Thoracic Initial Encounter Codes S24.0xxa Concussion and Edema of Thoracic Spinal Cord, Initial Encounter S24.1 Other and Unspecified Injuries of Thoracic Spinal Cord Lumbar & Sacral Initial Encounter Codes S34.0 Concussion and Edema of Lumbar and Sacral Spinal Cord S34.1 Other and Unspecified Injury of Lumbar and Sacral Spinal Cord S34.3xxa Injury of Cauda Equina, Initial Encounter Background: The following clinical practice guidelines for management of traumatic brain injury were abstracted directly from the Brain Trauma Foundation’s Guidelines for the Management of Severe Traumatic Brain Injury 4th Edition. -

Predictors of Clinical Complications in Patients with Spinomedullary Injury Preditores De Complicações Clínicas Em Pacientes Com Trauma Raquimedular
ORIGINAL ARTICLE/ARTIGO ORIGINAL/ARTÍCULO ORIGINAL PREDICTORS OF CLINICAL COMPLICATIONS IN PATIENTS WITH SPINOMEDULLARY INJURY PREDITORES DE COMPLICAÇÕES CLÍNICAS EM PACIENTES COM TRAUMA RAQUIMEDULAR PREDICTORES DE COMPLICACIONES EN PACIENTES CON TRAUMA RAQUIMEDULAR DIONEI FREITAS DE MORAIS1, JOÃO SIMÃO DE MELO NETO2, ANTONIO RONALdo SPOTTI1, WALDIR ANTONIO TOGNOLA1 ABSTRACT Objective: To analyze individuals with spinal cord injury who developed secondary clinical complications, and the variables that can influence the prog- nosis. Methods: A prospective study of 321 patients with spinal cord injury. The variables were collected: age, sex, cause of the accident, anatomical distribution, neurological status, associated injuries, in-hospital complications, and mortality only in patients who developed complications. Results: A total of 72 patients were analyzed (85% male) with a mean age of 44.72±19.19 years. The individuals with spinal cord injury who developed clinical complications were mostly male, over 50 years of age, and the main cause was accidental falls. These patients had longer hospitalization times and a higher risk of progressing to death. Pneumonia was the main clinical complication. With regard to the variables that can influence the prognosis of these patients, it was observed that spinal cord injury to the cervical segment with syndromic quadriplegia, and neurological status ASIA-A, have a higher risk of developing pneumonia, the most common complication, as well as increased mortality. Conclusion: Clinical complications secondary to spinal cord injury are influenced by demographic factors, as well as characteristics of the injury contributing to an increase in mortality. Keywords: Spinal cord injuries/complications; Spinal injuries; Mortality. RESUMO Objetivo: Analisar pacientes de um hospital terciário com trauma raquimedular que evoluíram com complicações clínicas intra-hospitalares, bem como as variáveis que podem interferir no prognóstico. -

A Patient with Severe Polytrauma with Massive Pulmonary Contusion And
Nagashima et al. Journal of Medical Case Reports (2020) 14:69 https://doi.org/10.1186/s13256-020-02406-9 CASE REPORT Open Access A patient with severe polytrauma with massive pulmonary contusion and hemorrhage successfully treated with multiple treatment modalities: a case report Futoshi Nagashima*†, Satoshi Inoue† and Miho Ohta Abstract Background: The mortality rate is very high for patients with severe multiple trauma with massive pulmonary contusion containing intrapulmonary hemorrhage. Multiple treatment modalities are needed not only for a prevention of cardiac arrest and quick hemostasis against multiple injuries, but also for recovery of oxygenation to save the patient’s life. Case presentation: A 48-year-old Japanese woman fell down stairs that had a height of approximately 4 m. An X- ray showed pneumothorax, pulmonary contusion in her right lung, and an unstable pelvic fracture. A chest drain was inserted and preperitoneal pelvic packing was performed to control bleeding, performing resuscitative endovascular balloon occlusion of the aorta. A computed tomography scan revealed massive lung contusion in the lower lobe of her right lung, pelvic fractures, and multiple fractures and hematoma in other areas. An emergency thoracotomy was performed, and then we performed wide wedge resection of the injured lung, clamping proximal to suture lines with two Satinsky blood vessel clamps. The vessel clamps were left in the right thoracic cavity. The other hemorrhagic areas were embolized by transcatheter arterial embolization. However, since her respiratory functions deteriorated in the intensive care unit, veno-venous extracorporeal membrane oxygenation was used for lung assist. Planned reoperation under veno-venous extracorporeal membrane oxygenation was performed on day 2. -

Blast Injuries – Essential Facts
BLAST INJURIES Essential Facts Key Concepts • Bombs and explosions can cause unique patterns of injury seldom seen outside combat • Expect half of all initial casualties to seek medical care over a one-hour period • Most severely injured arrive after the less injured, who bypass EMS triage and go directly to the closest hospitals • Predominant injuries involve multiple penetrating injuries and blunt trauma • Explosions in confined spaces (buildings, large vehicles, mines) and/or structural collapse are associated with greater morbidity and mortality • Primary blast injuries in survivors are predominantly seen in confined space explosions • Repeatedly examine and assess patients exposed to a blast • All bomb events have the potential for chemical and/or radiological contamination • Triage and life saving procedures should never be delayed because of the possibility of radioactive contamination of the victim; the risk of exposure to caregivers is small • Universal precautions effectively protect against radiological secondary contamination of first responders and first receivers • For those with injuries resulting in nonintact skin or mucous membrane exposure, hepatitis B immunization (within 7 days) and age-appropriate tetanus toxoid vaccine (if not current) Blast Injuries Essential Facts • Primary: Injury from over-pressurization force (blast wave) impacting the body surface — TM rupture, pulmonary damage and air embolization, hollow viscus injury • Secondary: Injury from projectiles (bomb fragments, flying debris) — Penetrating trauma, -
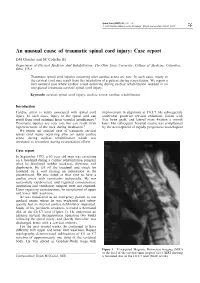
An Unusual Cause of Traumatic Spinal Cord Injury: Case Report
Spinal Cord (1997) 35, 181 ± 182 1997 International Medical Society of Paraplegia All rights reserved 1362 ± 4393/97 $12.00 An unusual cause of traumatic spinal cord injury: Case report DM Clinchot and SC Colachis III Department of Physical Medicine And Rehabilitation, The Ohio State University, College of Medicine, Columbus, Ohio, USA Traumatic spinal cord injuries occurring after cardiac arrest are rare. In such cases, injury to the cervical cord may result from the intubation of a patient during resuscitation. We report a very unusual case where cardiac arrest occurring during cardiac rehabilitation resulted in an unexpected traumatic cervical spinal cord injury. Keywords: cervical spinal cord injury; cardiac arrest; cardiac rehabilitation Introduction Cardiac arrest is rarely associated with spinal cord improvement in alignment at C6/C7. He subsequently injury. In such cases, injury to the spinal cord can underwent posterior cervical reduction, fusion with result from cord ischemia from vascular insuciency.1 iliac bone graft, and lateral mass ®xation a month Traumatic injuries are very rare but can result from later. His subsequent hospital course was complicated hyperextension of the neck during intubation.2 by the development of rapidly progressive neurological We report an unusual case of traumatic cervical spinal cord injury occurring after an acute cardiac arrest during cardiac rehabilitation which was unrelated to treatment during resuscitation eorts. Case report In September 1993, a 63 year old man was exercising on a treadmill during a cardiac rehabilitation program when he developed sudden weakness, dizziness, and diaphoresis. He fell o the treadmill and struck his forehead on a wall causing an indentation in the plasterboard.