Perphenazine (Trilafon)
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Papers and Originals
BRITISH MEDICAL JOURNAL 19 FEBRUARY 1972 463 PAPERS AND ORIGINALS Drug Interaction: Inhibitory Effect of Neuroleptics on Metabolism of Tricyclic Antidepressants in Man LARS F. GRAM, KERSTIN FREDRICSON OVERO British Medical Journal, 1972, 1, 463-465 excretion (Anders, 1971). There are relatively few reports on interaction concerning neuroleptics or tricyclic antidepressants. Summary Chlorpromazine has both stimulatory and inhibitory effects on the metabolism of hexobarbitone in Total urinary excretion of radioactivity after oral or experimental animals of a test of (Riimke and Bout, 1960-1). Furthermore, chlorpromazine intravenous administration dose '4C-imi- accelerates the metabolism pramine was measured in were tested ofmeprobamate (Kato and Vassanelli, eight patients. They 1962). Tricyclic antidepressants have been shown to inhibit the before, during, and after treatment with neuroleptics. metabolism Excretion diminished while the were of tremorine and oxotremorine in rats in vitro and patients being in vivo (Hammer and Sjoqvist, 1967). It has also been found treated with perphenazine, haloperidol, or chlorproma- that zine, not treatment. desipramine hydrochloride inhibits the metabolism of though during flupenthixol amphetamine in isolated, perfused rat liver (Dingell and Bass, Total urinary excretion of radioactivity and plasma 1969). Pretreatment levels of metabolites and were measured with phenobarbitone decreased steady-state unchanged drug plasma levels of desipramine and nortriptyline in man (Sjoqvist in five patients after a test dose of 14C-nortriptyline. Each et was before and al. 1968). These findings were later confirmed in a twin study patient tested again during perphenazine (Alexanderson et al., 1969). Forrest et treatment. In all patients perphenazine treatment caused: al. (1970) found increased (1) decrease of total urinary excretion, (2) decreased urinary excretion of chlorpromazine metabolites when patients plasma level of metabolites, and (3) increased plasma were given additional treatment with phenobarbitone. -
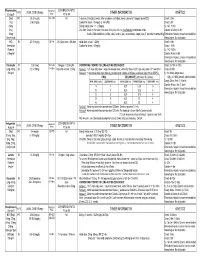
Medication Conversion Chart
Fluphenazine FREQUENCY CONVERSION RATIO ROUTE USUAL DOSE (Range) (Range) OTHER INFORMATION KINETICS Prolixin® PO to IM Oral PO 2.5-20 mg/dy QD - QID NA ↑ dose by 2.5mg/dy Q week. After symptoms controlled, slowly ↓ dose to 1-5mg/dy (dosed QD) Onset: ≤ 1hr 1mg (2-60 mg/dy) Caution for doses > 20mg/dy (↑ risk EPS) Cmax: 0.5hr 2.5mg Elderly: Initial dose = 1 - 2.5mg/dy t½: 14.7-15.3hr 5mg Oral Soln: Dilute in 2oz water, tomato or fruit juice, milk, or uncaffeinated carbonated drinks Duration of Action: 6-8hr 10mg Avoid caffeinated drinks (coffee, cola), tannics (tea), or pectinates (apple juice) 2° possible incompatibilityElimination: Hepatic to inactive metabolites 5mg/ml soln Hemodialysis: Not dialyzable HCl IM 2.5-10 mg/dy Q6-8 hr 1/3-1/2 po dose = IM dose Initial dose (usual): 1.25mg Onset: ≤ 1hr Immediate Caution for doses > 10mg/dy Cmax: 1.5-2hr Release t½: 14.7-15.3hr 2.5mg/ml Duration Action: 6-8hr Elimination: Hepatic to inactive metabolites Hemodialysis: Not dialyzable Decanoate IM 12.5-50mg Q2-3 wks 10mg po = 12.5mg IM CONVERTING FROM PO TO LONG-ACTING DECANOATE: Onset: 24-72hr (4-72hr) Long-Acting SC (12.5-100mg) (1-4 wks) Round to nearest 12.5mg Method 1: 1.25 X po daily dose = equiv decanoate dose; admin Q2-3wks. Cont ½ po daily dose X 1st few mths Cmax: 48-96hr 25mg/ml Method 2: ↑ decanoate dose over 4wks & ↓ po dose over 4-8wks as follows (accelerate taper for sx of EPS): t½: 6.8-9.6dy (single dose) ORAL DECANOATE (Administer Q 2 weeks) 15dy (14-100dy chronic administration) ORAL DOSE (mg/dy) ↓ DOSE OVER (wks) INITIAL DOSE (mg) TARGET DOSE (mg) DOSE OVER (wks) Steady State: 2mth (1.5-3mth) 5 4 6.25 6.25 0 Duration Action: 2wk (1-6wk) Elimination: Hepatic to inactive metabolites 10 4 6.25 12.5 4 Hemodialysis: Not dialyzable 20 8 6.25 12.5 4 30 8 6.25 25 4 40 8 6.25 25 4 Method 3: Admin equivalent decanoate dose Q2-3wks. -

Schizophrenia Care Guide
August 2015 CCHCS/DHCS Care Guide: Schizophrenia SUMMARY DECISION SUPPORT PATIENT EDUCATION/SELF MANAGEMENT GOALS ALERTS Minimize frequency and severity of psychotic episodes Suicidal ideation or gestures Encourage medication adherence Abnormal movements Manage medication side effects Delusions Monitor as clinically appropriate Neuroleptic Malignant Syndrome Danger to self or others DIAGNOSTIC CRITERIA/EVALUATION (PER DSM V) 1. Rule out delirium or other medical illnesses mimicking schizophrenia (see page 5), medications or drugs of abuse causing psychosis (see page 6), other mental illness causes of psychosis, e.g., Bipolar Mania or Depression, Major Depression, PTSD, borderline personality disorder (see page 4). Ideas in patients (even odd ideas) that we disagree with can be learned and are therefore not necessarily signs of schizophrenia. Schizophrenia is a world-wide phenomenon that can occur in cultures with widely differing ideas. 2. Diagnosis is made based on the following: (Criteria A and B must be met) A. Two of the following symptoms/signs must be present over much of at least one month (unless treated), with a significant impact on social or occupational functioning, over at least a 6-month period of time: Delusions, Hallucinations, Disorganized Speech, Negative symptoms (social withdrawal, poverty of thought, etc.), severely disorganized or catatonic behavior. B. At least one of the symptoms/signs should be Delusions, Hallucinations, or Disorganized Speech. TREATMENT OPTIONS MEDICATIONS Informed consent for psychotropic -

Opipramol and Trifluoperazine in the Treatment of Anxiety and Tension
A COMPARATIVE STUDY OF TWO ANTIHISTAMINES 395 In table VI are given the results of a question directed at discovering how effective the preferred treatment was compared to any other antihistamine used. Fifteen patients only were able to give this information but the results are interesting. Discussion TABLE VI The design of this study was very simple as COMPARISON WITH PREVIOUSLY USED ANTIHISTAMINE such studies must be if they are to be completed under the conditions of a busy general practice. In a condition such as hay fever where anti- Worse As good Better Total histamines are known to be etfective and where fairly rapid symptomatic relief is needed by the 2 4 9 15* patient, we did not feel justified in including a placebo. The results of the study seem fairly *In the majority of patients the previously used clear-cut that if patients are offered the choice antihistamine was the chemically related chlor- of a plain form of this antihistamine or a long- pheniramine maleate B.P. acting form more will choose the latter. Ofthose that do so, however, only about a third find a single tablet at night completely effective, the remainder have to take one further tablet during the day. Both forms of antihistamine are effective and where a retrospective comparison can be made this effectiveness is considered greater or equal to that of previously administered anti-histamines. Summary A simple comparative study under general-practice conditions of two formulations of pheniramine is described. Sixty-one per cent of patients preferred the long-acting form of this antihistamine. -

Is Aristada (Aripiprazole Lauroxil) a Safe and Effective Treatment for Schizophrenia in Adult Patients? Kyle J
Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Student Dissertations, Theses and Papers Scholarship 2017 Is Aristada (Aripiprazole Lauroxil) a Safe and Effective Treatment For Schizophrenia In Adult Patients? Kyle J. Knowles Philadelphia College of Osteopathic Medicine Follow this and additional works at: https://digitalcommons.pcom.edu/pa_systematic_reviews Part of the Psychiatry Commons Recommended Citation Knowles, Kyle J., "Is Aristada (Aripiprazole Lauroxil) a Safe and Effective Treatment For Schizophrenia In Adult Patients?" (2017). PCOM Physician Assistant Studies Student Scholarship. 381. https://digitalcommons.pcom.edu/pa_systematic_reviews/381 This Selective Evidence-Based Medicine Review is brought to you for free and open access by the Student Dissertations, Theses and Papers at DigitalCommons@PCOM. It has been accepted for inclusion in PCOM Physician Assistant Studies Student Scholarship by an authorized administrator of DigitalCommons@PCOM. For more information, please contact [email protected]. Is Aristada (Aripiprazole Lauroxil) a Safe and Effective Treatment For Schizophrenia In Adult Patients? Kyle J. Knowles, PA-S A SELECTIVE EVIDENCE BASED MEDICINE REVIEW In Partial Fulfillment of the Requirements For The Degree of Master of Science In Health Sciences- Physician Assistant Department of Physician Assistant Studies Philadelphia College of Osteopathic Medicine Philadelphia, Pennsylvania December 16, 2016 ABSTRACT OBJECTIVE: The objective of this selective EBM review is to determine whether or not “Is Aristada (aripiprazole lauroxil) a safe and effective treatment for schizophrenia in adult patients?” STUDY DESIGN: Review of three randomized controlled studies. All three trials were conducted between 2014 and 2015. DATA SOURCES: One randomized, controlled trial and two randomized, controlled, double- blind trials found via Cochrane Library and PubMed. -

Appendix 18: References to Studies from the Previous Guideline
Appendix 18: References to studies from the previous guideline This appendix contains references to the studies from the previous guideline, as they appeared in that guideline. References to studies added to the guideline update are in Appendix 17a-d. Contents Service references…………………………………………………………………..1 Psychology references……………………………………………………………..15 Pharmacology references………………………………………………………….28 Service references Araya2003 {published data only} Araya R, Rojas G, Fritsch R, Gaete J, Rojas M, Simon G, Peters TJ. Treating depression in primary care in low-income women in Santiago, Chile: A randomised controlled trial. Lancet 2003;361(9362):995-1000. Arthur2002 {published data only} Arthur AJ, Jagger C, Lindesay J, Matthews RJ. Evaluating a mental health assessment for older people with depressive symptoms in general practice: a randomised controlled trial. British Journal of General Practice 2002;52(476):202-207. Austin-Los Angeles Austin NK, Liberman RP, King LW, DeRisi WJ. A comparative evaluation of two day hospitals. Goal attainment scaling of behaviour therapy vs. milieu therapy. Journal of Nervous and Mental Disease 1976;163:253-62. Azim-Alberta Azim HF, Weiden TD, Ratcliffe WD, Nutter RW, Dyck RJ, Howarth BG. Current utilization of day hospitalization. Canadian Psychiatric Association Journal 1978;23:557-66 Baker2001 {published data only} Baker R, Reddish S, Robertson N, Hearnshaw H, Jones B. Randomised controlled trial of tailored strategies to implement guidelines for the management of patients with depression in general practice. British Journal of General Practice 2001;51:737-741. Barkley-Ontario Barkley AL, Fagen K, Lawson JS. Day care: can it prevent readmission to a psychiatric hospital? Psychiatric Journal of the University of Ottawa 1989;14:536-41. -

PERPHENAZINE and AMITRIPTYLINE HYDROCHLORIDE- Perphenazine and Amitriptyline Hydrochloride Tablet, Film Coated Mylan Pharmaceuticals Inc
PERPHENAZINE AND AMITRIPTYLINE HYDROCHLORIDE- perphenazine and amitriptyline hydrochloride tablet, film coated Mylan Pharmaceuticals Inc. ---------- WARNING Increased Mortality in Elderly Patients with Dementia-Related Psychosis Elderly patients with dementia-related psychosis treated with antipsychotic drugs are at an increased risk of death. Analyses of seventeen placebo-controlled trials (modal duration of 10 weeks), largely in patients taking atypical antipsychotic drugs, revealed a risk of death in drug-treated patients of between 1.6 to 1.7 times the risk of death in placebo-treated patients. Over the course of a typical 10-week controlled trial, the rate of death in drug- treated patients was about 4.5%, compared to a rate of about 2.6% in the placebo group. Although the causes of death were varied, most of the deaths appeared to be either cardiovascular (e.g., heart failure, sudden death) or infectious (e.g., pneumonia) in nature. Observational studies suggest that, similar to atypical antipsychotic drugs, treatment with conventional antipsychotic drugs may increase mortality. The extent to which the findings of increased mortality in observational studies may be attributed to the antipsychotic drug as opposed to some characteristic(s) of the patients is not clear. Perphenazine and amitriptyline hydrochloride is not approved for the treatment of patients with dementia- related psychosis (see WARNINGS). Suicidality and Antidepressant Drugs Antidepressants increased the risk compared to placebo of suicidal thinking and behavior (suicidality) in children, adolescents and young adults in short-term studies of major depressive disorder (MDD) and other psychiatric disorders. Anyone considering the use of perphenazine and amitriptyline or any other antidepressant in a child, adolescent, or young adult must balance this risk with the clinical need. -

Perphenazine Medical Facts from Drugs.Com Visited 10/07/2015
Perphenazine medical facts from Drugs.com http://www.drugs.com/mtm/perphenazine.html Visited 10/07/2015 Generic Name: perphenazine (per FEN a zeen) Brand Name: Trilafon What is perphenazine? Perphenazine is an anti-psychotic medicine in a group of drugs called phenothiazines (FEEN-oh-THYE-a-zeens). It works by changing the actions of chemicals in your brain. Perphenazine is used to treat psychotic disorders such as schizophrenia. It is also used to control severe nausea and vomiting. Perphenazine may also be used for purposes not listed in this medication guide. What is the most important information I should know about perphenazine? You should not use perphenazine if you have liver disease, brain damage, bone marrow depression, a blood cell disorder, or if you are also using large amounts of alcohol or medicines that make you sleepy. Call your doctor at once if you have twitching or uncontrollable movements of your eyes, lips, tongue, face, arms, or legs. These could be early signs of dangerous side effects. What should I discuss with my healthcare provider before taking perphenazine? You should not use this medicine if you are allergic to any phenothiazine (perphenazine, chlorpromazine, prochlorperazine, promethazine, thioridazine, Compazine, Phenergan, Mellaril, Thorazine, and others), or if you have: liver disease; brain damage; bone marrow depression; a blood cell disorder (such as low platelets or low red or white blood cell counts); or if you are also using large amounts of alcohol or medicines that make you sleepy. Perphenazine is not approved for use in psychotic conditions related to dementia. Perphenazine may increase the risk of death in older adults with dementia-related conditions. -

Perphenazine-151548-PI.Pdf
PRESCRIBING INFORMATION PERPHENAZINE Perphenazine Tablets USP 2 mg , 4 mg, 8mg, and 16 mg Antipsychotic/Antiemetic AA Pharma Inc. DATE OF REVISION: April 12, 2012 1165 Creditsone Road, Unit #1 Vaughan, Ontario L4K 4N7 Control Number: 151548 PRESCRIBING INFORMATION PERPHENAZINE Perphenazine Tablets USP 2 mg, 4 mg, 8 mg and 16 mg THERAPEUTIC CLASSIFICATION Antipsychotic/Antiemetic ACTIONS AND CLINICAL PHARMACOLOGY Perphenazine is a piperazine phenothiazine derivative with antipsychotic, antiemetic and weak sedative activity. Perphenazine has actions similar to those of other phenothiazine derivatives but appears to be less sedating and to have a weak propensity for causing hypotension or potentiating the effects of CNS depressants and anesthetics. However, it produces a high incidence of extrapyramidal reactions. Perphenazine is well absorbed from the gastrointestinal tract. Onset of action following oral administration is 30 to 40 minutes. Duration of action is 3 to 4 hours. Perphenazine distributes to most body tissues with high concentrations being distributed into liver and spleen. Perphenazine enters the enterohepatic circulation and is excreted chiefly in the feces. INDICATIONS AND CLINICAL USE Perphenazine is indicated in the management of manifestations of psychotic disorders. It is also effective in controlling nausea and vomiting due to stimulation of the chemoreceptor trigger zone. 1 Perphenazine has not been shown effective for the management of behavioral complications in patients with mental retardation. CONTRAINDICATIONS Should not be administered in the presence of circulatory collapse, altered states of consciousness or comatose states, particularly when these are due to intoxication with central depressant drugs (alcohol, hypnotics, narcotics). It is contraindicated in severely depressed patients, in the presence of blood dyscrasias, liver disease, renal insufficiency, pheochromocytoma, or in patients with severe cardiovascular disorders or a history of hypersensitivity to phenothiazine derivatives. -

Reversible and Irreversible Dyskinesia After Treatment with Perphenazine, Chlorpromazine, Reserpine and Eleetroeonvulsive Therapy* by L
Psychopharmacologia 1,408--418 (1960) From St. Hans Mental Hospital, Department D., Roskflde, Denmark (A. FAVl~B:Z~,M.D.) Reversible and Irreversible Dyskinesia after Treatment with Perphenazine, Chlorpromazine, Reserpine and Eleetroeonvulsive Therapy* By L. UnRnaANO and A. FAURBYE With 1 Figure in the Text (Received March 5, 1960) Neurological symptoms are often observed as side effects in the treatment of psychoses with psychopharmaca. Such neurological sym- ptoms have hitherto been considered as a minor inconvenience because they disappeared after reduction of the dose or cessation of the treat- ment but now we have observed that neurological symptoms may persist as irreversible phenomena after cessation of the treatment. The neurological symptoms which we have observed being irrevers- ible in some cases is a syndrome (bucco-linguo-mast~catory dyskinesia) consisting of incessant involuntary munching and masticatory move- ments of the jaw during which the tongue is protruded at short intervals with vigorous grimaces of the lips (see Fig. 1). In the most serious cases there are also rocking and torsionary body movements and in- cessant tripping and shuffling movements so that the patient can not stand still. SuA~o~ et al. (1957) have noted in patients treated with perphena- zinc occasional stiffness of the face and neck muscles together with protrusion of the tongue. The attacks disappeared after stopping per- phenazine, reduction of the dose or administration of barbituric acid compounds. CHmSTIAN and PAVLSE~ (1958) describe the case of a patient who was treated with small doses of prochlorperazine (stemetil). On the third day of treatment an alarming state developed with protrusion of the tongue, spasms of the neck muscles, and later on opisthotonus and increasing respiratory trouble. -

Trilafon Tablets & Trilafon Injection Final Printed Labeling
PAGE 1 TRILAFON TABLETS & TRILAFON INJECTION FINAL PRINTED LABELING 1 TRILAFON Ò 2 brand of perphenazine, USP 3 Tablets, 4 Injection 5 6 DESCRIPTION TRILAFON products contain perphenazine, USP (4-[3-(2- 7 chlorophenothiazin-10-yl)propyl]-1-piper-azineethanol), a piperazinyl phenothiazine 8 having the chemical formula, C21H26CIN3OS. They are available as Tablets, 2, 4, 9 8, and 16 mg; and Injection, perphenazine 5 mg per 1 mL. 10 The inactive ingredients for TRILAFON Tablets, 2, 4, 8, and 16 mg, include: 11 acacia, black iron oxide, butylparaben, calcium phosphate, calcium sulfate, 12 carnauba wax, corn starch, lactose, magnesium stearate, sugar, titanium dioxide, 13 and white wax. The inactive ingredients for TRILAFON Injection include: citric 14 acid, sodium bisulfite, sodium hydroxide, and water. 15 ACTIONS Perphenazine has actions at all levels of the central nervous system, 16 particularly the hypothalamus. However, the site and mechanism of action of 17 therapeutic effect are not known. 18 CLINICAL PHARMACOLOGY Pharmacokinetics: Following oral administration 19 of TRILAFON® Tablets, mean peak plasma perphenazine concentrations were 20 observed between 1 to 3 hours. The plasma elimination half-life of perphenazine 21 was independent of dose and ranged between 9 and 12 hours. In a study in which 22 normal volunteers (n=12) received TRILAFON 4 mg q8h for 5 days, steady-state 23 concentrations of perphenazine were reached within 72 hours. Mean (%CV) Cmax 24 and Cmin values for perphenazine and 7-hydroxyperphenazine at steady-state are 25 listed below: 26 ParameterPerphenazine 7-Hydroxyperphenazine 27 Cmax (pg/mL) 984 (43) 509 (25) 28 Cmin (pg/mL) 442 (76) 350 (56) 1 PAGE 2 TRILAFON TABLETS & TRILAFON INJECTION FINAL PRINTED LABELING 29 Peak 7-hydroxyperphenazine concentrations were observed between 2 to 4 hours 30 with a terminal phase half-life ranging between 9.9 to 18.8 hours. -

Medications to Be Avoided Or Used with Caution in Parkinson's Disease
Medications To Be Avoided Or Used With Caution in Parkinson’s Disease This medication list is not intended to be complete and additional brand names may be found for each medication. Every patient is different and you may need to take one of these medications despite caution against it. Please discuss your particular situation with your physician and do not stop any medication that you are currently taking without first seeking advice from your physician. Most medications should be tapered off and not stopped suddenly. Although you may not be taking these medications at home, one of these medications may be introduced while hospitalized. If a hospitalization is planned, please have your neurologist contact your treating physician in the hospital to advise which medications should be avoided. Medications to be avoided or used with caution in combination with Selegiline HCL (Eldepryl®, Deprenyl®, Zelapar®), Rasagiline (Azilect®) and Safinamide (Xadago®) Medication Type Medication Name Brand Name Narcotics/Analgesics Meperidine Demerol® Tramadol Ultram® Methadone Dolophine® Propoxyphene Darvon® Antidepressants St. John’s Wort Several Brands Muscle Relaxants Cyclobenzaprine Flexeril® Cough Suppressants Dextromethorphan Robitussin® products, other brands — found as an ingredient in various cough and cold medications Decongestants/Stimulants Pseudoephedrine Sudafed® products, other Phenylephrine brands — found as an ingredient Ephedrine in various cold and allergy medications Other medications Linezolid (antibiotic) Zyvox® that inhibit Monoamine oxidase Phenelzine Nardil® Tranylcypromine Parnate® Isocarboxazid Marplan® Note: Additional medications are cautioned against in people taking Monoamine oxidase inhibitors (MAOI), including other opioids (beyond what is mentioned in the chart above), most classes of antidepressants and other stimulants (beyond what is mentioned in the chart above).