Physical Assessment of the Newborn: Part 2
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-
CLAPA Adults Conference
Adults Cleft Conference Camden Lock, London, England Saturday 17 November 2018 The Cleft Lip and Palate Association (CLAPA) is the only national charity supporting people and families affected by cleft lip and/or palate in the UK from diagnosis through to adulthood. Timetable • • • • • • • • • • • • • • • • What’s today all about? • • • • Some ground rules and caveats • • • • • About the Adult Services Project • There are an estimated 75,000 people over the age of 16 living in the United Kingdom who were born with a cleft. • Understanding and supporting the unique needs and experiences of adults affected by cleft is very important to CLAPA. • From March 2018-February 2021, CLAPA is undertaking an exciting project looking at improving services for adults who were born with a cleft funded by the VTCT Foundation. • The goals are to research and understand the experiences, challenges and unmet needs of adults in the UK who were born with a cleft lip and/or palate. • The Adult Services Coordinator is the primary contact for this piece of work. What we did in Year One • • • • • So…what did we find at the roadshow? • We were humbled by how candidly people shared some of their most pivotal moments with us. • As you would expect, there were many different (oftentimes unique) experiences in the community, however there were some common themes that came up many times – these included: • The struggle of obtaining a successful referral to the cleft team as an adult • Being unsure what to expect at cleft team appointments • Not knowing (and health -

Oral Lichen Planus: a Case Report and Review of Literature
Journal of the American Osteopathic College of Dermatology Volume 10, Number 1 SPONSORS: ',/"!,0!4(/,/'9,!"/2!4/29s-%$)#)3 March 2008 34)%&%,,!"/2!4/2)%3s#/,,!'%.%8 www.aocd.org Journal of the American Osteopathic College of Dermatology 2007-2008 Officers President: Jay Gottlieb, DO President Elect: Donald Tillman, DO Journal of the First Vice President: Marc Epstein, DO Second Vice President: Leslie Kramer, DO Third Vice President: Bradley Glick, DO American Secretary-Treasurer: Jere Mammino, DO (2007-2010) Immediate Past President: Bill Way, DO Trustees: James Towry, DO (2006-2008) Osteopathic Mark Kuriata, DO (2007-2010) Karen Neubauer, DO (2006-2008) College of David Grice, DO (2007-2010) Dermatology Sponsors: Global Pathology Laboratory Stiefel Laboratories Editors +BZ4(PUUMJFC %0 '0$00 Medicis 4UBOMFZ&4LPQJU %0 '"0$% CollaGenex +BNFT2%FM3PTTP %0 '"0$% Editorial Review Board 3POBME.JMMFS %0 JAOCD &VHFOF$POUF %0 Founding Sponsor &WBOHFMPT1PVMPT .% A0$%t&*MMJOPJTt,JSLTWJMMF .0 4UFQIFO1VSDFMM %0 t'"9 %BSSFM3JHFM .% wwwBPDEPSg 3PCFSU4DIXBS[F %0 COPYRIGHT AND PERMISSION: written permission must "OESFX)BOMZ .% be obtained from the Journal of the American Osteopathic College of Dermatology for copying or reprinting text of .JDIBFM4DPUU %0 more than half page, tables or figurFT Permissions are $JOEZ)PGGNBO %0 normally granted contingent upon similar permission from $IBSMFT)VHIFT %0 the author(s), inclusion of acknowledgement of the original source, and a payment of per page, table or figure of #JMM8BZ %0 reproduced matFSJBMPermission fees -

Extrinsic Factors Influencing Fetal Deformations and Intrauterine
Hindawi Publishing Corporation Journal of Pregnancy Volume 2012, Article ID 750485, 11 pages doi:10.1155/2012/750485 Review Article Extrinsic Factors Influencing Fetal Deformations and Intrauterine Growth Restriction Wendy Moh, 1 John M. Graham Jr.,2 Isha Wadhawan,2 and Pedro A. Sanchez-Lara1 1 Center for Craniofacial Molecular Biology, Ostrow School of Dentistry and Children’s Hospital Los Angeles, Keck School of Medicine of the University of Southern California, 4650 Sunset Boulevard, MS 90, Los Angeles, CA 90027, USA 2 Cedars-Sinai Medical Center, Medical Genetics Institute and David Geffen School of Medicine at UCLA, 8700 Beverly Boulevard, PACT Suite 400, Los Angeles, CA 90048, USA Correspondence should be addressed to Pedro A. Sanchez-Lara, [email protected] Received 24 March 2012; Revised 4 June 2012; Accepted 4 June 2012 Academic Editor: Sinuhe Hahn Copyright © 2012 Wendy Moh et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. The causes of intrauterine growth restriction (IUGR) are multifactorial with both intrinsic and extrinsic influences. While many studies focus on the intrinsic pathological causes, the possible long-term consequences resulting from extrinsic intrauterine physiological constraints merit additional consideration and further investigation. Infants with IUGR can exhibit early symmetric or late asymmetric growth abnormality patterns depending on the fetal stage of development, of which the latter is most common occurring in 70–80% of growth-restricted infants. Deformation is the consequence of extrinsic biomechanical factors interfering with normal growth, functioning, or positioning of the fetus in utero, typically arising during late gestation. -

Neonatal Orthopaedics
NEONATAL ORTHOPAEDICS NEONATAL ORTHOPAEDICS Second Edition N De Mazumder MBBS MS Ex-Professor and Head Department of Orthopaedics Ramakrishna Mission Seva Pratishthan Vivekananda Institute of Medical Sciences Kolkata, West Bengal, India Visiting Surgeon Department of Orthopaedics Chittaranjan Sishu Sadan Kolkata, West Bengal, India Ex-President West Bengal Orthopaedic Association (A Chapter of Indian Orthopaedic Association) Kolkata, West Bengal, India Consultant Orthopaedic Surgeon Park Children’s Centre Kolkata, West Bengal, India Foreword AK Das ® JAYPEE BROTHERS MEDICAL PUBLISHERS (P) LTD. New Delhi • London • Philadelphia • Panama (021)66485438 66485457 www.ketabpezeshki.com ® Jaypee Brothers Medical Publishers (P) Ltd. Headquarters Jaypee Brothers Medical Publishers (P) Ltd. 4838/24, Ansari Road, Daryaganj New Delhi 110 002, India Phone: +91-11-43574357 Fax: +91-11-43574314 Email: [email protected] Overseas Offices J.P. Medical Ltd. Jaypee-Highlights Medical Publishers Inc. Jaypee Brothers Medical Publishers Ltd. 83, Victoria Street, London City of Knowledge, Bld. 237, Clayton The Bourse SW1H 0HW (UK) Panama City, Panama 111, South Independence Mall East Phone: +44-2031708910 Phone: +507-301-0496 Suite 835, Philadelphia, PA 19106, USA Fax: +02-03-0086180 Fax: +507-301-0499 Phone: +267-519-9789 Email: [email protected] Email: [email protected] Email: [email protected] Jaypee Brothers Medical Publishers (P) Ltd. Jaypee Brothers Medical Publishers (P) Ltd. 17/1-B, Babar Road, Block-B, Shaymali Shorakhute, Kathmandu Mohammadpur, Dhaka-1207 Nepal Bangladesh Phone: +00977-9841528578 Mobile: +08801912003485 Email: [email protected] Email: [email protected] Website: www.jaypeebrothers.com Website: www.jaypeedigital.com © 2013, Jaypee Brothers Medical Publishers All rights reserved. No part of this book may be reproduced in any form or by any means without the prior permission of the publisher. -

4Th Annual Texas Children's Hospital Advanced Practice Provider
A Potpourri of Pediatric Dermatology 4th Annual Texas Children’s Hospital Advanced Practice Provider Conference April 2017 MOISE L. LEVY, M.D. DELL CHILDREN’S MEDICAL CENTER DELL MEDICAL SCHOOL/UT, AUSTIN AUSTIN, TX Conflicts of Interest Ø Anacor Ø Scioderm Ø Castle Creek Pharmaceuticals Ø Up to Date None Should Apply For This Presentation One way we are viewed… It’s just a birthmark 9 month old with asymptomatic scalp lesion noted in NICU; increases in size with straining But maybe something else… Sinus Pericranii Ø Communication between intra- and extracranial venous drainage pathways Ø Most are midline and non.pulsatile Ø Connect pericranial veins with superior sagittal sinus Ø TX depends on flow pattern/direction -Dominant; main flow via SP -Accessory; small flow via SP Neuroradiology 2007;49:505 Neurology 2009;72:e66 Case History 5 y/o girl w celiac disease Seen for evaluation of perianal growth Present, by hx, x 2 yrs No prior tx Case History Was seen by pediatric surgery Excised Condyloma - HPV 6, 16 Management? ARS – Pediatric Anogenital Warts When seeing a 5 yo with anogenital warts A. HPV testing should be done B. All cases are due to abuse C. All cases should be treated with imiquimod D. History and physical examination are key for suspicion of abuse E. Call Dr Eichenfield; he’ll know what to do Pediatric Anogenital Warts Age of onset and abuse - 6.5 ± 3.8 yrs (5.3 yrs) - 37% 2-12 yrs; 70% > 8 yrs - 4 yrs 8 months (83% female) HPV testing felt not of use… high subclinical History and PE key - physical findings abuse rare Arch Dermatol 1990;126:1575 Pediatrics 2005;116:815 Arch Dis Child 2006;91:696 Pediatr Dermatol 2006;23:199 J Pediatr Adolesc Gynecol 2013;26:e121 Age of Onset and Abuse Pediatr Dermatol 2006;23:199 ARS – Pediatric Anogenital Warts When seeing a 5 yo with anogenital warts A. -

Nevus Sebaceous
Nevus Sebaceous A nevus sebaceous (NEE vuhs sih BAY shus) is a type of birthmark that usually appears on the scalp. It may also appear on the face but this is less common. It is made of extra oil glands in the skin. It starts as a flat pink or orange plaque (slightly raised area). Hair does not grow in a nevus sebaceous. Typically, these are fairly small areas of skin. However, they can sometimes be larger and more noticeable. These birthmarks usually look the same until puberty. Hormonal changes cause them to become more raised. During adolescence (teen years) they can become very bumpy and wart-like. This can make them bothersome when brushing, combing or cutting the hair. A nevus sebaceous does not go away on its own. The cause is unknown. As a person gets older, typically after adolescence, abnormal changes to the area can sometimes occur. Your child’s doctor will monitor it over time. Diagnosis Your child’s doctor can usually diagnosis this kind of birthmark. If unsure, the doctor may take a small piece of the birthmark as a biopsy. The doctor will send it to a lab to be looked at under a microscope. This can confirm the diagnosis. Treatment Generally, it is very safe for your child’s doctor to simply watch a nevus sebaceous over time. This is especially true while your child is young (before puberty). A nevus sebaceous will not affect your child’s health, but you or your child may still want it to be taken off. If your child’s nevus sebaceous is large or becomes bothersome, it may be removed. -

SUBGALEAL HEMATOMA Sarah Meyers MS4 Ilse Castro-Aragon MD CASE HISTORY
SUBGALEAL HEMATOMA Sarah Meyers MS4 Ilse Castro-Aragon MD CASE HISTORY Ex-FT (37w6d) male infant born by low transverse C-section for arrest of descent and chorioamnionitis to a 34-year-old G2P1 mother. The infant had 1- and 5-minute APGAR scores of 9 and 9, weighed 3.625 kg (54th %ile), and had a head circumference of 34.5 cm (30th %ile). Following a challenging delivery of the head during C/s, the infant was noted to have left-sided parietal and occipital bogginess, and an ultrasound was ordered due to concern for subgaleal hematoma. PEDIATRIC HEAD ULTRASOUND: SUBGALEAL HEMATOMA Superficial pediatric head ultrasound showing moderately echogenic fluid collection (green arrow), superficial to the periosteum (blue arrow), crossing the sagittal suture (red arrow). Findings on U/S consistent with large parieto-occipital subgaleal hematoma. PEDIATRIC HEAD ULTRASOUND: SUBGALEAL HEMATOMA Superficial pediatric head ultrasound showing moderately echogenic fluid collection (green arrow), consistent with large parieto-occipital subgaleal hematoma. CLINICAL FOLLOW UP - Subgaleal hematoma was confirmed on ultrasound and the infant was transferred from the newborn nursery to the NICU for close monitoring, including hourly head circumferences and repeat hematocrit measurements - Serial head circumferences remained stable around 34 cm and hematocrit remained stable between 39 and 41 throughout hospital course - The infant was subsequently treated with phototherapy for hyperbilirubinemia, thought to be secondary to resorption of the SGH IN A NUTSHELL: -

Genes in Eyecare Geneseyedoc 3 W.M
Genes in Eyecare geneseyedoc 3 W.M. Lyle and T.D. Williams 15 Mar 04 This information has been gathered from several sources; however, the principal source is V. A. McKusick’s Mendelian Inheritance in Man on CD-ROM. Baltimore, Johns Hopkins University Press, 1998. Other sources include McKusick’s, Mendelian Inheritance in Man. Catalogs of Human Genes and Genetic Disorders. Baltimore. Johns Hopkins University Press 1998 (12th edition). http://www.ncbi.nlm.nih.gov/Omim See also S.P.Daiger, L.S. Sullivan, and B.J.F. Rossiter Ret Net http://www.sph.uth.tmc.edu/Retnet disease.htm/. Also E.I. Traboulsi’s, Genetic Diseases of the Eye, New York, Oxford University Press, 1998. And Genetics in Primary Eyecare and Clinical Medicine by M.R. Seashore and R.S.Wappner, Appleton and Lange 1996. M. Ridley’s book Genome published in 2000 by Perennial provides additional information. Ridley estimates that we have 60,000 to 80,000 genes. See also R.M. Henig’s book The Monk in the Garden: The Lost and Found Genius of Gregor Mendel, published by Houghton Mifflin in 2001 which tells about the Father of Genetics. The 3rd edition of F. H. Roy’s book Ocular Syndromes and Systemic Diseases published by Lippincott Williams & Wilkins in 2002 facilitates differential diagnosis. Additional information is provided in D. Pavan-Langston’s Manual of Ocular Diagnosis and Therapy (5th edition) published by Lippincott Williams & Wilkins in 2002. M.A. Foote wrote Basic Human Genetics for Medical Writers in the AMWA Journal 2002;17:7-17. A compilation such as this might suggest that one gene = one disease. -

Cutaneous Manifestations of Newborns in Omdurman Maternity Hospital
ﺑﺴﻢ اﷲ اﻟﺮﺣﻤﻦ اﻟﺮﺣﻴﻢ Cutaneous Manifestations of Newborns in Omdurman Maternity Hospital A thesis submitted in the partial fulfillment of the degree of clinical MD in pediatrics and child health University of Khartoum By DR. AMNA ABDEL KHALIG MOHAMED ATTAR MBBS University of Khartoum Supervisor PROF. SALAH AHMED IBRAHIM MD, FRCP, FRCPCH Department of Pediatrics and Child Health University of Khartoum University of Khartoum The Graduate College Medical and Health Studies Board 2008 Dedication I dedicate my study to the Department of Pediatrics University of Khartoum hoping to be a true addition to neonatal care practice in Sudan. i Acknowledgment I would like to express my gratitude to my supervisor Prof. Salah Ahmed Ibrahim, Professor of Peadiatric and Child Health, who encouraged me throughout the study and provided me with advice and support. I am also grateful to Dr. Osman Suleiman Al-Khalifa, the Dermatologist for his support at the start of the study. Special thanks to the staff at Omdurman Maternity Hospital for their support. I am also grateful to all mothers and newborns without their participation and cooperation this study could not be possible. Love and appreciation to my family for their support, drive and kindness. ii Table of contents Dedication i Acknowledgement ii Table of contents iii English Abstract vii Arabic abstract ix List of abbreviations xi List of tables xiii List of figures xiv Chapter One: Introduction & Literature Review 1.1 The skin of NB 1 1.2 Traumatic lesions 5 1.3 Desquamation 8 1.4 Lanugo hair 9 1.5 -
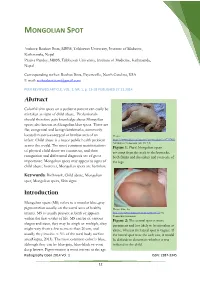
Mongolian Spot
MONGOLIAN SPOT Authors: Roshan Bista, MBBS, Tribhuvan University, Institute of Medicine, Kathmandu, Nepal Prativa Pandey, MBBS, Tribhuvan University, Institute of Medicine, Kathmandu, Nepal Corresponding author: Roshan Bista, Fayetteville, North Carolina, USA E-mail: [email protected] PEER REVIEWED ARTICLE, VOL. 1, NR. 1, p. 12-18 PUBLISHED 27.11.2014 Abstract Colorful skin spots on a pediatric patient can easily be mistaken as signs of child abuse. Professionals should therefore gain knowledge about Mongolian spots; also known as Mongolian blue spots. These are flat, congenital and benign birthmarks, commonly located in sacro-coccygeal or lumbar area of an Photo: infant. Child abuse is a major public health problem https://www.flickr.com/photos/geowombats/1667757455 Attribution 2.0 Generic (CC BY 2.0) across the world. The most common manifestations Figure 1: Plural Mongolian spots of physical child abuse are cutaneous, and their covering from the neck to the buttocks, recognition and differential diagnosis are of great both flanks and shoulders and even one of importance. Mongolian spots may appear as signs of the legs. child abuse; however, Mongolian spots are harmless. Keywords: Birthmark, Child abuse, Mongolian spot, Mongolian spots, Skin signs Introduction Mongolian spots (MS) refers to a macular blue-gray pigmentation usually on the sacral area of healthy Photo: Abby Lu infants. MS is usually present at birth or appears http://creativecommons.org/licenses/by/2.0 via Wikimedia Commons within the first weeks of life. MS can be of various Figure 2: The central spot is more shapes and sizes, they may be single or multiple, they prominent and less likely to be mistaken as might vary from a few to more than 20 cm, and abuse, whereas the lateral spot is vaguer. -

Child Abuse: Skin Markers and Differential Diagnosis
527 527 REVISÃO L Violência contra a criança: indicadores dermatológicos e diagnósticos diferenciais* Child abuse: skin markers and differential diagnosis Roberta Marinho Falcão Gondim 1 Daniel Romero Muñoz 2 Valeria Petri 3 Resumo: As denúncias de abuso contra a criança têm sido frequentes e configuram grave problema de saúde pública. O tema é desconfortável para muitos médicos, seja pelo treinamento insuficiente, seja pelo desconhecimento das dimensões do problema. Uma das formas mais comuns de violência contra a criança é o abuso físico. Como órgão mais exposto e extenso, a pele é o alvo mais sujeito aos maus- tratos. Equimoses e queimaduras são os sinais mais visíveis. Médicos (pediatras, clínicos-gerais e derma- tologistas) costumam ser os primeiros profissionais a observar e reconhecer sinais de lesões não aciden- tais ou intencionais. Os dermatologistas podem auxiliar na distinção entre lesões traumáticas inten- cionais, acidentais e doenças cutâneas que mimetizam maus-tratos. Palavras-chave: Contusões; Equimose; Queimaduras; Violência doméstica; Violência sexual Abstract: Reports of child abuse have increased significantly. The matter makes most physicians uncom- fortable for two reasons: a) Little guidance or no training in recognizing the problem; b - Not under- standing its true dimension. The most common form of child violence is physical abuse. The skin is the largest and frequently the most traumatized organ. Bruises and burns are the most visible signs. Physicians (pediatricians, general practitioners and dermatologists) -

Survey of Skin Disorders in Newborns: Clinical Observation in an Egyptian Medical Centre Nursery A.A
املجلة الصحية لرشق املتوسط املجلد الثامن عرش العدد اﻷول Survey of skin disorders in newborns: clinical observation in an Egyptian medical centre nursery A.A. El-Moneim 1 and R.E. El-Dawela 2 مسح لﻻضطرابات اجللدية لدى الولدان: مﻻحظة رسيرية يف حضانة يف مركز طبي يف مرص عبري أمحد عبد املنعم، رهيام عز الدولة الرشقاوي اخلﻻصة:مل َ ْت َظ اﻻضطرابات اجللدية لدى الولدان بدراسات جيدة يف مرص. وقد هدفت الباحثتان إىل دراسة أنامط التغريات اجللدية يف عينة من ِ الولدان املرصيني، وهي دراسة وصفية استباقية أترابية شملت ستة مئة وليد يف َّحضانة يف مستشفى جامعة سوهاج، َّوتضمنت الفحص اجللدي خﻻل اﻷيام اخلمسة اﻷوىل بعد الوﻻدة. وقد تم كشف اﻻضطرابات اجللدية لدى 240 ًوليدا )40%( ولوحظت الومحات لدى 100 وليد )%16.7(، ومعظمها من النمط ذي اخلﻻيا امليﻻنية )لطخات منغولية لدى 11.7% مع ومحات وﻻدية ذات ميﻻنية اخلﻻيا لدى 2.7%(. كام ُك ِش َف ْت العداوى الفطرية اجللدية، ومنها داء َّاملبيضات الفموية، وعدوى الفطريات يف مناطق احلفاظات أو َالـم َذح الناجم عن عدوى َّاملبيضات يف اﻷرفاغ )أصل الفخذ(، وذلك لدى 13.3%، ُوكشفت بعض العداوى اجلرثومية يف 1.3%من الولدان. وتشري املقارنات مع الدراسات اﻷخرى يف أرجاء العامل إىل معدل مرتفع للعدوى بالفطريات مع معدل منخفض للومحات الوﻻدية يف دراستنا للولدان، وتويص الباحثتان بإجراء تقييم روتيني جلدي للولدان، ّوﻻسيام يف ضوء املعدﻻت املرتفعة للعدوى اجللدية بالفطريات. ABSTRACT The frequency of neonatal skin disorders has not been well studied in Egypt. Our aim was to address patterns of dermatological changes in a sample of Egyptian newborns. In a descriptive prospective cohort study 600 newborns in Sohag University hospital nursery were dermatologically examined within the first 5 days of birth.