Oral Lichen Planus: a Case Report and Review of Literature
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-
CLAPA Adults Conference
Adults Cleft Conference Camden Lock, London, England Saturday 17 November 2018 The Cleft Lip and Palate Association (CLAPA) is the only national charity supporting people and families affected by cleft lip and/or palate in the UK from diagnosis through to adulthood. Timetable • • • • • • • • • • • • • • • • What’s today all about? • • • • Some ground rules and caveats • • • • • About the Adult Services Project • There are an estimated 75,000 people over the age of 16 living in the United Kingdom who were born with a cleft. • Understanding and supporting the unique needs and experiences of adults affected by cleft is very important to CLAPA. • From March 2018-February 2021, CLAPA is undertaking an exciting project looking at improving services for adults who were born with a cleft funded by the VTCT Foundation. • The goals are to research and understand the experiences, challenges and unmet needs of adults in the UK who were born with a cleft lip and/or palate. • The Adult Services Coordinator is the primary contact for this piece of work. What we did in Year One • • • • • So…what did we find at the roadshow? • We were humbled by how candidly people shared some of their most pivotal moments with us. • As you would expect, there were many different (oftentimes unique) experiences in the community, however there were some common themes that came up many times – these included: • The struggle of obtaining a successful referral to the cleft team as an adult • Being unsure what to expect at cleft team appointments • Not knowing (and health -

Communicable Disease Exclusion Guidelines for Schools and Child Care Settings
Deschutes County Health Services COMMUNICABLE DISEASE EXCLUSION GUIDELINES FOR SCHOOLS AND CHILD CARE SETTINGS Symptoms requiring exclusion of a child from school or childcare setting until either diagnosed and cleared by a licensed health care provider or recovery. FEVER: ANY fever greater than 100.5 F., may return when temperature decreases without use of fever-reducing medicine. VOMITTING: > 2 in the preceding 24 hours, unless determined to be from non-communicable conditions. May return when resolved. DIARRHEA: 3 or more watery or loose stools in 24 hours. May return when resolved for 24 hours. STIFF NECK: or headache with accompanying fever. May return after resolution of symptoms or diagnosis made and clearance given. RASHES: ANY new onset of rash if accompanied by fever; may return after rash resolves or if clearance given by health care providers. SKIN LESIONS: Drainage that cannot be contained within a bandage. JAUNDICE: Yellowing of eyes or skin. May return after diagnosis from physician and clearance given. BEHAVIOR CHANGE: Such as new onset of irritability, lethargy or somnolence. COUGH /SOB: Persistent cough with or without fever, serious sustained coughing, shortness of breath, or difficulty breathing. SYMPTOMS or complaints that prevent the student from active participation in usual school activities, or student requiring more care than the school staff can safely provide. Inform local county health department, (LHD), of all diseases listed as reportable. The local county health department should be consulted regarding any written communication that may be developed to inform parents/guardians about disease outbreaks, risk to students, families, and staff and/or control measures specific to an outbreak. -

4Th Annual Texas Children's Hospital Advanced Practice Provider
A Potpourri of Pediatric Dermatology 4th Annual Texas Children’s Hospital Advanced Practice Provider Conference April 2017 MOISE L. LEVY, M.D. DELL CHILDREN’S MEDICAL CENTER DELL MEDICAL SCHOOL/UT, AUSTIN AUSTIN, TX Conflicts of Interest Ø Anacor Ø Scioderm Ø Castle Creek Pharmaceuticals Ø Up to Date None Should Apply For This Presentation One way we are viewed… It’s just a birthmark 9 month old with asymptomatic scalp lesion noted in NICU; increases in size with straining But maybe something else… Sinus Pericranii Ø Communication between intra- and extracranial venous drainage pathways Ø Most are midline and non.pulsatile Ø Connect pericranial veins with superior sagittal sinus Ø TX depends on flow pattern/direction -Dominant; main flow via SP -Accessory; small flow via SP Neuroradiology 2007;49:505 Neurology 2009;72:e66 Case History 5 y/o girl w celiac disease Seen for evaluation of perianal growth Present, by hx, x 2 yrs No prior tx Case History Was seen by pediatric surgery Excised Condyloma - HPV 6, 16 Management? ARS – Pediatric Anogenital Warts When seeing a 5 yo with anogenital warts A. HPV testing should be done B. All cases are due to abuse C. All cases should be treated with imiquimod D. History and physical examination are key for suspicion of abuse E. Call Dr Eichenfield; he’ll know what to do Pediatric Anogenital Warts Age of onset and abuse - 6.5 ± 3.8 yrs (5.3 yrs) - 37% 2-12 yrs; 70% > 8 yrs - 4 yrs 8 months (83% female) HPV testing felt not of use… high subclinical History and PE key - physical findings abuse rare Arch Dermatol 1990;126:1575 Pediatrics 2005;116:815 Arch Dis Child 2006;91:696 Pediatr Dermatol 2006;23:199 J Pediatr Adolesc Gynecol 2013;26:e121 Age of Onset and Abuse Pediatr Dermatol 2006;23:199 ARS – Pediatric Anogenital Warts When seeing a 5 yo with anogenital warts A. -

Nevus Sebaceous
Nevus Sebaceous A nevus sebaceous (NEE vuhs sih BAY shus) is a type of birthmark that usually appears on the scalp. It may also appear on the face but this is less common. It is made of extra oil glands in the skin. It starts as a flat pink or orange plaque (slightly raised area). Hair does not grow in a nevus sebaceous. Typically, these are fairly small areas of skin. However, they can sometimes be larger and more noticeable. These birthmarks usually look the same until puberty. Hormonal changes cause them to become more raised. During adolescence (teen years) they can become very bumpy and wart-like. This can make them bothersome when brushing, combing or cutting the hair. A nevus sebaceous does not go away on its own. The cause is unknown. As a person gets older, typically after adolescence, abnormal changes to the area can sometimes occur. Your child’s doctor will monitor it over time. Diagnosis Your child’s doctor can usually diagnosis this kind of birthmark. If unsure, the doctor may take a small piece of the birthmark as a biopsy. The doctor will send it to a lab to be looked at under a microscope. This can confirm the diagnosis. Treatment Generally, it is very safe for your child’s doctor to simply watch a nevus sebaceous over time. This is especially true while your child is young (before puberty). A nevus sebaceous will not affect your child’s health, but you or your child may still want it to be taken off. If your child’s nevus sebaceous is large or becomes bothersome, it may be removed. -

Boils and Skin Infections Are Usually Caused by Bacteria
Communicable Diseases Factsheet Boils and skin infections are usually caused by bacteria. Avoid sharing items and wash hands thoroughly, especially after touching skin Boils and skin infections infections. Last updated: March 2017 What are boils? A boil (sometimes known as a furuncle) is an infection of the skin, often around a hair follicle. It is usually caused by Staphylococcus aureus bacteria (commonly known as golden staph). Many healthy people carry these bacteria on their skin or in their nose, but do not have any symptoms. Boils occur when bacteria get through broken skin and cause tender, swollen, pimple-like sores, which are full of pus. Boils usually get better on their own, but severe or recurring cases may require medical treatment and support. Staph bacteria may also cause other skin infections, including impetigo. Impetigo, commonly known as school sores (as they affect school-age children), are small blisters or flat crusty sores on the skin. See the Impetigo factsheet at http://www.health.nsw.gov.au/Infectious/factsheets/Pages/impetigo.aspx for specific information on Impetigo. How are they diagnosed? Most skin infections are diagnosed on the basis of their appearance and the presence of any related symptoms (such as fever). Your doctor may take swabs or samples from boils, wounds, or other sites of infection to identify the bacteria responsible. Some infections may be caused by bacteria that are resistant to some antibiotics. See the MRSA in the community factsheet for detailed information on infections caused by antibiotic -

Skin and Soft Tissue Infections Ohsuerin Bonura, MD, MCR Oregon Health & Science University Objectives
Difficult Skin and Soft tissue Infections OHSUErin Bonura, MD, MCR Oregon Health & Science University Objectives • Compare and contrast the epidemiology and clinical presentation of common skin and soft tissue diseases • State the management for skin and soft tissue infections OHSU• Differentiate true infection from infectious disease mimics of the skin Casey Casey is a 2 year old boy who presents with this rash. What is the best treatment? A. Soap and Water B. Ibuprofen, it will self OHSUresolve C. Dicloxacillin D. Mupirocin OHSUImpetigo Impetigo Epidemiology and Treatment OHSU Ellen Ellen is a 54 year old morbidly obese woman with DM, HTN and venous stasis who presented with a painful left leg and fever. She has had 3 episodes in the last 6 months. What do you recommend? A. Cefazolin followed by oral amoxicillin prophylaxis B. Vancomycin – this is likely OHSUMRSA C. Amoxicillin – this is likely erysipelas D. Clindamycin to cover staph and strep cellulitis Impetigo OHSUErysipelas Erysipelas Risk: lymphedema, stasis, obesity, paresis, DM, ETOH OHSURecurrence rate: 30% in 3 yrs Treatment: Penicillin Impetigo Erysipelas OHSUCellulitis Cellulitis • DEEPER than erysipelas • Microbiology: – 6-48hrs post op: think GAS… too early for staph (days in the making)! – Periorbital – Staph, Strep pneumoniae, GAS OHSU– Post Varicella - GAS – Skin popping – Staph + almost anything! Framework for Skin and Soft Tissue Infections (SSTIs) NONPurulent Purulent Necrotizing/Cellulitis/Erysipelas Furuncle/Carbuncle/Abscess Severe Moderate Mild Severe Moderate Mild I&D I&D I&D I&D IV Rx Oral Rx C&S C&S C&S C&S Vanc + Pip-tazo OHSUEmpiric IV Empiric MRSA Oral MRSA TMP/SMX Doxy What Are Your “Go-To” Oral Options For Non-Purulent SSTI? Amoxicillin Doxycycline OHSUCephalexin Doxycycline Trimethoprim-Sulfamethoxazole OHSU Miller LG, et al. -

Reportable Disease Surveillance in Virginia, 2013
Reportable Disease Surveillance in Virginia, 2013 Marissa J. Levine, MD, MPH State Health Commissioner Report Production Team: Division of Surveillance and Investigation, Division of Disease Prevention, Division of Environmental Epidemiology, and Division of Immunization Virginia Department of Health Post Office Box 2448 Richmond, Virginia 23218 www.vdh.virginia.gov ACKNOWLEDGEMENT In addition to the employees of the work units listed below, the Office of Epidemiology would like to acknowledge the contributions of all those engaged in disease surveillance and control activities across the state throughout the year. We appreciate the commitment to public health of all epidemiology staff in local and district health departments and the Regional and Central Offices, as well as the conscientious work of nurses, environmental health specialists, infection preventionists, physicians, laboratory staff, and administrators. These persons report or manage disease surveillance data on an ongoing basis and diligently strive to control morbidity in Virginia. This report would not be possible without the efforts of all those who collect and follow up on morbidity reports. Divisions in the Virginia Department of Health Office of Epidemiology Disease Prevention Telephone: 804-864-7964 Environmental Epidemiology Telephone: 804-864-8182 Immunization Telephone: 804-864-8055 Surveillance and Investigation Telephone: 804-864-8141 TABLE OF CONTENTS INTRODUCTION Introduction ......................................................................................................................................1 -

Viability of Methicillin-Resistant Staphylococcus Aureus on Artificial Turf Under
Viability of Methicillin-Resistant Staphylococcus aureus on Artificial Turf Under Outdoor and Laboratory Environmental Conditions A thesis presented to the faculty of the College of Health Sciences and Professions of Ohio University In partial fulfillment of the requirements for the degree Master of Science Ashley N. Hardbarger June 2012 © 2012 Ashley N. Hardbarger. All Rights Reserved. 2 This thesis titled Viability of Methicillin-Resistant Staphylococcus aureus on Artificial Turf Under Outdoor and Laboratory Environmental Conditions by ASHLEY N. HARDBARGER has been approved for the School of Applied Health Sciences and Wellness and the College of Health Sciences and Professions by Andrew Krause Assistant Professor of Applied Health Sciences and Wellness Randy Leite Dean, College of Health Sciences and Professions 3 ABSTRACT HARDBARGER, ASHLEY N., M.S., June 2012, Athletic Training Viability of Methicillin-Resistant Staphylococcus Aureus on Artificial Turf Under Outdoor and Laboratory Environmental Conditions Director of Thesis: Andrew Krause Methicillin-resistant Staphylococcus aureus has survived on artificial turf in a laboratory setting when provided a nutrient source. There is limited evidence on the viability of MRSA in outdoor environmental conditions. This study compared the survival of MRSA in a laboratory environment to an outdoor environment over seven days. Artificial turf was inoculated with MRSA strain USA300 and exposed to laboratory and outdoor environmental settings. Samples were collected daily. MRSA survival was determined by growth on CHROMagar plates. Results indicated a difference in the mean survival time of MRSA between a laboratory environment (7.00 ± 0.00 days) and an outdoor environment (4.67 ± 2.52). Conditions including surface temperature, ambient temperature, relative humidity, precipitation and solar radiation may have affected MRSA survival. -

Cutaneous Manifestations of Newborns in Omdurman Maternity Hospital
ﺑﺴﻢ اﷲ اﻟﺮﺣﻤﻦ اﻟﺮﺣﻴﻢ Cutaneous Manifestations of Newborns in Omdurman Maternity Hospital A thesis submitted in the partial fulfillment of the degree of clinical MD in pediatrics and child health University of Khartoum By DR. AMNA ABDEL KHALIG MOHAMED ATTAR MBBS University of Khartoum Supervisor PROF. SALAH AHMED IBRAHIM MD, FRCP, FRCPCH Department of Pediatrics and Child Health University of Khartoum University of Khartoum The Graduate College Medical and Health Studies Board 2008 Dedication I dedicate my study to the Department of Pediatrics University of Khartoum hoping to be a true addition to neonatal care practice in Sudan. i Acknowledgment I would like to express my gratitude to my supervisor Prof. Salah Ahmed Ibrahim, Professor of Peadiatric and Child Health, who encouraged me throughout the study and provided me with advice and support. I am also grateful to Dr. Osman Suleiman Al-Khalifa, the Dermatologist for his support at the start of the study. Special thanks to the staff at Omdurman Maternity Hospital for their support. I am also grateful to all mothers and newborns without their participation and cooperation this study could not be possible. Love and appreciation to my family for their support, drive and kindness. ii Table of contents Dedication i Acknowledgement ii Table of contents iii English Abstract vii Arabic abstract ix List of abbreviations xi List of tables xiii List of figures xiv Chapter One: Introduction & Literature Review 1.1 The skin of NB 1 1.2 Traumatic lesions 5 1.3 Desquamation 8 1.4 Lanugo hair 9 1.5 -
Mongolian Spot
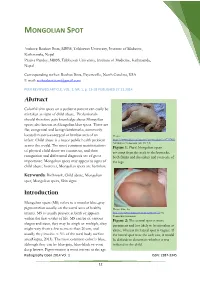
MONGOLIAN SPOT Authors: Roshan Bista, MBBS, Tribhuvan University, Institute of Medicine, Kathmandu, Nepal Prativa Pandey, MBBS, Tribhuvan University, Institute of Medicine, Kathmandu, Nepal Corresponding author: Roshan Bista, Fayetteville, North Carolina, USA E-mail: [email protected] PEER REVIEWED ARTICLE, VOL. 1, NR. 1, p. 12-18 PUBLISHED 27.11.2014 Abstract Colorful skin spots on a pediatric patient can easily be mistaken as signs of child abuse. Professionals should therefore gain knowledge about Mongolian spots; also known as Mongolian blue spots. These are flat, congenital and benign birthmarks, commonly located in sacro-coccygeal or lumbar area of an Photo: infant. Child abuse is a major public health problem https://www.flickr.com/photos/geowombats/1667757455 Attribution 2.0 Generic (CC BY 2.0) across the world. The most common manifestations Figure 1: Plural Mongolian spots of physical child abuse are cutaneous, and their covering from the neck to the buttocks, recognition and differential diagnosis are of great both flanks and shoulders and even one of importance. Mongolian spots may appear as signs of the legs. child abuse; however, Mongolian spots are harmless. Keywords: Birthmark, Child abuse, Mongolian spot, Mongolian spots, Skin signs Introduction Mongolian spots (MS) refers to a macular blue-gray pigmentation usually on the sacral area of healthy Photo: Abby Lu infants. MS is usually present at birth or appears http://creativecommons.org/licenses/by/2.0 via Wikimedia Commons within the first weeks of life. MS can be of various Figure 2: The central spot is more shapes and sizes, they may be single or multiple, they prominent and less likely to be mistaken as might vary from a few to more than 20 cm, and abuse, whereas the lateral spot is vaguer. -

Survey of Skin Disorders in Newborns: Clinical Observation in an Egyptian Medical Centre Nursery A.A
املجلة الصحية لرشق املتوسط املجلد الثامن عرش العدد اﻷول Survey of skin disorders in newborns: clinical observation in an Egyptian medical centre nursery A.A. El-Moneim 1 and R.E. El-Dawela 2 مسح لﻻضطرابات اجللدية لدى الولدان: مﻻحظة رسيرية يف حضانة يف مركز طبي يف مرص عبري أمحد عبد املنعم، رهيام عز الدولة الرشقاوي اخلﻻصة:مل َ ْت َظ اﻻضطرابات اجللدية لدى الولدان بدراسات جيدة يف مرص. وقد هدفت الباحثتان إىل دراسة أنامط التغريات اجللدية يف عينة من ِ الولدان املرصيني، وهي دراسة وصفية استباقية أترابية شملت ستة مئة وليد يف َّحضانة يف مستشفى جامعة سوهاج، َّوتضمنت الفحص اجللدي خﻻل اﻷيام اخلمسة اﻷوىل بعد الوﻻدة. وقد تم كشف اﻻضطرابات اجللدية لدى 240 ًوليدا )40%( ولوحظت الومحات لدى 100 وليد )%16.7(، ومعظمها من النمط ذي اخلﻻيا امليﻻنية )لطخات منغولية لدى 11.7% مع ومحات وﻻدية ذات ميﻻنية اخلﻻيا لدى 2.7%(. كام ُك ِش َف ْت العداوى الفطرية اجللدية، ومنها داء َّاملبيضات الفموية، وعدوى الفطريات يف مناطق احلفاظات أو َالـم َذح الناجم عن عدوى َّاملبيضات يف اﻷرفاغ )أصل الفخذ(، وذلك لدى 13.3%، ُوكشفت بعض العداوى اجلرثومية يف 1.3%من الولدان. وتشري املقارنات مع الدراسات اﻷخرى يف أرجاء العامل إىل معدل مرتفع للعدوى بالفطريات مع معدل منخفض للومحات الوﻻدية يف دراستنا للولدان، وتويص الباحثتان بإجراء تقييم روتيني جلدي للولدان، ّوﻻسيام يف ضوء املعدﻻت املرتفعة للعدوى اجللدية بالفطريات. ABSTRACT The frequency of neonatal skin disorders has not been well studied in Egypt. Our aim was to address patterns of dermatological changes in a sample of Egyptian newborns. In a descriptive prospective cohort study 600 newborns in Sohag University hospital nursery were dermatologically examined within the first 5 days of birth. -

Cutaneous Manifestations of Systemic Disease
Cutaneous Manifestations of Systemic Disease Dr. Lloyd J. Cleaver D.O. FAOCD FAAD Northeast Regional Medical Center A.T.Still University/KCOM Assistant Vice President/Professor ACOI Board Review Disclosure I have no financial relationships to disclose I will not discuss off label use and/or investigational use in my presentation I do not have direct knowledge of AOBIM questions I have been granted approvial by the AOA to do this board review Dermatology on the AOBIM ”1-4%” of exam is Dermatology Table of Test Specifications is unavailable Review Syllabus for Internal Medicine Large amount of information Cutaneous Multisystem Cutaneous Connective Tissue Conditions Connective Tissue Diease Discoid Lupus Erythematosus Subacute Cutaneous LE Systemic Lupus Erythematosus Scleroderma CREST Syndrome Dermatomyositis Lupus Erythematosus Spectrum from cutaneous to severe systemic involvement Discoid LE (DLE) / Chronic Cutaneous Subacute Cutaneous LE (SCLE) Systemic LE (SLE) Cutaneous findings common in all forms Related to autoimmunity Discoid LE (Chronic Cutaneous LE) Primarily cutaneous Scaly, erythematous, atrophic plaques with sharp margins, telangiectasias and follicular plugging Possible elevated ESR, anemia or leukopenia Progression to SLE only 1-2% Heals with scarring, atrophy and dyspigmentation 5% ANA positive Discoid LE (Chronic Cutaneous LE) Scaly, atrophic plaques with defined margins Discoid LE (Chronic Cutaneous LE) Scaly, erythematous plaques with scarring, atrophy, dyspigmentation DISCOID LUPUS Subacute Cutaneous