An Atypical Case of Chilaiditi Syndrome
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

IRRITABLE BOWEL SYNDROME by Michael Sperling MD
IRRITABLE BOWEL SYNDROME By Michael Sperling MD Irritable bowel syndrome (IBS) involves vague symptoms of abdominal pain, diarrhea, constipation, gas and bloating for which there is no understandable cause. Incredibly, IBS affects up to 20% of the population but only three- quarters of those people actually seek medical attention. It is the second most common reason for work absenteeism. Irritable bowel symptoms may also be related to other complaints such as belching, heartburn, swallowing problems, fullness after eating, nausea, frequent urination, painful menstruation and pain during intercourse. Extremely severe cases can sometimes be related to a history of traumatic abuse. Some common associations or factors: Michael Sperling, MD 1. ‘Spastic colon’ is frequently found along with irritable bowel syndrome. Spastic colon consists of painful muscle contractions which can be relieved by bulk agents or anti- spasm drugs. 2. Post-infectious IBS occurs when irritable bowel follows a gastrointestinal infection, such as the stomach flu. These recurrent symptoms can last up to two years. 3. Stress and anxiety can worsen IBS symptoms so occasionally anti-anxiety agents may be helpful. 4. Food intolerances classically worsen symptoms of irritable bowel in some people. Common “offending foods” include lactose, legumes (beans) and cruciferous vegetables like brussel sprouts, cauliflower, broccoli and cabbage. 5. Hypersensitivity of the bowel wall: Normal colon activity is not usually noticed however in “visceral hypersensitivity”, the bowel wall reacts painfully to normal activity. This condition may be helped by the use of low dose antidepressants, which can block these painful stimuli. Careful and selective testing of patients with these symptoms and the development of a long-term doctor/patient relationship is the key to diagnosing and managing these symptoms. -

And Diaphragm (Chilaiditi's Syndrome) in Children by A
Arch Dis Child: first published as 10.1136/adc.32.162.151 on 1 April 1957. Downloaded from INTERPOSITION OF THE COLON BETWEEN LIVER AND DIAPHRAGM (CHILAIDITI'S SYNDROME) IN CHILDREN BY A. D. M. JACKSON and C. J. HODSON From the Institute of Child Health, University ofLondon, and the Queen Elizabeth Hospitalfor Children, London (RECEIVED FOR PUBLICATION SEPTEMBER 24, 1956) In 1910 Chilaiditi published a paper in which he positions. On one occasion during the fluoroscopy the described three adult patients with gaseous ab- ascent of the colon and the displacement of the liver were dominal distension and intermittent displacement actually observed as the patient was rotated from the supine to the left lateral position. Fluoroscopy after an of the liver by a distended loop of colon. Although opaque meal excluded any form of intestinal obstruction there had been some earlier brief reports, for example and the interposed loop of bowel was identified as the those of Gontermann (1890), Cohn (1907) and hepatic flexure. Weinberger (1908), this was the first really detailed PROGRESS. During the six months following his first account of the condition which has come to be visit to hospital the child had recurrent attacks of severe known as Chilaiditi's syndrome. abdominal pain with vomiting and his mother became During the last 45 aware of his swallowing air. He was admitted to hos- years many more cases have copyright. been reported but very few of these have been pital in June, 1951, and put to bed. The attacks promptly children. It will be of some interest, therefore, ceased, although the abdominal distension persisted and the position of the liver could still be altered with posture. -

Stomach Flu (Viral Gastroenteritis)
Stomach Flu (Viral Gastroenteritis) The stomach flu (also called viral gastroenteritis) is caused by a virus (rotavirus, adenovirus, Norwalk virus to name a few) that affect the stomach and small intestines. It may come on suddenly or over the course of a few hours. The illness is usually brief, lasting 24-72 hours. Symptoms include: Nausea Vomiting Stomach cramps Diarrhea Mild fever Fatigue Body Chills/Sweats Loss of appetite Muscle aches To help take care of yourself: • The best thing to do is to let your stomach rest from solid foods. • Sip on clear liquids (Hi-C, apple, cranberry, and grape juices, Jell-O, Gatorade- type liquids and ginger-ale or ginger tea). There are special properties in ginger that help soothe the stomach. It is extremely important to keep up your hydration. Water is great for hydration but Gatorade-type products are better because they will restore your electrolytes (Sodium, Potassium and Chloride) which are essential for body functions. You may "stir" the bubbles out of the soda if the carbonation is harsh on your stomach. • Once you have not vomited for a few hours and your stomach is feeling better, you may start to eat solid foods. You may try crackers, plain noodles, eggs, broth, pretzels and yogurt. • The BRAT diet (Bananas, Rice, Applesauce & Toast) includes foods that are low in fiber and are easily digested. • Stay away from dairy products, citric (including orange and grapefruit juices), tomato-based & spicy foods. • SLOWLY increase your dietary intake to include fruits, vegetables and meat once symptoms are gone (usually over 2-3 days). -

Appendicitis
Appendicitis Your child has abdominal pain, it might be appendicitis. Appendicitis is swelling or infection in the appendix. The appendix is a small organ attached to the large intestine. Appendicitis usually develops over 12-24 hours. It has symptoms such as abdominal pain, nausea, vomiting, fever, and loss of appetite. Most importantly, pain that continues, worsens and moves to the right lower side of the abdomen is common in appendicitis. Appendicitis is the most common childhood “emergency” that must be treated in a timely manner. However, it’s important to know that many conditions have symptoms similar to appendicitis but don’t require surgery. At Hasbro Children’s Hospital (HCH), we evaluate your child’s abdominal pain to determine if appendicitis is the cause. That way, we avoid unnecessary operations. What happens now? Your child will be well cared for. First your child will be seen in the HCH emergency department (ED) by a nurse and doctor trained in pediatric emergency medicine. If necessary, your child will have tests that include blood work and a urinalysis. Your child’s pain will be managed with intravenous (IV) pain medication. Your child will not be allowed to eat or drink and may receive fluids through an intravenous line. Members of the pediatric surgical team will examine your child to help determine whether your child has appendicitis or another condition. We will perform a painless ultrasound on your child and the ultrasound images will be read by pediatric radiology doctors with advanced training in imaging children. Usually, ultrasound is the only imaging required but sometimes an MRI may be needed as well. -

Laparoscopic Management of a Small Bowel Obstruction of Unknown Cause
View metadata, citation and similar papers at core.ac.uk brought to you by CORE CASE REPORT provided by PubMed Central Laparoscopic Management of a Small Bowel Obstruction of Unknown Cause E´lan Burton, MD, John McKeating, MD, Kurt Stahlfeld, MD ABSTRACT INTRODUCTION With the expanding indications for minimally invasive Adhesive small bowel obstruction (SBO) is a common and surgery, the management of small bowel obstruction is frequently encountered problem. If initial conservative evolving. The laparoscope shortens hospital stay, hastens management fails, operative exploration, and lysis of ad- recovery, and reduces morbidity, such as wound infection hesions is required. In patients with multiple previous and incisional hernia associated with open surgery. How- surgeries and significantly dilated small bowel, surgical ever, many surgeons are reluctant to attempt laparoscopy access to the peritoneal cavity can be quite difficult and is in patients with significantly distended small bowel and a associated with significant complications. Traditional dic- history of multiple previous abdominal operations. We tum would state that laparoscopy is contraindicated in present the management of a patient with a virgin abdo- such patients. men who presented with a small bowel obstruction most likely secondary to Fitz-Hugh-Curtis syndrome who was However, we are seeing an increased incidence of SBO in successfully managed with laparoscopic lysis of adhe- patients whose only previous abdominal surgery was via sions. the laparoscope. In these patients, and in those with virgin abdomens, the laparoscopic approach may be the pre- Key Words: Fitz-Hugh-Curtis syndrome, Chilaiditi syn- ferred way to diagnose and treat SBO. The following case drome, Small bowel obstruction. -

Chilaiditi's Syndrome Complicated by Colon Perforation
CASE REPORT Chilaiditi’s syndrome complicated by colon perforation: a case report Turan Acar, M.D., Erdinç Kamer, M.D., Nihan Acar, M.D., Ahmet Er, M.D., Mustafa Peşkersoy, M.D. Department of Surgery, Izmir Katip Celebi University Ataturk Training and Research Hospital, Izmir ABSTRACT Hepatodiaphragmatic interposition of the small or large intestine is known as Chilaiditi syndrome, whichis a rare disease diagnosed incidentally. Chilaiditi syndrome is typically asymptomatic, but it can be associated with symptoms ranging from intermittent, mild ab- dominal pain to acute intestinal obstruction, constipation, chest pain and breathlessness. A 54-year-old male patient was admitted to the hospital with a history of abdominal pain, nausea and vomiting. Chest X-ray revealed an elevation of the right hemidiaphragma caused by the presence of a dilated colonic loop below. The patient underwent urgent surgery with perforation as preliminary diagnosis. The pa- tient underwent right hemicolectomy and ileocolic anastomosis because of the intestinal obstruction related to Chilaiditi’s Syndrome. Due to the rarity of this syndrome and typical radiological findings, this case was aimed to be presented. Key words: Abdominal pain; Chilaiditi’s syndrome; surgery. INTRODUCTION CASE REPORT Interposition of the bowel (usually transverse colon or he- A 54-year-oldmale patient was admitted to the Emergency patic flexura) or the small intestine between the liver and Department of Surgery, Izmir Katip Celebi University Ataturk diaphragm, which is a rare anomaly, was first defined by the Training and Research Hospital with a 24-hour history of right Greek radiologist Demetrius Chilaiditi in 1910.[1,2] It is inci- upper abdominal pain, nausea and vomiting. -

En 17-Chilaiditi™S Syndrome.P65
Nagem RG et al. SíndromeRELATO de Chilaiditi: DE CASO relato • CASE de caso REPORT Síndrome de Chilaiditi: relato de caso* Chilaiditi’s syndrome: a case report Rachid Guimarães Nagem1, Henrique Leite Freitas2 Resumo Os autores apresentam um caso de síndrome de Chilaiditi em uma mulher de 56 anos de idade. Mesmo tratando-se de condição benigna com rara indicação cirúrgica, reveste-se de grande importância pela implicação de urgência operatória que representa o diagnóstico equivocado de pneumoperitônio nesses pacientes. É realizada revisão da li- teratura, com ênfase na fisiopatologia, propedêutica e tratamento desta entidade. Unitermos: Síndrome de Chilaiditi; Sinal de Chilaiditi; Abdome agudo; Pneumoperitônio; Espaço hepatodiafragmático. Abstract The authors report a case of Chilaiditi’s syndrome in a 56-year-old woman. Although this is a benign condition with rare surgical indication, it has great importance for implying surgical emergency in cases where such condition is equivocally diagnosed as pneumoperitoneum. A literature review is performed with emphasis on pathophysiology, diagnostic work- up and treatment of this entity. Keywords: Chilaiditi’s syndrome; Chilaiditi’s sign; Acute abdomen; Pneumoperitoneum; Hepatodiaphragmatic space. Nagem RG, Freitas HL. Síndrome de Chilaiditi: relato de caso. Radiol Bras. 2011 Set/Out;44(5):333–335. INTRODUÇÃO RELATO DO CASO tricos, com pressão arterial de 130 × 90 mmHg. Abdome tenso, doloroso, sem irri- Denomina-se síndrome de Chilaiditi a Paciente do sexo feminino, 56 anos de tação peritoneal, com ruídos hidroaéreos interposição temporária ou permanente do idade, foi admitida na unidade de atendi- preservados. De imediato, foram solicita- cólon ou intestino delgado no espaço he- mento imediato com quadro de dor abdo- dos os seguintes exames: amilase: 94; PCR: patodiafragmático, causando sintomas. -

Nausea and Vomiting (Stomach “Bug” Or Gastroenteritis)
Nausea and Vomiting •(Stomach Nausea and vomiting “Bug” is most commonly or caused Gastroenteritis) by a viral infection and may be associated with diarrhea. • This illness is self-limited with the majority of people finding improvement within 24-hours and are back to normal by 72-hours after onset of the illness. • This illness can be treated at home and does not require a visit to a medical provider. Symptoms: • Nausea with or without vomiting • Muscle aches • Generalized or upper abdominal pain/cramping • Headache • Watery diarrhea (no blood) • Possible fever Self-care measures: • Stop eating solid foods • Rest • Suck on ice chips or sip small amounts of water on a frequent basis • If you vomit, wait about 20 minutes then resume fluid intake • Slowly increase the amount of fluid intake • Water, Pedialyte® or sports drinks are acceptable • Avoid caffeine, alcohol and carbonated beverages • Acetaminophen (Tylenol®) 650 mg every 6 hours as needed for fever, chills, headache or body aches • Use Imodium for diarrhea lasting more than 2 days Recovery: • You may try solid food when: 1) Nausea and vomiting have resolved 2) You are tolerating fluids 3) You feel hungry When you do eat: • Start with small amounts of simple foods (crackers, toast, Jello®, etc.) • Over the next 24-36 hours slowly build up to your normal diet • Add dairy, high-fat foods, raw vegetables, citrus and red meat last Limit spread to others: • Wash hands with soap and water frequently • Stay home (or in your residence hall) for at least the first 24-hours • If you live in a residence hall call 540-568-6949 to get information about obtaining some appropriate food or fluids When to seek medical attention: • If the vomiting persists more than 24-hours • If you develop bloody diarrhea • If you have obvious pain or tenderness isolated to the right lower abdomen UHC self-care guidelines are based on the most recent recommendations of national medical authorities.. -
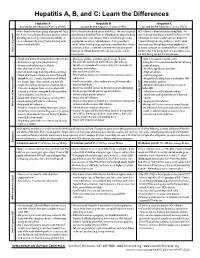
Hepatitis A, B, and C: Learn the Differences
Hepatitis A, B, and C: Learn the Differences Hepatitis A Hepatitis B Hepatitis C caused by the hepatitis A virus (HAV) caused by the hepatitis B virus (HBV) caused by the hepatitis C virus (HCV) HAV is found in the feces (poop) of people with hepa- HBV is found in blood and certain body fluids. The virus is spread HCV is found in blood and certain body fluids. The titis A and is usually spread by close personal contact when blood or body fluid from an infected person enters the body virus is spread when blood or body fluid from an HCV- (including sex or living in the same household). It of a person who is not immune. HBV is spread through having infected person enters another person’s body. HCV can also be spread by eating food or drinking water unprotected sex with an infected person, sharing needles or is spread through sharing needles or “works” when contaminated with HAV. “works” when shooting drugs, exposure to needlesticks or sharps shooting drugs, through exposure to needlesticks on the job, or from an infected mother to her baby during birth. or sharps on the job, or sometimes from an infected How is it spread? Exposure to infected blood in ANY situation can be a risk for mother to her baby during birth. It is possible to trans- transmission. mit HCV during sex, but it is not common. • People who wish to be protected from HAV infection • All infants, children, and teens ages 0 through 18 years There is no vaccine to prevent HCV. -

Travelers' Diarrhea
Travelers’ Diarrhea What is it and who gets it? Travelers’ diarrhea (TD) is the most common illness affecting travelers. Each year between 20%-50% of international travelers, an estimated 10 million persons, develop diarrhea. The onset of TD usually occurs within the first week of travel but may occur at any time while traveling and even after returning home. The primary source of infection is ingestion of fecally contaminated food or water. You can get TD whenever you travel from countries with a high level of hygiene to countries that have a low level of hygiene. Poor sanitation, the presence of stool in the environment, and the absence of safe restaurant practices lead to widespread risk of diarrhea from eating a wide variety of foods in restaurants, and elsewhere. Your destination is the most important determinant of risk. Developing countries in Latin America, Africa, the Middle East, and Asia are considered high risk. Most countries in Southern Europe and a few Caribbean islands are deemed intermediate risk. Low risk areas include the United States, Canada, Northern Europe, Australia, New Zealand, and several of the Caribbean islands. Anyone can get TD, but persons at particular high-risk include young adults , immunosuppressed persons, persons with inflammatory-bowel disease or diabetes, and persons taking H-2 blockers or antacids. Attack rates are similar for men and women. TD is caused by bacteria, protozoa or viruses that are ingested by eating contaminated food or beverages. For short-term travelers in most areas, bacteria are the cause of the majority of diarrhea episodes. What are common symptoms of travelers’ diarrhea? Most TD cases begin abruptly. -

Case Study of 100 Cases of Intestinal Obstruction
CASE STUDY OF 100 CASES OF INTESTINAL OBSTRUCTION Dissertation submitted in partial fulfillment of the Requirement for the award of the degree of MS DEGREE EXAMINATION GENERAL SURGERY TIRUNELVELI TIRUNELVELI MEDICAL COLLEGE THE TAMILNADU DR.M.G.R MEDICAL UNIVERSITY CHENNAI,TAMILNADU APRIL 2013 CERTIFICATE This is to certify that the dissertation titled “CASE STUDY OF 100 CASES OF INTESTINAL OBSTRUCTION “ is the original work done by DR.VARGHESE THOMAS,post graduate in Dept. Of General Surgery,Tirunelveli medical college,to be submitted to the TAMIL NADUDr.MGR Medical University Chennai-32 towards the partial fulfillment of the requirement for the award of MS Degree in General Surgery, April 2013. Prof.Dr.S.Soundararajan MS Dr.M.Manoharan MS Unit Chief Professor & The DEAN Head Of Department Tirunelveli Medical College Department of General Surgery Tirunelveli Tirunelveli Medical College Tirunelveli ii ACKNOWLEDGEMENT It is a great pleasure to express my deep sense of gratitude and heartfelt thanks to My beloved teacher and guide, Dr.S.Soundararajan MS Prof & HOD Dept. of General Surgery, Tirunelveli medical college. For his patient guidance, constant inspiration, scholarly suggestions, timely advice and encouragement in my tenure as a postgraduate. I am extremely grateful to Dr.Maheswari MS, Dr. Pandy MS, Dr.Varadharajan MS. Dr.Alex Edward MS, Dr.Sreethar MS, Dr.Manoharan MS, for their profound knowledge, encouragement and guidance during the study period. I am extremely grateful to my Assistant Professors, Dr.Raju MS and Dr.Rajkumar MS for their constant inspiration, invaluable guidance, constant supervision and timely advice in preparing this dissertation and also in my tenure as a postgraduate. -

Chapter 34 • Drugs Used to Treat Nausea and Vomiting
• Chapter 34 • Drugs Used to Treat Nausea and Vomiting • Learning Objectives • Compare the purposes of using antiemetic products • State the therapeutic classes of antiemetics • Discuss scheduling of antiemetics for maximum benefit • Nausea and Vomiting • Nausea : the sensation of abdominal discomfort that is intermittently accompanied by a desire to vomit • Vomiting (emesis): the forceful expulsion of gastric contents up the esophagus and out of the mouth • Regurgitation : the rising of gastric or esophageal contents to the pharynx as a result of stomach pressure • Common Causes of Nausea and Vomiting • Postoperative nausea and vomiting • Motion sickness • Pregnancy Hyperemesis gravidarum: a condition in pregnancy in which starvation, dehydration, and acidosis are superimposed on the vomiting syndrome • Common Causes of Nausea and Vomiting (cont’d) • Psychogenic vomiting: self-induced or involuntary vomiting in response to threatening or distasteful situations • Chemotherapy-induced emesis (CIE) Anticipatory nausea and vomiting: triggered by sight and smell associated with treatment Acute CIE: stimulated directly by chemotherapy 1 to 6 hours after treatment Delayed emesis: occurs 24 to 120 hours after treatment; may be induced by metabolic by-products of chemotherapy • Drug Therapy for Selected Causes of Nausea and Vomiting • Postoperative nausea and vomiting (PONV) • Antiemetics include: Dopamine antagonists Anticholinergic agents Serotonin antagonists H2 antagonists (cimetidine, ranitidine) • Nursing Process for Nausea and Vomiting