Stomach Flu (Viral Gastroenteritis)
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

IRRITABLE BOWEL SYNDROME by Michael Sperling MD
IRRITABLE BOWEL SYNDROME By Michael Sperling MD Irritable bowel syndrome (IBS) involves vague symptoms of abdominal pain, diarrhea, constipation, gas and bloating for which there is no understandable cause. Incredibly, IBS affects up to 20% of the population but only three- quarters of those people actually seek medical attention. It is the second most common reason for work absenteeism. Irritable bowel symptoms may also be related to other complaints such as belching, heartburn, swallowing problems, fullness after eating, nausea, frequent urination, painful menstruation and pain during intercourse. Extremely severe cases can sometimes be related to a history of traumatic abuse. Some common associations or factors: Michael Sperling, MD 1. ‘Spastic colon’ is frequently found along with irritable bowel syndrome. Spastic colon consists of painful muscle contractions which can be relieved by bulk agents or anti- spasm drugs. 2. Post-infectious IBS occurs when irritable bowel follows a gastrointestinal infection, such as the stomach flu. These recurrent symptoms can last up to two years. 3. Stress and anxiety can worsen IBS symptoms so occasionally anti-anxiety agents may be helpful. 4. Food intolerances classically worsen symptoms of irritable bowel in some people. Common “offending foods” include lactose, legumes (beans) and cruciferous vegetables like brussel sprouts, cauliflower, broccoli and cabbage. 5. Hypersensitivity of the bowel wall: Normal colon activity is not usually noticed however in “visceral hypersensitivity”, the bowel wall reacts painfully to normal activity. This condition may be helped by the use of low dose antidepressants, which can block these painful stimuli. Careful and selective testing of patients with these symptoms and the development of a long-term doctor/patient relationship is the key to diagnosing and managing these symptoms. -

Campylobacter:What You Need to Know
Queensland Health Campylobacter: what you need to know Campylobacter is one of the most Age groups most at risk common causes of foodborne illness Under in Australia. 60+ You can’t see it, smell it or even taste it on food, but if 5s it affects you, you won’t forget it. What is Campylobacter? Campylobacter is a little known foodborne bacteria similar to Salmonella. * In some cases Campylobacter can also lead to irritable 230,000 bowel syndrome, reactive arthritis and in rare cases cases a year Guillain-Barré syndrome—a type of paralysis. How do you get it? Most cases of Campylobacter infection are associated ** with eating raw or undercooked poultry or by cross 3200 contamination. hospitalisations as It is important to keep raw poultry and their juices a result of foodborne away from any already cooked or ready-to-eat foods illness caused by and fresh produce. Campylobacter Who is at risk? Anyone can be affected by Campylobacter but certain $1.25 billion people are at a greater risk for severe illness including annual total cost to society young children (under 5 years), older adults (over 60 for foodborne illness in years) and people with weakened immunity. Australia How to prevent it The easiest way to protect yourself and your family is to follow our four food safety tips every time you prepare raw poultry. ! Symptoms of Campylobacter Campylobacter infections cause gastroenteritis Follow these four safety tips (commonly known as gastro) diarrhoea, abdominal pains, cramping and fever. to prevent foodborne illness Symptoms usually start two to five days after from Campylobacter infection, and can last for one to three weeks. -

Astroviruses As Causative Agents of Gastroenteritis
Under the Microscope Astroviruses as causative agents of gastroenteritis with other enteric pathogens, especially rotaviruses, are known. Most infections in adults are asymptomatic. In other mammalian species, infection results in diarrhoea and gastroenteritis, while infection in birds leads to extraintestinal diseases, including Enzo A Palombo interstitial nephritis in young chicks and acute hepatitis in Environment and Biotechnology ducklings2. Centre Faculty of Life and Social Sciences Swinburne University of Epidemiology Technology Hawthorn VIC 3122 The first description of astrovirus came in 1975 after electron microscopic analysis of diarrhoeal stool samples from infants3,4. Astroviruses were first identified over 30 years ago and The unusual appearance of the virion particles (10% show a the virus was soon established as an important cause of characteristic five- or six-pointed star pattern on their surface) gastroenteritis, particularly in young children. Human indicated a previously unrecognised virus. Astroviruses have astrovirus disease was thought to result from infection since been reported worldwide in samples from infants and by a limited number of serotypes. However, recent young children with gastroenteritis. Soon after the first report in studies have indicated that the extent of genetic diversity humans, astrovirus-like particles were observed in domesticated is greater than previously assumed. In addition, the animals. There is now abundant evidence that astroviruses are widespread occurrence among animals and reports of widespread among domestic, synanthropic and wild animals, avian recombination and possible cross-species transmission and mammalian species in terrestrial and aquatic environments1. suggest that astroviruses have zoonotic potential. The list of animal species from which astroviruses have been Astroviruses are small (28–30 nm), non-enveloped viruses identified (chronologically) includes sheep, cattle, chickens, belonging to the family Astroviridae. -

Acute Pancreatitis Associated with Rotavirus Infection and Review Of
Case Report/Olgu Sunumu İstanbul Med J 2020; 21(1): 78-81 DO I: 10.4274/imj.galenos.2020.88319 Acute Pancreatitis Associated with Rotavirus Infection and Review of The Literature Rotavirüs Enfeksiyonuna Bağlı Akut Pankreatit Olguları ve Literatürün Gözden Geçirilmesi Kamil Şahin, Güzide Doğan University of Health Sciences, Haseki Training and Research Hospital, Department of Pediatrics, İstanbul, Turkey ABSTRACT ÖZ Agents causing acute gastroenteritis are not common causes of Çocuklarda pankreatit etiyolojisinde akut gastroenterit etkenleri pancreatitis etiology in children. Pancreatitis associated with sık görülen sebeplerden değildir. Rotavirüs enfeksiyonuna rotavirus infection is very rare. Cases with acute pancreatitis bağlı görülen pankreatit ise oldukça nadirdir. Rotavirüs during rotavirus gastroenteritis are reported due to rare gastroenteriti sırasında akut pankreatit gelişen olgular, associations. In this article, the causes of acute pancreatitis rotavirüs enfeksiyonuna bağlı akut pankreatitin nadir olması and cases of acute pancreatitis due to rotavirus infection were nedeniyle sunulmuştur. Bu yazıda, akut pankreatit sebepleri ve investigated. Clinical findings were mild, and complications rotavirüse bağlı gelişen akut pankreatit olguları incelenmiştir. were not observed in both of our patients, including a two- İki yaş kız ve üç yaşındaki erkek iki olgumuzda ve literatürde year-old female and a three-year-old male, and other cases değerlendirilen diğer olgularda klinik bulgular hafif seyretmiş, evaluated in the literature. The -

Hepatitis C – Screening, Diagnosis, Management & Treatment
12 Osteopathic Family Physician (2019) 12 - 19 Osteopathic Family Physician | Volume 11, No. 1 | January/February, 2019 Review ARTICLE Hepatitis C – Screening, Diagnosis, Management & Treatment Michael Ferraro, DO & Matthew StantsPainter, DO Washington Health System Family Medicine Residency Program, Washington, PA KEYWORDS: Abstract: Hepatitis C virus (HCV) infection is a major cause of chronic liver disease, hepatocellular carcinoma and cirrhosis with at least 185 million people infected worldwide, causing 399,000 deaths Disease Prevention annually. HCV is transmitted through blood or body fluids. Transmission most commonly occurs and Wellness through sharing of injection drug, occupational exposure through needlestick injuries in healthcare Hepatitis C settings, and birth to an HCV infected mother. There are seven known genotypes of HCV, 1a, 1b, 2, 3, 4, 5, and 6, with the most common genotypes in the U.S. being 1a, 1b, 2, and 3, which comprise Infectious Disease approximately 97% of all U.S. HCV infections. Risks for disease progression include baseline liver histology, age, ethnicity, gender, alcohol use, comorbidities and immune response. There are Jaundice multiple screening recommendations currently in place, some of which are based on risk factors, Transaminitis with others based on legislation. The screening test of choice is the anti-Hepatitis C virus antibody, with a confirmatory HCV RNA PCR with genotyping. Once the diagnosis is made, assessing the level of fibrosis and/or cirrhosis is an important step in determining the pathway to treatment. There are multiple new options for treatment with improved efficacy and less side effects. Patient being treated for HCV should be monitored and assessed for compliance with therapy and adverse effects, including new or worsening psychiatric illness and screened for alcohol and substance abuse. -

Acute Gastroenteritis
Article gastrointestinal disorders Acute Gastroenteritis Deise Granado-Villar, MD, Educational Gap MPH,* Beatriz Cunill-De Sautu, MD,† Andrea In managing acute diarrhea in children, clinicians need to be aware that management Granados, MDx based on “bowel rest” is outdated, and instead reinstitution of an appropriate diet has been associated with decreased stool volume and duration of diarrhea. In general, drug therapy is not indicated in managing diarrhea in children, although zinc supplementation Author Disclosure and probiotic use show promise. Drs Granado-Villar, Cunill-De Sautu, and Objectives After reading this article, readers should be able to: Granados have disclosed no financial 1. Recognize the electrolyte changes associated with isotonic dehydration. relationships relevant 2. Effectively manage a child who has isotonic dehydration. to this article. This 3. Understand the importance of early feedings on the nutritional status of a child who commentary does has gastroenteritis. contain a discussion of 4. Fully understand that antidiarrheal agents are not indicated nor recommended in the an unapproved/ treatment of acute gastroenteritis in children. investigative use of 5. Recognize the role of vomiting in the clinical presentation of acute gastroenteritis. a commercial product/ device. Introduction Acute gastroenteritis is an extremely common illness among infants and children world- wide. According to the Centers for Disease Control and Prevention (CDC), acute diarrhea among children in the United States accounts for more than 1.5 million outpatient visits, 200,000 hospitalizations, and approximately 300 deaths per year. In developing countries, diarrhea is a common cause of mortality among children younger than age 5 years, with an estimated 2 million deaths each year. -

Appendicitis
Appendicitis Your child has abdominal pain, it might be appendicitis. Appendicitis is swelling or infection in the appendix. The appendix is a small organ attached to the large intestine. Appendicitis usually develops over 12-24 hours. It has symptoms such as abdominal pain, nausea, vomiting, fever, and loss of appetite. Most importantly, pain that continues, worsens and moves to the right lower side of the abdomen is common in appendicitis. Appendicitis is the most common childhood “emergency” that must be treated in a timely manner. However, it’s important to know that many conditions have symptoms similar to appendicitis but don’t require surgery. At Hasbro Children’s Hospital (HCH), we evaluate your child’s abdominal pain to determine if appendicitis is the cause. That way, we avoid unnecessary operations. What happens now? Your child will be well cared for. First your child will be seen in the HCH emergency department (ED) by a nurse and doctor trained in pediatric emergency medicine. If necessary, your child will have tests that include blood work and a urinalysis. Your child’s pain will be managed with intravenous (IV) pain medication. Your child will not be allowed to eat or drink and may receive fluids through an intravenous line. Members of the pediatric surgical team will examine your child to help determine whether your child has appendicitis or another condition. We will perform a painless ultrasound on your child and the ultrasound images will be read by pediatric radiology doctors with advanced training in imaging children. Usually, ultrasound is the only imaging required but sometimes an MRI may be needed as well. -

Campylobacteriosis
Zoonotic Disease Prevention Series for Retailers Campylobacteriosis www.pijac.org Disease Vectors Campylobacteriosis is a bacterial disease typically causing gastroenteritis in humans. Several species of Campylobacter may cause ill- ness in livestock (calves, sheep, pigs) and companion animals (dogs, cats, ferrets, parrots). Among pets, dogs are more likely to be infected than cats; symptoms present primarily in animals less than 6 months old. Most cases of human campylobacteriosis result from exposure to contaminated food (particularly poultry), raw milk or water, but the bacteria may be transmitted via the feces of companion animals, typically puppies or kittens recently introduced to a household. The principal infectious agent in human cases, C. jejuni, is common in commercially raised chickens and turkeys that seldom show signs of illness. Dogs and cats may be infected through undercooked meat in their diets or through exposure to feces in crowded conditions. Campylobacter prevalence is higher in shelters than in household pets. Campylobacter infection should be considered in recently acquired puppies with diarrhea. Symptoms , Diagnosis and Treatment Symptoms of Campylobacter infection in humans typically oc- Antibiotic resistance has been documented among cur 2-5 days after exposure and include diarrhea (sometimes various Campylobacter species and subspecies. There- bloody), cramping, abdominal pain, fever, nausea and vomit- fore treatment should be under the direction of a ing. In the vast majority of cases, the illness resolves itself veterinarian. Typically, antibiotic therapy is reserved without treatment, generally within a week, and antibiotics are for young animals or pets with severe symptoms, but seldom recommended. Symptoms may be treated by in- treatment of symptomatic pets may be appropriate in creased fluid and electrolyte intake to counter the effects of households to reduce the risk of human infection. -

Nausea and Vomiting (Stomach “Bug” Or Gastroenteritis)
Nausea and Vomiting •(Stomach Nausea and vomiting “Bug” is most commonly or caused Gastroenteritis) by a viral infection and may be associated with diarrhea. • This illness is self-limited with the majority of people finding improvement within 24-hours and are back to normal by 72-hours after onset of the illness. • This illness can be treated at home and does not require a visit to a medical provider. Symptoms: • Nausea with or without vomiting • Muscle aches • Generalized or upper abdominal pain/cramping • Headache • Watery diarrhea (no blood) • Possible fever Self-care measures: • Stop eating solid foods • Rest • Suck on ice chips or sip small amounts of water on a frequent basis • If you vomit, wait about 20 minutes then resume fluid intake • Slowly increase the amount of fluid intake • Water, Pedialyte® or sports drinks are acceptable • Avoid caffeine, alcohol and carbonated beverages • Acetaminophen (Tylenol®) 650 mg every 6 hours as needed for fever, chills, headache or body aches • Use Imodium for diarrhea lasting more than 2 days Recovery: • You may try solid food when: 1) Nausea and vomiting have resolved 2) You are tolerating fluids 3) You feel hungry When you do eat: • Start with small amounts of simple foods (crackers, toast, Jello®, etc.) • Over the next 24-36 hours slowly build up to your normal diet • Add dairy, high-fat foods, raw vegetables, citrus and red meat last Limit spread to others: • Wash hands with soap and water frequently • Stay home (or in your residence hall) for at least the first 24-hours • If you live in a residence hall call 540-568-6949 to get information about obtaining some appropriate food or fluids When to seek medical attention: • If the vomiting persists more than 24-hours • If you develop bloody diarrhea • If you have obvious pain or tenderness isolated to the right lower abdomen UHC self-care guidelines are based on the most recent recommendations of national medical authorities.. -
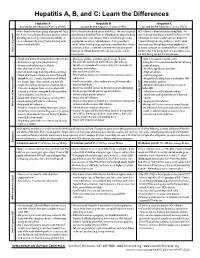
Hepatitis A, B, and C: Learn the Differences
Hepatitis A, B, and C: Learn the Differences Hepatitis A Hepatitis B Hepatitis C caused by the hepatitis A virus (HAV) caused by the hepatitis B virus (HBV) caused by the hepatitis C virus (HCV) HAV is found in the feces (poop) of people with hepa- HBV is found in blood and certain body fluids. The virus is spread HCV is found in blood and certain body fluids. The titis A and is usually spread by close personal contact when blood or body fluid from an infected person enters the body virus is spread when blood or body fluid from an HCV- (including sex or living in the same household). It of a person who is not immune. HBV is spread through having infected person enters another person’s body. HCV can also be spread by eating food or drinking water unprotected sex with an infected person, sharing needles or is spread through sharing needles or “works” when contaminated with HAV. “works” when shooting drugs, exposure to needlesticks or sharps shooting drugs, through exposure to needlesticks on the job, or from an infected mother to her baby during birth. or sharps on the job, or sometimes from an infected How is it spread? Exposure to infected blood in ANY situation can be a risk for mother to her baby during birth. It is possible to trans- transmission. mit HCV during sex, but it is not common. • People who wish to be protected from HAV infection • All infants, children, and teens ages 0 through 18 years There is no vaccine to prevent HCV. -

Eosinophilic Gastroenteritis Complicating Perforation in a Hepatitis C Patient Treated with Direct-Acting Antivirals
Case Study Clinical Case Reports International Published: 18 Feb, 2020 Eosinophilic Gastroenteritis Complicating Perforation in a Hepatitis C Patient Treated with Direct-Acting Antivirals Ming X Huang1, Chun N Li1, Ruo M Ke1, Zuo Q Zhang2, Zhe Zhu3 and Xiao M Peng1,4* 1Department of Infectious Diseases, Sun Yat-Sen University, China 2Department of Radiology, Sun Yat-Sen University, China 3Department of Medicine, University of California, USA 4Central Laboratory, Sun Yat-Sen University, China Abstract The Direct-Acting Antiviral (DAA) therapy of Hepatitis C Virus (HCV) infection has demonstrated excellent efficacy and safety profile. Based on large cohort studies, Serious Adverse Events (SAEs) are rare [1,2]. Here, we reported the first case of a patient with alcoholic liver cirrhosis super infected by HCV presenting with a SAE of Eosinophilic Gastro Enteritis (EGE) complicating acute perforation during daclatasvir plus sofosbuvir therapy. Abbreviations CT: Computed Tomography; DAA: Direct-Acting Antiviral; EGE: Eosinophilic Gastro Enteritis; HCV: Hepatitis C Virus; SAE: Serious Adverse Event Case Presentation A 58-year-old Chinese man with history of alcoholic liver cirrhosis (Child-Pugh A) more than 10 years had been diagnosed with HCV infection (serum HCV RNA 6.85 logIU/mL, genotype 6a) and was treated with daclatasvir plus sofosbuvir. (Velpanat composed of velpatasvir 100 mg plus sofosbuvir 400 mg) The patient’s virological response was achieved at week 7, but his peripheral eosinophils rose from normal baseline to 2.79 × 109/L (Figure 1). Since the patient was asymptomatic, OPEN ACCESS the dual therapy was continued. On September 24, 2017 (about at week 8), the man was hospitalized *Correspondence: due to sudden severe right upper abdominal pain, abdominal distention and a fever of 38.9°C. -

Travelers' Diarrhea
Travelers’ Diarrhea What is it and who gets it? Travelers’ diarrhea (TD) is the most common illness affecting travelers. Each year between 20%-50% of international travelers, an estimated 10 million persons, develop diarrhea. The onset of TD usually occurs within the first week of travel but may occur at any time while traveling and even after returning home. The primary source of infection is ingestion of fecally contaminated food or water. You can get TD whenever you travel from countries with a high level of hygiene to countries that have a low level of hygiene. Poor sanitation, the presence of stool in the environment, and the absence of safe restaurant practices lead to widespread risk of diarrhea from eating a wide variety of foods in restaurants, and elsewhere. Your destination is the most important determinant of risk. Developing countries in Latin America, Africa, the Middle East, and Asia are considered high risk. Most countries in Southern Europe and a few Caribbean islands are deemed intermediate risk. Low risk areas include the United States, Canada, Northern Europe, Australia, New Zealand, and several of the Caribbean islands. Anyone can get TD, but persons at particular high-risk include young adults , immunosuppressed persons, persons with inflammatory-bowel disease or diabetes, and persons taking H-2 blockers or antacids. Attack rates are similar for men and women. TD is caused by bacteria, protozoa or viruses that are ingested by eating contaminated food or beverages. For short-term travelers in most areas, bacteria are the cause of the majority of diarrhea episodes. What are common symptoms of travelers’ diarrhea? Most TD cases begin abruptly.