5Th Common Review Mission BIHAR Team Members
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Begusarai.Pdf
भूजल सूचना पुस्तिका बेगुसराय स्जला, बबहार Ground Water Information Booklet Begusarai District, Bihar State के न्द्रीय भमू िजल बो셍 ड Central Ground water Board जल संसाधन िंत्रालय Ministry of Water Resources (भारि सरकार) (Govt. of India) म鵍य-पूर्वी क्षेत्र Mid-Eastern Region पटना Patna ससिंबर 2013 September 2013 1 PREPARED BY - Sri R.R. Shukla, Sc-C - 2 Ground Water Information Booklet Begusarai District, Bihar State CONTENTS S.No TITLES PAGE NO. 1.0 Introduction 4 1.1 Administration 1.2 Basin/sub-basin, Drainage 1.3 Irrigation Practices 1.4 Studies/Activities by CGWB 2.0 Climate and Rainfall 8 3.0 Geomorphology and Soil types 8-10 4.0 Ground Water Scenario 10-15 4.1 Hydrogeology 4.2 Ground Water Resources 4.3 Chemical Quality of Groundwater 4.4 Status of Ground Water Development 5.0 Ground Water Management Strategy 15-16 5.1 Ground Water Development 5.2 Water Conservation and Artificial Recharge 6.0 Ground Water related issue and problems 16-17 7.0 Mass Awareness and Training Activity 17 8.0 Area Notified by CGWB/SGWA 17 9.0 Recommendations 17 FIGURE 1.0 Index Map of Begusarai district 7 2.0 Hydrogeological map of Begusarai district 11 3.0 Pre monsoon (May 2011) map of Begusarai district 12 4.0 Post monsoon (November 2011) map of Begusarai district 12 5.0 Blockwise Stage of Ground Water Development of 14 Begusarai district TABLE 1.0 Exploratory wells drilled by CGWB in Begusarai district 10 2.0 Block wise dynamic ground water resources of Begusarai 11 district 3.0 Range of different chemical constituents in ground of Begusarai 13 district 3 BEGUSARAI DISTRICT AT A GLANCE Sl. -

Deo List Bihar
Details of DEO-cum-DM Sl. No. District Name Name Designation E-mail Address Mobile No. 1 2 3 4 5 6 1 PASCHIM CHAMPARAN Kundan Kumar District Election Officer [email protected] 9473191294 2 PURVI CHAMPARAN Shirsat Kapil Ashok District Election Officer [email protected] 9473191301 3 SHEOHAR Avaneesh Kumar Singh District Election Officer [email protected] 9473191468 4 SITAMARHI Abhilasha Kumari Sharma District Election Officer [email protected] 9473191288 5 MADHUBANI Nilesh Ramchandra Deore District Election Officer [email protected] 9473191324 6 SUPAUL Sri Mahendra KUMAR District Election Officer [email protected] 9473191345 7 ARARIA Prashant Kumar District Election Officer [email protected] 9431228200 8 KISHANGANJ Aditya Prakash District Election Officer [email protected] 9473191371 9 PURNIA Rahul Kumar District Election Officer [email protected] 9473191358 10 KATIHAR Kanwal Tanuj District Election Officer [email protected] 9473191375 11 MADHEPURA Navdeep Shukla District Election Officer [email protected] 9473191353 12 SAHARSA Kaushal kumar District Election Officer [email protected] 9473191340 13 DARBHANGA Shri Thiyagrajan S. M. District Election Officer [email protected] 9473191317 14 MUZAFFARPUR Chandra Shekhar Singh District Election Officer [email protected] 9473191283 15 GOPALGANJ Arshad Aziz District Election Officer [email protected] 9473191278 16 SIWAN Amit Kumar Pandey District Election Officer [email protected] 9473191273 17 SARAN Subrat Kumar Sen District -

Observed Rainfall Variability and Changes Over Bihar State
CLIMATE RESEARCH AND SERVICES INDIA METEOROLOGICAL DEPARTMENT MINISTRY OF EARTH SCIENCES PUNE Observed Rainfall Variability and Changes over Bihar State Met Monograph No. : ESSO/IMD/HS/Rainfall Variability/04(2020)/28 Pulak Guhathakurta, Sudeepkumar B L, Preetha Menon, Ashwini Kumar Prasad, Neha Sangwan and S C Advani GOVERNMENT OF INDIA MINISTRY OF EARTH SCIENCES INDIA METEOROLOGICAL DEPARTMENT Met Monograph No.: ESSO/IMD/HS/Rainfall Variability/04(2020)/28 Observed Rainfall Variability and Changes Over Bihar State Pulak Guhathakurta, Sudeepkumar B L, Preetha Menon, Ashwini Kumar Prasad, Neha Sangwan and S C Advani INDIA METEOROLOGICAL DEPARTMENT PUNE - 411005 1 DOCUMENT AND DATA CONTROL SHEET 1 Document Title Observed Rainfall Variability and Changes Over Bihar State 2 Issue No. ESSO/IMD/HS/Rainfall Variability/04(2020)/28 3 Issue Date January 2020 4 Security Unclassified Classification 5 Control Status Uncontrolled 6 Document Type Scientific Publication 7 No. of Pages 27 8 No. of Figures 42 9 No. of References 4 10 Distribution Unrestricted 11 Language English 12 Authors Pulak Guhathakurta, Sudeepkumar B L, Preetha Menon, Ashwini Kumar Prasad, Neha Sangwan and S C Advani 13 Originating Division/ Climate Research Division/ Climate Application & Group User Interface Group/ Hydrometeorology 14 Reviewing and Director General of Meteorology, India Approving Authority Meteorological Department, New Delhi 15 End users Central and State Ministries of Water resources, agriculture and civic bodies, Science and Technology, Disaster Management Agencies, Planning Commission of India 16 Abstract India is in the tropical monsoon zone and receives plenty of rainfall as most of the annual rainfall during the monsoon season every year. However, the rainfall is having high temporal and spatial variability and due to the impact of climate changes there are significant changes in the mean rainfall pattern and their variability as well as in the intensity and frequencies of extreme rainfall events. -

District Health Society Begusarai
DISTRICT HEALTH ACTION PLAN 2012-2013 DISTRICT HEALTH SOCIETY BEGUSARAI-1- Foreword This District Health Action Plan (DHAP) is one of the key instruments to achieve NRHM goals. This plan is based on health needs of the district and recognizing the importance of Health in the process of economic and social development and improving the quality of life of our citizens, the Government of India has resolved to launch the National Rural Health Mission to carry out necessary architectural correction in the basic health care delivery system. After a thorough situation analysis of district health scenario this document has been prepared. In the plan, it is addressing health care needs of rural poor especially women and children, the teams have analyzed the coverage of poor women and children with preventive and primitive interventions, barriers in access to health care and spread of human resources catering health needs in the district. The focus has also been given on current availability of health care infrastructure in public/NGO/private sector, availability of wide range of providers. This DHAP has been evolved through a participatory and consultative process, wherein community and other stakeholders have participated and ascertained their specific health needs in villages, problems in accessing health services, especially poor women and children at local level. The goals of the Mission are to improve the availability of and access to quality health care by people, especially for those residing in rural areas, the poor, women and children. I need to congratulate the department of Health and Family Welfare and State Health Society of Bihar for their dynamic leadership of the health sector reform programme and we look forward to a rigorous and analytic documentation of their experiences so that we can learn from them and replicate successful strategies. -
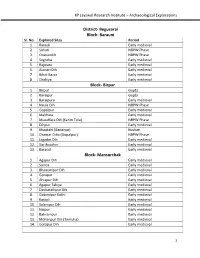

Begusarai Block- Barauni Sl
KP Jayswal Research Institute – Archaeological Explorations District- Begusarai Block- Barauni Sl. No. Explored Sites Period 1. Ratauli Early medieval 2. Sahuri NBPW Phase 3. Chanandih NBPW Phase 4. Sograha Early medieval 5. Rajwara Early medieval 6. Asurari Dih Early medieval 7. Bihat Bazar Early medieval 8. Chakiya Early medieval Block- Birpur 1. Birpur Gupta 2. Baraipur Gupta 3. Baraipura Early medieval 4. Naula Dih NBPW Phase 5. Gopalpur Early medieval 6. Makhwa Early medieval 7. Muzaffara Dih (Karim Tola) NBPW Phase 8. Dihpur Early medieval 9. Khaptahi (Badaiyar) Kushan 10. Chamar Diha (Gopalpur) NBPW Phase 11. Jagadar Dih Early medieval 12. Garihuather Early medieval 13. Baracol Early medieval Block- Mansurchak 1. Agapur Dih Early medieval 2. Samsa Early medieval 3. Bhawanipur Dih Early medieval 4. Gorapur Early medieval 5. Ahiapur Dih Early medieval 6. Agapur Takiya Early medieval 7. Dasharathpur Dih Early medieval 8. Gobindpur Kothi Early medieval 9. Kastoli Early medieval 10. Salampur Dih Early medieval 11. Naipur Early medieval 12. Bahrampur Early medieval 13. Mohanpur Dih (Temuha) Early medieval 14. Gorapur Dih Early medieval 1 KP Jayswal Research Institute – Archaeological Explorations Block- Bachhwara 1. Chiranjipur Dih Early medieval 2. Chamraha Dih (Fateha) Early medieval 3. Majhos Dih Early medieval 4. Rajapur Dih Early medieval 5. Bharaul Dih NBPW Phase 6. Bhikam chak Dih Early medieval 7. Chilawa Dih Early medieval 8. Rasidpur Dih Early medieval 9. Rudauli Dih Early medieval 10. Arwa Dih NBPW Phase 11. Bachhwara Dih Early medieval 12. Maranchi Dih Early medieval Block- Chhorahi 1. Narayanpipra Early medieval 2. Gauri Dih Early medieval 3. Lakhanpatti Dih Early medieval 4. -

BEGUSARAI DISTRICT GA 05.Pdf
85°50'0"E 86°0'0"E 86°10'0"E 86°20'0"E 86°30'0"E GEOGRAPHICAL AREA N N BEGUSARAI DISTRICT " " 0 0 ' ' 0 0 5 5 ° ° 5 5 2 ± 2 KEY MAP B I H A R ! Sihman Ñ ! Amari Ñ CA-12 ! Daulatpur KHUDABANDPUR ! Malipur! Korai a" Police Station ! Bariarpu!r - Chhorahi ! ! Sujanpur ! Phaphot ! ! Pansalla N Jana N " ! Narayanpipar " 0 0 ' ! Khodawandpur ' 0 0 4 ! 4 ° a" Police Station Parora P!olice Station ° 5 - Khodabandpur a" 5 2 - Garhpura 2 CA-13 ! Ekamba Á! Total Geographical Area (Sq Km) 1,918 ! !Meghaul MANSURCHAK ! Gopalpur ! Gobindpur (Part in Bachwara) * CA-09 ! Kumharson Total Population 29,70,541 ! Sakarbasa ! ! Santha Rasidpur CHHORAHI Total Household 5,89,667 Á! (! Mansur Chak Á! ! ! Chiranjipur Shahpur ! Ganpatau!l ! Sonwan ! Chak Hamid No. of Charge Area 18 Shamsa ! ! Basahi ! khanjahanpur ! Rajaur Salauna ! Gobindpur (Part in Mansur Chak) * ! CHARGE CHARGE ! Karor Sanjat ! Ghaghra ! NAME NAME ! Fateha ! Rudauli ! Siripur Á AREA ID AREA ID (! Bakhri ! CA-08 Bikrampur CA - 01 Bachhwara CA - 10 Dandari Á! ! Arwa ! Mukhtiarpur CHERIA-BARIARPUR ! CA-02 CA - 02 Bakhri CA - 11 Garhpura ! Kadrabad a" Police Station - Aadarsh ! Dadupur ! Police Station CA-06 a" ! Shahpur BAKHRI CA - 03 Balia CA - 12 Khudabandpur - Bachhwara BHAGWANPUR CA-15 CA - 04 Barauni CA - 13 Mansurchak ! ! Majhaul ! Chamtha CA-01 ! Chanaur ! Pabra ! ! Rani ! Naula ! NAOKOTHI CA - 05 Begusarai CA - 14 Matihani ! ! Samsa BACHHWARA Pahsara CA - 06 Bhagwanpur CA - 15 Naokothi ! Damodarpur ! Godhna ! Bhawanandpur ! ! Parihara CA - 07 Birpur CA - 16 Sahebpur Kamal ! Razakpur ! -
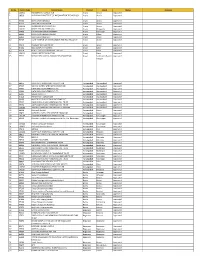

Sl. No. Centre Code Centre Name District Block Status Reasons 1 100935 PARAMPARA FOUNDATION Araria Araria Approved 2 98590 VIVEK
Sl. No. Centre Code Centre Name District Block Status Reasons 1 100935 PARAMPARA FOUNDATION Araria Araria Approved 2 98590 VIVEKANAND INSTITUTE OF INFORMATION TECHNOLOGY Araria Araria Approved 3 97500 DIVYA DRISTI BHARAT Araria Araria Approved 4 97613 SARTHAK FOUNDATION Araria Araria Approved 5 100610 AMBEDKAR SEVA SANSTHAN Araria Araria Approved 6 100101 YOUTH FORUM FORBEGANJ Araria Bhargama Approved 7 97688 LOK PRAGATI SEWA SANSTHAN Araria Kursakata Approved 8 98440 DIVYA DRISTI BHARAT PALASI Araria Palasi Approved 9 96053 SMB CLOUD INFOTECH Arwal Arwal Approved 10 96459 CICAT INSTITUE OF MANAGEMENT AND TECHNOLOGFY Arwal Arwal Approved 11 97015 PRABHAT WELFARE TRUST Arwal Arwal Approved 12 97434 MAX COMPUTER CENTRE Arwal Kaler Approved 13 96154 PERFECT DATATECH PRIVATE LIMITED Arwal Karpi Approved 14 101431 ADARSH KRITI FOUNDATION Arwal Karpi Approved 15 97792 KUSUM DEVI MAHILA SAMAJIK SEVA SANSTHAN Arwal Sonbhadra Banshi Approved Surypur 16 99176 COMPTECH TRAINING & TECH. PVT LTD Aurangabad Aurangabad Approved 17 97537 SAMAST MANAV JANKALYAN SANSTHAN Aurangabad Aurangabad Approved 18 95637 DATA PRO COMPUTERS PVT LTD Aurangabad Aurangabad Approved 19 95668 DATA PRO COMPUTERS PVT LTD Aurangabad Aurangabad Approved 20 96121 QUESS CORP LTD Aurangabad Aurangabad Approved 21 97428 PARMPARA FOUNDATION Aurangabad Aurangabad Approved 22 96169 MAHEYUGE EDUCATIONAL WELFARE SOC. Aurangabad Aurangabad Approved 23 99332 ZAKIRUDDIN GILANI MEMORIAL EDU. TRUST Aurangabad Aurangabad Approved 24 99334 ZAKIRUDDIN GILANI MEMORIAL EDU. TRUST Aurangabad Aurangabad Approved 25 100286 THITHOLI SAMAJIK EVAM SANSKRITIK DARPAN Aurangabad Aurangabad Approved 26 98128 Kriti Edify Pvt Ltd. Aurangabad Barun Approved 27 99872 NATIONAL RURAL DEVLOPMENT PROGRAM Aurangabad Barun Approved 28 101180 COMPTECH TRAINING & TECH. PVT LTD Aurangabad Daudnagar Approved 29 98262 Dharshan Institute of management & Pvt. -

Sheikhpura Nawadah-805 110 Pin-811 105
IINNDDIIAANN MMEEDDIICCAALL AASSSSOOCCIIAATTIIOONN::: BBIIHHAARR SSTTAATTEE BBRRAANNCCHH LLIIISSTT OOFF LLIIIFFEE MMEEMMBBEERRSS OOFF III... MM... AA... (((SSHHEEIIIKKHHPPUURRAA BBRRAANNCCHH))) SSHHEEIIKKHHPPUURRAA BBRRAANNCCHH 1. Dr. Rajendra Prasad Jaiswal 10. Dr. Ajit Ranjan Prasad BHR/3209/119/1/49049/95-96/L 11. Dr. (Mrs.) Shyama Roy Dr. Shakuntala Memorial Hospital BHR/3217/119/9/49057/95-96/CL Girhinda ‘Shashi Niwas’ Dist. Sheikhpura Nawadah-805 110 Pin-811 105 2. Dr. Ram Chandra Mahto 12. Dr. Shivendra Kumar Singh BHR/3210/119/2/49050/95-96/L BHR/3218/119/10/49058/95-96/L Deputy Superintendent Prof. Colony, Station Road Sub-divisional Hospital Sheikhpura-811 105 Sheikhpura-811 105 3. Dr. Ramashray Prasad Singh 13. Dr. Nityanand Kumar Singh BHR/3211/119/3/49051/95-96/L BHR/3219/119/11/49059/95-96/L Chandani Chowk Medical Officer Incharge Sheikhpura-811 105 At & P. O. – Ariari Dist. Sheikhpura 4. Dr. Mrigendra Prasad Singh 14. Dr. Arjun Prasad BHR/3212/119/4/49052/95-96/L BHR/3220/119/12/49060/95-96/L Nibha Nursing Home Girhinda Sheikhpura-811 105 Dist. Sheikhpura Pin-811 105 5. Dr. Jai Ram Pandit 15. Dr. Sunayana Kumari BHR/3213/119/5/49053/95-96/L BHR/3221/119/13/49061/95-96/L Girhinda At-Badshahpur Sheikhpura-811 105 P. O. – Mandaha-811 105 Dist. Sheikhpura 6. Dr. Deo Nandan Prasad 16. Dr. Sri Niwas Sharma BHR/3214/119/6/49054/95-96/L BHR/3498/119/14/57275/96-97/L Khandpar At & P. O. – Shekhopur, Sarai Sheikhpura-811 105 Dist. Sheikhpura 7. Dr. Arif Abdullah 17. -
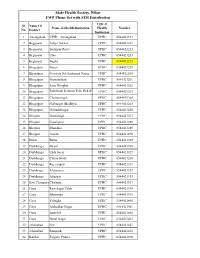
UPHC Contacts
State Health Society, Bihar FWP Phone Set with SIM Distribution Type of Sl. Name Of Name of Health Institution Health Number No. District Institution 1 Aurangabad UPHC Aurangabad UPHC 8544421183 2 Begusarai Teliya Pokhar UPHC 8544421231 3 Begusarai Bishnpur Purvi UPHC 8544421232 4 Begusarai Ulao UPHC 8544421233 5 Begusarai Bagha UPHC 8544421235 6 Bhagalpur Barari UPHC 8544421259 7 Bhagalpur Nayatola Sacchidanand Nagar UPHC 8544421260 8 Bhagalpur Hussainabad UPHC 8544421261 9 Bhagalpur Sarai Kilaghat UPHC 8544421262 10 Bhagalpur Sahebganj Harizon Tola, Rekab UPHC 8544421263 Ganj 11 Bhagalpur Champanagar UPHC 8544421264 12 Bhagalpur Nathnagar (Budhiya) UPHC 8544421265 13 Bhagalpur Mohaddinagar UPHC 8544421266 14 Bhojpur Maulabagh UPHC 8544421287 15 Bhojpur Gaushganj UPHC 8544421288 16 Bhojpur Dharahra UPHC 8544421289 17 Bhojpur Anaith UPHC 8544421290 18 Buxar Buxar UPHC 8544421305 19 Darbhanga Biraul UPHC 8544421328 20 Darbhanga Urdu bazar UPHC 8544421329 21 Darbhanga Chuna bhatti UPHC 8544421330 22 Darbhanga Raj campus UPHC 8544421331 23 Darbhanga Khajasarai UPHC 8544421332 24 Darbhanga Alinagar UPHC 8544421333 25 East ChamparanChatauni UPHC 8544421367 26 Gaya Ram Sagar Talab UPHC 8544421398 27 Gaya Bhusunda UPHC 8544421399 28 Gaya Telbigha UPHC 8544421400 29 Gaya Ambedkar Nagar UPHC 8544421401 30 Gaya katarihill UPHC 8544421402 31 Gaya Ekbal Nagar UPHC 8544421403 32 Jehanabad Erki UPHC 8544421451 33 Jehanabad Ramgarh UPHC 8544421452 34 Katihar Tajganj, Phasia UPHC 8544421490 Type of Sl. Name Of Name of Health Institution Health Number -
Begusarai Introduction
DISTRICT PROFILE BEGUSARAI INTRODUCTION Begusarai district is one of the thirty-eight administrative districts of Bihar. Begusarai was notified as a district in 1972 and falls in Darbhanga division. It is a part of the historic Mithila region. The rivers flowing through Begusarai district are Ganga, Burhi Gandak, Balan, Bainty, Baya and Chandrabhaga. The name Begusarai originates from the words ‘Begum sarai’ meaning ‘queen’s inn’. The place was so called because the Begum of Bhagalpur used to visit "Simaria Ghat"-a holy place on the northern banks of river Ganga , for pilgrimage. HISTORICAL BACKGROUND Begusarai was a sub-division of the erstwhile Munger district from 1870 to 1972. Begusarai was called ‘Anguttarapa’ in Buddhist literature Majjhim Nikaya. There is evidence of continued habitation in Begusarai since the Mauryan period. Jaimangalgarh and Naulagarh in Begusarai was an important centre of administration , art and culture during the Mauryan and Pala period. Archaeological explorations have revealed that Jaimangalgarh was an important Buddhist center. ADMINISTRATIVE Begusarai town is a municipal corporation town and district headquarters of Begusarai district. Begusarai district comprises of 5 sub-divisions, namely Begusarai, Manjhaul, Ballia, Bakhari and Teghara which is divided into 18 municipal blocks. o Begusarai o Bhagwanpur o Mansurchak o Manjahaul o Balia o Birpur o Teghra o Sahibpur Kamal o Dandari o Samho o Cheria Bariarpur o Nawkothi o Bachhwara o Khudabandpur o Garhpura o Barauni o Bakhari o Chhaurahi Total no. of Panchayats in Begusarai district: 257. Total no. of villages in Begusarai district: 1229. ECONOMIC PROFILE Agriculture is the mainstay of the economy. The main cash crops of Begusarai district are oilseeds, aniseed/ tisi, tobacco, jute, potato, red chillies, tomato and rape-seed. -

Saran, Vaishali, Samastipur, Begusarai and Patna Districts, Bihar
क� द्र�यू�म भ जल बोड셍 जल संसाधन, नद� �वकास और गंगा संर�ण मंत्रालय भारत सरकार Central Ground Water Board Ministry of Water Resources, River Development and Ganga Rejuvenation Government of India Report on AQUIFER MAPPING Parts of Saran, Vaishali, Samastipur, Begusarai and Patna Districts, Bihar म鵍य पूव� �ेत्र, पटना Mid-eastern Region, Patna Report on Aquifer Mapping in parts of Saran, Vaishali, Samastipur, Begusarai and Patna distrcits, Bihar (NAQUIM_Phase-II) कᴂ द्रीय भमू मजऱ बो셍ड जऱ संसाधन, नदी विकास और गंगा संरक्षण मंत्राऱय, भारत सरकार म鵍य ऩिू ी क्षेत्र , ऩटना CENTRAL GROUND WATER BOARD MINISTRY OF WATER RESOURCES, RIVER DEVELOPMENT & GANGA REJUVENATION GOVERNMENT OF INDIA MID EASTERN REGION, PATNA July 2016 i Report on Aquifer Mapping in parts of Saran, Vaishali, Samastipur, Begusarai and Patna distrcits, Bihar (NAQUIM_Phase-II) Principal Contributors Hydrogeologist Geophysist Sh. S .N. Dwivedi, Scientist C Dr. S.K.Adhikari, Scientist B (Nodal Officer) Dr. Rakesh Singh, Scientist B Sh. P. Raghavender, Sr.Tech. Astt. Sh. C.K.Gogoi, Scientist B Dr. Fakhre Alam, Sr.Tech. Astt. Chemist Sh. Suresh Kumar, Asst. Chemist Sushri. Supriya Singh, Sr.Tech. Astt. ii Report on Aquifer Mapping in parts of Saran, Vaishali, Samastipur, Begusarai and Patna distrcits, Bihar (NAQUIM_Phase-II) CONTENTS PAGE NO. List of Figures v List of Tables vi List of Annexures vii List of Block viii CHAPTER 1 INTRODUCTION 1-15 1.1 Objective and Scope 1-2 1.2 Approach and Methodology 2 1.3 Area Details 2-4 1.4 Brief Description 4 1.4.1 Data availability 4 1.4.2 Data -

Brief Industrial Profile of BEGUSARAI District
BEGUSARAI- DISTRICT INDUSTRIAL POTENTIAL SURVEY Contents S. No. Topic Page No. 1. General Characteristics of the District 3 1.1 Location & Geographical Area 4 1.2 Topography 5-6 1.3 Availability of Minerals. 7 1.4 Forest 7 1.5 Administrative set up 8 2. District at a glance 9-16 2.1 Existing Status of Industrial Area in the District –BEGUSARAI 16 3. Industrial Scenario Of BEGUSARAI 17 3.1 Industry at a Glance 17 3.2 Year Wise Trend Of Units Registered 17 3.3 Details Of Existing Micro & Small Enterprises & Artisan Units In 18 The District 3.4 Large Scale Industries / Public Sector undertakings 19 3.5 Major Exportable Item 19 3.6 Growth Trend 19 3.7 Vendorisation / Ancillarisation of the Industry 19 3.8 Medium Scale Enterprises 20 3.8.1 List of the units in ------ & near by Area 20 3.8.2 Major Exportable Item 20 3.9 Service Enterprises 20 3.9.1 Potentials areas for service industry 20 3.10 Potential for new MSMEs 20 4. Existing Clusters of Micro & Small Enterprise 20 4.1 Detail Of Major Clusters 20 4.1.1 Manufacturing Sector 20 4.1.2 Service Sector 20 4.2 Details of Identified cluster 21 4.2.1 Extraction of oil from aromatic plant cluster, Begusarai 21 4.2.2 General Engineering cluster, Barauni 22 4.2.3 4.2.4 4.2. 5 5. General issues raised by industry association during the course of 23 meeting 6 Steps to set up MSMEs 24 Page 2 of 25 BEGUSARAI- DISTRICT INDUSTRIAL POTENTIAL SURVEY Brief Industrial Profile of BEGUSARAI District 1.