Malnutrition Disease
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Title Steatitis and Vitamin E Deficiency in Captive Olive Ridley Turtles
Steatitis and Vitamin E deficiency in captive olive ridley turtles Title (Lepidochelys olivacea) MANAWATTHANA, SONTAYA; KASORNDORKBUA, Author(s) CHAIYAN Proceedings of the 2nd International symposium on Citation SEASTAR2000 and Asian Bio-logging Science (The 6th SEASTAR2000 Workshop) (2005): 85-87 Issue Date 2005 URL http://hdl.handle.net/2433/44090 Right Type Conference Paper Textversion publisher Kyoto University Steatitis and Vitamin E deficiency in captive olive ridley turtles (Lepidochelys olivacea) SONTAYA MANAWATTHANA1 and CHAIYAN KASORNDORKBUA2 1Phuket Marine Biological Center, 51 Sakdidach Rd. Phuket 83000, Thailand. E-mail: [email protected] 2 Veterinary Diagnostic Laboratory, Department of Veterinary Pathology, Faculty of Veterinary Medicine, Kasetsart University, Chatuchak, Bangkok 10903, Thailand. E-mail: [email protected] ABSTRACT Steatitis, which is caused by vitamin E deficiency, was observed in 3 captive Olive Ridley turtles (Lepidochelys olivacea) at Phuket Marine Biological Center, Phuket Province, Thailand during March to August 2005. Clinical findings had only shown depression and emaciation. Necropsy had revealed firm yellowish-brown masses distributed in fat tissues throughout the body. The predisposing cause of the disease is considered to be resulting from feeding these turtles mainly with frozen fish for more than 20 years, which can lead to vitamin E deficiency. Since there has been no effective treatment for chronic vitamin E deficiency, changes of the feeding from frozen fish to fresh fish and vitamin E supplementation of 100 IU/kg of fish fed have been recommended as a preventive treatment for the rest of the sea turtles in the center. KEYWORDS: olive ridley turtle, Lepidochelys olivacea, steatitis, vitamin E INTRODUCTION membranes, by preventing lipid peroxidation of Numerous scientific evidence indicates that reactive unsaturated fatty acids i.e. -

Kwashiokorl. Description of Kwashiorkor Kwashiorkor Is a Life-Threatening and Debilitating Form of Malnutrition. It's Caused B
Name ;OLAWUYI MUQTADIR OREDOLAPO COUSE AFE 101 DEPARTMENT ;ACCOUNTING KWASHIOKORl. Description of kwashiorkor kwashiorkor is a life-threatening and debilitating form of malnutrition. It’s caused by a lack of protein in your diet. Kwashiorkor is also commonly seen in low- and lower-middle-income regions facing famine. Signs and symptoms of kwashiorkor The symptoms of kwashiorkor include; • damaged immune system, which can lead to more frequent and severe infections • irritability. • flaky rash • shock. • change in skin and hair colour (to a rust colour) and texture • fatigue • diarrhea • loss of muscle mass • failure to grow or gain weight • edema (swelling) of the ankles, feet, and belly SUSCEPTIBLES If kwashiorkor is suspected, your doctor will first examine you to check for an enlarged liver (hepatomegaly) and swelling. Next, blood and urine tests may be ordered to measure the level of protein and sugar in your blood. Other tests may be performed on your blood and urine to measure signs of malnutrition and lack of protein. These tests may look for muscle breakdown and assess kidney function, overall health, and growth. These tests include: arterial blood gas, blood urea nitrogen , urinalysis e.t.c. TREATMENT Kwashiorkor can be corrected by eating more protein and more calories overall, especially if treatment is started early. You may first be given more calories in the form of carbohydrates, sugars, and fats. Once these calories provide energy, you will be given foods with proteins. Foods must be introduced and calories should be increased slowly because you have been without proper nutrition for a long period. Your body may need to adjust to the increased intake. -

Eating Disorders: About More Than Food
Eating Disorders: About More Than Food Has your urge to eat less or more food spiraled out of control? Are you overly concerned about your outward appearance? If so, you may have an eating disorder. National Institute of Mental Health What are eating disorders? Eating disorders are serious medical illnesses marked by severe disturbances to a person’s eating behaviors. Obsessions with food, body weight, and shape may be signs of an eating disorder. These disorders can affect a person’s physical and mental health; in some cases, they can be life-threatening. But eating disorders can be treated. Learning more about them can help you spot the warning signs and seek treatment early. Remember: Eating disorders are not a lifestyle choice. They are biologically-influenced medical illnesses. Who is at risk for eating disorders? Eating disorders can affect people of all ages, racial/ethnic backgrounds, body weights, and genders. Although eating disorders often appear during the teen years or young adulthood, they may also develop during childhood or later in life (40 years and older). Remember: People with eating disorders may appear healthy, yet be extremely ill. The exact cause of eating disorders is not fully understood, but research suggests a combination of genetic, biological, behavioral, psychological, and social factors can raise a person’s risk. What are the common types of eating disorders? Common eating disorders include anorexia nervosa, bulimia nervosa, and binge-eating disorder. If you or someone you know experiences the symptoms listed below, it could be a sign of an eating disorder—call a health provider right away for help. -

341 Nutrient Deficiency Or Disease Definition/Cut-Off Value
10/2019 341 Nutrient Deficiency or Disease Definition/Cut-off Value Any currently treated or untreated nutrient deficiency or disease. These include, but are not limited to, Protein Energy Malnutrition, Scurvy, Rickets, Beriberi, Hypocalcemia, Osteomalacia, Vitamin K Deficiency, Pellagra, Xerophthalmia, and Iron Deficiency. Presence of condition diagnosed, documented, or reported by a physician or someone working under a physician’s orders, or as self-reported by applicant/participant/caregiver. See Clarification for more information about self-reporting a diagnosis. Participant Category and Priority Level Category Priority Pregnant Women 1 Breastfeeding Women 1 Non-Breastfeeding Women 6 Infants 1 Children 3 Justification Nutrient deficiencies or diseases can be the result of poor nutritional intake, chronic health conditions, acute health conditions, medications, altered nutrient metabolism, or a combination of these factors, and can impact the levels of both macronutrients and micronutrients in the body. They can lead to alterations in energy metabolism, immune function, cognitive function, bone formation, and/or muscle function, as well as growth and development if the deficiency is present during fetal development and early childhood. The Centers for Disease Control and Prevention (CDC) estimates that less than 10% of the United States population has nutrient deficiencies; however, nutrient deficiencies vary by age, gender, and/or race and ethnicity (1). For certain segments of the population, nutrient deficiencies may be as high as one third of the population (1). Intake patterns of individuals can lead to nutrient inadequacy or nutrient deficiencies among the general population. Intakes of nutrients that are routinely below the Dietary Reference Intakes (DRI) can lead to a decrease in how much of the nutrient is stored in the body and how much is available for biological functions. -

Severe Malnutrition: a Global Approach. INSTITUTION International Children's Centre, Paris (France)
, DOCUMENT RESUME ED 371 865 PS 022 466 AUTHOR Pelletier, Jean-Gerard TITLE Severe Malnutrition: A Global Approach. INSTITUTION International Children's Centre, Paris (France). REPORT NO ISSN-0379-2269 PUB DATE 93 NOTE 88p. AVAILABLE FROMChildren in the Tropics, International Children's Centre, Chateau de Longchamp, Bois de Boulogne, 75016, Paris, France ($10; annual subscription: $40 for 6 issues). PUB TYPE Collected Works Serials (022) JOURNAL CIT Children in the Tropics; n208-209 1993 EDRS PRICE MF01/PC04 Plus Postage. DESCRIPTORS Biological Influences; *Child Health; Children; Cultural Influences; Developing Nations; Disease Incidence; *Diseases; Foreign Countries; Global - Approach; *Hunger; *Intervention; Medical Services; *Nutrition; Nutrition Instruction; Poverty; Program Evaluation; Rehabilitation; Socioeconomic Influences IDENTIFIERS Anthropometry; KwashisKor; Marasmus; Psychological Influences ABSTRACT This report examines the immediate and underlying causes of malnutrition in the developing world. The first section discusses the effects of malnutrition on childhood development and examines the efficacy of nutritional rehabilitation. The second section addresses the medical effects of severe malnutrition, including the onset of ponderostatural (weight) retardation, behavioral disorders, dehydration, anemia, hypothermia, hypoglycemia. and diarrhea. The third section focuses on anthropometric approaches to treating malnourished children, which treat children on an individual basis based upon their particular condition. The fourth section examines the biological effects of severe malnutrition, discussing deficiencies in serum proteins, electrolytes, trace elements, and hormonal levels, along with their immunological consequences. The fifth section explains the nutritional approach to the problem, looking at protein, vitamin, and mineral deficiencies lnd specific rehabilitation procedures and foods. The sixth section focuses on a cultural approach to malnutrition, discussing dietary and social customs that affect nutrition and eating behaviors. -

Marasmus- 1985
Postgraduate Medical Journal (1985) 61, 915-923 Postgrad Med J: first published as 10.1136/pgmj.61.720.915 on 1 October 1985. Downloaded from Marasmus- 1985 D. Barltrop and B.K. Sandhu Department ofChild Health, Charing Cross and Westminster Medical School, London, UK. Introduction Dr Wilfred J. Pearson writing for the first volume of In 1959 Jelliffe coined the term protein-calorie this Journal in 1925 defined marasmus (Greek: maras- malnutrition (PCM) of early childhood to include mos, wasting) as 'a chronic state of malnutrition of a mild, moderate and various types of severe degrees of severe grade' but pointed out that 'we must retain the malnutrition. The advent of the International System conception ofcases varying in severity from those who of Units (SI) resulted in the introduction of the term simply show an insufficient gain or stationary weight protein energy malnutrition (PEM). The World with few systemic changes, to the most extreme form Health Organisation (WHO, 1973) defined PEM as which is merely the end result of repeated nutritional follows: 'A range of pathological conditions arising or constitutional disturbances.' He described oedema from coincidental lack, in varying proportions, of in some cases as a complication of marasmus. The protein and calories, occurring most frequently in clinical picture of the syndrome, later described as infants and young children and commonly associated kwashiorkor, was not generally recognized at this with infection'. This is not dissimilar from Wilfred time, although a number of authors had described it Pearson's view of marasmus. (Czerney & Keller, 1928). In order to treat and, more importantly, to prevent a In 1933 Cicely D. -

Involvement of the Eye in Protein Malnutrition * -303
Bull. Org. mond. Sante 1958, 19, 303-314 Bull. Wld Hith Org. INVOLVEMENT OF THE EYE IN PROTEIN MALNUTRITION * D. S. McLAREN, M.D., Ph.D., D.T.M. & H. Medical Research Officer, East African Institute for Medical Research, Mwanza, Tanganyika Formerly at the MRC Human Nutrition Research Unit, National Institute for Medical Research, London SYNOPSIS An extensive review of the literature on protein malnutrition, with special reference to the frequency of involvement of the eyes, has been made by the author. Consideration of accounts from all parts of the world and in many different languages, including early as well as more recent descriptions of the syndrome, indicates that this important complication has not received sufficient attention hitherto. The evidence available suggests that it is nearly always an accompanying deficiency of vitamin A that is responsible. Less commonly reported-and producing less severe effects-is deficiency of the B-complex vitamins, and there is no clear evidence to date that protein deficiency itself damages the eyes in these cases. The ways in which protein lack might interfere with various aspects of vitamin-A metabolism are discussed, but it is pointed out that their actual significance in human disease is not yet known. A low dietary intake of vitamin A is regarded by the author as being the prime factor in the causation of eye complications, and attention is drawn to the necessity to correct this as part of any prophylactic or therapeutic programme aimed primarily at combat- ing protein malnutrition. The syndrome known by such various names as kwashiorkor, nutritional oedema syndrome, sindrome pluricarencial, and many others (Trowell, Davies & Dean, 1954), and characterized chiefly by a dietary deficiency ofprotein, has been reported as occurring amongst most of the malnourished communities of the world. -
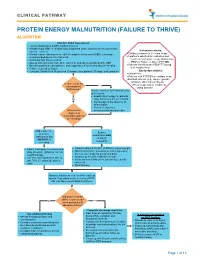
Protein Energy Malnutrition (Failure to Thrive) Algorithm
CLINICAL PATHWAY PROTEIN ENERGY MALNUTRITION (FAILURE TO THRIVE) ALGORITHM Conduct Initial Assessment • History and physical (H&P), nutrition focused • Weight height, BMI, % of ideal body weight and exam: assess severity (symmetric edema = severe) Inclusion criteria: • • Consider basic labs based on H&P; A complete blood count (CBC) is strongly Children newborn to 21 years of age • recommended due to risk of anemia Inpatients admitted for evaluation and • Additional labs based on H&P treatment of Protein Energy Malnutrition • Assess micronutrients: iron, zinc, vitamin D, and others as indicated by H&P (PEM) or Failure to thrive (FTT) OR • • Baseline potassium, phosphorus, and magnesium if concerned about re-feeding Patients identified with PEM/FTT during • Calorie count up to 3 days their hospital stay. • Consults: Social Work, Registered Dietician, Occupational Therapy, and Lactation Exclusion criteria: • Outpatients • Patients with FTT/PEM secondary to an identified concern (e.g., cancer, genetic condition, other chronic illness). Is there a risk for •Pts w/ suspected or confirmed micronutrient Yes eating disorder deficiencies? Initiate treatment for micronutrients deficiencies: • Empiric zinc therapy for patients No older than 6 months for 1 month • Iron therapy in the absence of inflammation • Vitamin D and other What are the micronutrients based on labs degrees of malnutrition and risk of refeeding? Mild, moderate, Severe or severe malnutrition AND malnutrition but at risk of NO RISK of refeeding refeeding • • Initiate feeding per recommended Initiate feeding at 30-50% of RDA for current weight • daily allowance (RDA) for current Monitor potassium, phosphorus, and magnesium weight and age once to twice a day for a total of 4 days • • Use PO route if patient is able to Advance by 10-20% if labs are normal • take 70% of estimated calories If labs abnormal hold off on advancing feed until orally corrected • Start thiamine Advance calories to meet level for catch up growth. -

Nutritional Dermatoses in the Hospitalized Patient
HOSPITAL CONSULT IN PARTNERSHIP WITH THE SOCIETY FOR DERMATOLOGY HOSPITALISTS Nutritional Dermatoses in the Hospitalized Patient Melissa Hoffman, MS; Robert G. Micheletti, MD; Bridget E. Shields, MD Nutritional deficiencies may arise from inadequate nutrient intake, abnormal nutrient absorption, or improper nutrient PRACTICE POINTS utilization.4 Unfortunately, no standardized algorithm for • Nutritional deficiencies are common in hospitalized screening and diagnosing patients with malnutrition exists, patients and often go unrecognized. making early physical examination findings of utmost • Awareness of the risk factors predisposing patients importance. Herein, we present a review of acquired nutri- to nutritional deficiencies and the cutaneous manifes- tional deficiency dermatoses in the inpatient setting. tations associated with undernutrition can promote copy early diagnosis. Protein-Energy Malnutrition • When investigating cutaneous findings, undernutri- tion should be considered in patients with chronic Protein-energy malnutrition (PEM) refers to a set of infections, malabsorptive states, psychiatric illness, related disorders that include marasmus, kwashiorkor and strict dietary practices, as well as in those using (KW), and marasmic KW. These conditions frequently are certain medications. seen in developing countries but also have been reported 5 • Prompt nutritional supplementation can prevent patient in developed nations. Marasmus occurs from a chronic morbidity and mortality and reverse skin disease. deficiencynot of protein and calories. Decreased insulin pro- duction and unopposed catabolism result in sarcopenia and loss of bone and subcutaneous fat.6 Affected patients include children who are less than 60% ideal body weight Cutaneous disease may be the first manifestation of an underlying nutri- 7 tional deficiency, highlighting the importance of early recognition by der- (IBW) without edema or hypoproteinemia. -

Nutritional Diseases of Fish in Aquaculture and Their Management: a Review
Acta Scientific Pharmaceutical Sciences (ISSN: 2581-5423) Volume 2 Issue 12 December 2018 Review Article Nutritional Diseases of Fish in Aquaculture and Their Management: A Review Shoaibe Hossain Talukder Shefat1* and Mohammed Abdul Karim2 1Department of Fisheries Management, Faculty of Graduate Studies, Bangabandhu Sheikh Mujibur Rahman Agricultural University, Gazipur, Bangladesh 2Department of Fish Health Management, Faculty of Postgraduate Studies, Sylhet Agricultural University, Bangladesh *Corresponding Author: Shoaibe Hossain Talukder Shefat, Postgraduate Researcher, Department of Fisheries Management, Faculty of Graduate Studies, Bangabandhu Sheikh Mujibur Rahman Agricultural University, Gazipur, Bangladesh. Received: September 26, 2018; Published: November 19, 2018 Abstract aquaculture production and health safety. Information were collected from different secondary sources and then arranged chrono- This review was conducted to investigate the significance, underlying causes and negative effects of nutritional diseases of fish on logically. Investigation reveals that, Aquaculture is the largest single animal food producing agricultural sector that is growing rapidly all over the world. Nutritional disease is one of most devastating threats to aquaculture production because it is very difficult to quality and quantity. Public health hazards are also in dangerous situation due to frequent disease outbreak and treatment involving identify nutritional diseases. Production cost get increased due to investment lost, fish mortality, -

INCIDENCE of UTRITIONAL DEFICIENCY DISEASES AMONG the BANTU and COLOURED Populanons in SOUTH AFRICA AS REFLECTED by the RESULTS of a QUESTIONNAIRE SURVEY*
504 S.A. MEDICAL JOUR AL 18 June 1966 N22 (Supplemenr-SlJIl1h African Jo//mal of Nurririun) INCIDENCE OF UTRITIONAL DEFICIENCY DISEASES AMONG THE BANTU AND COLOURED POPULAnONS IN SOUTH AFRICA AS REFLECTED BY THE RESULTS OF A QUESTIONNAIRE SURVEY* J. F. POTGIETER,** S. A. FELLINGHAM.t AND M. L. ESER** Although it is today generally conceded by nutritionists (vii) Crireria for rhe clillical diagllosis of the specific IIl11ri that malnutrition is a major problem in the Republic and rional diseases, and assumes serious proportions in the younger non-White (viii). Descripriolls of 1I01l-specific sigm alld symprol1ls. In formatIon under (vii) and (viii) was provided in order t age-groups, no reliable information is at present available facilitate the diagnosis of the various diseases and the recoo which gives a true picture of the extent of the problem nition of signs and symptoms referred to in the questionnair~. throughout the country. This information was considered necessary as, without it, the cnteria adopted by different practitioners and their evaluatior To obtain detailed and accurate information on the of the severity of the diseases might vary considerably. prevalence of nutritional disease in all areas of the coun In an accompanying letter, the doctors were asked to keer try, it would be necessary to conduct field surveys on records for a 4-week period during May/June and anotheI samples from all sections of the population-a large and during NovemberfDecember 1960. An additional copy of the unwieldy task. As it was thought that medical practitioners questionnaire was included for use during the latter period. -

Pediatric Malnutrition: Under- and Over-Weight in Children
Pediatric Malnutrition: Under- and Over-weight in Children Daniel Jackson, MD University of Utah School of Medicine 2012 Undernutrition: Global and Local Famine •Political Instability •Distribution of Resources •Social Chaos •Survival/Recovery Nutrient Deficiency Maternal-Child Dyad •Maternal Nutrition/Health •Intrauterine Onset •Nursing insufficiency •Weaning/transition Malabsorption •Environmental Factors •Infection: parasitosis •MalabsorptionÆreduced intake •InflammationÆincreased energy needs Kwashiorkor Displaced from nursing Low protein alternatives Endemic Infection GI protein loss HypoalbuminemiaÆEdema Marasmus Protein-Calorie Undernutrition Fat and Muscle depletion Preserved plasma proteins Preserved homeostasis Failure to Thrive: Our world Genetics Prenatal environment Behavioral factors Psychosocial context Disease factors To Thrive HomeostasisHomeostasis FullFull physiologicphysiologic functionfunction WeightWeight gaingain LinearLinear growthgrowth CranialCranial growthgrowth NeurodevelopmentNeurodevelopment SocialSocial integrationintegration Navigating The Growth Curve ExpectationsExpectations DeviationsDeviations RecoveryRecovery FalteringFaltering AcuteAcute wastingwasting ChronicChronic stuntingstunting CranialCranial stasisstasis CDC Growth Curves: 0-36 months CDC Growth Curves: 2-20 years Body Mass Index: kg/m2 Body Mass Index [BMI]: 2 years to 20 years BMI = weight (kg) / height2 (m2) Extremely Obese: BMI >99th %ile 95 Obese: BMI 95th to <99th %ile 90 85 Overweight: BMI 85th to <95th %ile 75 50 25 10