Vision Therapy: Beyond Compensations and Addressing the Root of the Problem + Objectives
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-
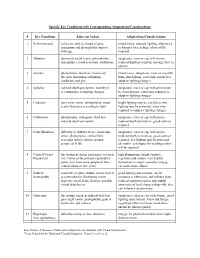
Specific Eye Conditions with Corresponding Adaptations/Considerations
Specific Eye Conditions with Corresponding Adaptations/Considerations # Eye Condition Effect on Vision Adaptations/Considerations 1 Achromotopsia colors are seen as shades of grey, tinted lenses, reduced lighting, alternative nystagmus and photophobia improve techniques for teaching colors will be with age required 2 Albinism decreased visual acuity, photophobia, sunglasses, visor or cap with a brim, nystagmus, central scotomas, strabismus reduced depth perception, moving close to objects 3 Aniridia photophobia, field loss, vision may tinted lenses, sunglasses, visor or cap with fluctuate depending on lighting brim, dim lighting, extra time required to conditions and glare adapt to lighting changes 4 Aphakia reduced depth perception, inability to sunglasses, visor or cap with a brim may accommodate to lighting changes be worn indoors, extra time required to adapt to lighting changes 5 Cataracts poor color vision, photophobia, visual bright lighting may be a problem, low acuity fluctuates according to light lighting may be preferred, extra time required to adapt to lighting changes 6 Colobomas photophobia, nystagmus, field loss, sunglasses, visor or cap with a brim, reduced depth perception reduced depth perception, good contrast required 7 Color Blindness difficulty or inability to see colors and sunglasses, visor or cap with a brim, detail, photophobia, central field reduced depth perception, good contrast scotomas (spotty vision), normal required, low lighting may be preferred, peripheral fields alternative techniques for teaching colors -

Vision Therapy and Post-Concussion Syndrome Management: a Case Report Elizabeth Murray OD, Katie Connolly OD
Vision Therapy and Post-Concussion Syndrome Management: A Case Report Elizabeth Murray OD, Katie Connolly OD Abstract: Current therapy for post-concussion syndrome with visual symptoms are to rest and decrease visual demand. This case looks at vision therapy for first line treatment when decreasing visual demand is not ideal. I. Case History On 5/30/2017, a 37 year old white male presented for persistent visual symptoms following a traumatic brain injury to the occipital lobe with torsion on the brain stem. The injury occurred on 4/3/2017 from a motor vehicle accident, and he had since been cleared from cognitive rest. At the time of the accident, he reported no loss of consciousness but did have post traumatic amnesia. Initially, he reported feeling fine, but his symptoms progressively worsened. He denied blur and diplopia, but was symptomatic for significant cognitive fatigue, gaze instability, visual stimuli triggered headaches, photophobia, and noise sensitivity. He is a pediatric oncologist with significant visual and cognitive demanding duties that exacerbate his symptoms. Ocular and medical history were unremarkable prior to the accident. At the time, he was taking Fioricet and Amitriptyline as directed for headaches and to aid in sleep, respectively. He had been seeing a Chiropractor for vestibular therapy that included some oculomotor therapy and planned to begin cognitive therapy at an outpatient rehabilitation hospital. II. Pertinent findings Entering distance visual acuities were 20/20 OD, OS and OU and near visual acuities were 20/20 OD, 20/25-1 OS, and 20/15-1 OU, without correction. Pupils and extraocular muscles were unremarkable. -

Plan Q Full Benefit Description
B E N E F I T D E S C R I P T I O N State Employee Health Plan This booklet describes the health benefits that the Kansas State Employees Health Care Commission provides to Members and their Dependents. These benefits are funded by: The Kansas State Employees Health Care Commission Third Party Administrator (TPA): : Blue Cross Blue Shield of Kansas has been retained to administer claims under this Plan. The TPA provides Administrative Services Only pursuant to this Benefit Description, including claims processing and administration of appeals and grievances. For answers to questions regarding eligibility for benefits, payment of claims, and other information about this Plan contact: Blue Cross Blue Shield of Kansas 1133 SW Topeka Blvd Topeka, KS 66629 By Phone 785-291-4185 or Toll Free at 1-800-332-0307 www.bcbsks.com/state Company is not the insurer under this Program and does not assume any financial risk or obligation with respect to claims. Plan Q Benefit Description 2021 Section I Coverage ................................................................................................. 1 Part 1: General Provisions ................................................................................ 1 Responsibilities of the Third Party Administrator (TPA) ..................................... 1 Case Management/Cost Effective Care ............................................................ 1 How to Contact the TPA .................................................................................... 2 Services from Non Network Providers -

Year in Review Issue
Gregg’s LANDING The exclusiveG newsletter for the residentsLife of Gregg’s Landing January 2021 2020 YEAR IN REVIEW ISSUE YOUR STORIES. YOUR PHOTOS. YOUR COMMUNITY. New Year (finally), New You ! LEAVE IT TO TOPTEC $500 OFF! WE'LL TAKE CARE OF IT. YEAR END SPECIAL $85.00 BRACES Furnace Tune-up INVISALIGN Special *12/1/2020 - 1/31/2021 COMPREHENSIVE TREATMENT ONLY **COUPON MUST BE PRESENT Don't pay until 2021 when you nance a new Lennox* YOUR SPECIALIST FOR: systemfor as little as $132 a month. Early Treatment • Adult Treatment Plus get up to $1,200 in rebates. Ronald S. Jacobson Raymond Y. Tsou No contact service call policy – Techs. D.D.S., M.S. D.M.D., M.S. Diamond Plus Provider wears face masks, gloves & booties IL. Lic. #055-042909 Visit us Online Vernon Hills Office: Chicago Office: 280 W. Townline Rd. 4200 W. Peterson Ave. JTORTHO.COM Suite 220 Suite 116 Vernon Hills, IL 60061 Chicago, IL 60646 Visit our Doctors at our Vernon Hills or Chicago Location 847-816-0633 773-545-5333 2 Gregg's Landing Life • January 2021 January 2021 • Gregg's Landing Life 3 847-780-8200 You can purchase sessions, membership plans and gift cards... please call or Visit our Facebook page or website for promotions. Northshoresalt.com CONDITIONS BENEFITS • Asthma • Clear Pollens, Pollutants, Toxins & Airways • Cough • Reduce Bronchial Inflammation • Sinusitis • Relieve Skin Conditions such as Dermatitis, • COPD Eczema, & Psoriasis • Bronchitis • Improve Lung Function • Stress • Strengthen the Immune System against • Ear Infection Cold, Flu, & Lung Irritants • Allergies • Reduce Triggers that Promote Respiratory Illness • Eczema • Clean Nasal Cavities and Sinuses • Psoriasis • Cystic Fibrosis WE SELL 1282 Old Skokie Rd. -

Amblyopia: Can Laser Acupuncture Be an Option?
JAMS272_proof ■ 1 March 2016 ■ 1/8 + MODEL J Acupunct Meridian Stud 2016;--(-):--e-- Available online at www.sciencedirect.com 61 62 1 63 2 Journal of Acupuncture and Meridian Studies 64 3 65 4 66 5 journal homepage: www.jams-kpi.com 67 6 68 7 69 8 70 9 CLINICAL CASE REPORT 71 10 72 11 73 12 74 13 75 14 76 15 Amblyopia: Can Laser Acupuncture be an 77 16 78 17 Option? 79 18 80 19 Q27 Q1 81 20 Marzio Vanzini, Michele Gallamini* 82 21 83 22 Available online --- 84 23 85 24 86 25 Received: Nov 20, 2015 Abstract 87 26 Revised: Jan 11, 2016 This paper describes the results of the treatment of amblyopia in young patients using an 88 27 Accepted: Jan 13, 2016 unconventional laser-acupuncture technique. After obtaining satisfactory results in the 89 28 treatment of a 14-year-old amblyopic girl, the treatment was applied to 13 amblyopic 90 29 children aged 3e11 years, with an encouraging outcome. An ultralow-light-intensity laser KEYWORDS 91 30 with a square-wave modulated emission was applied over a sequence of acupuncture acupuncture; 92 31 points. Each session lasted <15 minutes, and the treatment was performed once a week amblyopia; 93 32 in 6-week cycles. Patients were followed for several years to evaluate the long-term re- laser acupuncture; 94 33 lazy eye; sults and/or to extend the treatment. All except two of the treated patients showed a 95 34 ultralow-light-intensity rapid increase in visual acuity after several treatment sessions. -

The Persistence of Fad Interventions in the Face of Negative Scientific Evidence: Facilitated Communication for Autism As a Case Example
Evidence-Based Communication Assessment and Intervention ISSN: 1748-9539 (Print) 1748-9547 (Online) Journal homepage: http://www.tandfonline.com/loi/tebc20 The persistence of fad interventions in the face of negative scientific evidence: Facilitated communication for autism as a case example Scott O. Lilienfeld, Julia Marshall, James T. Todd & Howard C. Shane To cite this article: Scott O. Lilienfeld, Julia Marshall, James T. Todd & Howard C. Shane (2014) The persistence of fad interventions in the face of negative scientific evidence: Facilitated communication for autism as a case example, Evidence-Based Communication Assessment and Intervention, 8:2, 62-101, DOI: 10.1080/17489539.2014.976332 To link to this article: http://dx.doi.org/10.1080/17489539.2014.976332 Published online: 02 Feb 2015. Submit your article to this journal Article views: 5252 View related articles View Crossmark data Citing articles: 1 View citing articles Full Terms & Conditions of access and use can be found at http://www.tandfonline.com/action/journalInformation?journalCode=tebc20 Download by: [University of Lethbridge] Date: 05 October 2015, At: 05:52 Evidence-Based Communication Assessment and Intervention, 2014 Vol. 8, No. 2, 62–101, http://dx.doi.org/10.1080/17489539.2014.976332 EBP Advancement Corner The persistence of fad interventions in the face of negative scientific evidence: Facilitated communication for autism as a case example Scott O. Lilienfeld1, Julia Marshall1, James T. Todd2 & Howard C. Shane3 1Department of Psychology, Emory University, Atlanta, GA, USA, 2Department of Psychology, Eastern Michigan University, Ypsilanti, MI, USA, 3Boston Children’s Hospital, Boston, MA, USA ................................................................................................................................................. Abstract Communication disorder and mental health professionals may assume that once novel clinical techniques have been refuted by research, they will be promptly abandoned. -

Vision Therapy
bmchp.org | 888-566-0008 wellsense.org | 877-957-1300 Medical Policy Vision Therapy Policy Number: OCA 3.40 Version Number: 20 Version Effective Date: 06/01/21 + Product Applicability All Plan Products Well Sense Health Plan Boston Medical Center HealthNet Plan Well Sense Health Plan MassHealth ACO MassHealth MCO Qualified Health Plans/ConnectorCare/Employer Choice Direct Senior Care Options ◊ Notes: + Disclaimer and audit information is located at the end of this document. ◊ The guidelines included in this Plan policy are applicable to members enrolled in Senior Care Options only if there are no criteria established for the specified service in a Centers for Medicare & Medicaid Services (CMS) national coverage determination (NCD) or local coverage determination (LCD) on the date of the prior authorization request. Review the member’s product-specific benefit documents at www.SeniorsGetMore.org to determine coverage guidelines for Senior Care Options. Policy Summary The Plan considers vision therapy as a standard treatment option for certain conditions medically necessary when medical criteria are met. Prior authorization is required. It will be determined during the Plan’s prior authorization process if the service is considered medically necessary for the requested use. The Plan’s Medically Necessary medical policy, policy number OCA 3.14, specifies the product- specific definitions of medically necessary treatment, and the Plan’s Experimental and Investigational Treatment medical policy, policy number OCA 3.12, indicates the product-specific definitions of experimental or investigational treatment. Review the member’s applicable benefit documents rather Vision Therapy + Plan refers to Boston Medical Center Health Plan, Inc. and its affiliates and subsidiaries offering health coverage plans to enrolled members. -

Vision Problems in TBI: Impacts on Cognition & Attention
Vision Problems in TBI: Impacts on Cognition & Attention David H. Biberdorf, OD, FCOVD [email protected] www.valleyvision.net www.advancedneurovision.com Affiliations • Diplomate, American Board of Optometry (DABO) • Fellow, College of Optometry in Vision Development (FCOVD) • Member, Neuro-Optometric Rehabilitation Association (NORA) • Certified Brain Injury Specialist (CBIS) • Board Member, North Dakota Brain Injury Advisory Council • Board Member, International Sports Vision Association (ISVA) • Partner, Valley Vision Clinic, Ltd. Grand Forks, ND • Clinical director, Advanced Neuro-Vision Systems, LLC., Grand Forks & Fargo, ND. • Adjunct faculty, UND Dept. of Psychology, Grand Forks, ND. Disclaimers/Disclosures • Consultant, RightEye (Bethesda, MD) mTBI/TBI eye tracking metrics and App development • Consultant, Diopsys (Pine Brook, NJ) VEP biomarker algorithm for mTBI • Consultant, A.M.P. Systems (St. Louis, MO) concussion protocols. • Consultant, EyeNext (Turin, Italy) visual aspects of dyslexia/mTBI. 80-90% Why Vision? • 80-90% of all information entering the brain is visual • Over 50% of brain is involved in visual processing (over 30 brain regions and 8 cranial nerves) • Visual processing alone consumes 45% of brain’s energy • 90% of all concussions will have 1 or more ocular problems • Hidden vision problems frequently persist 6-9 months after a concussion • Vision problems can undermine the efficacy of other therapies and affect workplace productivity TBI Vision Problems: Visual Impairment vs. Visual Dysfunction • Visual Impairment: Visual acuity is decreased and/or the visual field is constricted; More common in moderate or severe TBI; More obvious and therefore easier to diagnose; Tends to be more “focal”; Relatively more “permanent”. Patient is rarely unaware of it. • Visual Dysfunction: Any disorder of afferent or efferent function. -

Two Eyes See More Than One Human Beings Have Two Eyes Located About 6 Cm (About 2.4 In.) Apart
ivi act ty 2 TTwowo EyesEyes SeeSee MoreMore ThanThan OneOne OBJECTIVES 1 straw 1 card, index (cut in half widthwise) Students discover how having two eyes helps us see in three dimensions and 3 pennies* increases our field of vision. 1 ruler, metric* The students For the class discover that each eye sees objects from a 1 roll string slightly different viewpoint to give us depth 1 roll tape, masking perception 1 pair scissors* observe that depth perception decreases *provided by the teacher with the use of just one eye measure their field of vision observe that their field of vision decreases PREPARATION with the use of just one eye Session I 1 Make a copy of Activity Sheet 2, Part A, for each student. SCHEDULE 2 Each team of two will need a metric ruler, Session I About 30 minutes three paper cups, and three pennies. Session II About 40 minutes Students will either close or cover their eyes, or you may use blindfolds. (Students should use their own blindfold—a bandanna or long strip VOCABULARY of cloth brought from home and stored in their science journals for use—in this depth perception and other activities.) field of vision peripheral vision Session II 1 Make a copy of Activity Sheet 2, Part B, for each student. MATERIALS 2 For each team, cut a length of string 50 cm (about 20 in.) long. Cut enough index For each student cards in half (widthwise) to give each team 1 Activity Sheet 2, Parts A and B half a card. Snip the corners of the cards to eliminate sharp edges. -

Binocular Vision
BINOCULAR VISION Rahul Bhola, MD Pediatric Ophthalmology Fellow The University of Iowa Department of Ophthalmology & Visual Sciences posted Jan. 18, 2006, updated Jan. 23, 2006 Binocular vision is one of the hallmarks of the human race that has bestowed on it the supremacy in the hierarchy of the animal kingdom. It is an asset with normal alignment of the two eyes, but becomes a liability when the alignment is lost. Binocular Single Vision may be defined as the state of simultaneous vision, which is achieved by the coordinated use of both eyes, so that separate and slightly dissimilar images arising in each eye are appreciated as a single image by the process of fusion. Thus binocular vision implies fusion, the blending of sight from the two eyes to form a single percept. Binocular Single Vision can be: 1. Normal – Binocular Single vision can be classified as normal when it is bifoveal and there is no manifest deviation. 2. Anomalous - Binocular Single vision is anomalous when the images of the fixated object are projected from the fovea of one eye and an extrafoveal area of the other eye i.e. when the visual direction of the retinal elements has changed. A small manifest strabismus is therefore always present in anomalous Binocular Single vision. Normal Binocular Single vision requires: 1. Clear Visual Axis leading to a reasonably clear vision in both eyes 2. The ability of the retino-cortical elements to function in association with each other to promote the fusion of two slightly dissimilar images i.e. Sensory fusion. 3. The precise co-ordination of the two eyes for all direction of gazes, so that corresponding retino-cortical element are placed in a position to deal with two images i.e. -

Collaborative Treatment for Vision After TBI
Collaborative Treatment for Vision After TBI Tom Wilson, OD, COVD Terri Cassidy, OTR, CDRS Vision is Primary • Human vision is a complex process that involves the coordinated efforts of both the eyes and the brain. • We use central vision (focal) to see detail. • We use peripheral vision (ambient) to inform us of movement or a direction we should point our eyes. • Even if we feel like our eyes (and brain) are not giving us accurate information – we believe our eyes. 2 Case Study 1 56 y/o woman involved in a motor vehicle crash. She was able to walk and talk. MRI was negative. Not long after she notices symptoms of not being able to read correctly, headaches, motion sickness is much worse than normal, she can’t go back to work on the computer, she is very tentative about driving. Her eye doctor tells her that her eyes are fine, it must be her medications. Finally she is referred to Dr. Wilson who does an evaluation and refers her to vision rehab with OT. Presentation Title – Date (month #, ####) 3 Evaluation Neuro-optometric Assessment • Eye health • Binocular Vision • Prism evaluation • Function Occupational Therapy Vision Assessment • Goal of OT is to improve the client’s level of performance in a needed ADL. • Deficiencies in visual processing are significant to the OT Process if they interfere with occupational performance – doing the tasks that she wants and needs to do. Presentation Title – Date (month #, ####) 4 Evaluation Results OD Finds: OT Finds: Characteristics of Post Trauma Pt is not able to work more than 2 Vision Syndrome -

Health Care Flexible Spending Account Expense Eligibility List
Health Care Flexible Spending Account Expense Eligibility List The health care FSA expense eligibility list will help you identify specific services, products and medications that are eligible for reimbursement under your health care flexible spending account (HC FSA) or your limited health care flexible spending account (if you have an HSA, your participation in the health care FSA is limited to out-of-pocket dental and vision expenses). You can use the list to search for the expense you have a question about, and it will show you if that expense is covered under the HC FSA and/or the limited HC FSA. It will also show you whether you need to submit a Letter of Medical Necessity and/or a doctor’s prescription for the expense to be reimbursed. Although not every expense is listed here, there are over 500 services, products, and medications that serve as a guide to eligible expenses. As additional information is available, this summary list will be updated, but the information is general and may be changed or updated without notice. Expenses are determined to be eligible for FSA reimbursement depending on the TriNet plan document, which must comply with Internal Revenue Code rulings. If a difference occurs between this list and either TriNet’s plan document or an Internal Revenue Code ruling, TriNet’s plan document, in compliance with the Internal Revenue Code, will govern. As FSA regulations are constantly changing, this summary does not guarantee reimbursement, but can be used as a guideline for submitting claims. If you have specific questions, you may call the TriNet Solution Center at 800.638.0461, Monday through Friday, 4:30 a.m.- 9 p.m.