Thoracoscopy: Assessment of a Physician Service and Comparison of a Flexible Bronchoscope Used As a Thoracoscope Wi-Th a Rigid Thoracoscope
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

The Point of the Needle. Occult Pneumothorax: a Review P Gilligan, D Hegarty, T B Hassan
293 CASE REPORTS Emerg Med J: first published as 10.1136/emj.20.3.296 on 1 May 2003. Downloaded from The point of the needle. Occult pneumothorax: a review P Gilligan, D Hegarty, T B Hassan ............................................................................................................................. Emerg Med J 2003;20:293–296 maximal resonance, which was the left sixth intercostal space The case of a patient with an unusual medical condition in the anterior axillary line. Some 300 ml of air was aspirated and an occult pneumothorax is presented. The evidence from the left hemithorax and the patient clinically improved. for management of occult pneumothorax particularly in The chest radiograph revealed bilateral infiltrates and under- patients with underlying lung disease is reviewed and solu- lying cystic and bullous disease but failed to reveal evidence of tions to the acute clinical problems that may arise are a pneumothorax (fig 1). A chest radiograph performed after suggested. the needle decompression also failed to show a pneumotho- rax. Computed tomography (CT) of the thorax revealed an anterior pneumothorax (fig 2). This was drained under CT guidance by the placement of a chest drain catheter. 27 year old man with histiocytosis X presented to the During the patient’s in hospital stay his chest drain was emergency department with left posterior chest wall removed as his chest radiograph showed no evidence of Apain and marked dyspnoea. The patient previously had residual pneumothorax. The patient became markedly dysp- recurrent pneumothoraces, eight on the right and two on the noeic within 24 hours. Because of the clinical impression of left. He had undergone pleurodesis of the right lung. -

Thoracoscopy for Spontaneous Pneumothorax
Journal of Clinical Medicine Review Thoracoscopy for Spontaneous Pneumothorax José M. Porcel 1,2,3,* and Pyng Lee 4 1 Pleural Medicine Unit, Department of Internal Medicine, Hospital Universitari Arnau de Vilanova, 25198 Lleida, Spain 2 Institut de Recerca Biomèdica de Lleida Fundació Dr. Pifarré, IRBLleida, 25198 Lleida, Spain 3 School of Medicine, Universitat de Lleida, 25008 Lleida, Spain 4 Division of Respiratory and Critical Care Medicine, The National University Hospital, Singapore 119228, Singapore; [email protected] * Correspondence: [email protected] Abstract: Video-assisted thoracic surgery (VATS) is the treatment of choice for recurrence preven- tion in patients with spontaneous pneumothorax (SP). Although the optimal surgical technique is uncertain, bullous resection using staplers in combination with mechanical pleurodesis, chemical pleurodesis and/or staple line coverage is usually undertaken. Currently, patient satisfaction, post- operative pain and other perioperative parameters have significantly improved with advancements in thoracoscopic technology, which include uniportal, needlescopic and nonintubated VATS variants. Ipsilateral recurrences after VATS occur in less than 5% of patients, in which case a redo-VATS is a feasible therapeutical option. Randomized controlled trials are urgently needed to shed light on the best definitive management of SP. Keywords: thoracoscopy; VATS; spontaneous pneumothorax; bullectomy; pleurodesis Citation: Porcel, J.M.; Lee, P. Thoracoscopy for Spontaneous 1. Introduction Pneumothorax. J. Clin. Med. 2021, 10, Pneumothorax can occur spontaneously or because of trauma or procedural compli- 3835. https://doi.org/10.3390/ cation. Spontaneous pneumothoraces (SP) are divided into primary (PSP) and secondary jcm10173835 (SSP). PSP occurs in someone without a known underlying lung disease, whereas SPP appears as a complication of an underlying lung disease, such as chronic obstructive pul- Academic Editors: Paola Ciriaco and Robert Hallifax monary disease, lung cancer, interstitial lung disease, or tuberculosis. -

Nonintubated Thoracoscopic Surgery Using Regional Anesthesia and Vagal Block and Targeted Sedation
Original Article Nonintubated thoracoscopic surgery using regional anesthesia and vagal block and targeted sedation Ke-Cheng Chen1,2, Ya-Jung Cheng3, Ming-Hui Hung3, Yu-Ding Tseng1, Jin-Shing Chen1,2 1Department of Surgery, National Taiwan University Hospital Yun-Lin Branch, Yun-Lin County, Taiwan; 2Division of Thoracic Surgery, Department of Surgery, National Taiwan University Hospital and National Taiwan University College of Medicine, Taipei, Taiwan; 3Department of Anesthesiology, National Taiwan University Hospital and National Taiwan University College of Medicine, Taipei, Taiwan Corresponding to: Dr. Jin-Shing Chen. Department of Surgery, National Taiwan University Hospital, No. 7, Chung Shan South Road, Taipei, Taiwan. Email: [email protected]. Objective: Thoracoscopic surgery without endotracheal intubation is a novel technique for diagnosis and treatment of thoracic diseases. This study reported the experience of nonintubated thoracoscopic surgery in a tertiary medical center in Taiwan. Methods: From August 2009 through August 2013, 446 consecutive patients with lung or pleural diseases were treated by nonintubated thoracoscopic surgery. Regional anesthesia was achieved by thoracic epidural anesthesia or internal intercostal blockade. Targeted sedation was performed with propofol infusion to achieve a bispectral index value between 40 and 60. The demographic data and clinical outcomes were evaluated by retrospective chart review. Results: Thoracic epidural anesthesia was used in 290 patients (65.0%) while internal intercostal blockade was used in 156 patients (35.0%). The final diagnosis were primary lung cancer in 263 patients (59.0%), metastatic lung cancer in 38 (8.5%), benign lung tumor in 140 (31.4%), and pneumothorax in 5 (1.1%). The median anesthetic induction time was 30 minutes by thoracic epidural anesthesia and was 10 minutes by internal intercostal blockade. -

Diagnostic Direct Laryngoscopy, Bronchoscopy & Esophagoscopy
Post-Operative Instruction Sheet Diagnostic Direct Laryngoscopy, Bronchoscopy & Esophagoscopy Direct Laryngoscopy: Examination of the voice box or larynx (pronounced “lair-inks”) under general anesthesia. An instrument called a laryngoscope is carefully placed into the mouth and used to visualize the larynx and surrounding structures. Bronchoscopy: Examination of the windpipe below the voice box in the neck and chest under general anesthesia. A long narrow telescope is passed through the larynx and used to carefully inspect the structures of the trachea and bronchi. Esophagoscopy: Examination of the swallowing pipe in the neck and chest under general anesthesia. An instrument called an esophagoscope is passed into the esophagus (just behind the larynx and trachea) and used to visualize the mucus membranes and surrounding structures of the esophagus. Frequently a small biopsy is taken to evaluate for signs of esophageal inflammation (esophagitis). What to Expect: Diagnostic airway endoscopy procedures generally take about 45 minutes to complete. Usually the procedure is well-tolerated and the child is back-to-normal the next day. Mild throat or tongue discomfort may persist for a few days after the procedure and is usually well-controlled with over-the-counter acetaminophen (Tylenol) or ibuprofen (Motrin). Warning Signs: Contact the office immediately at (603) 650-4399 if any of the following develop: • Worsening harsh, high-pitched noisy-breathing (stridor) • Labored breathing with chest retractions or flaring of the nostrils • Bluish discoloration of the lips or fingernails (cyanosis) • Persistent fever above 102°F that does not respond to Tylenol or Motrin • Excessive coughing or respiratory distress during feeding • Coughing or throwing up bright red blood • Excessive drowsiness or unresponsiveness Diet: Resume baseline diet (no special postoperative diet restrictions). -
The Method of Medical Thoracoscopy 2Nd Edition
® THE METHOD OF MEDICAL THORACOSCOPY 2nd Edition Ralf HEINE Jan Hendrik BARTELS Christian WEISS THE METHOD OF MEDICAL THORACOSCOPY 2nd Edition Ralf HEINE, MD Jan Hendrik BARTELS, MD Christian WEISS Medical Clinic III – Pneumonology, Hematology-Oncology and Palliative Medicine Hospital of St. Elisabeth and St. Barbara Halle (Saale), Germany 4 The Method of Medical Thoracoscopy Cover image: The Method of Medical Thoracoscopy Andreas Heine 2nd Edition Ralf Heine, MD Jan Hendrik Bartels, MD Christian Weiss Medical Clinic III – Pneumonology, Hematology-Oncology and Palliative Medicine, Hospital of St. Elisabeth and St. Barbara, Halle (Saale), Germany Correspondence address of the author: Dr. med. Ralf Heine Facharzt für Innere Medizin, Pneumologie Important notes: und Notfallmedizin Medical knowledge is ever changing. As new research and clinical Chefarzt der Medizinischen Klinik III – Pneumologie, experience broaden our knowledge, changes in treat ment and therapy Häma tologie-Onkologie und Palliativmedizin may be required. The authors and editors of the material herein Krankenhaus St. Elisabeth und St. Barbara, Halle/Saale have consulted sources believed to be reliable in their efforts to provide information that is complete and in accord with the Mauerstr. 5 standards accept ed at the time of publication. However, in view of 06110 Halle/Saale, Germany the possibili ty of human error by the authors, editors, or publisher, or changes in medical knowledge, neither the authors, editors, All rights reserved. publisher, nor any other party who has been involved in the prepara- nd | st tion of this booklet, warrants that the information contained herein is 2 edition 1 edition 2007 in every respect accurate or complete, and they are not responsible © 2015 GmbH for any errors or omissions or for the results obtained from use of P.O. -

A Clinical Prediction Rule for Pulmonary Complications After Thoracic Surgery for Primary Lung Cancer
A Clinical Prediction Rule for Pulmonary Complications After Thoracic Surgery for Primary Lung Cancer David Amar, MD,* Daisy Munoz, MD,* Weiji Shi, MS,† Hao Zhang, MD,* and Howard T. Thaler, PhD† BACKGROUND: There is controversy surrounding the value of the predicted postoperative diffusing capacity of lung for carbon monoxide (DLCOppo) in comparison to the forced expired volume in 1 s for prediction of pulmonary complications (PCs) after thoracic surgery. METHODS: Using a prospective database, we performed an analysis of 956 patients who had resection for lung cancer at a single institution. PC was defined as the occurrence of any of the following: atelectasis, pneumonia, pulmonary embolism, respiratory failure, and need for supplemental oxygen at hospital discharge. RESULTS: PCs occurred in 121 of 956 patients (12.7%). Preoperative chemotherapy (odds ratio 1.64, 95% confidence interval 1.06–2.55, P ϭ 0.02, point score 2) and a lower DLCOppo (odds ratio per each 5% decrement 1.13, 95% confidence interval 1.06–1.19, P Ͻ 0.0001, point score 1 per each 5% decrement of DLCOppo less than 100%) were independent risk factors for PCs. We defined 3 overall risk categories for PCs: low Յ10 points, 39 of 448 patients (9%); intermediate 11–13 points, 37 of 256 patients (14%); and high Ն14 points, 42 of 159 patients (26%). The median (range) length of hospital stay was significantly greater for patients who developed PCs than for those who did not: 12 (3–113) days vs 6 (2–39) days, P Ͻ 0.0001, respectively. Similarly, 30-day mortality was significantly more frequent for patients who developed PCs than for those who did not: 16 of 121 (13.2%) vs 6 of 835 (0.7%), P Ͻ 0.0001. -

Answer Key Chapter 1
Instructor's Guide AC210610: Basic CPT/HCPCS Exercises Page 1 of 101 Answer Key Chapter 1 Introduction to Clinical Coding 1.1: Self-Assessment Exercise 1. The patient is seen as an outpatient for a bilateral mammogram. CPT Code: 77055-50 Note that the description for code 77055 is for a unilateral (one side) mammogram. 77056 is the correct code for a bilateral mammogram. Use of modifier -50 for bilateral is not appropriate when CPT code descriptions differentiate between unilateral and bilateral. 2. Physician performs a closed manipulation of a medial malleolus fracture—left ankle. CPT Code: 27766-LT The code represents an open treatment of the fracture, but the physician performed a closed manipulation. Correct code: 27762-LT 3. Surgeon performs a cystourethroscopy with dilation of a urethral stricture. CPT Code: 52341 The documentation states that it was a urethral stricture, but the CPT code identifies treatment of ureteral stricture. Correct code: 52281 4. The operative report states that the physician performed Strabismus surgery, requiring resection of the medial rectus muscle. CPT Code: 67314 The CPT code selection is for resection of one vertical muscle, but the medial rectus muscle is horizontal. Correct code: 67311 5. The chiropractor documents that he performed osteopathic manipulation on the neck and back (lumbar/thoracic). CPT Code: 98925 Note in the paragraph before code 98925, the body regions are identified. The neck would be the cervical region; the thoracic and lumbar regions are identified separately. Therefore, three body regions are identified. Correct code: 98926 Instructor's Guide AC210610: Basic CPT/HCPCS Exercises Page 2 of 101 6. -
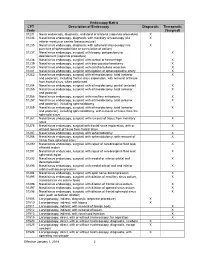

Endoscopy Matrix
Endoscopy Matrix CPT Description of Endoscopy Diagnostic Therapeutic Code (Surgical) 31231 Nasal endoscopy, diagnostic, unilateral or bilateral (separate procedure) X 31233 Nasal/sinus endoscopy, diagnostic with maxillary sinusoscopy (via X inferior meatus or canine fossa puncture) 31235 Nasal/sinus endoscopy, diagnostic with sphenoid sinusoscopy (via X puncture of sphenoidal face or cannulation of ostium) 31237 Nasal/sinus endoscopy, surgical; with biopsy, polypectomy or X debridement (separate procedure) 31238 Nasal/sinus endoscopy, surgical; with control of hemorrhage X 31239 Nasal/sinus endoscopy, surgical; with dacryocystorhinostomy X 31240 Nasal/sinus endoscopy, surgical; with concha bullosa resection X 31241 Nasal/sinus endoscopy, surgical; with ligation of sphenopalatine artery X 31253 Nasal/sinus endoscopy, surgical; with ethmoidectomy, total (anterior X and posterior), including frontal sinus exploration, with removal of tissue from frontal sinus, when performed 31254 Nasal/sinus endoscopy, surgical; with ethmoidectomy, partial (anterior) X 31255 Nasal/sinus endoscopy, surgical; with ethmoidectomy, total (anterior X and posterior 31256 Nasal/sinus endoscopy, surgical; with maxillary antrostomy X 31257 Nasal/sinus endoscopy, surgical; with ethmoidectomy, total (anterior X and posterior), including sphenoidotomy 31259 Nasal/sinus endoscopy, surgical; with ethmoidectomy, total (anterior X and posterior), including sphenoidotomy, with removal of tissue from the sphenoid sinus 31267 Nasal/sinus endoscopy, surgical; with removal of -

Local Anaesthetic Thoracoscopy Information for Patients
Oxford Centre for Respiratory Medicine Local Anaesthetic Thoracoscopy Information for patients Provisional appointment date and time……...............................…. Important information about your thoracoscopy • Do not eat or drink anything for 6 hours before your procedure. You can take any medicines you need to have with a sip of water up until 2 hours before your procedure. • Tell your doctor about all the medication you take and any medical conditions you have. • Tell us if you are on any blood thinning or diabetes medications – these are normally stopped before your procedure. It is important that you continue to take any other medications (including those for high blood pressure). • Bring enough belongings for a five night stay in hospital – please do not bring in any valuables. • If your doctor tells you that you are likely to go home the same day, please arrange for someone to bring you in and take you home from the thoracoscopy. You should also not be alone overnight after your thoracoscopy. For 24 hours after the thoracoscopy you cannot drive, return to work, operate machinery, drink alcohol, sign legal documents or be responsible for small children. • Contact your doctor if you are short of breath or having increasing chest pain. Page 2 What is a thoracoscopy? A thoracoscopy is an examination of the pleural cavity (the space between your lung and chest wall) with a special camera called a thoracoscope. This allows us to learn more about your illness and the cause of the fluid or air in your chest. Lining of lung (lined by pleural membranes) Lung Ribs Fluid (pleural effusion) or air (pneumothorax) in the pleural space/cavity around the lung Inside of chest wall (lined by pleural membranes) During the thoracoscopy, the doctor can also take small samples (called biopsies) from the pleural membranes on the inside of your chest and drain any fluid that has collected there. -

Airway Versus Transbronchial Biopsy and BAL in Lung Transplant Recipients: Different but Complementary
Eur Respir J 1997; 10: 2876–2880 Copyright ERS Journals Ltd 1997 DOI: 10.1183/09031936.97.10122876 European Respiratory Journal Printed in UK - all rights reserved ISSN 0903 - 1936 Airway versus transbronchial biopsy and BAL in lung transplant recipients: different but complementary C. Ward, G.I. Snell, B. Orsida, L. Zheng, T.J. Williams, E.H. Walters Airway versus transbronchial biopsy and BAL in lung transplant recipients: different Dept of Respiratory Medicine, Alfred but complementary. C. Ward, G.I. Snell, B. Orsida, L. Zheng, T.J. Williams, E.H. Walters. Hospital and Monash University Medical ©ERS Journals Ltd 1997. School, Melbourne, Australia. ABSTRACT: Lung transplantation is now an established therapeutic intervention Correspondence: E.H Walters for end-stage cardiopulmonary disease in humans. Chronic rejection, in the form Dept of Respiratory Medicine of bronchiolitis obliterans syndrome (BOS), remains the commonest cause of mor- Alfred Hospital bidity and mortality in those surviving more than 3 months. The pathology of BOS Prahran involves airway changes. We have evaluated the potential for endobronchial biop- Melbourne sies (EBB) to complement existing sampling methods used in allograft monitoring Victoria 3181 and have compared the results of EBB findings with those of bronchoalveolar Australia lavage (BAL) and transbronchial biopsy (TBB) in 18 clinically stable patients. Keywords: Bronchoalveolar lavage We found that all the EBB had inflammatory cells present but that only five endobronchial biopsy TBB specimens had evidence of inflammation, with airway material being present lung transplant in 78% of the TBB. Paired BAL and EBB yielded different results, with no cor- transbronchial biopsy relations between total macrophages, lymphocytes, CD4+ cells or CD8+ cells. -
A Late Complication of a Diagnostic Mediastinoscopy
Thorax: first published as 10.1136/thx.33.1.115 on 1 February 1978. Downloaded from Thorax, 1978, 33, 115-116 A late complication of a diagnostic mediastinoscopy H. F. W. HOITSMA1, E. T. T. TJHO2, AND M. A. CUESTA' From the Departments of General Surgery' and Thoracic Medicine2, Het Academisch Ziekenhuis der Vrije Universiteit, Amsterdam, The Netherlands Hoitsma, H. F. W., Tjho, E. T. T., and Cuesta, M. A. (1978). Thorax, 33, 115-116. A late complication of a diagnostic mediastinoscopy. A 69-year-old man with a moderately well differentiated squamous-cell carcinoma of the lung, underwent a mediastinoscopy. All histological examinations of the mediastinal nodes were negative. The patient was treated with a curative left pneumonectomy. Three months after this negative mediastinoscopy the patient developed a metastasis in the mediastinoscopy scar. A report of this case and a review of the literature are presented. In 1959, Carlens wrote the article, which has since all of them at biopsy. Histological investigation of become famous, entitled 'Mediastinoscopy: a the biopsy specimens showed fragmented and com- method for inspection and tissue biopsy in the plete lymph nodes with an intact structure. Besides superior mediastinum'. He described a method anthracotic infiltration there was a firm, histiocytic which he had developed in order to assess the reaction. No tumour cells were found. copyright. stage of lymphatic metastasis of carcinoma of the Ten days later the patient underwent a left lung. Since its introduction it has become a much pneumonectomy. All visible nodes in the hilus and used method to avoid unnecessary thoracotomies. -

Coding Billing
Coding&Billing Quarterly JANUARY 2018 Welcome to the January issue of the ATS Coding and Billing Quarterly. This issue covers a lot of new Medicare EDITOR payment policies that will impact ATS members and their ALAN L. PLUMMER, MD ATS RUC Advisor practices starting Jan. 1, 2018. ADVISORY BOARD MEMBERS: Medicare released the final rules for both the 2018 Medicare KEVIN KOVITZ, MD Chair, ATS Clinical Practice Committee Physician Fee Schedule – which covers payment and coverage KATINA NICOLACAKIS, MD policies for physicians and other Medicare Part B providers Member, ATS Clinical Practice Committee – and the Medicare Hospital Outpatient Prospective ATS Alternate RUC Advisorr Payment Rule – which deals with reimbursement STEPHEN P. HOFFMANN, MD Member, ATS Clinical Practice Committee for hospital outpatients services. While neither rule includes any major ATS CPT Advisor policy shifts that will directly impact ATS members, there are a number of MICHAEL NELSON, MD reimbursement changes (positive and negative) that will affect procedure code Member, ATS Clinical Practice Committee ATS Alternate CPT Advisor families of interest to ATS members. This issue will both alert you to these STEVE G. PETERS, MD payment changes and provide some background on why these reimbursement Member, ATS Clinical Practice Committee changes are happening. The New Year will bring in some revised CPT codes of interest to the ATS In This Issue community. This issue explains these revised CPT codes. Also covered in Revised CPT Codes for 2018, page 2 this edition is news about the revised ICD-10-CM codes for pulmonary hypertension. While the revised family of codes was in use starting Oct.