Assessment and Retrieval of Aspirated Tracheoesophageal Prosthesis in the Ambulatory Setting
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Diagnostic Direct Laryngoscopy, Bronchoscopy & Esophagoscopy
Post-Operative Instruction Sheet Diagnostic Direct Laryngoscopy, Bronchoscopy & Esophagoscopy Direct Laryngoscopy: Examination of the voice box or larynx (pronounced “lair-inks”) under general anesthesia. An instrument called a laryngoscope is carefully placed into the mouth and used to visualize the larynx and surrounding structures. Bronchoscopy: Examination of the windpipe below the voice box in the neck and chest under general anesthesia. A long narrow telescope is passed through the larynx and used to carefully inspect the structures of the trachea and bronchi. Esophagoscopy: Examination of the swallowing pipe in the neck and chest under general anesthesia. An instrument called an esophagoscope is passed into the esophagus (just behind the larynx and trachea) and used to visualize the mucus membranes and surrounding structures of the esophagus. Frequently a small biopsy is taken to evaluate for signs of esophageal inflammation (esophagitis). What to Expect: Diagnostic airway endoscopy procedures generally take about 45 minutes to complete. Usually the procedure is well-tolerated and the child is back-to-normal the next day. Mild throat or tongue discomfort may persist for a few days after the procedure and is usually well-controlled with over-the-counter acetaminophen (Tylenol) or ibuprofen (Motrin). Warning Signs: Contact the office immediately at (603) 650-4399 if any of the following develop: • Worsening harsh, high-pitched noisy-breathing (stridor) • Labored breathing with chest retractions or flaring of the nostrils • Bluish discoloration of the lips or fingernails (cyanosis) • Persistent fever above 102°F that does not respond to Tylenol or Motrin • Excessive coughing or respiratory distress during feeding • Coughing or throwing up bright red blood • Excessive drowsiness or unresponsiveness Diet: Resume baseline diet (no special postoperative diet restrictions). -

Effectiveness and Superiority of Ventilation with Laryngeal Mask
a & hesi C st lin e ic n a A l f R o e l s Journal of Anesthesia & Clinical e a a n r r Wu et al., J Anesth Clin Res 2017, 8:7 c u h o J DOI: 10.4172/2155-6148.1000738 ISSN: 2155-6148 Research Research Article Open Access Effectiveness and Superiority of Ventilation with Laryngeal Mask Airway in Partial Laryngectomy Jinhong Wu, Weixing Li and Wenxian Li* Department of Anesthesiology, Eye, Ear, Nose and Throat Hospital, Fudan University, China *Corresponding author: Wenxian Li, Department of Anesthesiology, Eye, Ear, Nose and Throat Hospital, Fudan University, 83 Fenyang Road, Xuhui District, Shanghai 200031, China, Tel: +86-21-64377134; Fax: +86-21-64377151; E-mail: [email protected] Received date: Jun 06, 2017; Accepted date: Jul 01, 2017; Published date: Jul 04, 2017 Copyright: © 2017 Wu J, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. Abstract Background: Laryngeal carcinoma occupies the space of glottis. It may lead to difficult airway, and is prone to bleed if intubated with endotracheal tube (ETI). Intubation can also result in the possibility of tumor cultivation in the lung. Use of laryngeal mask airway (LMA) could avoid the disadvantages of endotracheal intubation, which would benefit patients undergoing partial laryngectomy. Methods: This was a randomized controlled clinical trial. Thirty adult patients scheduled to receive partial laryngectomy were enrolled. All study subjects received an ASA rating of grade III. -

A Clinical Prediction Rule for Pulmonary Complications After Thoracic Surgery for Primary Lung Cancer
A Clinical Prediction Rule for Pulmonary Complications After Thoracic Surgery for Primary Lung Cancer David Amar, MD,* Daisy Munoz, MD,* Weiji Shi, MS,† Hao Zhang, MD,* and Howard T. Thaler, PhD† BACKGROUND: There is controversy surrounding the value of the predicted postoperative diffusing capacity of lung for carbon monoxide (DLCOppo) in comparison to the forced expired volume in 1 s for prediction of pulmonary complications (PCs) after thoracic surgery. METHODS: Using a prospective database, we performed an analysis of 956 patients who had resection for lung cancer at a single institution. PC was defined as the occurrence of any of the following: atelectasis, pneumonia, pulmonary embolism, respiratory failure, and need for supplemental oxygen at hospital discharge. RESULTS: PCs occurred in 121 of 956 patients (12.7%). Preoperative chemotherapy (odds ratio 1.64, 95% confidence interval 1.06–2.55, P ϭ 0.02, point score 2) and a lower DLCOppo (odds ratio per each 5% decrement 1.13, 95% confidence interval 1.06–1.19, P Ͻ 0.0001, point score 1 per each 5% decrement of DLCOppo less than 100%) were independent risk factors for PCs. We defined 3 overall risk categories for PCs: low Յ10 points, 39 of 448 patients (9%); intermediate 11–13 points, 37 of 256 patients (14%); and high Ն14 points, 42 of 159 patients (26%). The median (range) length of hospital stay was significantly greater for patients who developed PCs than for those who did not: 12 (3–113) days vs 6 (2–39) days, P Ͻ 0.0001, respectively. Similarly, 30-day mortality was significantly more frequent for patients who developed PCs than for those who did not: 16 of 121 (13.2%) vs 6 of 835 (0.7%), P Ͻ 0.0001. -

Gemstone Spectral Imaging Technique
Gemstone Spectral Imaging HANDBOOK OF CLINICAL EVIDENCE for Radiologists and Radiographers Vascular Performance Artefact Innovation Reduction Technology Material Decomposition Oncology gehealthcare.com Introduction Diagnostic Imaging is a fast-moving field harvesting the latest technologies from the newest in hardware capabilities to the first artificial intelligence applications in radiology. The objective is improving patient clinical outcomes and we are now expecting to go beyond by improving the patient pathway, reducing the number of exams and giving access to the right diagnosis, effortlessly. CT imaging has quickly become the cornerstone of imaging departments, not only providing more and more anatomical information by improving image quality, but also taking the lead in functional information to really assess the impact of disease. Gemstone™ Spectral Imaging (GSI) is the avenue to answer challenging clinical questions by using a single scan to provide both anatomical and functional information in one study thereby reducing the number of exams needed to deliver a diagnosis. This technique is widely accepted by clinical societies and peer reviewed publications show patient & clinical outcomes. Through this handbook, you will find the latest uses of our GSI technology, its outcomes and real testimonials from our users. We truly want to help you integrate this into your daily clinical practice in multiple clinical applications to further add value to your patient care pathway in CT. We have gathered infographics illustrating the use of GSI, clinical examples from all over Europe and a brief literature review. This handbook is for your patients, for your team and for you. We hope you find it valuable and as always contact your GE Healthcare representative if you have any questions. -

ACR Manual on Contrast Media
ACR Manual On Contrast Media 2021 ACR Committee on Drugs and Contrast Media Preface 2 ACR Manual on Contrast Media 2021 ACR Committee on Drugs and Contrast Media © Copyright 2021 American College of Radiology ISBN: 978-1-55903-012-0 TABLE OF CONTENTS Topic Page 1. Preface 1 2. Version History 2 3. Introduction 4 4. Patient Selection and Preparation Strategies Before Contrast 5 Medium Administration 5. Fasting Prior to Intravascular Contrast Media Administration 14 6. Safe Injection of Contrast Media 15 7. Extravasation of Contrast Media 18 8. Allergic-Like And Physiologic Reactions to Intravascular 22 Iodinated Contrast Media 9. Contrast Media Warming 29 10. Contrast-Associated Acute Kidney Injury and Contrast 33 Induced Acute Kidney Injury in Adults 11. Metformin 45 12. Contrast Media in Children 48 13. Gastrointestinal (GI) Contrast Media in Adults: Indications and 57 Guidelines 14. ACR–ASNR Position Statement On the Use of Gadolinium 78 Contrast Agents 15. Adverse Reactions To Gadolinium-Based Contrast Media 79 16. Nephrogenic Systemic Fibrosis (NSF) 83 17. Ultrasound Contrast Media 92 18. Treatment of Contrast Reactions 95 19. Administration of Contrast Media to Pregnant or Potentially 97 Pregnant Patients 20. Administration of Contrast Media to Women Who are Breast- 101 Feeding Table 1 – Categories Of Acute Reactions 103 Table 2 – Treatment Of Acute Reactions To Contrast Media In 105 Children Table 3 – Management Of Acute Reactions To Contrast Media In 114 Adults Table 4 – Equipment For Contrast Reaction Kits In Radiology 122 Appendix A – Contrast Media Specifications 124 PREFACE This edition of the ACR Manual on Contrast Media replaces all earlier editions. -

Closed Rhinoplasty: Effects and Changes on Voice - a Preliminary Report
Topic: EuRePS Meeting 2015: best five papers Closed rhinoplasty: effects and changes on voice - a preliminary report Giuseppe Guarro, Romano Maffia, Barbara Rasile, Carmine Alfano Department of Plastic and Reconstructive Surgery, University of Perugia, 06156 Perugia, Italy. Address for correspondence: Dr. Giuseppe Guarro, Department of Plastic and Reconstructive Surgery, University of Perugia, S. Andrea delle Fratte, 06156 Perugia, Italy. E-mail: [email protected] ABSTRACT Aim: Effects of rhinoplasty were already studied from many points of view: otherwise poor is scientific production focused on changes of voice after rhinoplasty. This preliminary study analyzed objectively and subjectively these potential effects on 19 patients who underwent exclusively closed rhinoplasty. Methods: This preliminary evaluation was conducted from September 2012 to May 2013 and 19 patients have undergone primary rhinoplasty with exclusively closed approach (7 males, 12 females). All patients were evaluated before and 6 months after surgery. Each of them answered to a questionnaire (Voice Handicap Index Score) and the voice was recorded for spectrographic analysis: this system allowed to perform the measurement of the intensity and frequency of vowels (“A” and “E”) and nasal consonants (“N” and “M”) before and after surgery. Data were analysed with the Mann-Whitney test. Results: Sixteen patients showed statistically significant differences after surgery. It was detected in 69% of cases an increased frequency of emission of the consonant sounds (P = 0.046), while in 74% of cases the same phenomenon was noticed for vowel sounds (P = 0.048). Conclusion: Many patients who undergo rhinoplasty think that the intervention only leads to anatomical changes and improvement of respiratory function. -

Laryngectomy
The Head+Neck Center John U. Coniglio, MD, LLC 1065 Senator Keating Blvd. Suite 240 Rochester, NY 14618 Office Hours: 8-4 Monday-Friday t 585.256.3550 f 585.256.3554 www.RochesterHNC.com Laryngectomy SINUS Voice change, difficulty swallowing, unexplained weight loss, ear or ENDOCRINE HEAD AND NECK CANCER throat pain and a lump in the throat, smoking and alcohol use are all VOICE DISORDERS SALIVARY GLANDS indications for further evaluation. Smoking and alcohol can contribute TONSILS AND ADENOIDS to these symptoms. A direct laryngoscopy – an exam of larynx (voice EARS PEDIATRICS box), with biopsy – will help determine if a laryngectomy is indicated. SNORING / SLEEP APNEA Laryngectomy may involve partial or total removal of one or more or both vocal cords. Alteration of voice will occur with either total or partial laryngectomy. Postoperative rehabilitation is usually successful in helping the patient recover a voice that can be understood. The degree of alteration in voice depends on the extent of the disease. Partial or total laryngectomy has been a highly successful method to remove cancer of the larynx. The extent of the tumor invasion, and therefore the extent of surgery, determines the way you will communicate following surgery. The choice of surgery over other forms of treatment such as radiation or chemotherapy is determined by the site of the tumor. It is quite likely that there has been spread of the tumor to the neck; a neck or lymph node dissection may also be recommended. Complete neck dissection (exploration of the neck tissues) is performed in order to remove known or suspected lymph nodes containing cancer that has spread from the primary tumor site. -

Laryngectomy
LARYNGECTOMY Definitlon Laryngectomy is the partial or complete surgical removal of the larynx, usually as a treatment for cancer of the larynx. Purpose Normally a laryngectomy is performed to remove tumors or cancerous tissue. In rare cases, it may be done when the larynx is badly damaged by gunshot, automobile injuries, or similar violent accidents. Laryngectomies can be total or partial. Total laryngectomies are done when cancer is advanced. The entire larynx is removed. Often if the cancer has spread, other surrounding structures in the neck, such as lymph nodes, are removed at the same time. Partial laryngectomies are done when cancer is limited to one spot. Only the area with the tumor Is removed. Laryngectomies may also be performed when other cancer treatment options, such as radiation or chemotherapy. fail. Precautions Laryngectomy is done only after cancer of the larynx has been diagnosed by a series of tests that allow the otolaryngologist (a specialist often called an ear, nose, and throat doctor) to look into the throat and take tissue samples (biopsies) to confirm and stage the cancer. People need to be in good general health to undergo a laryngectomy, and will have standard pre-operative blood work and tests to make sure they are able to safely withstand the operation. Description The larynx is located slightly below the point where the throat divides into the esophagus, which takes food to the stomach, and the trachea (windpipe), which takes air to the lungs. Because of its location, the larynx plays a critical role in normal breathing, swallowing, and speaking. -

Airway Versus Transbronchial Biopsy and BAL in Lung Transplant Recipients: Different but Complementary
Eur Respir J 1997; 10: 2876–2880 Copyright ERS Journals Ltd 1997 DOI: 10.1183/09031936.97.10122876 European Respiratory Journal Printed in UK - all rights reserved ISSN 0903 - 1936 Airway versus transbronchial biopsy and BAL in lung transplant recipients: different but complementary C. Ward, G.I. Snell, B. Orsida, L. Zheng, T.J. Williams, E.H. Walters Airway versus transbronchial biopsy and BAL in lung transplant recipients: different Dept of Respiratory Medicine, Alfred but complementary. C. Ward, G.I. Snell, B. Orsida, L. Zheng, T.J. Williams, E.H. Walters. Hospital and Monash University Medical ©ERS Journals Ltd 1997. School, Melbourne, Australia. ABSTRACT: Lung transplantation is now an established therapeutic intervention Correspondence: E.H Walters for end-stage cardiopulmonary disease in humans. Chronic rejection, in the form Dept of Respiratory Medicine of bronchiolitis obliterans syndrome (BOS), remains the commonest cause of mor- Alfred Hospital bidity and mortality in those surviving more than 3 months. The pathology of BOS Prahran involves airway changes. We have evaluated the potential for endobronchial biop- Melbourne sies (EBB) to complement existing sampling methods used in allograft monitoring Victoria 3181 and have compared the results of EBB findings with those of bronchoalveolar Australia lavage (BAL) and transbronchial biopsy (TBB) in 18 clinically stable patients. Keywords: Bronchoalveolar lavage We found that all the EBB had inflammatory cells present but that only five endobronchial biopsy TBB specimens had evidence of inflammation, with airway material being present lung transplant in 78% of the TBB. Paired BAL and EBB yielded different results, with no cor- transbronchial biopsy relations between total macrophages, lymphocytes, CD4+ cells or CD8+ cells. -
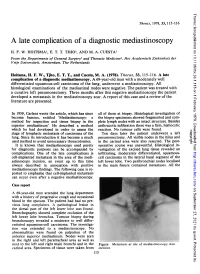
A Late Complication of a Diagnostic Mediastinoscopy
Thorax: first published as 10.1136/thx.33.1.115 on 1 February 1978. Downloaded from Thorax, 1978, 33, 115-116 A late complication of a diagnostic mediastinoscopy H. F. W. HOITSMA1, E. T. T. TJHO2, AND M. A. CUESTA' From the Departments of General Surgery' and Thoracic Medicine2, Het Academisch Ziekenhuis der Vrije Universiteit, Amsterdam, The Netherlands Hoitsma, H. F. W., Tjho, E. T. T., and Cuesta, M. A. (1978). Thorax, 33, 115-116. A late complication of a diagnostic mediastinoscopy. A 69-year-old man with a moderately well differentiated squamous-cell carcinoma of the lung, underwent a mediastinoscopy. All histological examinations of the mediastinal nodes were negative. The patient was treated with a curative left pneumonectomy. Three months after this negative mediastinoscopy the patient developed a metastasis in the mediastinoscopy scar. A report of this case and a review of the literature are presented. In 1959, Carlens wrote the article, which has since all of them at biopsy. Histological investigation of become famous, entitled 'Mediastinoscopy: a the biopsy specimens showed fragmented and com- method for inspection and tissue biopsy in the plete lymph nodes with an intact structure. Besides superior mediastinum'. He described a method anthracotic infiltration there was a firm, histiocytic which he had developed in order to assess the reaction. No tumour cells were found. copyright. stage of lymphatic metastasis of carcinoma of the Ten days later the patient underwent a left lung. Since its introduction it has become a much pneumonectomy. All visible nodes in the hilus and used method to avoid unnecessary thoracotomies. -

Coding Billing
Coding&Billing Quarterly JANUARY 2018 Welcome to the January issue of the ATS Coding and Billing Quarterly. This issue covers a lot of new Medicare EDITOR payment policies that will impact ATS members and their ALAN L. PLUMMER, MD ATS RUC Advisor practices starting Jan. 1, 2018. ADVISORY BOARD MEMBERS: Medicare released the final rules for both the 2018 Medicare KEVIN KOVITZ, MD Chair, ATS Clinical Practice Committee Physician Fee Schedule – which covers payment and coverage KATINA NICOLACAKIS, MD policies for physicians and other Medicare Part B providers Member, ATS Clinical Practice Committee – and the Medicare Hospital Outpatient Prospective ATS Alternate RUC Advisorr Payment Rule – which deals with reimbursement STEPHEN P. HOFFMANN, MD Member, ATS Clinical Practice Committee for hospital outpatients services. While neither rule includes any major ATS CPT Advisor policy shifts that will directly impact ATS members, there are a number of MICHAEL NELSON, MD reimbursement changes (positive and negative) that will affect procedure code Member, ATS Clinical Practice Committee ATS Alternate CPT Advisor families of interest to ATS members. This issue will both alert you to these STEVE G. PETERS, MD payment changes and provide some background on why these reimbursement Member, ATS Clinical Practice Committee changes are happening. The New Year will bring in some revised CPT codes of interest to the ATS In This Issue community. This issue explains these revised CPT codes. Also covered in Revised CPT Codes for 2018, page 2 this edition is news about the revised ICD-10-CM codes for pulmonary hypertension. While the revised family of codes was in use starting Oct. -

Icd-9-Cm (2010)
ICD-9-CM (2010) PROCEDURE CODE LONG DESCRIPTION SHORT DESCRIPTION 0001 Therapeutic ultrasound of vessels of head and neck Ther ult head & neck ves 0002 Therapeutic ultrasound of heart Ther ultrasound of heart 0003 Therapeutic ultrasound of peripheral vascular vessels Ther ult peripheral ves 0009 Other therapeutic ultrasound Other therapeutic ultsnd 0010 Implantation of chemotherapeutic agent Implant chemothera agent 0011 Infusion of drotrecogin alfa (activated) Infus drotrecogin alfa 0012 Administration of inhaled nitric oxide Adm inhal nitric oxide 0013 Injection or infusion of nesiritide Inject/infus nesiritide 0014 Injection or infusion of oxazolidinone class of antibiotics Injection oxazolidinone 0015 High-dose infusion interleukin-2 [IL-2] High-dose infusion IL-2 0016 Pressurized treatment of venous bypass graft [conduit] with pharmaceutical substance Pressurized treat graft 0017 Infusion of vasopressor agent Infusion of vasopressor 0018 Infusion of immunosuppressive antibody therapy Infus immunosup antibody 0019 Disruption of blood brain barrier via infusion [BBBD] BBBD via infusion 0021 Intravascular imaging of extracranial cerebral vessels IVUS extracran cereb ves 0022 Intravascular imaging of intrathoracic vessels IVUS intrathoracic ves 0023 Intravascular imaging of peripheral vessels IVUS peripheral vessels 0024 Intravascular imaging of coronary vessels IVUS coronary vessels 0025 Intravascular imaging of renal vessels IVUS renal vessels 0028 Intravascular imaging, other specified vessel(s) Intravascul imaging NEC 0029 Intravascular