Emerging Pathogens in Meat and Poultry U.S
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Kongre Kitabı
Book of Abstracts International VETistanbul Group Congress 2014 28-30 April, 2014 Istanbul, Turkey Book of Abstracts www.vetistanbul2014.org International VETistanbul Group Congress 2014 28-30 April 2014 International VETistanbul Group Congress 2014 28-30 April, 2014 Istanbul, Turkey Organizing Committee Prof. Dr. Halil GÜNEŞ, Chair Prof. Dr. Bülent EKİZ Prof. Dr. Ali AYDIN Assoc. Prof. Dr. Serkan İKİZ Assoc. Prof. Dr. Hasret DEMİRCAN YARDİBİ Assoc. Prof. Dr. Gülsün PAZVANT Scientific Committee* Prof. Dr. Kemal AK, Turkey Prof. Dr. Anatoliy ALEXANDROVICH STEKOLNIKOV, Russia Prof. Dr. Bogdan AMINKOV, Bulgaria Prof. Dr. Geno ATASANOV ANGELOV, Bulgaria Prof. Dr. Hajrudin BESIROVIC, Bosnia and Herzegovina Prof. Dr. Nihad FEJZIC, Bosnia and Herzegovina Assoc. Prof. Dr. Plamen GEORGIEV, Bulgaria Prof. Dr. Zehra HAJRULAI MUSLIU, Macedonia Assoc. Prof. Dr. Afrim HAMIDI, Kosovo Prof. Dr. Telman ISKENDEROV, Azerbaijan Prof. Dr. Larisa KARPENKO, Russia Prof. Dr. Ismail KIRSAN, Turkey Prof. Dr. Mihni LYUTSKANOV, Bulgaria Assoc. Prof. Dr. Avni ROBAJ, Kosovo Prof. Dr. Velimir STOJKOVSKI, Macedonia Prof. Dr. Semsir VELIYEV, Azerbaijan *Alphabetically listed by the according to the family name Scientific Secreteria Prof. Dr. Bülent EKİZ, Turkey Dr. Karlo MURATOĞLU, Turkey International VETistanbul Group Congress 2014, 28-30 April, Istanbul, Turkey IV International VETistanbul Group Congress 2014 28-30 April 2014 Dear Respectable Colleagues and Guests, First of all, I greet you all with my heart. Also, I would like to thank you for taking place on our side due to the contribution given to the establishment of VETistanbul Group. Known as, VETistanbul Group was established, under the coordination of Istanbul University, with joint decision of Veterinary Faculty of the University of Sarajevo, Saint Petersburg State Academy of Veterinary Medicine, Stara Zagora Trakia University, Ss. -
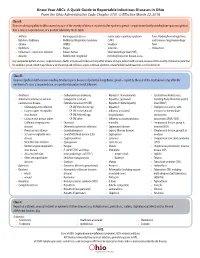
The Know Your Abcs: a Quick Guide to Reportable Infectious Diseases
Know Your ABCs: A Quick Guide to Reportable Infectious Diseases in Ohio From the Ohio Administrative Code Chapter 3701-3; Effective March 22, 2018 Class A: Diseases of major public health concern because of the severity of disease or potential for epidemic spread – report immediately via telephone upon recognition that a case, a suspected case, or a positive laboratory result exists. • Anthrax • Meningococcal disease • Severe acute respiratory syndrome fever, Marburg hemorrhagic fever, • Botulism, foodborne • Middle East Respiratory Syndrome (SARS) and Crimean-Congo hemorrhagic • Cholera (MERS) • Smallpox fever • Diphtheria • Plague • Tularemia • Yellow fever • Influenza A – novel virus infection • Rabies, human • Viral hemorrhagic fever (VHF), • Measles • Rubella (not congenital) including Ebola virus disease, Lassa Any unexpected pattern of cases, suspected cases, deaths or increased incidence of any other disease of major public health concern, because of the severity of disease or potential for epidemic spread, which may indicate a newly recognized infectious agent, outbreak, epidemic, related public health hazard or act of bioterrorism. Class B: Disease of public health concern needing timely response because of potential for epidemic spread – report by the end of the next business day after the existence of a case, a suspected case, or a positive laboratory result is known. • Amebiasis • Carbapenemase-producing • Hepatitis C (non-perinatal) • Spotted Fever Rickettsiosis, • Arboviral neuroinvasive and non- carbapenem-resistant • Hepatitis C (perinatal) including Rocky Mountain spotted neuroinvasive disease: Enterobacteriaceae (CP-CRE) • Hepatitis D (delta hepatitis) fever (RMSF) • Chikungunya virus infection • CP-CRE Enterobacter spp. • Hepatitis E • Staphylococcus aureus, with • Eastern equine encephalitis • CP-CRE Escherichia coli • Influenza-associated resistance or intermediate virus disease • CP-CRE Klebsiella spp. -

Reportable Diseases and Conditions
KINGS COUNTY DEPARTMENT of PUBLIC HEALTH 330 CAMPUS DRIVE, HANFORD, CA 93230 REPORTABLE DISEASES AND CONDITIONS Title 17, California Code of Regulations, §2500, requires that known or suspected cases of any of the diseases or conditions listed below are to be reported to the local health jurisdiction within the specified time frame: REPORT IMMEDIATELY BY PHONE During Business Hours: (559) 852-2579 After Hours: (559) 852-2720 for Immediate Reportable Disease and Conditions Anthrax Escherichia coli: Shiga Toxin producing (STEC), Rabies (Specify Human or Animal) Botulism (Specify Infant, Foodborne, Wound, Other) including E. coli O157:H7 Scrombroid Fish Poisoning Brucellosis, Human Flavivirus Infection of Undetermined Species Shiga Toxin (Detected in Feces) Cholera Foodborne Disease (2 or More Cases) Smallpox (Variola) Ciguatera Fish Poisoning Hemolytic Uremic Syndrome Tularemia, human Dengue Virus Infection Influenza, Novel Strains, Human Viral Hemorrhagic Fever (Crimean-Congo, Ebola, Diphtheria Measles (Rubeola) Lassa, and Marburg Viruses) Domonic Acid Poisoning (Amnesic Shellfish Meningococcal Infections Yellow Fever Poisoning) Novel Virus Infection with Pandemic Potential Zika Virus Infection Paralytic Shellfish Poisoning Plague (Specify Human or Animal) Immediately report the occurrence of any unusual disease OR outbreaks of any disease. REPORT BY PHONE, FAX, MAIL WITHIN ONE (1) WORKING DAY Phone: (559) 852-2579 Fax: (559) 589-0482 Mail: 330 Campus Drive, Hanford 93230 Conditions may also be reported electronically via the California -
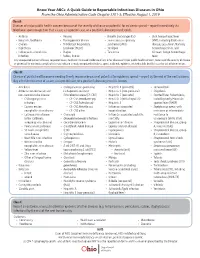
Know Your Abcs: a Quick Guide to Reportable Infectious Diseases in Ohio
Know Your ABCs: A Quick Guide to Reportable Infectious Diseases in Ohio From the Ohio Administrative Code Chapter 3701-3; Effective August 1, 2019 Class A: Diseases of major public health concern because of the severity of disease or potential for epidemic spread – report immediately via telephone upon recognition that a case, a suspected case, or a positive laboratory result exists. • Anthrax • Measles • Rubella (not congenital) • Viral hemorrhagic fever • Botulism, foodborne • Meningococcal disease • Severe acute respiratory (VHF), including Ebola virus • Cholera • Middle East Respiratory syndrome (SARS) disease, Lassa fever, Marburg • Diphtheria Syndrome (MERS) • Smallpox hemorrhagic fever, and • Influenza A – novel virus • Plague • Tularemia Crimean-Congo hemorrhagic infection • Rabies, human fever Any unexpected pattern of cases, suspected cases, deaths or increased incidence of any other disease of major public health concern, because of the severity of disease or potential for epidemic spread, which may indicate a newly recognized infectious agent, outbreak, epidemic, related public health hazard or act of bioterrorism. Class B: Disease of public health concern needing timely response because of potential for epidemic spread – report by the end of the next business day after the existence of a case, a suspected case, or a positive laboratory result is known. • Amebiasis • Carbapenemase-producing • Hepatitis B (perinatal) • Salmonellosis • Arboviral neuroinvasive and carbapenem-resistant • Hepatitis C (non-perinatal) • Shigellosis -

Global Burden of Norovirus and Prospects for Vaccine Development
Global Burden of Norovirus and Prospects for Vaccine Development Primary author Ben Lopman Centers for Disease Control and Prevention Contributors and Reviewers Robert Atmar, Baylor College of Medicine Ralph Baric, University of North Carolina Mary Estes, Baylor College of Medicine Kim Green, NIH; National Institute of Allergy and Infectious Diseases Roger Glass, NIH; Fogarty International Center Aron Hall, Centers for Disease Control and Prevention Miren Iturriza-Gómara, University of Liverpool Cherry Kang, Christian Medical College Bruce Lee, Johns Hopkins University Umesh Parashar, Centers for Disease Control and Prevention Mark Riddle, Naval Medical Research Center Jan Vinjé, Centers for Disease Control and Prevention The findings and conclusions in this report are those of the authors and do not necessarily represent the official position of the Centers for Disease Control and Prevention, or the US Department of Health and Human Services. This work was funded in part by a grant from the Bill & Melinda Gates Foundation to the CDC Foundation. GLOBAL BURDEN OF NOROVIRUS AND PROSPECTS FOR VACCINE DEVELOPMENT | 1 Table of Contents 1. Executive summary ....................................................................3 2. Burden of disease and epidemiology 7 a. Burden 7 i. Global burden and trends of diarrheal disease in children and adults 7 ii. The role of norovirus 8 b. Epidemiology 9 i. Early childhood infections 9 ii. Risk factors, modes and settings of transmission 10 iii. Chronic health consequences associated with norovirus infection? 11 c. Challenges in attributing disease to norovirus 12 3. Norovirus biology, diagnostics and their interpretation for field studies and clinical trials..15 a. Norovirus virology 15 i. Genetic diversity, evolution and related challenges for diagnosis 15 ii. -

Supplemental Material S1.Pdf
Phylogeny of Selenophosphate synthetases (SPS) Supplementary Material S1 ! SelD in prokaryotes! ! ! SelD gene finding in sequenced prokaryotes! We downloaded a total of 8263 prokaryotic genomes from NCBI (see Supplementary Material S7). We scanned them with the program selenoprofiles (Mariotti 2010, http:// big.crg.cat/services/selenoprofiles) using two SPS-family profiles, one prokaryotic (seld) and one mixed eukaryotic-prokaryotic (SPS). Selenoprofiles removes overlapping predictions from different profiles, keeping only the prediction from the profile that seems closer to the candidate sequence. As expected, the great majority of output predictions in prokaryotic genomes were from the seld profile. We will refer to the prokaryotic SPS/SelD !genes as SelD, following the most common nomenclature in literature.! To be able to inspect results by hand, and also to focus on good-quality genomes, we considered a reduced set of species. We took the prok_reference_genomes.txt list from ftp://ftp.ncbi.nlm.nih.gov/genomes/GENOME_REPORTS/, which NCBI claims to be a "small curated subset of really good and scientifically important prokaryotic genomes". We named this the prokaryotic reference set (223 species - see Supplementary Material S8). We manually curated most of the analysis in this set, while we kept automatized the !analysis on the full set.! We detected SelD proteins in 58 genomes (26.0%) in the prokaryotic reference set (figure 1 in main paper), which become 2805 (33.9%) when considering the prokaryotic full set (figure SM1.1). The difference in proportion between the two sets is due largely to the presence of genomes of very close strains in the full set, which we consider redundant. -

African Meningitis Belt
WHO/EMC/BAC/98.3 Control of epidemic meningococcal disease. WHO practical guidelines. 2nd edition World Health Organization Emerging and other Communicable Diseases, Surveillance and Control This document has been downloaded from the WHO/EMC Web site. The original cover pages and lists of participants are not included. See http://www.who.int/emc for more information. © World Health Organization This document is not a formal publication of the World Health Organization (WHO), and all rights are reserved by the Organization. The document may, however, be freely reviewed, abstracted, reproduced and translated, in part or in whole, but not for sale nor for use in conjunction with commercial purposes. The views expressed in documents by named authors are solely the responsibility of those authors. The mention of specific companies or specific manufacturers' products does no imply that they are endorsed or recommended by the World Health Organization in preference to others of a similar nature that are not mentioned. CONTENTS CONTENTS ................................................................................... i PREFACE ..................................................................................... vii INTRODUCTION ......................................................................... 1 1. MAGNITUDE OF THE PROBLEM ........................................................3 1.1 REVIEW OF EPIDEMICS SINCE THE 1970S .......................................................................................... 3 Geographical distribution -

Hepatitis E Virus Genotype 3 in Shellfish, United Kingdom
LETTERS term to dramatically reduce the high 3. Biswas PK, Christensen JP, Ahmed SS, biologically relevant sentinels and incidence of HPAI in Bangladesh. We Barua H, Das A, Rahman MH. at al. Avian can indicate potential pathogens that infl uenza outbreaks in chickens, Bangla- have progressively and dramatically desh. Emerg Infect Dis. 2008;14:1909–12. are contaminating the environment. increased the scope and benefi ts of our http://dx.doi.org/10.3201/eid1412.071567 It is essential to ensure that this pilot PVC implementation program, 4. Biswas PK, Christensen JP, Ahmed SS, sustainable resource of coastal areas, but additional work is needed. To Das A, Rahman MH, Barua H, et al. where mussels and oysters are farmed Risk for infection with highly pathogenic help spread PVC approaches through- avian infl uenza virus (H5N1) in back- or collected wild, is not subjected to out the country, community leaders, yard chickens, Bangladesh. Emerg In- environmental contamination that imams of local mosques, and school fect Dis. 2009;15:1931–6. http://dx.doi. could lead to public health risks. teachers can be trained to implement org/10.3201/eid1512.090643 Risk management for bivalve 5. Biswas PK, Rahman MH, Das A, Ahmed awareness programs on safe practices SS, Giasuddin M, Christensen JP. Risk mollusks, aimed at control of fecal for raising poultry and regular clean- for highly pathogenic avian infl uenza pollution, relies heavily on the use ing and disinfection of live bird mar- H5N1 virus infection in chickens in of Escherichia coli as an indicator kets. The strengthening of biosecurity small-scale commercial farms, in a high- of fecal (sewage) contamination risk area, Bangladesh, 2008. -

Emerging Water-Borne Pathogens
Appl Microbiol Biotechnol (2003) 61:424–428 DOI 10.1007/s00253-003-1302-y MINI-REVIEW S. Sharma · P. Sachdeva · J. S. Virdi Emerging water-borne pathogens Received: 1 October 2002 / Revised: 27 February 2003 / Accepted: 28 February 2003 / Published online: 9 April 2003 Springer-Verlag 2003 Abstract Emerging water-borne pathogens constitute a number of reviews and other publications available on the major health hazard in both developed and developing subject discuss emerging and re-emerging pathogens in nations. A new dimension to the global epidemiology of general, including water-borne, without addressing the cholera—an ancient scourge—was provided by the issues specifically pertinent to emerging water-borne emergence of Vibrio cholerae O139. Also, water-borne pathogens. This review critically examines which organ- enterohaemorrhagic Escherichia coli (E. coli O157:H7), isms really qualify as emerging water-borne pathogens, although regarded as a problem of the industrialized west, the possible reasons underlying their emergence and has recently caused outbreaks in Africa. Outbreaks of specific measures to face the challenge posed by them. chlorine-resistant Cryptosporidium have motivated water Due to the paucity of data, it may be difficult to decide authorities to reassess the adequacy of current water- which of all water-borne pathogens are emerging. Nev- quality regulations. Of late, a host of other organisms, ertheless, there are some clear-cut candidates. such as hepatitis viruses (including hepatitis E virus), No organism other than Vibrio cholerae could serve as Campylobacter jejuni, microsporidia, cyclospora, Yersin- a better example of an emerging water-borne pathogen. ia enterocolitica, calciviruses and environmental bacteria Cholera is an ancient scourge and to date seven like Mycobacterium spp, aeromonads, Legionella pneu- pandemics have been recorded. -

Disease Reporting-Clinician
Infections, diseases and conditions reportable by clinicians: 2015 Report immediately • Anthrax (Bacillus anthracis) • Botulism (Clostridium botulinum) • Cholera (Vibrio cholerae O1, O139, or toxigenic) • Diphtheria (Corynebacterium diphtheriae) • Hemorrhagic fever caused by viruses of the filovirus (e.g., Ebola, Marburg) or arenavirus (e.g., Lassa, Machupo) families • Influenza (novel)1 (From footnote: Influenza A virus that cannot be subtyped by commercially distributed assays) • Marine intoxication (intoxication caused by marine microorganisms or their byproducts (e.g., paralytic shellfish poisoning, domoic acid intoxication, ciguatera, scombroid) • Measles (rubeola) • Plague (Yersinia pestis) • Poliomyelitis • Rabies (human) • Rubella • SARS (Severe Acute Respiratory Syndrome or SARS-coronavirus) • Smallpox (variola) • Tularemia (Francisella tularensis) • Yellow fever • Outbreaks and uncommon illnesses (any known or suspected common-source outbreak; any uncommon illness of potential public health significance) Report within 24 hours (including weekends and holidays) • Haemophilus influenzae (any isolation or identification from a normally sterile specimen type) • Neisseria meningitidis • Pesticide poisoning Public Health Division | Infections, diseases and conditions reportable by clinicians 128 Report within one working day • Amebic infections (central nervous system only) (for example infection by Naegleria or Balamuthia spp. • Animal bites (of humans) • Arthropod vector-borne disease (babesiosis, California encephalitis, Colorado -

Helicobacter Spp. — Food- Or Waterborne Pathogens?
FRI FOOD SAFETY REVIEWS Helicobacter spp. — Food- or Waterborne Pathogens? M. Ellin Doyle Food Research Institute University of Wisconsin–Madison Madison WI 53706 Contents34B Introduction....................................................................................................................................1 Virulence Factors ...........................................................................................................................2 Associated Diseases .......................................................................................................................2 Gastrointestinal Disease .........................................................................................................2 Neurological Disease..............................................................................................................3 Other Diseases........................................................................................................................4 Epidemiology.................................................................................................................................4 Prevalence..............................................................................................................................4 Transmission ..........................................................................................................................4 Summary .......................................................................................................................................5 -

Novel Risk Factors for Coronavirus Disease-Associated Mucormycosis (CAM): a Case Control Study During the Outbreak in India
medRxiv preprint doi: https://doi.org/10.1101/2021.07.24.21261040; this version posted July 26, 2021. The copyright holder for this preprint (which was not certified by peer review) is the author/funder, who has granted medRxiv a license to display the preprint in perpetuity. It is made available under a CC-BY-NC-ND 4.0 International license . Novel risk factors for Coronavirus disease-associated mucormycosis (CAM): a case control study during the outbreak in India Umang Arora1, Megha Priyadarshi1, Varidh Katiyar2, Manish Soneja1, Prerna Garg1, Ishan Gupta1,- Vishwesh Bharadiya1, Parul Berry1, Tamoghna Ghosh1, Lajjaben Patel1 , Radhika Sarda1, Shreya Garg3, Shubham Agarwal1, Veronica Arora4, Aishwarya Ramprasad1, Amit Kumar1, Rohit Kumar Garg1, Parul Kodan1, Neeraj Nischal1, Gagandeep Singh5, Pankaj Jorwal1, Arvind Kumar1, Upendra Baitha1, Ved Prakash Meena1, Animesh Ray1, Prayas Sethi1, , Immaculata Xess5, Naval Vikram1, Sanjeev Sinha1, Ashutosh Biswas1,Alok Thakar3, Sushma Bhatnagar6, Anjan Trikha7, Naveet Wig1 1Department of Medicine, AIIMS, Delhi, India 2Department of Neurosurgery, AIIMS, Delhi, India 3Department of Otolaryngology & Head-Neck Surgery, AIIMS, Delhi, India 4Department of Medical Genetics, Sir Ganga Ram Hospital, Delhi, India 5Department of Microbiology, AIIMS, Delhi, India 6Department of Onco-anaesthesia and Palliative Medicine, AIIMS, Delhi, India 7Department of Anaesthesiology, Pain Medicine and Critical Care, AIIMS, Delhi, India 1. Umang Arora, MD (Medicine), Junior Resident, Department of Medicine, AIIMS, Delhi, India. E-mail ID: [email protected] 2. Megha Priyadarshi, DM (Infectious disease), Junior Resident, Department of Medicine, AIIMS, Delhi, India. E-mail ID: [email protected] 3. Varidh Katiyar, MCh (Neurosurgery), Chief Resident, Department of Neurosurgery AIIMS, Delhi, India. E-mail ID: [email protected] 4.