Patella Tendon Repair
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Patellofemoral Syndrome: Evaluation & Management Scott Sevinsky MSPT
Patellofemoral Syndrome: Evaluation & Management Scott Sevinsky MSPT What is Patellofemoral Syndrome? Patellofemoral syndrome (PFS) is a term commonly used to describe a condition where the patella ‘tracks’ or glides improperly between the femoral condyles. This improper tracking causes pain in the anterior knee and may lead to degenerative changes or dislocation of the knee cap. To be more precise the term ‘anterior knee pain’ is suggested to encompass all pain-related problems of the anterior part of the knee. By excluding anterior knee pain due to intra-articular pathology, peripatellar tendinitis or bursitis, plica syndromes, Sinding Larsen’s disease, Osgood Schlatter’s disease, neuromas and other rarely occurring pathologies it is suggested that remaining patients with a clinical presentation of anterior knee pain could be diagnosed with PFPS. The term ‘patellofemoral’ is used as no distinction can be made as to which specific structure of the patella or femur is affected. The term ‘chondromalacia patellae’, defined at the beginning of the 20th century to describe pathological changes of the retropatellar cartilage,7,8 was for half a century, used as a synonym for the syndrome of patellofemoral pain. However, several studies during the last 2 decades have shown a poor correlation between articular cartilage damage and the still not well-defined pain mechanism of retropatellar pain. Review of Knee Anatomy 1. Femur – thigh bone; longest bone in the body. · Lateral femoral condyle larger than medial condyle & projects farther anteriorly. · Medial femoral condyle longer anterior to posterior · Distal surfaces are convex · Intercondylar (trochlear) notch: groove in which the patella glides or ‘tracks’ 2. -

Patella Problems
Patella Problems Introduction The patella, or kneecap, can be the reason your knee hurts if it fails to function properly. Over time, wear and tear underneath the patella can also lead to degeneration of the cartilage behind the patella and cause pain, weakness and swelling of the knee joint. There are several different problems that affect the patella and the groove that it runs through as the knee is bent. These problems can affect people of all ages. Anatomy The patella, or kneecap, is the moveable bone on the front of the knee. The patella is wrapped inside a large tendon that connects the large muscles on the front of the thigh, the quadriceps muscles, to the lower leg bone. This large tendon when combined with the patella, is called the quadriceps mechanism. The quadriceps mechanism is usually referred to as two separate tendons the quadriceps tendon on top of the patella and the patellar tendon below the patella. The quadriceps mechanism allows you to straighten out the knee. The patella acts like a fulcrum to increase the force of the quadriceps muscle. The underside of the patella is covered with articular cartilage, the smooth covering of joint surfaces. This slippery surface helps the patella glide in a special groove of the thigh bone, or femur. Together the patella and the groove in the femur are called the patellofemoral mechanism. Causes Problems commonly develop when the patella suffers wear and tear. The underlying cartilage begins to degenerate, a condition sometimes referred to as chondromalacia patellae. Wear and tear can develop for several reasons. -

About Your Knee
OrthoInfo Basics About Your Knee What are the parts of the knee? Your knee is Your knee is made up of four main things: bones, cartilage, ligaments, the largest joint and tendons. in your body Bones. Three bones meet to form your knee joint: your thighbone and one of the (femur), shinbone (tibia), and kneecap (patella). Your patella sits in most complex. front of the joint and provides some protection. It is also vital Articular cartilage. The ends of your thighbone and shinbone are covered with articular cartilage. This slippery substance to movement. helps your knee bones glide smoothly across each other as you bend or straighten your leg. Because you use it so Two wedge-shaped pieces of meniscal cartilage act as much, it is vulnerable to Meniscus. “shock absorbers” between your thighbone and shinbone. Different injury. Because it is made from articular cartilage, the meniscus is tough and rubbery to help up of so many parts, cushion and stabilize the joint. When people talk about torn cartilage many different things in the knee, they are usually referring to torn meniscus. can go wrong. Knee pain or injury Femur is one of the most (thighbone) common reasons people Patella (kneecap) see their doctors. Most knee problems can be prevented or treated with simple measures, such as exercise or Articular cartilage training programs. Other problems require surgery Meniscus to correct. Tibia (shinbone) 1 OrthoInfo Basics — About Your Knee What are ligaments and tendons? Ligaments and tendons connect your thighbone Collateral ligaments. These are found on to the bones in your lower leg. -

Physio Med Self Help for Anterior Knee Pain
Physio Med Self Help 0113 229 1300 for Anterior Knee Pain There can be many causes of knee pain. Anterior knee pain or patella-femoral pain is pain that is felt under the knee cap (patella) at the front of the knee. The patella, or kneecap, can be a source of knee pain when it fails to function properly. Alignment or overuse problems of the patella can lead to wear and tear of the cartilage behind the patella. Patella-femoral pain syndrome (anterior knee pain) is a common knee problem that affects the patella and the groove that the patella slides in over the femur (thigh bone). The kneecap together with the lower end of the femur is considered to be the patella-femoral joint. Anatomy of the Area What is the patella, and what does it do? The patella (kneecap) is the moveable bone on the front of the knee. This unique bone is wrapped inside a tendon that connects the large muscles on the front of the thigh, the quadriceps muscles, to the lower leg bone. The large quadriceps tendon together with the patella and patellar ligament is called the extensor mechanism. Though we think of it as a single device, the extensor mechanism has two separate tendons, the quadriceps tendon on top of the patella, which connects the quadriceps muscle to the top of the patella, and the patellar tendon below the patella, which connects the lower portion of the patella to the shinbone (tibia). The tendon above the patella is called the suprapatella tendon and the tendon below the patella is called the infrapatella tendon. -
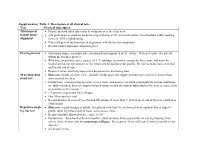
Supplementary Table 1: Description of All Clinical Tests Test Protocol
Supplementary Table 1: Description of all clinical tests Test Protocol description Tibiofemoral • Palpate & mark tibial tuberosity & midpoint over the talus neck frontal plane • Ask participant to stand on footprint map with foot at 10° external rotation, feet shoulder width, looking alignment forward, 50% weightbearing • Place callipers of inclinometer in alignment with the the two landmarks • Record varus/valgus direction in degrees Herrington test • Participant supine on plinth, knee positioned and supported in 20° of knee flexion (to place the patella within the trochlea groove) • With knee in position, place a piece of 1” Leukotape (or similar) across the knee joint, and mark the medial and lateral epicondyles of the femur and mid-point of the patella. Be sure to make note of medial and lateral end of tape • Repeat 3 times, attaching tape to this document for measuring later 30 second chair • Shoes on, middle of chair, feet ~ shoulder width apart and slightly behind knees with feet flat on floor, stand test arms crossed on chest • Instructions “stand up keeping arms across chest, and ensure you stand completely up so hips and knees are fully extended; then sit completely back down, so that the bottom fully touches the seat, as many times as possible in 30 seconds,” • 1-2 practice repetitions for technique • One 30-second test trial • Record number of correctly performed full stands (if more than ½ of way up at end of the test, counted as a full stand) Repetitive single • Shoes on, seated on edge of plinth, foot placed with heel 10 cm forward from a plumb line at edge of leg rise test plinth, other leg held at side of body, arms across chest. -

Two Cases of Combined Patellar Tendon Avulsion from the Tibia and Patella
SICOT-J 2018, 4,17 © The Authors, published by EDP Sciences, 2018 https://doi.org/10.1051/sicotj/2018014 Available online at: www.sicot-j.org CASE REPORT Two cases of combined patellar tendon avulsion from the tibia and patella Viachaslau Bradko1,2,*, William T. Stoll1, Lee S. Haruno1, Scott B. Rosenfeld1,2, and Scott D. McKay1,2 1 Department of Orthopaedic Surgery, Baylor College of Medicine, Houston, TX, USA 2 Division of Orthopaedic Surgery, Texas Children’s Hospital, Houston, TX, USA Received 2 October 2017, Accepted 8 April 2018, Published online 23 May 2018 Abstract- -Avulsion fractures of the inferior pole of the patella and proximal tibial apophysis are independently rare injuries. They occur in children due to the relative weakness of the apophyseal cartilage compared to the ligaments and tendons. The combination of these two fractures, is exceedingly rare, with only a few previously described cases in the literature. Due to the infrequent presentation of this injury, careful examination and consideration of advanced imaging is important for diagnosis and preoperative planning. Here we present two cases of combined sleeve fractures of the inferior pole of the patella and tibial apophysis, with discussion of the pathophysiology, classification, identification and management of the injury. Key words: Knee injuries, Bifocal avulsion, Patella, Patella tendon, Tibial tuberosity. Introduction Case description Case 1 An intense muscle contraction may result in the rupture of a muscle or tendon, or an avulsion fracture. In A 13-year-old male runner with history of contralateral contrast to adults, children are more likely to suffer from (left) patellar dislocation developed pain and inability to avulsion fractures due to the relative weakness of their bear weight in his right lower extremity following an apohyseal cartilage compared to connective tissues such as awkward landing after jumping over a hurdle. -

Patellofemoral Syndrome (PFS)
Scott Gudeman, MD 1260 Innovation Pkwy., Suite 100 Greenwood, IN 46143 317.884.5161 OrthoIndy.com ScottGudemanMD.com Patellofemoral Syndrome (PFS) Knee Anatomy The patella is a moveable bone in front of the knee wrapped inside a large tendon that connects the quadriceps (thigh) muscles to the tibia (lower leg bone). A healthy patella moves smoothly in a groove on the lower end of the femur. If the patella is moving incorrectly through this groove, Patellofemoral Syndrome (PFS) could form. Many muscle groups and ligaments control the triangular-shaped patella. The patella is coated on its bottom with a smooth covering called articular cartilage. The patella and the femur form a joint, called the patellofemoral joint, that is made up of muscles, soft tissue attachments and the groove where the patella rests. What is Patellofemoral Syndrome (PFS)? PFS is the medical name for a condition that causes pain in and around the kneecap. The patella (kneecap) is designed to move smoothly over a groove on the femur (thigh bone). When the patella is not moving or “tracking” properly over the femur, PFS can develop. This knee problem commonly appears in runners and athletes but non-athletes can also be affected. For the pediatric population, PFS can be jump-started during times of growth. PFS can strike at any age to any population. Causes of Patellofemoral Syndrome • Muscle imbalances in the quadriceps can cause the patella to move improperly through the groove in the femur. If one or more of the quadriceps muscles are weak, a muscle imbalance could occur. This imbalance pulls the patella off its track through the groove. -

Does the Calcaneus Serve As Hypomochlion Within the Lower Limb by a Myofascial Connection?—A Systematic Review
life Review Does the Calcaneus Serve as Hypomochlion within the Lower Limb by a Myofascial Connection?—A Systematic Review Luise Weinrich 1, Melissa Paraskevaidis 1, Robert Schleip 2,3 , Alison N. Agres 4 and Serafeim Tsitsilonis 1,* 1 Center for Musculoskeletal Surgery, Charité—Universitätsmedizin Berlin, 13353 Berlin, Germany; [email protected] (L.W.); [email protected] (M.P.) 2 Technische Universität München, 80333 München, Germany; [email protected] 3 Diploma University of Applied Sciences, 37242 Bad Sooden-Allendorf, Germany 4 Julius Wolff Institute, Berlin Institute of Health and Charité—Universitätsmedizin Berlin, 13353 Berlin, Germany; [email protected] * Correspondence: [email protected] Abstract: (1) Background: Clinical approaches have depicted interconnectivity between the Achilles tendon and the plantar fascia. This concept has been applied in rehabilitation, prevention, and in conservative management plans, yet potential anatomical and histological connection is not fully understood. (2) Objective: To explore the possible explanation that the calcaneus acts as a hypomochlion. (3) Methods: 2 databases (Pubmed and Livivo) were searched and studies, including those that examined the relationship of the calcaneus to the Achilles tendon and plantar fascia and its biomechanical role. The included studies highlighted either the anatomical, histological, or biomechanical aspect of the lower limb. (4) Results: Seventeen studies were included. Some studies depicted an anatomical connection that slowly declines with age. Others mention a histological Citation: Weinrich, L.; similarity and continuity via the paratenon, while a few papers have brought forward mechanical Paraskevaidis, M.; Schleip, R.; reasoning. (5) Conclusion: The concept of the calcaneus acting as a fulcrum in the lower limb can Agres, A.N.; Tsitsilonis, S. -

Patellofemoral Arthritis
Patellofemoral Arthritis Description Patellofemoral arthritis occurs when the articular cartilage along the trochlear groove and on the underside of the patella wears down and becomes inflamed. When cartilage wears away, it becomes frayed, and when the wear is severe, the underlying bone may become exposed. Moving the bones along this rough surface is painful. Cause Kneecap Fracture: Patellar (kneecap) fractures often damage the articular cartilage that covers and protects the Arthritis of the knee is a leading cause of underside of the bone. Even though the disability in the United States. broken bone heals, the joint surface may Patellofemoral arthritis affects your no longer be smooth. There is friction kneecap (patella bone). It causes pain in when the patella moves against the joint the front of your knee and can make it surface of the femur. Over time, this can difficult to kneel and climb stairs. lead to arthritis. Anatomy Dysplasia: Dysplasia occurs when the patella does not fit properly in the The patella is a small bone located in trochlear groove of the femur. Because of front of your knee joint — where the this, when the knee moves, there are thighbone (femur) and shinbone (tibia) increased stresses on the cartilage. This meet. It protects your knee and connects begins to wear the cartilage down. the muscles in the front of your thigh to your tibia. The patella rests in a groove on top of the femur called the trochlear groove. When you bend and straighten your knee, the patella moves back and forth inside the groove. This x-ray taken from above the knee shows The ends of the femur, trochlear groove, dysplasia that has developed into severe and the under-sides of the patella are arthritis. -

Hypothesis: Morphology & Development of Patella
International Journal of Scientific and Research Publications, Volume 3, Issue 5, May 2013 1 ISSN 2250-3153 Hypothesis: Morphology & Development of Patella Dr.Deepak S.Howale*, Dr.Zarna K.Patel** * Associate Professor- Anatomy Department, GMERS Medical College, Dharpur-Patan(Gujarat ) ** Assistant Professor- Anatomy Department, GMERS Medical College, Dharpur-Patan (Gujarat) Abstract- A Sesamoid bones are embedded in tendons, and are fibrocartilaginous according to Minowa & Gardner (1970)11 essentially hardened calcifications of the tendon itself. The Llorca (1963)12 states that it is formed by bone tissue and that its largest sesamoid bone in the human body is the patella, which prevalence is larger in men. Sesamoid bones and their functions lies suspended in between the quadriceps tendon above and the probably are to modify pressure, to diminish friction, and patellar tendon below. They are found in locations where a occasionally to alter the direction of a muscle pull. That they are tendon passes over a joint, such as the hand, knee, and foot. developed to meet certain physical requirements, evidenced by Functionally, they act to protect the tendon and to increase its the fact that they are present as cartilaginous nodules in the fetus, mechanical effect, The presence of a bone serves to hold the and in greater numbers than in the adult. According to Thilenius, tendon slightly further away from the centre of the joint this as integral parts of the skeleton phylogenetically inherited. increases its movement, and stops the tendon from flattening into Physical necessities probably come into play in selecting and in the joint. This differs from menisci, which are made of cartilage regulating the degree of development of the original cartilaginous and rather act to disperse the weight of the body on joints and nodules. -

Patella Tibia Patella Tendon Tibial Tubercle Screw
601 West Fifth Avenue, Suite 400 Spokane, WA 99204 Tibial Tubercle Osteotomy Overview This procedure, also called bone realignment, is designed to improve the movement of the patella (the kneecap) to correct patellar tracking disorder. The procedure usually requires hospitalization and general anesthesia. Incision Made After anesthesia is administered, the surgeon makes a four- to six-inch incision over the tibial tubercle. Patella Tubercle Detached The surgeon uses a bone chisel and/or a surgical saw to partially or completely detach the tibial Patella tubercle from the tibia. The patellar tendon, which tendon connects the patella to the tibia, remains connected to the tubercle. Tibia Tubercle Realigned Tibial The tibial tubercle is realigned with the patella in a tubercle position that allows for proper movement when the knee bends. Once in place, the bone is reattached to the tibia with a metal plate, wires or screws. The attachment parts are permanent unless they cause pain. If they do, they can be removed after the bone has healed in its new position. Patella Adjusted In some cases, attachments on either side of the patella may be loosened or tightened to ensure Medial retinaculum proper alignment of the patella. This procedure is may be tightened called lateral release and medial imbrication. (imbrication). End of Procedure The incision is closed with sutures or staples, and a cast or knee immobilizer is placed around the knee to restrict movement. The knee is iced and elevated. The sutures or staples are removed after two to three weeks. The knee will be swollen and Tibial crutches may be necessary for four to six weeks, tubercle with physical therapy to follow. -

Femur - Patella - Tibia - Fibula - Soft Tissue: Depending on the Degree of Exposure
DISPLAYED STRUCTURES - Femur - Patella - Tibia - Fibula - Soft tissue: depending on the degree of exposure VIEWS Lateromedial and caudolateral view craneomedial oblique (30 °) The chassis is positioned medially in the region of the stifle flow and dorsal as possible, with caution because it is a sensitive area on the horse. The beam is directed parallel to the ground laterally and centered on the patella. Depending on the temperament of the horse sometimes can not be fully appreciated in this view of the distal femur and patella. The side view oblique (caudolateral oblique craneomedial) permte appreciate osteochondral lesions of the medial condyle and the lateral edge of the trochlea on the distal femur. View caudocranial The chassis is positioned superiorly in the area of the stifle and the beam is focused on the concave region is seen in the soft tissues of the joint. Sometimes it is useful to perform two projections with varying degrees of exposure in order to appreciate all structures. View proximodistal ("skyline") Depending on the temperament of the horse can do this by extending or flexing view the tarsus. The chassis is held pressed against the proximal tibia and cranially and the beam is directed vertically proximal and lateral to the lumbar region. We extend the foot in maximum amplitude caudally leading him, and put the frame parallel to the ground supporting it the joint. The beam perpendicular to the ground 70 cm. dorsal to the stifle. DIAGNOSTIC UTILITY • Osteochondrosis • In the area of the lateral trochlear ridge of the femur and the patella articular surface is where we find most often an osteochondral defect with cartilage separation.