Patellar Dislocation and Subluxation
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Patellofemoral Syndrome: Evaluation & Management Scott Sevinsky MSPT
Patellofemoral Syndrome: Evaluation & Management Scott Sevinsky MSPT What is Patellofemoral Syndrome? Patellofemoral syndrome (PFS) is a term commonly used to describe a condition where the patella ‘tracks’ or glides improperly between the femoral condyles. This improper tracking causes pain in the anterior knee and may lead to degenerative changes or dislocation of the knee cap. To be more precise the term ‘anterior knee pain’ is suggested to encompass all pain-related problems of the anterior part of the knee. By excluding anterior knee pain due to intra-articular pathology, peripatellar tendinitis or bursitis, plica syndromes, Sinding Larsen’s disease, Osgood Schlatter’s disease, neuromas and other rarely occurring pathologies it is suggested that remaining patients with a clinical presentation of anterior knee pain could be diagnosed with PFPS. The term ‘patellofemoral’ is used as no distinction can be made as to which specific structure of the patella or femur is affected. The term ‘chondromalacia patellae’, defined at the beginning of the 20th century to describe pathological changes of the retropatellar cartilage,7,8 was for half a century, used as a synonym for the syndrome of patellofemoral pain. However, several studies during the last 2 decades have shown a poor correlation between articular cartilage damage and the still not well-defined pain mechanism of retropatellar pain. Review of Knee Anatomy 1. Femur – thigh bone; longest bone in the body. · Lateral femoral condyle larger than medial condyle & projects farther anteriorly. · Medial femoral condyle longer anterior to posterior · Distal surfaces are convex · Intercondylar (trochlear) notch: groove in which the patella glides or ‘tracks’ 2. -

Patella Problems
Patella Problems Introduction The patella, or kneecap, can be the reason your knee hurts if it fails to function properly. Over time, wear and tear underneath the patella can also lead to degeneration of the cartilage behind the patella and cause pain, weakness and swelling of the knee joint. There are several different problems that affect the patella and the groove that it runs through as the knee is bent. These problems can affect people of all ages. Anatomy The patella, or kneecap, is the moveable bone on the front of the knee. The patella is wrapped inside a large tendon that connects the large muscles on the front of the thigh, the quadriceps muscles, to the lower leg bone. This large tendon when combined with the patella, is called the quadriceps mechanism. The quadriceps mechanism is usually referred to as two separate tendons the quadriceps tendon on top of the patella and the patellar tendon below the patella. The quadriceps mechanism allows you to straighten out the knee. The patella acts like a fulcrum to increase the force of the quadriceps muscle. The underside of the patella is covered with articular cartilage, the smooth covering of joint surfaces. This slippery surface helps the patella glide in a special groove of the thigh bone, or femur. Together the patella and the groove in the femur are called the patellofemoral mechanism. Causes Problems commonly develop when the patella suffers wear and tear. The underlying cartilage begins to degenerate, a condition sometimes referred to as chondromalacia patellae. Wear and tear can develop for several reasons. -

About Your Knee
OrthoInfo Basics About Your Knee What are the parts of the knee? Your knee is Your knee is made up of four main things: bones, cartilage, ligaments, the largest joint and tendons. in your body Bones. Three bones meet to form your knee joint: your thighbone and one of the (femur), shinbone (tibia), and kneecap (patella). Your patella sits in most complex. front of the joint and provides some protection. It is also vital Articular cartilage. The ends of your thighbone and shinbone are covered with articular cartilage. This slippery substance to movement. helps your knee bones glide smoothly across each other as you bend or straighten your leg. Because you use it so Two wedge-shaped pieces of meniscal cartilage act as much, it is vulnerable to Meniscus. “shock absorbers” between your thighbone and shinbone. Different injury. Because it is made from articular cartilage, the meniscus is tough and rubbery to help up of so many parts, cushion and stabilize the joint. When people talk about torn cartilage many different things in the knee, they are usually referring to torn meniscus. can go wrong. Knee pain or injury Femur is one of the most (thighbone) common reasons people Patella (kneecap) see their doctors. Most knee problems can be prevented or treated with simple measures, such as exercise or Articular cartilage training programs. Other problems require surgery Meniscus to correct. Tibia (shinbone) 1 OrthoInfo Basics — About Your Knee What are ligaments and tendons? Ligaments and tendons connect your thighbone Collateral ligaments. These are found on to the bones in your lower leg. -

Cartilage Restoration in the Patellofemoral Joint
A Review Paper Cartilage Restoration in the Patellofemoral Joint Betina B. Hinckel, MD, PhD, Andreas H. Gomoll, MD, and Jack Farr II, MD malalignment, deconditioning, muscle imbalance Abstract and overuse) and can coexist with other lesions Although patellofemoral (PF) chondral in the knee (ligament tears, meniscal injuries, and lesions are common, the presence of cartilage lesions in other compartments). There- a cartilage lesion does not implicate a fore, careful evaluation is key in attributing knee chondral lesion as the sole source of pain. pain to PF cartilage lesions—that is, in making a As attributing PF pain to a chondral lesion “diagnosis by exclusion.” is “diagnosis by exclusion,” thorough From the start, it must be assessment of all potential structural appreciated that the vast majority and nonstructural sources of pain is the of patients will not require surgery, key to proper management. Commonly, and many who require surgery Take-Home Points for pain will not require cartilage multiple factors contribute to a patient’s ◾ Careful evaluation is symptoms. Each comorbidity must be restoration. One key to success key in attributing knee identified and addressed, and the carti- with PF patients is a good working pain to patellofemoral lage lesion treatment determined. relationship with an experienced cartilage lesions—that is, Comprehensive preoperative assess- physical therapist. in making a “diagnosis by exclusion.” ment is essential and should include a ◾ Initial treatment is non- thorough “core-to-floor” physical exam- Etiology The primary causes of PF carti- operative management ination. Treatment of symptomatic chon- focused on weight loss dral lesions in the PF joint requires specific lage lesions are patellar instabil- and extensive “core-to- technical and postoperative management, ity, chronic maltracking without floor” rehabilitation. -

Common Problems in Sports Medicine Update and Pearls for Practice
Common Problems in Sports Speaker Disclosure: Medicine Update and Pearls for Practice Founder, RunSafe™ Anthony Luke MD, MPH, CAQ (Sport Med) Founder, SportZPeak Inc. Benioff Distinguished Professor in Sports Medicine Director, Primary Care Sports Medicine, Departments of Orthopedics & Family & Community Medicine University of California, San Francisco Sanofi, Investigator initiated grant May 25, 2017 Overview Acute Hemarthrosis §Highlight common presentations 1) ACL (almost 50% in children, >70% in adults) 2) Fracture (Patella, tibial plateau, Femoral supracondylar, §Knee Physeal) §Shoulder 3) Patellar dislocation §Hip §Concussion § Unlikely meniscal lesions §Discuss basics of conservative and surgical management Emergencies Urgent Orthopedic Referral 1. Neurovascular injury §Fracture 2. Knee Dislocation §Patellar Dislocation • Associated with multiple ligament injuries “ ” (posterolateral) § Locked Joint - unable to fully extend the knee (OCD or Meniscal tear) • High risk of popliteal artery injury §Tumor • Needs arteriogram 3. Fractures (open, unstable) 4. Septic Arthritis Anterior Cruciate Ligament (ACL) What is True About ACL Tears? Tear Mechanism 1. An MRI is the best test to diagnose the ACL §Landing from a 2. The medial meniscus is most commonly torn jump, pivoting or with an ACL tear decelerating 3. All patients with an ACL tear are better off suddenly getting reconstruction vs non-op treatment §Foot fixed, valgus 4. Athletes can expect full recovery after ACL stress reconstruction Anterior Cruciate Ligament (ACL) ACL physical -

Physio Med Self Help for Anterior Knee Pain
Physio Med Self Help 0113 229 1300 for Anterior Knee Pain There can be many causes of knee pain. Anterior knee pain or patella-femoral pain is pain that is felt under the knee cap (patella) at the front of the knee. The patella, or kneecap, can be a source of knee pain when it fails to function properly. Alignment or overuse problems of the patella can lead to wear and tear of the cartilage behind the patella. Patella-femoral pain syndrome (anterior knee pain) is a common knee problem that affects the patella and the groove that the patella slides in over the femur (thigh bone). The kneecap together with the lower end of the femur is considered to be the patella-femoral joint. Anatomy of the Area What is the patella, and what does it do? The patella (kneecap) is the moveable bone on the front of the knee. This unique bone is wrapped inside a tendon that connects the large muscles on the front of the thigh, the quadriceps muscles, to the lower leg bone. The large quadriceps tendon together with the patella and patellar ligament is called the extensor mechanism. Though we think of it as a single device, the extensor mechanism has two separate tendons, the quadriceps tendon on top of the patella, which connects the quadriceps muscle to the top of the patella, and the patellar tendon below the patella, which connects the lower portion of the patella to the shinbone (tibia). The tendon above the patella is called the suprapatella tendon and the tendon below the patella is called the infrapatella tendon. -

Superior Dislocation of the Patella: Case Report and Literature Review
Orthopedics and Rheumatology Open Access Journal ISSN: 2471-6804 Case Report Ortho & Rheum Open Access Volume 4 Issue 3 - January 2017 Copyright © All rights are reserved by Paul E. Caldwell DOI: 10.19080/OROAJ.2017.04.555639 Superior Dislocation of the Patella: Case Report and Literature Review Paul E. Caldwell*, Samuel Carter and Sara E. Pearson Orthopedic Research of Virginia (SC, PEC and SEP) and Tuckahoe Orthopedic Associates, Ltd., (PEC), USA Submission: December 20, 2016; Published: January 09, 2017 *Corresponding author: Paul E. Caldwell III MD, 1501 Maple Avenue, Suite 200, Richmond, VA 23226, Ph: ; Fax: (804) 527-5961; Email: Abstract A 46-year-old female presented to the emergency department with a rare superior dislocation of the patella. Magnetic resonance imaging patellar dislocation. A closed reduction was performed, resulting in immediate pain relief and nearly full active range of motion. revealed inferior osteophytes on the patella engaging osteophytes on the superior portion of the trochlear groove resulting in a locked superior Keywords: Superior patellar dislocation; Closed reduction; Non operative treatment Case Report A 46-year-old female presented to the emergency department displacement of the patella without fracture and an unusual X-rays (Figure 1) taken in the ED demonstrated superior anterior tilt of the patella. The initial diagnosis in the ED was (ED) with complaints of significant anterior knee discomfort, a patellar tendon rupture, and a magnetic resonance image swelling and inability to ambulate or actively flex her knee. She on a piano stool. She denied any history of injury to the right reported falling at home and striking her right knee directly (MRI) of the right knee was performed after orthopedic tendon and the remainder of the extensor mechanism were consultation. -

Evaluation of Humeral and Glenoid Bone Deformity in Glenohumeral Arthritis 5
Evaluation of Humeral and Glenoid Bone Deformity 1 in Glenohumeral Arthritis Brian F. Grogan and Charles M. Jobin Introduction glenoid bone wear helps the surgeon formulate a successful treatment plan and surgical goals Glenohumeral arthritis is the sequela of a vari- to address the pathoanatomy and improve the ety of pathologic shoulder processes, most durability of shoulder arthroplasty. The evalu- commonly degenerative osteoarthritis, but may ation of humeral and glenoid bone deformity also be secondary to post-traumatic conditions, in glenohumeral arthritis has profound surgical inflammatory arthritis, rotator cuff tear arthrop- implications and is fundamental to successful athy, and postsurgical conditions most com- shoulder arthroplasty. monly post-capsulorrhaphy arthritis. Patients with glenohumeral arthritis commonly demon- strate patterns of bony deformity on the glenoid Glenoid Deformity in Osteoarthritis and humerus that are caused by the etiology of the arthritis. For example, osteoarthritis com- Glenoid deformity and glenohumeral subluxation monly presents with posterior glenoid wear, are commonly seen in the setting of primary osteo- secondary glenoid retroversion, and posterior arthritis of the glenohumeral joint. The glenoid humeral head subluxation, while inflammatory wear tends to occur posteriorly and may be best arthritis routinely causes concentric glenoid viewed on axial radiographs or computed tomog- wear with central glenoid erosion. A thorough raphy (CT) axial images. Glenoid erosion, as first history and physical, as well as laboratory and characterized by Walch, is noted to be either central radiographic workup, are keys to understanding or posterior, with varying degrees of wear and pos- the etiology of arthritis and understanding the terior subluxation of the humerus [1, 2] (Fig. -

Peroneal Tendon Subluxation
CHAPTER 4 Peroneal Tendon Subluxation Jessica Lickiss, DPM Jay D. Ryan, DPM INTRODUCTION Peroneal tendon subluxation/ instability can be challenging IMAGING AND CLASSIFICATION to diagnose depending on the level of disruption and deformity present. Subtle cases will appear in the clinical Radiographs can be used to identify an avulsion and rule out setting similar to a lateral ankle sprain. This can cause a delay fracture. Computed tomography (CT) scan and MRI are in care and poorer outcomes for patients. both viable options for evaluation. MRI better evaluates the health of the peroneal tendons and CT scan demonstrates ANATOMY the shape and position of the fibula and fibular groove. While advanced imaging is a great adjunct, the diagnosis is mainly The peroneus longus and brevis muscle bellies travel clinical. For more subtle injuries where the tendons do not posterior to the fibula and fibular groove. At the fibular completely sublux or dislocate the fibula, dynamic ultrasound groove they are combined into one sheath; they separate can be used for diagnosing intrasheath instability (5). usually at the level of the peroneal tubercle. They are bound Eckert and Davis created a classification in 1976 for superiorly by the superior peroneal retinaculum (SPR) and SPR injuries (6). Grade I injuries involve elevation of the inferiorly by the calcaneofibular ligament (CFL) and the retinaculum from the lateral malleolus and the tendons inferior peroneal retinaculum (IPR). The superior peroneal can dislocate between the bone and periosteum. Grade II retinaculum has fibers that extend superiorly, posteriorly, injuries involve the fibrocartilaginous ridge elevating with and medially approximately 3.5 cm from the distal tip of the the retinaculum and tendon subluxed between it and the fibula (1). -
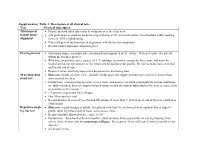
Supplementary Table 1: Description of All Clinical Tests Test Protocol
Supplementary Table 1: Description of all clinical tests Test Protocol description Tibiofemoral • Palpate & mark tibial tuberosity & midpoint over the talus neck frontal plane • Ask participant to stand on footprint map with foot at 10° external rotation, feet shoulder width, looking alignment forward, 50% weightbearing • Place callipers of inclinometer in alignment with the the two landmarks • Record varus/valgus direction in degrees Herrington test • Participant supine on plinth, knee positioned and supported in 20° of knee flexion (to place the patella within the trochlea groove) • With knee in position, place a piece of 1” Leukotape (or similar) across the knee joint, and mark the medial and lateral epicondyles of the femur and mid-point of the patella. Be sure to make note of medial and lateral end of tape • Repeat 3 times, attaching tape to this document for measuring later 30 second chair • Shoes on, middle of chair, feet ~ shoulder width apart and slightly behind knees with feet flat on floor, stand test arms crossed on chest • Instructions “stand up keeping arms across chest, and ensure you stand completely up so hips and knees are fully extended; then sit completely back down, so that the bottom fully touches the seat, as many times as possible in 30 seconds,” • 1-2 practice repetitions for technique • One 30-second test trial • Record number of correctly performed full stands (if more than ½ of way up at end of the test, counted as a full stand) Repetitive single • Shoes on, seated on edge of plinth, foot placed with heel 10 cm forward from a plumb line at edge of leg rise test plinth, other leg held at side of body, arms across chest. -

Health Policy & Clinical Effectiveness Program
Evidence-Based Care Guideline for Conservative Management of patellar instability and dislocation in children and adults aged 8-25 Guideline 44 James M. Anderson Center for Health Systems Excellence Introduction References in parentheses ( ) Evidence level in [ ] (See last page for definitions) Evidence-Based Care Guideline Lateral patellar dislocations/subluxations and lateral patellar instability are conditions that can result in short- Conservative Management of Lateral Patellar term and long-term anterior knee pain, functional Dislocations and Instability disability and potentially degenerative joint changes (Smith 2010b [1b], Fithian 2004 [2a], Atkin 2000 [3b]). Both In children and young adults aged 8-25 yearsa conditions are often managed with a non-surgical, Publication date: March 18, 2014 conservative approach that entails physical therapy care (Stefancin 2007 [1b]). While a variety of expert opinion and Target Population review articles have been published with suggestions for physical therapy interventions for lateral patellar Inclusions: Children or young adults: dislocation and patellar instability, higher level studies With history of lateral patellar dislocation, specifically investigating rehabilitation interventions for subluxation or general patellar instability in one or these conditions are limited. Consequently, optimal both knees who are going to be conservatively physical therapy strategies have not yet been determined managed (Smith 2010b [1b]). Therefore, the purpose of this guideline Ages 8-25 years is to provide a comprehensive description of evaluation and intervention strategies for conservative management Exclusions: Children or young adults: of lateral patellar instability. Following surgical patellar stabilization techniques This guideline was developed based on a synthesis of With Neuro-developmental conditions associated current evidence relative to the non- surgical, with patellar instability or dislocation (e.g. -

Two Cases of Combined Patellar Tendon Avulsion from the Tibia and Patella
SICOT-J 2018, 4,17 © The Authors, published by EDP Sciences, 2018 https://doi.org/10.1051/sicotj/2018014 Available online at: www.sicot-j.org CASE REPORT Two cases of combined patellar tendon avulsion from the tibia and patella Viachaslau Bradko1,2,*, William T. Stoll1, Lee S. Haruno1, Scott B. Rosenfeld1,2, and Scott D. McKay1,2 1 Department of Orthopaedic Surgery, Baylor College of Medicine, Houston, TX, USA 2 Division of Orthopaedic Surgery, Texas Children’s Hospital, Houston, TX, USA Received 2 October 2017, Accepted 8 April 2018, Published online 23 May 2018 Abstract- -Avulsion fractures of the inferior pole of the patella and proximal tibial apophysis are independently rare injuries. They occur in children due to the relative weakness of the apophyseal cartilage compared to the ligaments and tendons. The combination of these two fractures, is exceedingly rare, with only a few previously described cases in the literature. Due to the infrequent presentation of this injury, careful examination and consideration of advanced imaging is important for diagnosis and preoperative planning. Here we present two cases of combined sleeve fractures of the inferior pole of the patella and tibial apophysis, with discussion of the pathophysiology, classification, identification and management of the injury. Key words: Knee injuries, Bifocal avulsion, Patella, Patella tendon, Tibial tuberosity. Introduction Case description Case 1 An intense muscle contraction may result in the rupture of a muscle or tendon, or an avulsion fracture. In A 13-year-old male runner with history of contralateral contrast to adults, children are more likely to suffer from (left) patellar dislocation developed pain and inability to avulsion fractures due to the relative weakness of their bear weight in his right lower extremity following an apohyseal cartilage compared to connective tissues such as awkward landing after jumping over a hurdle.