November 19, 2018
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

OREGON RURAL HOSPITAL LISTENING TOUR: 2014 2014 RURAL HOSPITAL LISTENING TOUR FINAL REPORT 1 July 1, 2015
OREGON RURAL HOSPITAL LISTENING TOUR: 2014 2014 RURAL HOSPITAL LISTENING TOUR FINAL REPORT 1 July 1, 2015 Organized by: The Oregon Office of Rural Health Sponsored by: The Oregon Rural Healthcare Quality Network In partnership with: The Oregon Health Authority The Oregon Association of Hospitals and Health Systems The Office of Rural Health would like to acknowledge the following for their support and participation in production of this report: Max Brown, Department of Human Services Jon Collins, Oregon Health Authority: Office of Health Analytics Christopher Coon, Oregon Health Authority: Office of Health Analytics Fritz Jenkins, Oregon Health Authority: Designated State Health Programs Asante Ashland Hospital, Blue Mountain Hospital, CHI St. Anthony Hospital, Coquille Valley Hospital, Curry General Hospital, Good Shepherd Medical Center, Grande Ronde Hospital, Harney District Hospital, Lake Health District Hospital, Lower Umpqua Hospital, Mercy Medical Center, Mid-Columbia Medical Center, Peace Health Cottage Grove Hospital, Peace Health Peace Harbor Hospital, Pioneer Memorial Hospital, Providence Hood River Hospital, Samaritan North Lincoln Hospital, Samaritan Pacific Communities Hospital, Southern Coos Hospital, St. Charles Madras Hospital, St. Charles Prineville, St. Charles Redmond Hospital, Three Rivers Medical Center, Tillamook Regional Medical Center, Wallowa Memorial District Hospital, Willamette Valley Medical Center If you have any questions about this report, please contact: Oregon Office of Rural Health: Meredith Guardino|[email protected] -

2016 Recognition Targets for Hospitals
Patient Safety Reporting Program 2016 Recognition Targets for Hospitals March 2016 Recognition targets provide attainable goals for healthcare facilities participating in the Patient Safety Reporting Program (PSRP). Targets can also help facilities incrementally and effectively build adverse event review and reporting into their culture of safety. On a statewide level, targets ensure OPSC receives enough adverse event reports to build a strong database of prevention strategies so that all Oregon healthcare facilities can learn from one another. Targets are effective as of January 1, 2016. Although a participant may meet or exceed targets at any time throughout the year, the facility should continue to report adverse events according to reporting program guidelines. Healthcare facilities that meet targets are recognized annually for their transparency efforts and commitment to patient safety. For more information, visit oregonpatientsafety.org. Meet Targets Exceed Targets Quantity The number of reports submitted by a participating Submit at least the Submit at least the facility minimum quantity minimum quantity target for target for Goal: Help ensure PSRP obtains enough reports to your facility your facility build a strong database for learning. (see page 2) (see page 2) Acceptable Quality The report identifies contributing factors, root Submit at least 2 Submit 75% of causes, and system-level action plans reports that are reports with acceptable quality acceptable quality Goal: Provide enough information so that your experience can help others learn and improve. See the Guide to Quality Reporting Timeliness The amount of time that passes between discovery Submit 50% of reports of an adverse event and when a report is submitted within 45 days of to PSRP event discovery Goal: Respond immediately after an adverse event to collect full and reliable information, reduce delays, and develop strong solutions. -

Trauma Surge Plan-HPO Compress Part 1
Oregon Healthcare Preparedness Region 1 Trauma Surge Plan TRAUMA SURGE PLAN: CORE PLANNING GROUP About Us Our Mission: To assist hospitals, hospital staff, and first responders in preparing for events which overwhelm the region’s trauma system through education and the provision of resources. The outcome is the safe management and care of the critically injured, and enhancement of a seamless transition of care. Who we are: A collaborative team of experts representing the region's emergency preparedness, first responder, and trauma center leadership. Core Planning Group Members: Tanya Shanks-Connors, Legacy Health Roy Ball, Legacy Health Angela Heckathorn, Legacy Health Mark Dollar, Legacy Health Kathryn Richer, NW Oregon Health Preparedness Organization Jonathan Jui, Multnomah County Emergency Medical Services Sherrie Forsloff, Oregon Health & Science University Mercedes Wilson, Oregon Health & Science University Acknowledgements This was truly a multi-discipline, multi-agency, multi-jurisdiction, and multi-year effort. Its success is due to our many partners in contributing agencies, as well as funders. We express our deep gratitude to the following for their support: o Clackamas County Emergency Management o Legacy Health o Multnomah County Emergency Management o Multnomah County Emergency Medical Services o NW Oregon Health Preparedness Organization o Oregon Health Authority o Oregon Health Science & University o Regional Disaster Preparedness Organization o U.S Department of Health and Human Services o Washington County Emergency Management For further information, or to contact a member of the Core Planning Group please go to our Hospital Emergency Preparedness website at: hospitalemergencypreparedness.org Oregon Healthcare Preparedness Region 1 | Trauma Surge Plan 1 | P a g e Table of Contents Introduction ................................................................................................................................................. -

Oregon COVID-19 Weekly Report
Informe semanal de COVID-19 Resumen de vigilancia semanal de Oregón Nuevo coronavirus (COVID-19) División de Salud Pública de Oregón Publicado el 9 de diciembre de 2020 Antecedentes Los datos del Informe semanal de COVID-19 se concluirán todos los domingos a las 11 p. m., hora de verano del Pacífico, y el informe se publicará el miércoles. Tenga en cuenta que los datos informados aquí se están actualizando continuamente. Para obtener información actualizada a diario, visite el sitio web sobre COVID-19 de la Autoridad de Salud de Oregón (Oregon Health Authority, OHA): https://govstatus.egov.com/OR-OHA-COVID-19. Hasta las 11 p. m. del domingo, 6 de diciembre, hubo 85,788 casos de COVID-19 informados a la Autoridad de Salud de Oregón. De estos, 3,741 (4.4 %) son casos “presuntos”, digamos personas que tienen síntomas compatibles con COVID-19 y contacto cercano con un caso confirmado, pero no tuvieron una prueba de laboratorio que lo confirme. Aunque no están confirmados, los casos presuntos muy probablemente tengan COVID-19, debido a los síntomas específicos y a la exposición conocida. Se les recomienda a los casos presuntos que se realicen pruebas de detección para confirmar si tienen COVID-19. Los casos presuntos que obtengan un resultado positivo se recategorizan a casos confirmados. Estos datos representan una visión global de los factores de riesgo de COVID-19, características clínicas y demográficas de los casos e incluyen datos sobre casos con exámenes complementarios pendientes. No se ha entrevistado a todos los casos al momento del presente informe. -

Impact of Policies on Rural Communities Oregon
Impact of Policies on Rural Communities Oregon Sequestration2 Bad Debt Reimbursement Cut3 2% Inpatient and Outpatient Medicare Revenue Cut 35% Medicare Bad Debt Reimburesment Cut Provider Operating Annual Potential Job Potential GDP Annual Potential Job Potential GDP Provider Name/Number 1 Type Margin 1 Revenue Lost 1 Loss 4 Loss 5 Revenue Lost Loss 4 Loss 5 Bay Area Hospital (380090) RPPS 5.1% $1,402,674 21 $2,694,287 $335,951 5 $645,302 Blue Mountain Hospital (381305) CAH 12.4% $103,038 2 $230,097 $22,265 0 $49,721 CHI St. Anthony Hospital (381319) CAH 14.1% $295,649 4 $570,912 $62,980 1 $121,616 Columbia Memorial Hospital (381320) CAH 13.3% $536,031 9 $1,188,408 $312,917 5 $693,753 Coquille Valley Hospital (381312) CAH -1.0% $221,858 3 $409,956 $18,291 0 $33,799 Curry General Hospital (381322) CAH -0.2% $285,231 5 $630,182 $100,353 2 $221,718 Good Shepherd Health Care System (381325) CAH 4.5% $425,575 7 $923,659 $62,123 1 $134,829 Grande Ronde Hospital (381321) CAH 3.6% $445,021 7 $879,693 $167,414 3 $330,936 Harney District Hospital (381307) CAH -1.8% $103,560 2 $240,129 $17,862 0 $41,417 Lake District Hospital (381309) CAH 0.3% $120,338 3 $338,664 $11,533 0 $32,456 Lower Umpqua Hospital District (381311) CAH -5.8% $121,920 2 $285,842 $68,875 1 $161,478 Mercy Medical Center (380027) RPPS 16.5% $1,187,722 20 $2,610,228 $101,817 2 $223,760 Mid-Columbia Medical Center (380001) RPPS 3.2% $477,045 9 $1,109,291 $139,303 3 $323,927 PeaceHealth Cottage Grove Community Medical Center CAH 19.4% $237,056 4 $483,247 $87,272 1 $177,907 (381301) 1 CMS Healthcare Cost Report Information System (HCRIS) Q1 2020. -

Beacon Name Changing to Affinity
September 30, 2016 Dear Provider, A few months ago we sent you some information and an attestation of acknowledgement that the Beacon network name will be changing to the Affinity network for the 2017 plan year. With 2017 open enrollment beginning in November, we want to make sure you are aware of changes to Moda’s Beacon Network, which is available to individuals purchasing health coverage directly from Moda or through the federal marketplace exchange. For plans effective January 1, 2017, the Beacon Network name in your area will change to the Affinity Network. The Beacon Network will continue to serve members in select Western Oregon counties. The Affinity Network will be available to individual members residing in the following counties: Baker Morrow Gilliam Sherman Grant Umatilla Harney Union Lake Wallowa Malheur Wheeler Affinity is designed to ensure members find the care they need, when they need it, Affinity helps members looking for customized care that fits their individual lifestyle and budget, and find the care they need, when they need it. With Affinity, members have access to a large selection of providers including Blue Mountain Hospital District, Good Shepherd, Grande Ronde Hospital, Harney District Hospital, Lake District Hospital, Pioneer Memorial Hospital (Heppner), St. Alphonsus Baker City, St. Alphonsus Ontario, and Wallowa Memorial Hospital. Although the Affinity name is new, we don’t expect any changes to your current workflow. Reimbursement, referrals to in-network providers, prior authorizations and processes will be the same. Individuals choosing plans supported by the Affinity network will be asked to select a primary care physician (PCP) to coordinate care. -

City of Salem Natural Hazards Mitigation Plan
City of Salem Natural Hazards Mitigation Plan Photo Credits Gary Halvorson, Oregon State Archives September 2017 Volume I: Basic Plan Prepared for: City of Salem Emergency Management June 2015 Final Report Prepared by: University of Oregon Community Service Center Oregon Partnership for Disaster Resilience June 2015 Final Report June 2015 Final Report June 2015 Final Report This Natural Hazard Mitigation Plan was prepared by: With support from: Planning grant funding provided by: Federal Emergency Management Agency (FEMA) Pre-Disaster Mitigation Program Grant: EMS-2014-PC-0011 Sub-grant Application Reference: PDMC-PL-10-OR-2014-002 Additional Support Provided by: This material is a result of tax-supported research and, as such, is not copyrightable. It may be freely reprinted with the customary crediting of the source. SPECIAL THANKS & ACKNOWLEDGEMENTS City of Salem developed this Natural Hazards Mitigation Plan (NHMP) through a regional partnership funded by the Federal Emergency Management Agency’s (FEMA) Pre-Disaster Mitigation (PDM) Competitive Grant Program: EMS-2014-PC-0011, Sub-grant Application Reference: PDMC-PL-10-OR-2014-002. The city utilized a four-phased planning process, plan templates and plan development support provided by the Oregon Partnership for Disaster Resilience (OPDR) at the University of Oregon’s Community Service Center. Special thanks to Roger Stevenson, City of Salem Emergency Manager for his leadership in convening the committee. City of Salem NHMP Update Steering Committee • Convener, Roger Stevenson, City -

Umatilla &Morrow
Safe Kids Oregon 2012 State Report Dear Child Safety Advocates, Injury prevention efforts continue to make a difference to Oregon’s children. Between 2005-2007 and 2009-2011 deaths to children ages 0 – 14 from unintentional injuries decreased by 18.9% (from 148 to 120) and hospitalizations decreased by 17.3% (from 3,539 to 3,214). The important injury prevention messages and events hosted by Safe Kids Coalitions and partners throughout communities in 2012 continue to help families make safe INSIDE THIS REPORT: choices. This report details the extensive work of Safe Kids Oregon and the eight coalitions and three chapters in Introduction 1-3 Oregon. Please take a moment to read about our efforts. Prevention Activity Statewide 4-6 2012 was a year of transition for Safe Kids Oregon. I wish Motor Vehicle Occupant Safety to thank Adrienne Greene for her support as she moved Pedestrian Safety into her role as CDC Grant Manager and Tam Peterson for Bicycle and Wheeled Sports Safety her valuable training in website maintenance and Suffocation Prevention and Safe newsletter design. Additionally, the Safe Kids Oregon Sleep Advisory Board has been very active and involved in Fire and Burn Prevention providing guidance to Safe Kids Oregon. Fall Prevention Water Safety Sports Safety Ruth Harshfield Safe Kids Oregon Director Chapters & Coalitions 7 - 18 Safe Kids Oregon Safe Kids Central Oregon Safe Kids Columbia County Safe Kid Columbia Gorge Safe Kids Harney County Safe Kids Malheur County A MESSAGE FROM Safe Kids Portland Metro Safe Kids Rogue Valley KAREN GUNSON, MD ~ Safe Kids Umatilla/Morrow Counties HONORARY CHAIR Safe Kids Union County Safe Kids Washington County The work of Safe Kids Oregon continues to be important. -

Oregon's Acute Care Hospitals
OREGON’S ACUTE CARE HOSPITALS Capacity, Utilization, and Financial Trends 2009 - 2011 June 2013 Oregon Health Authority Office of Health Analytics Oregon’s Acute Care Hospitals, 2009 - 2011 Oregon’s Acute Care Hospitals Capacity, Utilization and Financial Trends 2009-2011 June 2013 Prepared by: The Oregon Health Authority, Office of Health Analytics http://www.oregon.gov/OHA/OHPR/RSCH Tina Edlund Chief of Policy Gretchen Morley Director of Health Analytics Russell Voth Health System Research and Data Manager Mark Whitaker Senior Financial Policy Analyst Paulos Sanna Research Analyst Steven Ranzoni Research Analyst Shawna Kennedy Research Assistant Oregon Health Authority, Office of Health Analytics Oregon’s Acute Care Hospitals, 2009 - 2011 TABLE OF CONTENTS Contents Executive Summary ______________________________________________________________________________________ 1 Chapter 1: Background __________________________________________________________________________________ 3 Hospital Reimbursement Classifications ________________________________________________________________________3 Overall Trends _____________________________________________________________________________________________________8 Hospital Ownership _____________________________________________________________________________________________ 12 Chapter 2: Hospital Capacity ___________________________________________________________________________ 13 Bed Capacity _____________________________________________________________________________________________________ -
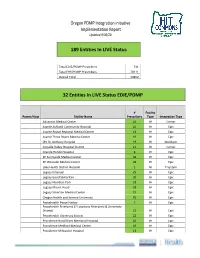
157 Entities in LIVE Status EHR/PDMP
Oregon PDMP Integration initiative Implementation Report Updated 9/30/20 189 Entities In LIVE Status Total EDIE/PDMP Prescribers 741 Total EHR/PDMP Prescribers 20111 Overall Total 20852 32 Entities In LIVE Status EDIE/PDMP # Facility Parent/Host Facility Name Prescribers Type Integration Type Adventist Medical Center 26 IH Cerner Asante Ashland Community Hospital 10 IH Epic Asante Rogue Regional Medical Center 41 IH Epic Asante Three Rivers Medical Center 19 IH Epic CHI St. Anthony Hospital 19 IH Meditech Coquille Valley Hospital District 12 IH Cerner Grande Ronde Hospital 8 IH Epic KP Sunnyside Medical Center 36 IH Epic KP Westside Medical Center 36 IH Epic Lake Health District Hospital 5 IH T-System Legacy Emanuel 25 IH Epic Legacy Good Samaritan 30 IH Epic Legacy Meridian Park 18 IH Epic Legacy Mount Hood 28 IH Epic Legacy Silverton Medical Center 15 IH Epic Oregon Health and Science University 70 IH Epic Peacehealth Peace Harbor 7 IH Epic Peacehealth Riverbend (2 Locations Riverbend & University District) 22 IH Epic Peacehealth University District 22 IH Epic Providence Hood River Memorial Hospital 10 IH Epic Providence Medford Medical Center 19 IH Epic Providence Milwaukie Hospital 13 IH Epic # Facility Parent/Host Facility Name Prescribers Type Integration Type Providence Newberg Hospital 26 IH Epic Providence Portland Medical Center 43 IH Epic Providence Seaside Hospital 7 IH Epic Providence St Vincent Medical Center 47 IH Epic Providence Willamette Falls Medical Center 12 IH Epic Salem Hospital 42 IH Epic Sky Lakes Medical Center -

Majoris Health Systems MCO Provider Directory
Majoris Health Systems, Inc. Employee Information and Medical Provider and Facilities DIRECTORY May 2021 R-2031 Majoris Health Systems, Inc. ________________________________________________________________________________________________________ SAIF Corporation, has contracted with Majoris Am I required to see one of the Majoris doctors Health Systems, Inc., a state-certified managed if I am injured on the job and need medical care organization (MCO) to provide services to care? employees injured on the job. In most cases, yes. Once your claim is “enrolled” We understand that dealing with an injury can with Majoris Health Systems, (which means you sometimes be stressful and confusing. We have been given written notice of your therefore recommend that you become familiar requirement to treat within the MCO) you will be with the Majoris procedures before you may need required to treat with an MCO provider unless to seek care for a work-related injury or illness. one of the circumstances explained below applies. Following are answers to some of the more commonly-asked questions concerning our The situations in which you may receive managed care program. Should you have compensable care from a non-Majoris provider additional questions, please feel free to contact after your claim is enrolled are as follows: SAIF Corporation at 800.285.8525, or Majoris 1. You have a private physician, Health Systems directly at 800.525.0394. chiropractic physician, or nurse practitioner who qualifies as a primary What is Majoris Health Systems? care physician, chiropractic physician Majoris is a state-certified managed care or authorized nurse practitioner. organization that contracts with physicians, Your family physician, chiropractic physician, hospitals, and other health care providers to or authorized nurse practitioner may qualify to provide medical services to covered employees treat you under the managed care with work-related injuries or illnesses. -

COVID-19 Relief Funds Grant Recipients
COVID-19 Relief Funds Grant Recipients Oregon Small Business Relief Fund Awards Business Oregon released the latest of the state's recovery efforts for Oregon small businesses suffering in the wake of the COVID-19 pandemic—funding to stand up local small business grant programs across the state. The Oregon Legislature and Governor Kate Brown allocated $5 million from the state's General Fund, which we combined with another $5 million redirected from existing programs at Business Oregon. Round 1—eligible applicants are cities, counties, and economic development districts that have existing small business COVID-relief programs or will stand up new programs to issue grants to local small businesses. Round 2—eligible applicants are community development financial institutions (CDFIs) and economic development districts (EDDs). Round 3—eligible applicants are cities, counties, and Economic Development Districts (EDDs). Applicant Region Award Round COIC Central $167,500 1 CCD (Coos, Curry, Douglas) Coast $115,000 1 Clatsop County (CEDR) Coast $120,000 1 Lincoln County Coast $120,000 1 City of Wheeler Coast $10,000 1 Grant County Eastern $70,000 1 La Grande Eastern $65,000 1 Ontario Eastern $65,000 1 Pendleton Eastern $65,000 1 City of Umatilla Eastern $50,000 1 City of Union Eastern $20,000 1 Wallowa County Eastern $30,000 1 Beaverton Portland Metro $35,000 1 Clackamas County Portland Metro $45,000 1 Fairview Portland Metro $15,000 1 Gladstone Portland Metro $35,000 1 Gresham Portland Metro $35,000 1 Happy Valley Portland Metro $35,000 1 Hillsboro