Urethral Syndrome in Women
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Mimickers of Urothelial Carcinoma and the Approach to Differential Diagnosis
Review Mimickers of Urothelial Carcinoma and the Approach to Differential Diagnosis Claudia Manini 1, Javier C. Angulo 2,3 and José I. López 4,* 1 Department of Pathology, San Giovanni Bosco Hospital, 10154 Turin, Italy; [email protected] 2 Clinical Department, Faculty of Medical Sciences, European University of Madrid, 28907 Getafe, Spain; [email protected] 3 Department of Urology, University Hospital of Getafe, 28905 Getafe, Spain 4 Department of Pathology, Cruces University Hospital, Biocruces-Bizkaia Health Research Institute, 48903 Barakaldo, Spain * Correspondence: [email protected]; Tel.: +34-94-600-6084 Received: 17 December 2020; Accepted: 18 February 2021; Published: 25 February 2021 Abstract: A broad spectrum of lesions, including hyperplastic, metaplastic, inflammatory, infectious, and reactive, may mimic cancer all along the urinary tract. This narrative collects most of them from a clinical and pathologic perspective, offering urologists and general pathologists their most salient definitory features. Together with classical, well-known, entities such as urothelial papillomas (conventional (UP) and inverted (IUP)), nephrogenic adenoma (NA), polypoid cystitis (PC), fibroepithelial polyp (FP), prostatic-type polyp (PP), verumontanum cyst (VC), xanthogranulomatous inflammation (XI), reactive changes secondary to BCG instillations (BCGitis), schistosomiasis (SC), keratinizing desquamative squamous metaplasia (KSM), post-radiation changes (PRC), vaginal-type metaplasia (VM), endocervicosis (EC)/endometriosis (EM) (müllerianosis), -

A New Look at the Etiology of Interstitial Cystitis/Bladder Pain Syndrome: Extraordinary Cultivations
International Urology and Nephrology (2019) 51:1961–1967 https://doi.org/10.1007/s11255-019-02248-5 UROLOGY - ORIGINAL PAPER A new look at the etiology of interstitial cystitis/bladder pain syndrome: extraordinary cultivations Tahsin Batuhan Aydogan1 · Oznur Gurpinar2 · Ozgen Koseoglu Eser2 · Begum Aydogan Mathyk3 · Ali Ergen1 Received: 25 April 2019 / Accepted: 24 July 2019 / Published online: 30 July 2019 © Springer Nature B.V. 2019 Abstract Purpose So far, studies have not clearly identifed infectious agents as an etiological factor for interstitial cystitis (IC). Spe- cifc microbiological diagnosis for detecting the pathogen with higher sensitivity in IC may decrease the treatment costs and increase psychosocial health of the patients. Methods A prospective clinical study was performed in 26 IC patients and 20 controls between April and September 2017. All participants were asked to give mid-stream urine sample for routine urine cultures. Followed by the negative results, symptomatic 26 patients were evaluated for L-form pathogen existence by extraordinary cultivation methods. Biopsy sam- ples were taken from 19 patients with ulcerative lesions in the bladder while collecting sterile urine samples from all 26 patients. PG broth, 5% sheep blood agar, EMB, Sabouraud’s dextrose, LEM, and GYPA were used. Followed by the 1st day inoculations, all inoculated PG broths were subcultured into the same solid media at the 2nd and 10th days in case of any growth after incubation of 24 h under 35–37 °C. The “O’Leary Sant Symptom and Problem Index” score forms were used to evaluate response to the appropriate treatment for those patients with documented pathogens. -

Interstitial Cystitis/Painful Bladder Syndrome
What I need to know about Interstitial Cystitis/Painful Bladder Syndrome U.S. Department of Health and Human Services National Kidney and Urologic Diseases NATIONAL INSTITUTES OF HEALTH Information Clearinghouse What I need to know about Interstitial Cystitis/Painful Bladder Syndrome U.S. Department of Health and Human Services National Kidney and Urologic Diseases NATIONAL INSTITUTES OF HEALTH Information Clearinghouse Contents What is interstitial cystitis/painful bladder syndrome (IC/PBS)? ............................................... 1 What are the signs of a bladder problem? ............ 2 What causes bladder problems? ............................ 3 Who gets IC/PBS? ................................................... 4 What tests will my doctor use for diagnosis of IC/PBS? ............................................................... 5 What treatments can help IC/PBS? ....................... 7 Points to Remember ............................................. 14 Hope through Research........................................ 15 Pronunciation Guide ............................................. 16 For More Information .......................................... 17 Acknowledgments ................................................. 18 What is interstitial cystitis/painful bladder syndrome (IC/PBS)? Interstitial cystitis*/painful bladder syndrome (IC/PBS) is one of several conditions that causes bladder pain and a need to urinate frequently and urgently. Some doctors have started using the term bladder pain syndrome (BPS) to describe this condition. Your bladder is a balloon-shaped organ where your body holds urine. When you have a bladder problem, you may notice certain signs or symptoms. *See page 16 for tips on how to say the words in bold type. 1 What are the signs of a bladder problem? Signs of bladder problems include ● Urgency. The feeling that you need to go right now! Urgency is normal if you haven’t been near a bathroom for a few hours or if you have been drinking a lot of fluids. -
Symptoms of Overactive Bladder and Interstitial Cystitis – How Different?
183 Homma Y1, Tanaka M1, Niimi A1 1. Japan Red Cross Medical Centre SYMPTOMS OF OVERACTIVE BLADDER AND INTERSTITIAL CYSTITIS – HOW DIFFERENT? Hypothesis / aims of study Overactive bladder (OAB) is a symptom syndrome of urgency, frequency or urgency incontinence [1]. Interstitial cystitis (IC) is a bladder disease with a symptom syndrome of urgency, frequency, or bladder pain. Difference in symptoms of these confusable disorders is to be examined. Study design, materials and methods Female patients with OAB or IC and asymptomatic controls were recruited for the study. Diagnosis of OAB is based on 1) OAB symptom score [2] larger than 5 and/or urgency incontinence, and 2) exclusion of stress urinary incontinence and other obvious diseases. IC was diagnosed by 1) O’Leary & Sant’s symptom score [3] larger than 7 and/or bladder pain, 2) exclusion of other obvious diseases, and 3) Hunner’s ulcer or bladder bleeding at hydrodistension under anesthesia. The subjects recorded, in 3-day bladder diary, time voided, voided volume and intensity (0: none, 1: slightly, 2: moderately, 3: a lot) of 6 sensations or symptoms (urge to void, fear of leakage, amount of leakage, bladder discomfort, bladder pain and feeling of incomplete emptying) for each micturition. Additionally the urge questionnaire of 5 questions addressing the conditions during the last week was administered: 1) Did you feel urge to void that was not followed by voiding? (Response: yes, no), 2) Did you feel strong urge to void? (yes, no), 3) In case of yes in question 2, did you feel strong urge to void suddenly? (yes, no), 4) What happened or might happen, if you held strong urge to void for a long time, 1 hour for example ? (Response: leak urine, feel discomfort and/or pain, both), 5) In case of discomfort and/or pain in question 4, could you tell these 2 sensations apart? (yes, no). -
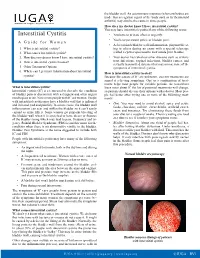
Interstitial Cystitis? You May Have Interstitial Cystitis If Any of the Following Occur: Interstitial Cystitis • You Have to Urinate Often Or Urgently
the bladder wall. An autoimmune response (when antibodies are made that act against a part of the body such as in rheumatoid arthritis) may also be the cause in some people. How does my doctor know I have interstitial cystitis? You may have interstitial cystitis if any of the following occur: Interstitial Cystitis • You have to urinate often or urgently. • You have persistent pelvic or bladder pain. A Guide for Women • A doctor finds bladder wall inflammation, pinpoint bleed- 1. What is interstitial cystitis? ing or ulcers during an exam with a special telescope 2. What causes interstitial cystitis? (called a cystoscope) used to look inside your bladder. 3. How does my doctor know I have interstitial cystitis? • Your doctor has ruled out other diseases such as urinary 4. How is interstitial cystitis treated? tract infections, vaginal infections, bladder cancer, and sexually transmitted diseases that may mimic some of the 5. Other Treatment Options symptoms of interstitial cystitis. 6. Where can I get more information about interstitial How is interstitial cystitis treated? cystitis? Because the causes of IC are unknown, current treatments are aimed at relieving symptoms. One or a combination of treat- ments helps most people for variable periods. As researchers What is interstitial cystitis? learn more about IC the list of potential treatments will change, Interstitial cystitis (IC) is a term used to describe the condition so patients should discuss their options with a doctor. Most peo- of bladder pain or discomfort with a frequent and often urgent ple feel better after trying one or more of the following treat- need to pass urine. -

Lesions of the Female Urethra: a Review
Please do not remove this page Lesions of the Female Urethra: a Review Heller, Debra https://scholarship.libraries.rutgers.edu/discovery/delivery/01RUT_INST:ResearchRepository/12643401980004646?l#13643527750004646 Heller, D. (2015). Lesions of the Female Urethra: a Review. In Journal of Gynecologic Surgery (Vol. 31, Issue 4, pp. 189–197). Rutgers University. https://doi.org/10.7282/T3DB8439 This work is protected by copyright. You are free to use this resource, with proper attribution, for research and educational purposes. Other uses, such as reproduction or publication, may require the permission of the copyright holder. Downloaded On 2021/09/29 23:15:18 -0400 Heller DS Lesions of the Female Urethra: a Review Debra S. Heller, MD From the Department of Pathology & Laboratory Medicine, Rutgers-New Jersey Medical School, Newark, NJ Address Correspondence to: Debra S. Heller, MD Dept of Pathology-UH/E158 Rutgers-New Jersey Medical School 185 South Orange Ave Newark, NJ, 07103 Tel 973-972-0751 Fax 973-972-5724 [email protected] There are no conflicts of interest. The entire manuscript was conceived of and written by the author. Word count 3754 1 Heller DS Precis: Lesions of the female urethra are reviewed. Key words: Female, urethral neoplasms, urethral lesions 2 Heller DS Abstract: Objectives: The female urethra may become involved by a variety of conditions, which may be challenging to providers who treat women. Mass-like urethral lesions need to be distinguished from other lesions arising from the anterior(ventral) vagina. Methods: A literature review was conducted. A Medline search was used, using the terms urethral neoplasms, urethral diseases, and female. -

Case Report Pseudomembranous Trigonitis in a Male with Klinefelter Syndrome: a Case Report and Evidence of a Hormonal Etiology
Int J Clin Exp Pathol 2014;7(6):3375-3379 www.ijcep.com /ISSN:1936-2625/IJCEP0000435 Case Report Pseudomembranous trigonitis in a male with Klinefelter syndrome: a case report and evidence of a hormonal etiology Derrick WQ Lian1, Fay X Li2, Caroline CP Ong2, CH Kuick1, Kenneth TE Chang1 Departments of 1Pathology and Laboratory Medicine, 2Paediatric Surgery, KK Women’s and Children’s Hospital, Singapore Received April 6, 2014; Accepted May 26, 2014; Epub May 15, 2014; Published June 1, 2014 Abstract: Klinefelter syndrome is a clinical syndrome with a distinct 47, XXY karyotype. Patients are characterized by a tall eunuchoid stature, small testes, hypergonotrophic hypogonadism, gynecomastia, learning difficulties and infertility. These patients have also been found to have raised estrogen levels. We report a 16 year old boy with Kline- felter syndrome presenting to our institution with gross hematuria. Cystoscopy and biopsy revealed the diagnosis of pseudomembranous trigonitis. Immunohistochemical stains showed an increase in estrogen and progesterone receptors in the trigone area but not in the rest of the bladder. In view of the patient’s mildly raised estrogen levels and the histological findings, we postulate that estrogen is the driver of the development of pseudomembranous trigonitis. This is the first reported case of pseudomembranous trigonitis seen in association with Klinefelter syn- drome, and also the first case of pseudomembranous trigonitis occurring within the male adolescent age group. Keywords: Klinefelter syndrome, pseudomembranous trigonitis, pediatric Introduction with a sense of incomplete voiding. These epi- sodes were initially treated with a course of oral Klinefelter syndrome is the most common chro- antibiotics by a primary care physician with no mosomal aberration in males and the most resolution of symptoms. -

Associated Diseases in Interstitial Cystitis/Bladder Pain Syndrome
Associated diseases in interstitial cystitis/bladder pain syndrome Joop P. van de Merwe [email protected] Associated diseases in IC/BPS patients Table 1. Examples of associated disorders diagnosed in IC/BPS patients in comparison with Associated diseases are diseases that occur more often the general population 2,5,6 together in the same person than by chance. Associated diseases for IC/BPS (interstitial cystitis/bladder pain diagnosis prevalence (%) syndrome) include allergy, fibromyalgia, irritable bowel IC/BPS general syndrome, Crohn's disease, ulcerative colitis, systemic lupus population erythematosus, rheumatoid arthritis and Sjögren's syndrome allergy 40.6 22.5 (table 1). irritable bowel syndrome 25.4 2.9 sensitive skin 22.6 10.6 Allergy vulvodynia 10.9 15.0 An allergy occurs when a person's immune system causes an fibromyalgia 12.8 3.2 adverse reaction to substances in the environment that are chronic fatigue syndrome 7.7 8.5 harmless to most other people. These substances (so-called migraine 18.8 18.0 allergens) are found in dust mites, pets, pollen, insects, ticks, asthma 9.2 6.1 15 moulds, foods and many medications. Adverse reactions Crohn’s disease/ulcerative colitis 7.3 0.07 without involvement of the immune system are called rheumatoid arthritis 4-13 1.0 intolerance. Intolerance mainly occurs to food ingredients and systemic lupus erythematosus 1.7 0.05 drugs. Sjögren’s syndrome 8.0 0.5 People experience different symptoms, depending on the allergen, the individual's immune system, previous contact with the same allergen and where it enters the body. -

Interstitial Cystitis
DIAGNOSIS AND TREATMENT OF INTERSTITIAL CYSTITIS Women with interstitial cystitis (IC) often feel the need to urinate frequently WHAT IS INTERSTITIAL in addition to experiencing painful urination even though bladder infection CYSTITIS (PAINFUL is not the cause. For many women IC interrupts their normal daily activities BLADDER SYNDROME)? because of the need to stay close to a bathroom and a constant feeling of discomfort. Interstitial cystitis (IC), also DIAGNOSING INTERSTITIAL CYSTITIS known as painful bladder Chesapeake Urology’s pelvic health specialists will run a series of diagnostic syndrome, is a chronic tests for other conditions that cause the same symptoms as IC and come to infl ammatory condition a diagnosis once all other causes are ruled out. Our experienced physicians of the bladder lining that perform a comprehensive physical exam and may order additional tests including: causes pain and pressure • Urine analysis and urine culture in the pelvic area around • Cystoscopy with bladder distention the bladder. • Biopsy of the bladder • CT scan of the bladder IC affects approximately • Urodynamic testing eight million young and middle-aged women in the HOW IS IC TREATED? U.S. While there is no cure for IC, treatments can provide relief from painful symptoms. Our physicians provide several different therapies that have Symptoms of IC can been shown to alleviate and/or diminish many of the symptoms of IC include: including: • Pain in the bladder • Physical therapy – As a treatment for underlying pelvic fl oor dysfunction, physical -

CLEVELAND AMBULATORY SURGERY CENTER DELINEATION of CLINICAL PRIVILEGES Urology Applicant’S Signature Date
CLEVELAND AMBULATORY SURGERY CENTER DELINEATION OF CLINICAL PRIVILEGES Urology Applicant’s Signature Date The granting, reviewing and changing of clinical privileges will be in accordance with the Medical Staff Bylaws. Assignment of such clinical privileges must be based upon education, clinical training, demonstrated skills and capacity to manage procedurally related complications. Indicate procedures for which you do and do not wish to be credentialed. Return this form with your Application. Recommendation by Procedures Credentialing Request QM Committee Yes No Yes No Hernia hydrocele repair Repair inguinal hernia w/orchiectomy Repair inguinal hernia w/excision of hydrocele Repair inguinal hernia, recurrent Repair inguinal hernia, sliding Repair ventral hernia Repair ventral hernia, recurrent Repair unbilical hernia, age 5 or over Drain perineal abscess Cath or stent ureter Injection for pyelography thru cath Injection procedure for pyelography Change nephrostomy tube Renal endoscopy thru established nephrostomy Renal endoscopy w/fulguration and/or excision Injection ureterography thru cath Injection vis ileal conduit Ureteral endoscopy w/ureteral cath Ureteral endoscopy w/biopsy Fulguration prostate Urethrotomy pendulous urethra Urethrotomy perineal urethra Meatotomy Meatotomy infant Drainage deep periurethral abscess Excision or fulguration carcinoma urethra Excision urethral diverticulum female Excision urethral diverticulum male Marsup urethral caruncle Excision urethral caruncle Excision urethral prolapse Page 1 of 5 MS2O DELINEATION -

Neuro-Urology for the Urogynaecologist and Urologist W42, 30 August 2011 14:00 - 18:00
Neuro-urology for the Urogynaecologist and Urologist W42, 30 August 2011 14:00 - 18:00 Start End Topic Speakers 14:00 14:05 Introduction to the Workshop Sohier Suzy Elneil 14:05 14:25 Neurology of the bladder and the pelvic floor Thomas Kessler 14:25 14:45 Bladder Symptoms in the Neurological Patient Xavier Game 14:45 15:05 Pelvic Floor Dysfunction in the Neurological Patient Alex Digesu 15:05 15:20 Bladder and Pelvic Floor Assement in Neurogenic Xavier Game Bladder and Pelvic Floor Dysfunction 15:20 15:30 Discussion All 15:30 16:00 Break None 16:00 16:25 Indications and Limitations of Botulinum Toxin in Rizwan Hamid Neurogenic Bladder 16:25 16:50 Indications and Limitations of Botulinum toxin in the Sohier Suzy Elneil Pelvic Floor 16:50 17:10 Discussion All 17:10 17:25 Indications and Limitations of Neuromodulation Alex Digesu (PTNS) in Neurogenic Bladder and Pelvic Floor Disorders 17:25 17:45 Indications and Limitations of Neuromodulation Sohier Suzy Elneil (SNM) in Neurogenic Bladder and Pelvic Floor Thomas Kessler Disorders 17:45 18:00 Discussion All Aims of course/workshop Aims and Objectives: -Current concepts relating to the neurogical control of the bladder and the pelvic floor. -Urinary and pelvic floor symptoms in patients with cerebral leisons, multiple sclerosis, Parkinson's disease, spinal cord injury and cauda equina -Urinary and pelvic floor symptoms in bladder pain syndrome/IC and chronic pelvic pain syndromes (neurological basis of disease). -Investigating neurogenic bladder and pelvic floor dysfunction -Innovative therapies in treating neurogenic bladder and pelvic floor disorders: Indications and limitations of botulinum toxin -Innovative therapies in treating neurogenic bladder and pelvic floor disorders:Indications and limitations of neuromodulation Educational Objectives This workshop will provide a fresh approach to the understanding of the neurological basis of bladder and pelvic floor conditions encountered in urogynaecology and urology. -

Underlying Causes of Chronic Bladder Dysfunction
South African Family Practice 2018; 60(2):24-27 S Afr Fam Pract Open Access article distributed under the terms of the ISSN 2078-6190 EISSN 2078-6204 Creative Commons License [CC BY-NC-ND 4.0] © 2018 The Author(s) http://creativecommons.org/licenses/by-nc-nd/4.0 REVIEW Underlying causes of chronic bladder dysfunction Andre Marais,1 Senior lecturer and Clinical Pharmacologist, Elzbieta Osuch,2 Professor and Clinical Pharmacologist 1Department of Pharmacology, School of Medicine, Faculty of Health Sciences, University of Pretoria, South Africa 2Department of Pharmacology& Therapeutics, School of Medicine, Sefako Makghato Health Sciences University, South Africa Corresponding author, email: [email protected] / [email protected] Abstract General practitioners and family physicians frequently encounter patients suffering from voiding disorders. Various underlying causes such as spinal cord injury, cerebrovascular accidents, traumatic brain injury and several neurological diseases including Parkinson’s disease, dementia, multiple sclerosis and vitamin deficiencies have been implicated. Chronic bladder conditions may cause social embarrassment and decrease quality of life in affected individuals. It is important to identify the most common underlying causes of bladder dysfunction and have adequate knowledge regarding the primary treatment and prevention of complications in order to reduce the economic burden created by this group of disorders. Keywords: Chronic bladder conditions; interstitial cystitis; painful bladder syndrome; chronic