Abbreviations - Diagnosis
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Selecting Different Approaches for Palate and Pharynx Surgery
SPECIAL ISSUE 4: INVITED ARTICLE Selecting Different Approaches for Palate and Pharynx Surgery: Palatopharyngeal Arch Staging System Rodolfo Lugo-Saldaña1 , Karina Saldívar-Ponce2 , Irina González-Sáez3 , Daniela Hernández-Sirit4 , Patricia Mireles-García5 ABSTRACT The examination of the anatomical structures involved in the upper airway collapse in patients with the obstructive sleep apnea-hypopnea syndrome (OSAHS) is a key for integrated evaluation of patients. Our proposal is for a noninvasive classification system that guides us about the presence of anatomical differences between the palatopharyngeal muscle (PFM). The functions of the PFM are narrowing the isthmus, descending the palate, and raising the larynx during swallowing; these characteristics give the PFM a special role in the collapse of the lateral pharyngeal wall. Complete knowledge of the anatomy and classification of different variants can guide us to choose the appropriate surgical procedures for the lateral wall collapse. Until now there is not a consensus about description of the trajectory or anatomical variants of the PFM into oropharynx, the distance between both muscles, and the muscle tone. Here we also present the relationship between the lateral wall surgeries currently available (lateral pharyngoplasty by Cahali, expansion sphincteroplasty by Pang, relocation pharyngoplasty by Li, Roman blinds pharyngoplasty by Mantovani, and barbed sutures pharyngoplasty by Vicini) with the proposed classification of the palatopharyngeal arch staging system (PASS). Keywords: -

Lecture 2 – Bone
Oral Histology Summary Notes Enoch Ng Lecture 2 – Bone - Protection of brain, lungs, other internal organs - Structural support for heart, lungs, and marrow - Attachment sites for muscles - Mineral reservoir for calcium (99% of body’s) and phosphorous (85% of body’s) - Trap for dangerous minerals (ex:// lead) - Transduction of sound - Endocrine organ (osteocalcin regulates insulin signaling, glucose metabolism, and fat mass) Structure - Compact/Cortical o Diaphysis of long bone, “envelope” of cuboid bones (vertebrae) o 10% porosity, 70-80% calcified (4x mass of trabecular bone) o Protective, subject to bending/torsion/compressive forces o Has Haversian system structure - Trabecular/Cancellous o Metaphysis and epiphysis of long bone, cuboid bone o 3D branching lattice formed along areas of mechanical stress o 50-90% porosity, 15-25% calcified (1/4 mass of compact bone) o High surface area high cellular activity (has marrow) o Metabolic turnover 8x greater than cortical bone o Subject to compressive forces o Trabeculae lined with endosteum (contains osteoprogenitors, osteoblasts, osteoclasts) - Woven Bone o Immature/primitive, rapidly growing . Normally – embryos, newborns, fracture calluses, metaphyseal region of bone . Abnormally – tumors, osteogenesis imperfecta, Pagetic bone o Disorganized, no uniform orientation of collagen fibers, coarse fibers, cells randomly arranged, varying mineral content, isotropic mechanical behavior (behavior the same no matter direction of applied force) - Lamellar Bone o Mature bone, remodeling of woven -

Vestibule Lingual Frenulum Tongue Hyoid Bone Trachea (A) Soft Palate
Mouth (oral cavity) Parotid gland Tongue Sublingual gland Salivary Submandibular glands gland Esophagus Pharynx Stomach Pancreas (Spleen) Liver Gallbladder Transverse colon Duodenum Descending colon Small Jejunum Ascending colon intestine Ileum Large Cecum intestine Sigmoid colon Rectum Appendix Anus Anal canal © 2018 Pearson Education, Inc. 1 Nasopharynx Hard palate Soft palate Oral cavity Uvula Lips (labia) Palatine tonsil Vestibule Lingual tonsil Oropharynx Lingual frenulum Epiglottis Tongue Laryngopharynx Hyoid bone Esophagus Trachea (a) © 2018 Pearson Education, Inc. 2 Upper lip Gingivae Hard palate (gums) Soft palate Uvula Palatine tonsil Oropharynx Tongue (b) © 2018 Pearson Education, Inc. 3 Nasopharynx Hard palate Soft palate Oral cavity Uvula Lips (labia) Palatine tonsil Vestibule Lingual tonsil Oropharynx Lingual frenulum Epiglottis Tongue Laryngopharynx Hyoid bone Esophagus Trachea (a) © 2018 Pearson Education, Inc. 4 Visceral peritoneum Intrinsic nerve plexuses • Myenteric nerve plexus • Submucosal nerve plexus Submucosal glands Mucosa • Surface epithelium • Lamina propria • Muscle layer Submucosa Muscularis externa • Longitudinal muscle layer • Circular muscle layer Serosa (visceral peritoneum) Nerve Gland in Lumen Artery mucosa Mesentery Vein Duct oF gland Lymphoid tissue outside alimentary canal © 2018 Pearson Education, Inc. 5 Diaphragm Falciform ligament Lesser Liver omentum Spleen Pancreas Gallbladder Stomach Duodenum Visceral peritoneum Transverse colon Greater omentum Mesenteries Parietal peritoneum Small intestine Peritoneal cavity Uterus Large intestine Cecum Rectum Anus Urinary bladder (a) (b) © 2018 Pearson Education, Inc. 6 Cardia Fundus Esophagus Muscularis Serosa externa • Longitudinal layer • Circular layer • Oblique layer Body Lesser Rugae curvature of Pylorus mucosa Greater curvature Duodenum Pyloric Pyloric sphincter antrum (a) (valve) © 2018 Pearson Education, Inc. 7 Fundus Body Rugae of mucosa Pyloric Pyloric (b) sphincter antrum © 2018 Pearson Education, Inc. -

Basic Histology (23 Questions): Oral Histology (16 Questions
Board Question Breakdown (Anatomic Sciences section) The Anatomic Sciences portion of part I of the Dental Board exams consists of 100 test items. They are broken up into the following distribution: Gross Anatomy (50 questions): Head - 28 questions broken down in this fashion: - Oral cavity - 6 questions - Extraoral structures - 12 questions - Osteology - 6 questions - TMJ and muscles of mastication - 4 questions Neck - 5 questions Upper Limb - 3 questions Thoracic cavity - 5 questions Abdominopelvic cavity - 2 questions Neuroanatomy (CNS, ANS +) - 7 questions Basic Histology (23 questions): Ultrastructure (cell organelles) - 4 questions Basic tissues - 4 questions Bone, cartilage & joints - 3 questions Lymphatic & circulatory systems - 3 questions Endocrine system - 2 questions Respiratory system - 1 question Gastrointestinal system - 3 questions Genitouirinary systems - (reproductive & urinary) 2 questions Integument - 1 question Oral Histology (16 questions): Tooth & supporting structures - 9 questions Soft oral tissues (including dentin) - 5 questions Temporomandibular joint - 2 questions Developmental Biology (11 questions): Osteogenesis (bone formation) - 2 questions Tooth development, eruption & movement - 4 questions General embryology - 2 questions 2 National Board Part 1: Review questions for histology/oral histology (Answers follow at the end) 1. Normally most of the circulating white blood cells are a. basophilic leukocytes b. monocytes c. lymphocytes d. eosinophilic leukocytes e. neutrophilic leukocytes 2. Blood platelets are products of a. osteoclasts b. basophils c. red blood cells d. plasma cells e. megakaryocytes 3. Bacteria are frequently ingested by a. neutrophilic leukocytes b. basophilic leukocytes c. mast cells d. small lymphocytes e. fibrocytes 4. It is believed that worn out red cells are normally destroyed in the spleen by a. neutrophils b. -

Oral-Peripheral Examination
Oral-Peripheral Examination SCSD 632 Week 2 Phonological Disorders 3. General Cautions Relating to the Oral-Peripheral Examination a. Use your initial impressions of the child’s speech and facial characteristics to guide your examination. b. Remember that one facial or oral abnormality may be associated with others. c. If you suspect an abnormality in structure or function you may want to get a second opinion from a more experienced SLP or an SLP who specializes in craniofacial or motor-speech disorders before initiating referrals to other professionals. d. Remember that in the case of most “special” conditions, it is not your role to diagnose the condition; rather it is your responsibility to make appropriate referrals. e. Remember that in Canada you cannot usually refer directly to a specialist; be sensitive in your approach to the family doctor or referring physician. f. Be sensitive about how you present your results to parents, especially when you are recommending referrals to other professionals. The parents have the right to refuse the referral. g. An oral-peripheral examination is at least as important for your young patients as for your older patients. 1 Oral-Peripheral Examination | Oral and Facial Structure z Face z Lips z Teeth z Hard palate z Soft palate z Tongue When you perform an oral-peripheral examination what are you looking for when you examine each of the following structures? a. Facial Characteristics: overall expression and appearance, size, shape and overall symmetry of the head and facial structures b. Teeth: maxillary central incisors should extend just slightly over the mandibular central incisors; the lower canine tooth should be half-way between the upper lateral incisor and the upper canine tooth c. -

Pharyngeal Flap
Cincinnati Children’s Hospital Medical Center Craniofacial Center and VPI Clinic Pharyngeal Flap What is Velopharyngeal Insufficiency (VPI)? During normal speech, the soft palate (also called velum) raises and closes against the back wall of the throat (also called pharynx or pharyngeal wall). This closes off the nose from the mouth for speech. If the soft palate is not long enough to firmly close against the back of the throat during speech, sound and air can leak into the nose through the gap. This condition is called velopharyngeal insufficiency (VPI). VPI can affect resonance, which is the quality of the voice. The voice may sound hypernasal because there is too much sound in the nose during speech. (Hyponasality is the opposite problem. It is due to blockage in the nose and occurs when the person has a bad cold.) VPI can also affect speech sound production. The child may not have enough air pressure in the mouth to make certain speech sounds. Also, a leak of air through the nose may be heard during speech. To correct VPI for normal speech, the opening between the nose and mouth must be closed. The Furlow Z-plasty can correct VPI, particularly for children with a history of cleft palate or submucous cleft (where the muscles under the skin of the soft palate have not come together properly). Procedure: The pharyngeal flap is done by taking a flap of tissue from the back of the throat (pharyngeal wall) and attaching it to the soft palate (velum). This flap forms a “bridge” to close the gap between the back of the throat and the soft palate. -

Giant Sialolith at Sublingual Salivary Gland. Biggest? 4
CASE REPORT Journal of Dentomaxillofacial Science (J Dentomaxillofac Sci ) August 2018, Volume 3, Number 2: 123-125 P-ISSN.2503-0817, E-ISSN.2503-0825 Giant sialolith at sublingual salivary gland. Biggest? Case Report Abul Fauzi,* Irfan Rasul CrossMark http://dx.doi.org/10.15562/jdmfs.v3i2.704 Abstract Objective: Sialoliths or salivary gland duct calculus are the most (sialolithotomy) was planned intraorally with sialodochoplasty under Month: April common pathologies of the salivary gland. The majority of sialoliths general anesthesia. occur in the submandibular gland or its duct and are a common cause Results: CBCT and intra operation obtained the stone in the wharton’s of acute and chronic infections. Sialoliths are deposits obstructing the duct with 26.5 mm in length and 17 mm in diameter. Volume No.: 3 ducts of major or minor salivary glands. Conclusion: The main complaint of sialolithiasis is pain accompanied Methods: Clinical and radiographic examination panoramic and by swelling. The therapy that can be done for this sialolith is divided CBCT was conducted and the diagnosis is sialolithiasis on salivary into conventional techniques without surgery, surgical therapy and Issue: 2 ducts sublingual gland sinistra and removal of salivary glands stone therapy with Extracorporeal Shock Wave Lithotripter (ECSWL) techniques. Keywords: Giant sialolith, Sublingual salivary gland First page No.: 87 Cite this Article: Fauzi A, Rasul I. 2018. Giant sialolith at sublingual salivary gland. Biggest?. Journal of Dentomaxillofacial Science 3(2): 123-125. DOI: 10.15562/jdmfs.v3i2.704 P-ISSN.2503-0817 Department of Oral and Introduction the mouth that has been occured since the pre- Maxilllofacial Surgery, Faculty of vious 3 months. -

Absence of Uvula: an Accidental Or an Incidental Finding. J Human Anat
Journal of Human Anatomy ISSN: 2578-5079 Is Uvula Important? Absence of Uvula: An Accidental or an Incidental Finding 1 2 3 4 Vivek J *, Safeer K , Sanjib D and Bhargavi Joshi 1Department of Biochemistry & Basic sciences, Kentucky College of Osteopathic Case Report Volume 3 Issue 2 Medicine, USA Received Date: September 12, 2019 2Department of Anatomy & Embryology, Windsor University School of Published Date: October 21, 2019 Medicine, Saint Kitts and Nevis DOI: 10.23880/jhua-16000142 3Department of Pharmacology, Govt Medical College, Ratlam, India 4Research Volunteer, Windsor University School of Medicine, St Kitts and Nevis *Corresponding author: Vivek Joshi, MD, Associate Professor Biochemistry, Department of Basic Science, Kentucky College of Osteopathic Medicine, 147 Sycamore Street, Hambley Blvd, University of Pikeville (UPike), Pikeville, KY, 41501, USA, Tel : 606-218-5552; Email: [email protected] Abstract Introduction: Absence of the uvula is very rare in the general population, which is mostly acquired secondary to surgery or is rarely congenitally absent since birth. Uvula is a small band of connective tissue, gland and small muscle fibers and is documented to be useful in speech, lubrication and central support of the palatopharyngeal arch during swallowing. Cultural practice of uvulectomy is very common in African countries as a treatment or prophylactic measure for chronic cough or frequent respiratory infection. Congenital absence of uvula is a rare condition and is also accompanied by other genetic abnormalities such as cleft lip or cleft palate. Case Report: This case report is based on an accidental finding in a 20-year-old African-American male who was acting as a standardized patient in a clinical course at a medical college. -

Uvula in Snoring and Obstructive Sleep Apnea: Role and Surgical Intervention
Opinion American Journal of Otolaryngology and Head and Neck Surgery Published: 13 Apr, 2020 Uvula in Snoring and Obstructive Sleep Apnea: Role and Surgical Intervention Elbassiouny AM* Department of Otolaryngology, Cairo University, Egypt Abstract Objective: Currently, the consideration of the enlarged uvula as a cause of snoring and Obstructive Sleep Apnea (OSA) lacks data for objective interpretation. This article focused on some concepts on how we can manage the enlarged uvula in cases of snoring and OSA. The purpose of the present article is to discuss the cost benefits of uvular surgery versus its preservation. Conclusion: The direct correlation between the uvula and OSA needs to be reevaluated to maintain a balance between reserving its anatomical and physiological functions and surgically manipulating it as a part of palatopharyngeal surgery, yet further objective studies are needed to reach optimal results. Keywords: Uvula; Snoring; Obstructive sleep apnea Introduction The palatine uvula, usually referred to as simply the uvula, is that part of the soft palate that has an anatomical structure and serves some functions. Anatomically, the uvula, a conic projection from the back edge of the middle of the soft palate, is composed of connective tissue containing several racemose glands, and some muscular fibers, musculus uvulae muscle; arises from the posterior nasal spine and the palatine aponeurosis and inserts into the mucous membrane of the uvula. It contains many serous glands, which produce thin saliva [1]. Physiologically, the uvula serves several functions. First during swallowing, the soft palate and the uvula move together to close off the nasopharynx OPEN ACCESS and prevent food from entering the nasal cavity. -

Anatomy and Physiology of the Velopharyngeal Mechanism
Anatomy and Physiology of the Velopharyngeal Mechanism Jamie L. Perry, Ph.D.1 ABSTRACT Understanding the normal anatomy and physiology of the velopharyngeal mechanism is the first step in providing appropriate diagnosis and treatment for children born with cleft lip and palate. The velopharyngeal mechanism consists of a muscular valve that extends from the posterior surface of the hard palate (roof of mouth) to the posterior pharyngeal wall and includes the velum (soft palate), lateral pharyngeal walls (sides of the throat), and the posterior pharyngeal wall (back wall of the throat). The function of the velopharyngeal mechanism is to create a tight seal between the velum and pharyngeal walls to separate the oral and nasal cavities for various purposes, including speech. Velopharyngeal closure is accomplished through the contraction of several velopharyngeal muscles including the levator veli palatini, musculus uvulae, superior pharyngeal con- strictor, palatopharyngeus, palatoglossus, and salpingopharyngeus. The tensor veli palatini is thought to be responsible for eustachian tube function. KEYWORDS: Anatomy, physiology, velopharyngeal muscles, cleft palate anatomy Downloaded by: SASLHA. Copyrighted material. Learning Outcomes: As a result of this activity, the reader will be able to (1) list the major muscles of the velopharyngeal mechanism and discuss their functions; (2) list the sensory and motor innervation patterns for the muscles of the velopharyngeal mechanism; and (3) discuss the variations in velopharyngeal anatomy found in an unrepaired cleft palate. Understanding the normal anatomy and and treatment for children born with cleft lip physiology of the velopharyngeal mechanism is and palate. Most of the diagnostic and therapy the first step in providing appropriate diagnosis approaches are based on a strong foundation of 1Department of Communication Sciences and Disorders, Guest Editor, Ann W. -
PE1706 Early Speech Development in Children with Cleft Palate
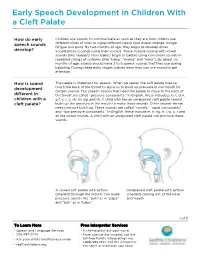
Early Speech Development in Children With a Cleft Palate How do early Children use sounds to communicate as soon as they are born. Infants use speech sounds different kinds of cries to signal different needs (like diaper change, hunger, fatigue and pain). By two months of age, they begin to develop other develop? vocalizations (sounds using their voices). These include cooing with vowel sounds (like “aaaaa”). Next babies begin to babble using consonant sounds in repeated strings of syllables (like “baba,” “mama” and “nana”). By about six months of age, a baby should have 2 to 5 speech sounds that they use during babbling. During these early stages, babies learn they can use sound to get attention. How is sound The palate is important for speech. When we speak, the soft palate rises to development touch the back of the throat to allow us to build up pressure in our mouth for certain sounds. The speech sounds that need the palate to close to the back of different in the throat are called “pressure consonants.” In English, these include p, b, t, d, k, children with a g f, v, s, z, sh, ch, dg, and th. A child who has an unrepaired cleft palate cannot cleft palate? build up the pressure in the mouth to make these sounds. Other sounds do not need pressure build-up. These sounds are called “vowels,” “nasal consonants” and “low pressure consonants.” In English, these include m, n, ng, h, l, w, y, r and all the vowel sounds. A child with an unrepaired cleft palate can produce these sounds. -

Soft Palate and Its Motor Innervation: a Brief Review
Review Article Anatomy Physiol Biochem Int J Volume 5 Issue 4 - April 2019 Copyright © All rights are reserved by Liancai Mu DOI: 10.19080/APBIJ.2019.05.555672 Soft Palate and Its Motor Innervation: A Brief Review Liancai Mu1*, Jingming Chen1, Jing Li1, Stanislaw Sobotka1,2 and Mary Fowkes3 1Department of Biomedical Research, Upper Airway Research Laboratory, Hackensack University Medical Center, USA 2Department of Neurosurgery, Icahn School of Medicine at Mount Sinai, USA 3Department of Pathology, Icahn School of Medicine at Mount Sinai, USA Submission: March 29, 2019; Published: April 18, 2019 *Corresponding author: Liancai Mu, MD, Ph.D, Upper Airway Research Laboratory, Department of Biomedical Research, Hackensack University Medical Center, 40 Prospect Avenue, Hackensack, NJ, 07601, USA Abstract Human soft palate plays an important role in upper airway functions such as speech, swallowing and respiration. However, neural control of the soft palate is poorly understood because innervation of this structure has long been controversial. In this review, the inconsistent and even contradictory observations regarding the motor innervation of the palatal muscles are summarized. We emphasize to use Sihler’s stain for documenting the nerves and their supply patterns within individual palatal muscles as studies have demonstrated that Sihler’s stain permits mapping of entire nerve supply within organs, skeletal muscles, mucosa, skin, and other structures. This wholemount nerve staining has unique advantage over other anatomical methods as all the nerves within the muscles processed with Sihler’s stain can be visualized in their 3-dimensional positions. Advanced knowledge of the neural organization of the soft palate is critical for a better understanding of its functions and for the development of novel neuromodulation therapies to treat soft palate-related upper airway disorders such as obstructive sleep apnea.