Title TRP Channels As Sensors of Oxygen Availability. Author(S)
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Transient Receptor Potential Channel Promiscuity Frustrates Constellation
the sole sensor responsible for noxious cold responses in M+A+ LETTER neurons (1). However, TRPA1 is also activated by cooling and underlies at least part of the noxious cold responsiveness of Transient receptor potential channel AITC-sensitive neurons (3). Third, the authors used nicardipine 2+ promiscuity frustrates to selectively inhibit CaV1-type voltage-gated Ca channels (1). However, several dihydropyridines, including nicardipine, also constellation pharmacology act as TRPA1 agonists (4). These considerations led us to propose an alternative Sensory neurons from the trigeminal and dorsal root ganglia molecular interpretation of the difference between M+A− (DRG) have nerve endings in the skin and mucosa, where they and M+A+ neurons, which is in much better agreement with detect environmental stimuli and convey this information to published work. In accord with the authors, we conclude that the central nervous system. Several members of the transient M+A− neurons express TRPM8 but lack expression of receptor potential (TRP) superfamily of ion channels act as TRPA1. In contrast to the authors, we propose that M+A+ prime molecular sensors for thermal and chemical stimuli in neurons express TRPA1 as the prime cold and menthol these sensory neurons. However, it is incompletely understood sensor (2, 3). This interpretation is consistent with published how TRP channel expression and modulation affect the stimulus observations that menthol responses in M+A− but not in sensitivities of distinct neuronal subtypes. M+A+ neurons are inhibited by TRPM8 antagonists (5) In a recent article, Teichert et al. (1) described a “constellation and that TRPA1-mediated responses to cold in neurons are pharmacology approach” to identify and characterize subtypes characterized by a higher (colder) threshold (3). -

Single-Particle Cryo-EM of the Ryanodine Receptor Channel in an Aqueous Environment
Single-particle cryo-EM of the ryanodine receptor channel Eur J Transl Myol - Basic Appl Myol 2015; 25 (1): 35-48 Single-particle cryo-EM of the ryanodine receptor channel in an aqueous environment Mariah R. Baker, Guizhen Fan and Irina I. Serysheva Department of Biochemistry and Molecular Biology, The University of Texas Medical School at Houston, 6431 Fannin Street, Houston, TX 77030, USA Abstract Ryanodine receptors (RyRs) are tetrameric ligand-gated Ca2+ release channels that are responsible for the increase of cytosolic Ca2+ concentration leading to muscle contraction. Our current understanding of RyR channel gating and regulation is greatly limited due to the lack of a high-resolution structure of the channel protein. The enormous size and unwieldy shape of Ca2+ release channels make X-ray or NMR methods difficult to apply for high-resolution structural analysis of the full-length functional channel. Single-particle electron cryo- microscopy (cryo-EM) is one of the only effective techniques for the study of such a large integral membrane protein and its molecular interactions. Despite recent developments in cryo- EM technologies and break-through single-particle cryo-EM studies of ion channels, cryospecimen preparation, particularly the presence of detergent in the buffer, remains the main impediment to obtaining atomic-resolution structures of ion channels and a multitude of other integral membrane protein complexes. In this review we will discuss properties of several detergents that have been successfully utilized in cryo-EM studies of ion channels and the emergence of the detergent alternative amphipol to stabilize ion channels for structure- function characterization. Future structural studies of challenging specimen like ion channels are likely to be facilitated by cryo-EM amenable detergents or alternative surfactants. -

Chapter Four – TRPA1 Channels: Chemical and Temperature Sensitivity
CHAPTER FOUR TRPA1 Channels: Chemical and Temperature Sensitivity Willem J. Laursen1,2, Sviatoslav N. Bagriantsev1,* and Elena O. Gracheva1,2,* 1Department of Cellular and Molecular Physiology, Yale University School of Medicine, New Haven, CT, USA 2Program in Cellular Neuroscience, Neurodegeneration and Repair, Yale University School of Medicine, New Haven, CT, USA *Corresponding author: E-mail: [email protected], [email protected] Contents 1. Introduction 90 2. Activation and Regulation of TRPA1 by Chemical Compounds 91 2.1 Chemical activation of TRPA1 by covalent modification 91 2.2 Noncovalent activation of TRPA1 97 2.3 Receptor-operated activation of TRPA1 99 3. Temperature Sensitivity of TRPA1 101 3.1 TRPA1 in mammals 101 3.2 TRPA1 in insects and worms 103 3.3 TRPA1 in fish, birds, reptiles, and amphibians 103 3.4 TRPA1: Molecular mechanism of temperature sensitivity 104 Acknowledgments 107 References 107 Abstract Transient receptor potential ankyrin 1 (TRPA1) is a polymodal excitatory ion channel found in sensory neurons of different organisms, ranging from worms to humans. Since its discovery as an uncharacterized transmembrane protein in human fibroblasts, TRPA1 has become one of the most intensively studied ion channels. Its function has been linked to regulation of heat and cold perception, mechanosensitivity, hearing, inflam- mation, pain, circadian rhythms, chemoreception, and other processes. Some of these proposed functions remain controversial, while others have gathered considerable experimental support. A truly polymodal ion channel, TRPA1 is activated by various stimuli, including electrophilic chemicals, oxygen, temperature, and mechanical force, yet the molecular mechanism of TRPA1 gating remains obscure. In this review, we discuss recent advances in the understanding of TRPA1 physiology, pharmacology, and molecular function. -

Minding the Calcium Store: Ryanodine Receptor Activation As a Convergent Mechanism of PCB Toxicity
Pharmacology & Therapeutics 125 (2010) 260–285 Contents lists available at ScienceDirect Pharmacology & Therapeutics journal homepage: www.elsevier.com/locate/pharmthera Associate Editor: Carey Pope Minding the calcium store: Ryanodine receptor activation as a convergent mechanism of PCB toxicity Isaac N. Pessah ⁎, Gennady Cherednichenko, Pamela J. Lein Department of Molecular Biosciences, School of Veterinary Medicine, University of California, Davis, CA 95616, USA article info abstract Keywords: Chronic low-level polychlorinated biphenyl (PCB) exposures remain a significant public health concern since Ryanodine receptor (RyR) results from epidemiological studies indicate that PCB burden is associated with immune system Calcium-induced calcium release dysfunction, cardiovascular disease, and impairment of the developing nervous system. Of these various Calcium regulation adverse health effects, developmental neurotoxicity has emerged as a particularly vulnerable endpoint in Polychlorinated biphenyls PCB toxicity. Arguably the most pervasive biological effects of PCBs could be mediated by their ability to alter Triclosan fi 2+ Bastadins the spatial and temporal delity of Ca signals through one or more receptor-mediated processes. This Polybrominated diphenylethers review will focus on our current knowledge of the structure and function of ryanodine receptors (RyRs) in Developmental neurotoxicity muscle and nerve cells and how PCBs and related non-coplanar structures alter these functions. The Activity dependent plasticity molecular and cellular mechanisms by which non-coplanar PCBs and related structures alter local and global Ca2+ signaling properties and the possible short and long-term consequences of these perturbations on neurodevelopment and neurodegeneration are reviewed. © 2009 Elsevier Inc. All rights reserved. Contents 1. Introduction ............................................... 260 2. Ryanodine receptor macromolecular complexes: significance to polychlorinated biphenyl-mediated Ca2+ dysregulation . -

Comparative Genomic Analysis of Integral Membrane Transport Proteins in Ciliates
UC San Diego UC San Diego Previously Published Works Title Comparative genomic analysis of integral membrane transport proteins in ciliates. Permalink https://escholarship.org/uc/item/3g98s19z Journal The Journal of eukaryotic microbiology, 62(2) ISSN 1066-5234 Authors Kumar, Ujjwal Saier, Milton H Publication Date 2015-03-01 DOI 10.1111/jeu.12156 Peer reviewed eScholarship.org Powered by the California Digital Library University of California The Journal of Published by the International Society of Eukaryotic Microbiology Protistologists Journal of Eukaryotic Microbiology ISSN 1066-5234 ORIGINAL ARTICLE Comparative Genomic Analysis of Integral Membrane Transport Proteins in Ciliates Ujjwal Kumar & Milton H. Saier Jr Division of Biological Sciences, University of California at San Diego, La Jolla, California Keywords ABSTRACT Channels; evolution; genome analyses; secondary carriers. Integral membrane transport proteins homologous to those found in the Transporter Classification Database (TCDB; www.tcdb.org) were identified and Correspondence bioinformatically characterized by transporter class, family, and substrate speci- M. H. Saier Jr, Division of Biological ficity in three ciliates, Paramecium tetraurelia (Para), Tetrahymena thermophila Sciences, University of California at San (Tetra), and Ichthyophthirius multifiliis (Ich). In these three organisms, 1,326 of Diego, La Jolla, CA 92093-0116, USA 39,600 proteins (3.4%), 1,017 of 24,800 proteins (4.2%), and 504 out of 8,100 Telephone number: +858-534-4084; proteins (6.2%) integral membrane transport proteins were identified, respec- FAX number: +858-534-7108; tively. Thus, an inverse relationship was observed between the % transporters e-mail: [email protected] identified and the number of total proteins per genome reported. -

TRPM8 Channels and Dry Eye
UC Berkeley UC Berkeley Previously Published Works Title TRPM8 Channels and Dry Eye. Permalink https://escholarship.org/uc/item/2gz2d8s3 Journal Pharmaceuticals (Basel, Switzerland), 11(4) ISSN 1424-8247 Authors Yang, Jee Myung Wei, Edward T Kim, Seong Jin et al. Publication Date 2018-11-15 DOI 10.3390/ph11040125 Peer reviewed eScholarship.org Powered by the California Digital Library University of California pharmaceuticals Review TRPM8 Channels and Dry Eye Jee Myung Yang 1,2 , Edward T. Wei 3, Seong Jin Kim 4 and Kyung Chul Yoon 1,* 1 Department of Ophthalmology, Chonnam National University Medical School and Hospital, Gwangju 61469, Korea; [email protected] 2 Graduate School of Medical Science and Engineering, Korea Advanced Institute of Science and Technology, Daejeon 34141, Korea 3 School of Public Health, University of California, Berkeley, CA 94720, USA; [email protected] 4 Department of Dermatology, Chonnam National University Medical School and Hospital, Gwangju 61469, Korea; [email protected] * Correspondence: [email protected] Received: 17 September 2018; Accepted: 12 November 2018; Published: 15 November 2018 Abstract: Transient receptor potential (TRP) channels transduce signals of chemical irritation and temperature change from the ocular surface to the brain. Dry eye disease (DED) is a multifactorial disorder wherein the eyes react to trivial stimuli with abnormal sensations, such as dryness, blurring, presence of foreign body, discomfort, irritation, and pain. There is increasing evidence of TRP channel dysfunction (i.e., TRPV1 and TRPM8) in DED pathophysiology. Here, we review some of this literature and discuss one strategy on how to manage DED using a TRPM8 agonist. -

Investigational Drugs in Early Phase Clinical Trials Targeting Thermotransient Receptor Potential (Thermotrp) Channels
Expert Opinion on Investigational Drugs ISSN: (Print) (Online) Journal homepage: https://www.tandfonline.com/loi/ieid20 Investigational drugs in early phase clinical trials targeting thermotransient receptor potential (thermoTRP) channels Asia Fernández-Carvajal , Rosario González-Muñiz , Gregorio Fernández- Ballester & Antonio Ferrer-Montiel To cite this article: Asia Fernández-Carvajal , Rosario González-Muñiz , Gregorio Fernández- Ballester & Antonio Ferrer-Montiel (2020): Investigational drugs in early phase clinical trials targeting thermotransient receptor potential (thermoTRP) channels, Expert Opinion on Investigational Drugs, DOI: 10.1080/13543784.2020.1825680 To link to this article: https://doi.org/10.1080/13543784.2020.1825680 Published online: 29 Sep 2020. Submit your article to this journal Article views: 31 View related articles View Crossmark data Full Terms & Conditions of access and use can be found at https://www.tandfonline.com/action/journalInformation?journalCode=ieid20 EXPERT OPINION ON INVESTIGATIONAL DRUGS https://doi.org/10.1080/13543784.2020.1825680 REVIEW Investigational drugs in early phase clinical trials targeting thermotransient receptor potential (thermoTRP) channels Asia Fernández-Carvajala, Rosario González-Muñizb, Gregorio Fernández-Ballestera and Antonio Ferrer-Montiela aInstituto De Investigación, Desarrollo E Innovación En Biotecnología Sanitaria De Elche (Idibe), Universitas Miguel Hernández, Alicante, Spain; bInstituto De Química Médica, CSIC, Madrid, Spain ABSTRACT ARTICLE HISTORY Introduction: Thermo transient receptor potential (thermoTRP) channels are some of the most inten Received 15 June 2020 sely pursued therapeutic targets of the past decade. They are considered promising targets of numer Accepted 15 September ous diseases including chronic pain and cancer. Modulators of these proteins, in particular TRPV1-4, 2020 TRPM8 and TRPA1, have reached clinical development, but none has been approved for clinical practice KEYWORDS yet. -

New Natural Agonists of the Transient Receptor Potential Ankyrin 1 (TRPA1
www.nature.com/scientificreports OPEN New natural agonists of the transient receptor potential Ankyrin 1 (TRPA1) channel Coline Legrand, Jenny Meylan Merlini, Carole de Senarclens‑Bezençon & Stéphanie Michlig* The transient receptor potential (TRP) channels family are cationic channels involved in various physiological processes as pain, infammation, metabolism, swallowing function, gut motility, thermoregulation or adipogenesis. In the oral cavity, TRP channels are involved in chemesthesis, the sensory chemical transduction of spicy ingredients. Among them, TRPA1 is activated by natural molecules producing pungent, tingling or irritating sensations during their consumption. TRPA1 can be activated by diferent chemicals found in plants or spices such as the electrophiles isothiocyanates, thiosulfnates or unsaturated aldehydes. TRPA1 has been as well associated to various physiological mechanisms like gut motility, infammation or pain. Cinnamaldehyde, its well known potent agonist from cinnamon, is reported to impact metabolism and exert anti-obesity and anti-hyperglycemic efects. Recently, a structurally similar molecule to cinnamaldehyde, cuminaldehyde was shown to possess anti-obesity and anti-hyperglycemic efect as well. We hypothesized that both cinnamaldehyde and cuminaldehyde might exert this metabolic efects through TRPA1 activation and evaluated the impact of cuminaldehyde on TRPA1. The results presented here show that cuminaldehyde activates TRPA1 as well. Additionally, a new natural agonist of TRPA1, tiglic aldehyde, was identifed -
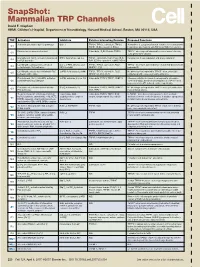
Snapshot: Mammalian TRP Channels David E
SnapShot: Mammalian TRP Channels David E. Clapham HHMI, Children’s Hospital, Department of Neurobiology, Harvard Medical School, Boston, MA 02115, USA TRP Activators Inhibitors Putative Interacting Proteins Proposed Functions Activation potentiated by PLC pathways Gd, La TRPC4, TRPC5, calmodulin, TRPC3, Homodimer is a purported stretch-sensitive ion channel; form C1 TRPP1, IP3Rs, caveolin-1, PMCA heteromeric ion channels with TRPC4 or TRPC5 in neurons -/- Pheromone receptor mechanism? Calmodulin, IP3R3, Enkurin, TRPC6 TRPC2 mice respond abnormally to urine-based olfactory C2 cues; pheromone sensing 2+ Diacylglycerol, [Ca ]I, activation potentiated BTP2, flufenamate, Gd, La TRPC1, calmodulin, PLCβ, PLCγ, IP3R, Potential role in vasoregulation and airway regulation C3 by PLC pathways RyR, SERCA, caveolin-1, αSNAP, NCX1 La (100 µM), calmidazolium, activation [Ca2+] , 2-APB, niflumic acid, TRPC1, TRPC5, calmodulin, PLCβ, TRPC4-/- mice have abnormalities in endothelial-based vessel C4 i potentiated by PLC pathways DIDS, La (mM) NHERF1, IP3R permeability La (100 µM), activation potentiated by PLC 2-APB, flufenamate, La (mM) TRPC1, TRPC4, calmodulin, PLCβ, No phenotype yet reported in TRPC5-/- mice; potentially C5 pathways, nitric oxide NHERF1/2, ZO-1, IP3R regulates growth cones and neurite extension 2+ Diacylglycerol, [Ca ]I, 20-HETE, activation 2-APB, amiloride, Cd, La, Gd Calmodulin, TRPC3, TRPC7, FKBP12 Missense mutation in human focal segmental glomerulo- C6 potentiated by PLC pathways sclerosis (FSGS); abnormal vasoregulation in TRPC6-/- -

Ca Signaling in Cardiac Fibroblasts and Fibrosis-Associated Heart
Journal of Cardiovascular Development and Disease Review Ca2+ Signaling in Cardiac Fibroblasts and Fibrosis-Associated Heart Diseases Jianlin Feng 1, Maria K. Armillei 1, Albert S. Yu 1, Bruce T. Liang 1, Loren W. Runnels 2,* and Lixia Yue 1,* 1 Calhoun Cardiology Center, Department of Cell Biology, University of Connecticut Health Center, Farmington, CT 06030, USA; [email protected] (J.F.); [email protected] (M.K.A.); [email protected] (A.S.Y.); [email protected] (B.T.L.) 2 Department of Pharmacology, Rutgers, Robert Wood Johnson Medical School, Piscataway, NJ 08854, USA * Correspondence: [email protected] (L.W.R.); [email protected] (L.Y.) Received: 11 August 2019; Accepted: 18 September 2019; Published: 23 September 2019 Abstract: Cardiac fibrosis is the excessive deposition of extracellular matrix proteins by cardiac fibroblasts and myofibroblasts, and is a hallmark feature of most heart diseases, including arrhythmia, hypertrophy, and heart failure. This maladaptive process occurs in response to a variety of stimuli, including myocardial injury, inflammation, and mechanical overload. There are multiple signaling pathways and various cell types that influence the fibrogenesis cascade. Fibroblasts and myofibroblasts are central effectors. Although it is clear that Ca2+ signaling plays a vital role in this pathological process, what contributes to Ca2+ signaling in fibroblasts and myofibroblasts is still not wholly understood, chiefly because of the large and diverse number of receptors, transporters, and ion channels that influence intracellular Ca2+ signaling. Intracellular Ca2+ signals are generated by Ca2+ release from intracellular Ca2+ stores and by Ca2+ entry through a multitude of Ca2+-permeable ion channels in the plasma membrane. -

Preclinical Model Systems of Ryanodine Receptor 1-Related Myopathies and Malignant Hyperthermia
Lawal et al. Orphanet Journal of Rare Diseases (2020) 15:113 https://doi.org/10.1186/s13023-020-01384-x REVIEW Open Access Preclinical model systems of ryanodine receptor 1-related myopathies and malignant hyperthermia: a comprehensive scoping review of works published 1990– 2019 Tokunbor A. Lawal1, Emily S. Wires2, Nancy L. Terry3, James J. Dowling4 and Joshua J. Todd1* Abstract Background: Pathogenic variations in the gene encoding the skeletal muscle ryanodine receptor (RyR1) are associated with malignant hyperthermia (MH) susceptibility, a life-threatening hypermetabolic condition and RYR1- related myopathies (RYR1-RM), a spectrum of rare neuromuscular disorders. In RYR1-RM, intracellular calcium dysregulation, post-translational modifications, and decreased protein expression lead to a heterogenous clinical presentation including proximal muscle weakness, contractures, scoliosis, respiratory insufficiency, and ophthalmoplegia. Preclinical model systems of RYR1-RM and MH have been developed to better understand underlying pathomechanisms and test potential therapeutics. Methods: We conducted a comprehensive scoping review of scientific literature pertaining to RYR1-RM and MH preclinical model systems in accordance with the PRISMA Scoping Reviews Checklist and the framework proposed by Arksey and O’Malley. Two major electronic databases (PubMed and EMBASE) were searched without language restriction for articles and abstracts published between January 1, 1990 and July 3, 2019. Results: Our search yielded 5049 publications from which 262 were included in this review. A majority of variants tested in RYR1 preclinical models were localized to established MH/central core disease (MH/CCD) hot spots. A total of 250 unique RYR1 variations were reported in human/rodent/porcine models with 95% being missense substitutions. -
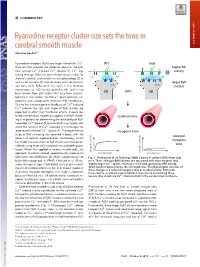
Ryanodine Receptor Cluster Size Sets the Tone in Cerebral Smooth Muscle
COMMENTARY Ryanodine receptor cluster size sets the tone in cerebral smooth muscle COMMENTARY Christian Soellera,1 + Ryanodine receptors (RyRs) are large intracellular Ca2 WT mdx channels that provide the molecular basis of the pro- K+ K+ higher BK + + + cess termed Ca2 -induced Ca2 release (1). Ca2 sig- activity naling through RyRs has been shown to be critical for CaC BK BK skeletal, cardiac, and smooth muscle physiology (2) as well as for neurons (3) and secretory cells like pancre- larger RyR atic beta cells. RyRs were first seen in the electron RyRs RyRs clusters microscope as ∼30-nm-size particles (4), and it had SMCs been known from EM studies that they form clusters, SR SR typically in the narrow “junctional” space between sar- colemma and sarcoplasmic reticulum (SR) membranes. + Due to the inherent positive feedback of Ca2 -induced + Ca2 release, the size and shape of RyR clusters are expected to affect their functional activity. Indeed, de- SMCs SMCs tailed mathematical modeling suggests that RyR cluster- cerebral artery ing is important for determining the excitability of RyR- + mediated Ca2 release (5, 6) and could, in principle, also + affect the amount of Ca2 released in microscopic re- 2+ lease events termed Ca sparks (7). The experimental myogenic tone study of RyR clustering has received a boost with the reduced advent of optical superresolution microscopy, which myogenic has made the assessment of RyR cluster size more acces- sible by using essentially standard immunolabeling pro- tone tocols. When first applied in cardiac muscle cells, this myogenic tone (%) tone myogenic approach revealed a broad, approximately exponential vessel pressure (%) tone myogenic vessel pressure RyR cluster size distribution (8), which had previously not Fig.