86A1bedb377096cf412d7e5f593
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Primary Cutaneous Nocardiosis: a Case Study and Review
Study Primary cutaneous nocardiosis: A case study and review Arun C. Inamadar, Aparna Palit Department of Dermatology, Venereology & Leprosy, BLDEA’s SBMP Medical College, Hospital & Research Centre, Bijapur, India. Address for correspondence: Dr. Arun C. Inamadar, Professor & Head, Department of Dermatology, Venereology & Leprosy, BLDEA’s SBMP Medical College, Hospital & Research Centre, Bijapur - 586103, India. E-mail: [email protected]. ABSTRACT Background: Primary cutaneous nocardiosis is an uncommon entity. It usually occurs among immunocompetent but occupationally predisposed individuals. Aim: To study clinical profile of patients with primary cutaneous nocardiosis in a tertiary care hospital and to review the literature. Methods: The records of 10 cases of primary cutaneous nocardiosis were analyzed for clinical pattern, site of involvement with cultural study and response to treatment. Results: All the patients were agricultural workers (nine male) except one housewife. The commonest clinical type was mycetoma. Unusual sites like the scalp and back were involved in two cases. Culture was positive in six cases with N. brasiliensis being commonest organism. N. nova which was previously unreported cause of lymphocutaneous nocardiosis, was noted in one patient, who had associated HIV infection. All the patients responded to cotrimaxazole. Conclusion: Mycetoma is the commonest form of primary cutaneous nocardiosis and responds well to cotrimoxazole. KEY WORDS: Primary cutaneous nocardiosis, Mycetoma, Lymphocutaneous nocardiosis INTRODUCTION infection is prevalent. Many of the large series on nocardial infections mention the incidence of Cutaneous nocardiosis presents either as a part of cutaneous nocardiosis without specifying whether the disseminated infection or as a primary infection infection is primary or secondary. Indian reports of resulting from inoculation. -

Granulomatous Diseases: Disease: Tuberculosis Leprosy Buruli Ulcer
Granulomatous diseases: Disease: Tuberculosis Leprosy Buruli ulcer MOTT diseases Actinomycosis Nocardiosis Etiology Mycobacterium M. leprae M. ulcerans M. kansasii Actinomyces israelii Nocardia asteroides tuberculosis M. scrofulaceum M. africanum M. avium- M. bovis intracellulare M. marinum Reservoir Humans (M. tuberculosis, HUMANS only Environment Environment HUMANS only Environment M. africanum*) (uncertain) Animals (M. bovis) Infects animals Transmission Air-borne route Air-borne route Uncertain: Air-borne NONE Air-borne route to humans Food-borne route Direct contact traumatic Traumatic inoculation endogenous infection Traumatic (M. bovis) inoculation, Habitat: oral cavity, inoculation insect bite? intestines, female genital tract Clinical Tuberculosis (TB): Leprosy=Hansen’s Disseminating Lung disease Abscesses in the skin Broncho-pulmonary picture pulmonary and/or disease skin ulcers Cervical lymphadenitis adjacent to mucosal surfaces (lung abscesses) extra-pulmonary Tuberculoid leprosy Disseminated (cervicofacial actinomycosis), Cutaneous infections (disseminated: kidneys, Lepromatous leprosy infection in the lungs (pulmonary) or such as: mycetoma, bones, spleen, meninges) Skin infections in the abdominal cavity lymphocutaneous (peritonitis, abscesses in infections, ulcerative appendix and ileocecal lesions, abscesses, regions) cellulitis; Dissemination: brain abscesses Distribution All over the world India, Brazil, Tropical disease All over the world All humans Tropical disease * Africa Indonesia, Africa (e.g. Africa, Asia, (e.g. -

A Diagnostic Approach to Pruritus
View metadata, citation and similar papers at core.ac.uk brought to you by CORE provided by DigitalCommons@University of Nebraska University of Nebraska - Lincoln DigitalCommons@University of Nebraska - Lincoln U.S. Air Force Research U.S. Department of Defense 2011 A Diagnostic Approach to Pruritus Brian V. Reamy Christopher W. Bunt Stacy Fletcher Follow this and additional works at: https://digitalcommons.unl.edu/usafresearch This Article is brought to you for free and open access by the U.S. Department of Defense at DigitalCommons@University of Nebraska - Lincoln. It has been accepted for inclusion in U.S. Air Force Research by an authorized administrator of DigitalCommons@University of Nebraska - Lincoln. A Diagnostic Approach to Pruritus BRIAN V. REAMY, MD, Uniformed Services University of the Health Sciences, Bethesda, Maryland CHRISTOPHER W. BUNT, MAJ, USAF, MC, and STACY FLETCHER, CAPT, USAF, MC Ehrling Bergquist Family Medicine Residency Program, Offutt Air Force Base, Nebraska, and the University of Nebraska Medical Center, Omaha, Nebraska Pruritus can be a symptom of a distinct dermatologic condition or of an occult underlying systemic disease. Of the patients referred to a dermatologist for generalized pruritus with no apparent primary cutaneous cause, 14 to 24 percent have a systemic etiology. In the absence of a primary skin lesion, the review of systems should include evaluation for thyroid disorders, lymphoma, kidney and liver diseases, and diabetes mellitus. Findings suggestive of less seri- ous etiologies include younger age, localized symptoms, acute onset, involvement limited to exposed areas, and a clear association with a sick contact or recent travel. Chronic or general- ized pruritus, older age, and abnormal physical findings should increase concern for underly- ing systemic conditions. -

Vesiculobullous Diseases Larkin Community Hospital/NSU-COM Presenters: Yuri Kim, DO, Sam Ecker, DO, Jennifer David, DO, MBA
Vesiculobullous Diseases Larkin Community Hospital/NSU-COM Presenters: Yuri Kim, DO, Sam Ecker, DO, Jennifer David, DO, MBA Program Director: Stanley Skopit, DO, MSE, FAOCD, FAAD •We have no relevant disclosures Topics of Discussion • Subcorneal Vesiculobullous Disorders – Pemphigus foliaceous – Pemphigus erythematosus – Subcorneal pustular dermatosis (Sneddon-Wilkinson Disease) – Acute Generalized Exanthematous Pustulosis • Intraepidermal Vesiculobullous Disorders – Pemphigus vulgaris – Pemphigus vegetans – Hailey-Hailey Disease – Darier’s Disease – Grover’s Disease – Paraneoplastic Pemphigus – IgA Pemphigus Topics of Discussion (Continued) • Pauci-inflammatory Subepidermal Vesiculobullous Disorders – Porphyria Cutanea Tarda (PCT) – Epidermolysis Bullosa Acquisita (EBA) – Pemphigoid Gestationis • Inflammatory Subepidermal Disorders – Bullous Pemphigoid – Cicatricial Pemphigoid – Dermatitis Herpetiformis – Linear IgA Subcorneal Vesiculobullous Disorders • Pemphigus foliaceous • Pemphigus erythematosus • Subcorneal pustular dermatosis (Sneddon- Wilkinson Disease) • AGEP Pemphigus Foliaceous • IgG Ab to desmoglein 1 (Dsg-1, 160 kDa) • Peak onset middle age, no gender preference • Endemic form – Fogo selvagem in Brazil and other parts of South America • Pemphigus erythematosus- Localized variant of pemphigus foliaceous with features of lupus erythematosus Overview Clinical H&E DIF Treatment Pemphigus Foliaceous Overview Clinical H&E DIF Treatment Pemphigus Foliaceous Overview Clinical H&E DIF Treatment Pemphigus Foliaceous Overview Clinical -

Chapter 3 Bacterial and Viral Infections
GBB03 10/4/06 12:20 PM Page 19 Chapter 3 Bacterial and viral infections A mighty creature is the germ gain entry into the skin via minor abrasions, or fis- Though smaller than the pachyderm sures between the toes associated with tinea pedis, His customary dwelling place and leg ulcers provide a portal of entry in many Is deep within the human race cases. A frequent predisposing factor is oedema of His childish pride he often pleases the legs, and cellulitis is a common condition in By giving people strange diseases elderly people, who often suffer from leg oedema Do you, my poppet, feel infirm? of cardiac, venous or lymphatic origin. You probably contain a germ The affected area becomes red, hot and swollen (Ogden Nash, The Germ) (Fig. 3.1), and blister formation and areas of skin necrosis may occur. The patient is pyrexial and feels unwell. Rigors may occur and, in elderly Bacterial infections people, a toxic confusional state. In presumed streptococcal cellulitis, penicillin is Streptococcal infection the treatment of choice, initially given as ben- zylpenicillin intravenously. If the leg is affected, Cellulitis bed rest is an important aspect of treatment. Where Cellulitis is a bacterial infection of subcutaneous there is extensive tissue necrosis, surgical debride- tissues that, in immunologically normal individu- ment may be necessary. als, is usually caused by Streptococcus pyogenes. A particularly severe, deep form of cellulitis, in- ‘Erysipelas’ is a term applied to superficial volving fascia and muscles, is known as ‘necrotiz- streptococcal cellulitis that has a well-demarcated ing fasciitis’. This disorder achieved notoriety a few edge. -

Guidelines for Case-Based Reporting
澳門特別行政區 傳染病強制申報機制 Macao SAR Notifiable Communicable Diseases Guidelines for Case-based Reporting (FIRST DRAFT) 2008 澳門特別行局區政府衛生局 Health Bureau, Government of Macao Special Administrative Region ii iii Contents Contents ............................................................................................................................................................ iii Signs and abbreviations .................................................................................................................................... 5 Acquired immunodeficiency syndrome (AIDS) ............................................................................................... 6 Acute gastroenteropathy due to Norwalk agent (ICD-9 : 008.6, ICD-10 : A08.1 ) ...................................... 11 Acute haemorrhagic conjunctivitis (ICD-9 : 077, ICD-10 : B30.3 ) ............................................................. 12 Acute poliomyelitis ICD-9 045 ICD-10 A80 ................................................................................... 13 Amoebiasis ICD-9 006 ICD-10 A06 ............................................................................................... 14 Anogenital herpesviral (herpes simplex) infection ICD-9 054 ICD-10 A60 ............................... 16 Anthrax ICD-9 022 ICD-10 A22 .................................................................................................. 17 Chickenpox (Varicella) ICD-9 052 ICD-10 B01 ............................................................................ 19 Cholera ICD-9 -

Extrafacial Granuloma Faciale
Journal of the American Osteopathic College of Dermatology Volume 11, Number 1 SPONSORS: ',/"!,0!4(/,/'9,!"/2!4/29s-%$)#)3 July 2008 34)%&%,,!"/2!4/2)%3s'!,$%2-! www.aocd.org Journal of the American Osteopathic College of Dermatology Journal of the American Osteopathic College of Dermatology 2007-2008 Officers President: Jay Gottlieb, DO President Elect: Donald Tillman, DO First Vice President: Marc Epstein, DO Second Vice President: Leslie Kramer, DO Third Vice President: Bradley Glick, DO Secretary-Treasurer: Jere Mammino, DO (2007-2010) Immediate Past President: Bill Way, DO Trustees: James Towry, DO (2006-2008) Mark Kuriata, DO (2007-2010) Karen Neubauer, DO (2006-2008) David Grice, DO (2007-2010) Sponsors: Global Pathology Laboratory Editors Stiefel Laboratories Jay S. Gottlieb, D.O., F.O.C.O.O. Medicis Stanley E. Skopit, D.O., F.A.O.C.D. James Q. Del Rosso, D.O., F.A.O.C.D. Galderma Editorial Review Board Ronald Miller, D.O. JAOCD Eugene Conte, D.O. Founding Sponsor Evangelos Poulos, M.D. Stephen Purcell, D.O. Darrel Rigel, M.D. !/#$s%)LLINOISs+IRKSVILLE -/ s&!8 Robert Schwarze, D.O. WWWAOCDORG Andrew Hanly, M.D. #/092)'(4!.$0%2-)33)/.WRITTENPERMISSIONMUSTBEOBTAINED Michael Scott, D.O. FROMTHE*OURNALOFTHE!MERICAN/STEOPATHIC#OLLEGEOF$ERMATOLOGY FORCOPYINGORREPRINTINGTEXTOFMORETHANHALFPAGE TABLESORlGURES Cindy Hoffman, D.O. 0ERMISSIONSARENORMALLYGRANTEDCONTINGENTUPONSIMILARPERMISSION Charles Hughes, D.O. FROMTHEAUTHORS INCLUSIONOFACKNOWLEDGEMENTOFTHEORIGINALSOURCE ANDAPAYMENTOFPERPAGE TABLEORlGUREOFREPRODUCEDMATERIAL Bill Way, D.O. 0ERMISSIONFEESAREWAIVEDFORAUTHORSWISHINGTOREPRODUCETHEIROWN Daniel Hurd, D.O. ARTICLES2EQUESTFORPERMISSIONSHOULDBEDIRECTEDTO*!/#$CO!/#$ 0/"OX+IRKSVILLE -/ Mark Lebwohl, M.D. #OPYRIGHTBYTHE*OURNALOFTHE!MERICAN/STEOPATHIC#OLLEGEOF Edward Yob, D.O. $ERMATOLOGY Jere Mammino, D.O. Printed by: Stoyles Graphics Services, Mason City, IA 50401 Schield M. -
Lepromatous Leprosy with Erythema Nodosum Leprosum Presenting As
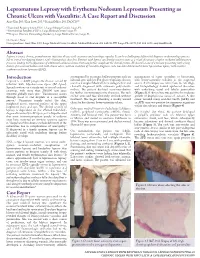
Lepromatous Leprosy with Erythema Nodosum Leprosum Presenting as Chronic Ulcers with Vasculitis: A Case Report and Discussion Anny Xiao, DO,* Erin Lowe, DO,** Richard Miller, DO, FAOCD*** *Traditional Rotating Intern, PGY-1, Largo Medical Center, Largo, FL **Dermatology Resident, PGY-2, Largo Medical Center, Largo, FL ***Program Director, Dermatology Residency, Largo Medical Center, Largo, FL Disclosures: None Correspondence: Anny Xiao, DO; Largo Medical Center, Graduate Medical Education, 201 14th St. SW, Largo, FL 33770; 510-684-4190; [email protected] Abstract Leprosy is a rare, chronic, granulomatous infectious disease with cutaneous and neurologic sequelae. It can be a challenging differential diagnosis in dermatology practice due to several overlapping features with rheumatologic disorders. Patients with leprosy can develop reactive states as a result of immune complex-mediated inflammatory processes, leading to the appearance of additional cutaneous lesions that may further complicate the clinical picture. We describe a case of a woman presenting with a long history of a recurrent bullous rash with chronic ulcers, with an evolution of vasculitic diagnoses, who was later determined to have lepromatous leprosy with reactive erythema nodosum leprosum (ENL). Introduction accompanied by an intense bullous purpuric rash on management of sepsis secondary to bacteremia, Leprosy is a slowly progressive disease caused by bilateral arms and face. For these complaints she was with lower-extremity cellulitis as the suspected infection with Mycobacterium leprae (M. leprae). seen in a Complex Medical Dermatology Clinic and source. A skin biopsy was taken from the left thigh, Spread continues at a steady rate in several endemic clinically diagnosed with cutaneous polyarteritis and histopathology showed epidermal ulceration countries, with more than 200,000 new cases nodosa. -

ORIGINAL ARTICLE a Clinical and Histopathological Study of Lichenoid Eruption of Skin in Two Tertiary Care Hospitals of Dhaka
ORIGINAL ARTICLE A Clinical and Histopathological study of Lichenoid Eruption of Skin in Two Tertiary Care Hospitals of Dhaka. Khaled A1, Banu SG 2, Kamal M 3, Manzoor J 4, Nasir TA 5 Introduction studies from other countries. Skin diseases manifested by lichenoid eruption, With this background, this present study was is common in our country. Patients usually undertaken to know the clinical and attend the skin disease clinic in advanced stage histopathological pattern of lichenoid eruption, of disease because of improper treatment due to age and sex distribution of the diseases and to difficulties in differentiation of myriads of well assess the clinical diagnostic accuracy by established diseases which present as lichenoid histopathology. eruption. When we call a clinical eruption lichenoid, we Materials and Method usually mean it resembles lichen planus1, the A total of 134 cases were included in this study prototype of this group of disease. The term and these cases were collected from lichenoid used clinically to describe a flat Bangabandhu Sheikh Mujib Medical University topped, shiny papular eruption resembling 2 (Jan 2003 to Feb 2005) and Apollo Hospitals lichen planus. Histopathologically these Dhaka (Oct 2006 to May 2008), both of these are diseases show lichenoid tissue reaction. The large tertiary care hospitals in Dhaka. Biopsy lichenoid tissue reaction is characterized by specimen from patients of all age group having epidermal basal cell damage that is intimately lichenoid eruption was included in this study. associated with massive infiltration of T cells in 3 Detailed clinical history including age, sex, upper dermis. distribution of lesions, presence of itching, The spectrum of clinical diseases related to exacerbating factors, drug history, family history lichenoid tissue reaction is wider and usually and any systemic manifestation were noted. -

Unit 3 Bites and Stings
First Aid in Common and Environmental Emergencies UNIT 3 BITES AND STINGS Structure 3.0 Introduction 3.1 Objectives 3.2 Bites and Stings 3.2.1 Definition, Causes, Types and Recognition of Bites and Stings 3.2.2 Assessment of the Victim and General First Aid 3.3 Various Bites/Stings 3.3.1 Scorpion Bite and Spider Bite 3.3.2 Snake Bite 3.3.3 Insect Bite 3.3.4 Animal Bites (Dog Bite/Monkey Bites) 3.3.5 Human Bites 3.4 Let Us Sum Up 3.5 Keywords 3.6 Answers to Check Your Progress 3.7 References and Further Readings 3.0 INTRODUCTION Bites and stings are commonly seen in the rural and remote areas. Nowadays, however, they can occur in urban areas also. Lakhs of people every year are bitten or stung by someone or something. These emergencies include bites and stings due to various reasons. These bites or stings need to be identified and treated early as they affect some part or the whole of the body which can cause mild, moderate or severe reaction and can even be life-threatening. Most are not medical emergencies but however, treatment is usually required if there is bleeding, wounds or infection. All bites and stings are not same. Different First Aid treatment and care is needed depending on the type of insect or animal that has caused the bite. Some species are more dangerous and cause more harm compared to others. Hence, in this unit we shall discuss the different types of bites and stings, causes, recognition and first aid in these situations. -

Case for Diagnosis* Caso Para Diagnóstico*
RevABDV81N5.qxd 09.11.06 09:42 Page 490 490 Qual o seu diagnóstico? Caso para diagnóstico* Case for diagnosis* Rodrigo Pereira Duquia1 Hiram Larangeira de Almeida Jr2 Ernani Siegmann Duvelius3 Manfred Wolter4 HISTÓRIA DA DOENÇA Paciente do sexo feminino, de 76 anos, há lesões liquenóides dorsais, solicitação do teste de dois anos apresentou linfadenopatias na região Mantoux e exames laboratoriais, com a suspeita de cervical (Figura 1) e axilar esquerda. Após um ano scrofuloderma e líquen scrofulosorum. Nessa oca- iniciou fistulização e drenagem de material esbran- sião a paciente apresentava-se em mau estado geral quiçado das lesões, emagrecimento e aparecimen- com febre persistente, emagrecimento importante to de lesões anulares liquenóides com centro atró- e astenia. fico na região dorsal (Figura 2), levemente prurigi- O Mantoux foi fortemente reator, 24mm, velo- nosas. Há seis meses realizou biópsia da região cer- cidade de sedimentação globular de 96mm, a cultura vical, que foi inconclusiva. Posteriormente foi enca- da secreção cervical foi negativa, e PCR foi positiva minhada para avaliação dermatológica, sendo reali- para Mycobacterium tuberculosis. zada coleta de material da região cervical, enviado O exame histopatológico das lesões do dorso então para cultura e reação em cadeia pela polime- revelou espongiose focal na epiderme com alguns rase (PCR). Além disso, realizaram-se biópsia das queratinócitos necróticos, apresentando na derme FIGURA 1: Lesões eritematosas com crosta hemática recobrindo as FIGURA 2: Lesões liquenóides, anulares, com atrofia central na fístulas na região cervical esquerda região dorsal. No detalhe à direita, a atrofia central e os bordos papulosos e anulares ficam mais evidentes Recebido em 22.02.2006. -

A Case of Igg/Iga Pemphigus Presenting Malar Rash-Like Erythema
164 Letters to the Editor A Case of IgG/IgA Pemphigus Presenting Malar Rash-like Erythema Satomi Hosoda1, Masayuki Suzuki1, Mayumi Komine1*, Satoru Murata1, Takashi Hashimoto2 and Mamitaro Ohtsuki1 Departments of Dermatology, 1Jichi Medical University, 3311-1 Yakushiji, Shimotsuke, Tochigi 329-0498 and 2Kurume University School of Medicine, and Kurume University Institute of Cutaneous Cell Biology, Fukuoka, Japan. *E-mail: [email protected] Accepted August 17, 2011. Pemphigus is an autoimmune mucocutaneous bullous disease characterized by auto-antibodies against cell surface antigens of epidermal keratinocytes. Pemphigus vulgaris (PV) and pemphigus foliaceus (PF) are the major subtypes. Several other variants have been proposed, in- cluding pemphigus erythematosus, pemphigus vegetans, pemphigus herpetiformis (PH), and paraneoplastic pem- phigus. Deposition of IgG on epidermal keratinocyte cell surfaces and circulating anti-cell surface antibodies are characteristic in pemphigus. Cases involving IgA depo- sition on epidermal keratinocyte cell surfaces have been reported as IgA pemphigus. IgA pemphigus is divided into 4 subgroups based on clinical manifestation: subcorneal pustular dermatosis type, intraepidermal neutrophilic IgA dermatosis type, pemphigus foliaceus type, and pemphi- gus vulgaris type. Cases involving deposition of both IgG and IgA on keratinocyte cell surfaces have been reported (1–13). Some authors describe them as IgG/IgA pemphi- gus (1). Seventeen such cases have been reported so far, and heterogeneity of clinical features and target antigen has been detected in this group of pemphigus. Fig. 1. (A) Annular erythematous areas on the back covered with scales CASE REPOrt and superficial crusts. (B) Malar rash-like facial A 62-year-old Japanese woman was referred to our department erythemas with vesicles on with a 1-month history of pruritic skin lesions.