Congenital Limb Differences
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Neonatal Orthopaedics
NEONATAL ORTHOPAEDICS NEONATAL ORTHOPAEDICS Second Edition N De Mazumder MBBS MS Ex-Professor and Head Department of Orthopaedics Ramakrishna Mission Seva Pratishthan Vivekananda Institute of Medical Sciences Kolkata, West Bengal, India Visiting Surgeon Department of Orthopaedics Chittaranjan Sishu Sadan Kolkata, West Bengal, India Ex-President West Bengal Orthopaedic Association (A Chapter of Indian Orthopaedic Association) Kolkata, West Bengal, India Consultant Orthopaedic Surgeon Park Children’s Centre Kolkata, West Bengal, India Foreword AK Das ® JAYPEE BROTHERS MEDICAL PUBLISHERS (P) LTD. New Delhi • London • Philadelphia • Panama (021)66485438 66485457 www.ketabpezeshki.com ® Jaypee Brothers Medical Publishers (P) Ltd. Headquarters Jaypee Brothers Medical Publishers (P) Ltd. 4838/24, Ansari Road, Daryaganj New Delhi 110 002, India Phone: +91-11-43574357 Fax: +91-11-43574314 Email: [email protected] Overseas Offices J.P. Medical Ltd. Jaypee-Highlights Medical Publishers Inc. Jaypee Brothers Medical Publishers Ltd. 83, Victoria Street, London City of Knowledge, Bld. 237, Clayton The Bourse SW1H 0HW (UK) Panama City, Panama 111, South Independence Mall East Phone: +44-2031708910 Phone: +507-301-0496 Suite 835, Philadelphia, PA 19106, USA Fax: +02-03-0086180 Fax: +507-301-0499 Phone: +267-519-9789 Email: [email protected] Email: [email protected] Email: [email protected] Jaypee Brothers Medical Publishers (P) Ltd. Jaypee Brothers Medical Publishers (P) Ltd. 17/1-B, Babar Road, Block-B, Shaymali Shorakhute, Kathmandu Mohammadpur, Dhaka-1207 Nepal Bangladesh Phone: +00977-9841528578 Mobile: +08801912003485 Email: [email protected] Email: [email protected] Website: www.jaypeebrothers.com Website: www.jaypeedigital.com © 2013, Jaypee Brothers Medical Publishers All rights reserved. No part of this book may be reproduced in any form or by any means without the prior permission of the publisher. -

Genetic Causes of Congenital Malformation in India
International Journal of Human Genetics ISSN: 0972-3757 (Print) (Online) Journal homepage: http://www.tandfonline.com/loi/rhug20 Genetic Causes of Congenital Malformation in India Geeta Talukder & Archana Sharma To cite this article: Geeta Talukder & Archana Sharma (2006) Genetic Causes of Congenital Malformation in India, International Journal of Human Genetics, 6:1, 15-25, DOI: 10.1080/09723757.2006.11885942 To link to this article: https://doi.org/10.1080/09723757.2006.11885942 Published online: 04 Sep 2017. Submit your article to this journal Article views: 2 View related articles Full Terms & Conditions of access and use can be found at http://www.tandfonline.com/action/journalInformation?journalCode=rhug20 © Kamla-Raj 2006 Int J Hum Genet, 6(1): 15-25 (2006) Genetic Causes of Congenital Malformation in India Geeta Talukder1 and Archana Sharma2 1. Vivekananda Institute of Medical Sciences, 99 Sarat Bose Road, Kolkata 700 026, West Bengal, India E-mail: geetatalukdar @hotmail.com 2. CAS in Cell & Chromosome Research, Department of Botany, University College of Science, 35 Ballygunj Circular Road, Kolkata 700 019, West Bengal, India KEYWORDS Congenital malformations; neonates; stillbirths; prenatal detection; prevention ABSTRACT Congenital malformations are a major cause of death of neonates in India where prenatal detection and treatment are not adequate in many hospitals and health centers. Incidence is specially high in stillbirths. It is not realized that genetic causes - chromosomal, single gene and polygenic - are the main causes of many congenital defects and early detection and prevention should be essential to make the small family norm a success. INTRODUCTION Recently Patel and Adhia (2005) detected major malformations in 7.92% of 17653 births and Phenotypic changes of genetic diseases at were able to attribute chromosomal cause to birth include congenital malformations in 4%,polygenic to 45.1% and total genetic chromosomes and single gene defects. -

Genetics of Congenital Hand Anomalies
G. C. Schwabe1 S. Mundlos2 Genetics of Congenital Hand Anomalies Die Genetik angeborener Handfehlbildungen Original Article Abstract Zusammenfassung Congenital limb malformations exhibit a wide spectrum of phe- Angeborene Handfehlbildungen sind durch ein breites Spektrum notypic manifestations and may occur as an isolated malforma- an phänotypischen Manifestationen gekennzeichnet. Sie treten tion and as part of a syndrome. They are individually rare, but als isolierte Malformation oder als Teil verschiedener Syndrome due to their overall frequency and severity they are of clinical auf. Die einzelnen Formen kongenitaler Handfehlbildungen sind relevance. In recent years, increasing knowledge of the molecu- selten, besitzen aber aufgrund ihrer Häufigkeit insgesamt und lar basis of embryonic development has significantly enhanced der hohen Belastung für Betroffene erhebliche klinische Rele- our understanding of congenital limb malformations. In addi- vanz. Die fortschreitende Erkenntnis über die molekularen Me- tion, genetic studies have revealed the molecular basis of an in- chanismen der Embryonalentwicklung haben in den letzten Jah- creasing number of conditions with primary or secondary limb ren wesentlich dazu beigetragen, die genetischen Ursachen kon- involvement. The molecular findings have led to a regrouping of genitaler Malformationen besser zu verstehen. Der hohe Grad an malformations in genetic terms. However, the establishment of phänotypischer Variabilität kongenitaler Handfehlbildungen er- precise genotype-phenotype correlations for limb malforma- schwert jedoch eine Etablierung präziser Genotyp-Phänotyp- tions is difficult due to the high degree of phenotypic variability. Korrelationen. In diesem Übersichtsartikel präsentieren wir das We present an overview of congenital limb malformations based Spektrum kongenitaler Malformationen, basierend auf einer ent- 85 on an anatomic and genetic concept reflecting recent molecular wicklungsbiologischen, anatomischen und genetischen Klassifi- and developmental insights. -

Syndromic Ear Anomalies and Renal Ultrasounds
Syndromic Ear Anomalies and Renal Ultrasounds Raymond Y. Wang, MD*; Dawn L. Earl, RN, CPNP‡; Robert O. Ruder, MD§; and John M. Graham, Jr, MD, ScD‡ ABSTRACT. Objective. Although many pediatricians cific MCA syndromes that have high incidences of renal pursue renal ultrasonography when patients are noted to anomalies. These include CHARGE association, Townes- have external ear malformations, there is much confusion Brocks syndrome, branchio-oto-renal syndrome, Nager over which specific ear malformations do and do not syndrome, Miller syndrome, and diabetic embryopathy. require imaging. The objective of this study was to de- Patients with auricular anomalies should be assessed lineate characteristics of a child with external ear malfor- carefully for accompanying dysmorphic features, includ- mations that suggest a greater risk of renal anomalies. We ing facial asymmetry; colobomas of the lid, iris, and highlight several multiple congenital anomaly (MCA) retina; choanal atresia; jaw hypoplasia; branchial cysts or syndromes that should be considered in a patient who sinuses; cardiac murmurs; distal limb anomalies; and has both ear and renal anomalies. imperforate or anteriorly placed anus. If any of these Methods. Charts of patients who had ear anomalies features are present, then a renal ultrasound is useful not and were seen for clinical genetics evaluations between only in discovering renal anomalies but also in the diag- 1981 and 2000 at Cedars-Sinai Medical Center in Los nosis and management of MCA syndromes themselves. Angeles and Dartmouth-Hitchcock Medical Center in A renal ultrasound should be performed in patients with New Hampshire were reviewed retrospectively. Only pa- isolated preauricular pits, cup ears, or any other ear tients who underwent renal ultrasound were included in anomaly accompanied by 1 or more of the following: the chart review. -
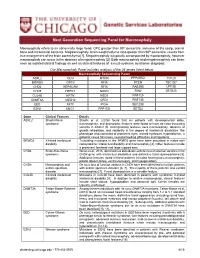
Macrocephaly Information Sheet 6-13-19
Next Generation Sequencing Panel for Macrocephaly Clinical Features: Macrocephaly refers to an abnormally large head, OFC greater than 98th percentile, inclusive of the scalp, cranial bone and intracranial contents. Megalencephaly, brain weight/volume ratio greater than 98th percentile, results from true enlargement of the brain parenchyma [1]. Megalencephaly is typically accompanied by macrocephaly, however macrocephaly can occur in the absence of megalencephaly [2]. Both macrocephaly and megalencephaly can been seen as isolated clinical findings as well as clinical features of a mutli-systemic syndromic diagnosis. Our Macrocephaly Panel includes analysis of the 36 genes listed below. Macrocephaly Sequencing Panel ASXL2 GLI3 MTOR PPP2R5D TCF20 BRWD3 GPC3 NFIA PTEN TBC1D7 CHD4 HEPACAM NFIX RAB39B UPF3B CHD8 HERC1 NONO RIN2 ZBTB20 CUL4B KPTN NSD1 RNF125 DNMT3A MED12 OFD1 RNF135 EED MITF PIGA SEC23B EZH2 MLC1 PPP1CB SETD2 Gene Clinical Features Details ASXL2 Shashi-Pena Shashi et al. (2016) found that six patients with developmental delay, syndrome macrocephaly, and dysmorphic features were found to have de novo truncating variants in ASXL2 [3]. Distinguishing features were macrocephaly, absence of growth retardation, and variability in the degree of intellectual disabilities The phenotype also consisted of prominent eyes, arched eyebrows, hypertelorism, a glabellar nevus flammeus, neonatal feeding difficulties and hypotonia. BRWD3 X-linked intellectual Truncating mutations in the BRWD3 gene have been described in males with disability nonsyndromic intellectual disability and macrocephaly [4]. Other features include a prominent forehead and large cupped ears. CHD4 Sifrim-Hitz-Weiss Weiss et al., 2016, identified five individuals with de novo missense variants in the syndrome CHD4 gene with intellectual disabilities and distinctive facial dysmorphisms [5]. -

Congenital Transverse Defects of Limbs and Digits* ('Intrauterine Amputation') by H
Arch Dis Child: first published as 10.1136/adc.37.193.263 on 1 June 1962. Downloaded from CONGENITAL TRANSVERSE DEFECTS OF LIMBS AND DIGITS* ('INTRAUTERINE AMPUTATION') BY H. G. KOHLER From the Department ofPathology, Birmingham Maternity Hospital (RECEIVED FOR PUBLICATION OCTOBER 23, 1961) Intrauterine amputation of the extremities is an Thomas Bartholin of Copenhagen (1616-1680) uncommon and peculiar congenital deformity which is said to be the first to mention a congenitally is characterized by the absence of one or more distal deficient extremity. He lived at the very threshold limb portions. Termination of the proximal part of the modern scientific era and belonged to a family is usually abrupt and bears no apparent relation to well known for their contributions to medicine and anatomical boundaries. The term 'amputation' biology: Thomas Bartholin's son, Caspar Secundus, suggests separation, by mechanical force, of a limb was the first to describe the vestibulo-vaginal glands. already formed rather than a failure of develop- Thomas was a man of great learning and wide ment, but such a view of the pathogenesis of this interests (Rhodes, 1957). His textbook on anatomy abnormality is far from universally accepted. It was translated into English and used widely for a would probably be better to use a neutral term such long time. Bartholin's descriptions of monsters, as 'transverse defects', but for the conservatism of however, tend to be more imaginative than factual medical nomenclature. (Hendry and Kohler, 1956). The essay which copyright. Circular grooves around the digits or limbs, and contains a reference to limb defects bears the title similar soft tissue defects, also known as ring con- 'Gravidarum Imaginatio' and there, in passing, he strictions, are seen usually in association with 'intra- tells us of a deformed male infant with only one uterine amputation', but also on their own. -

Unilateral Proximal Focal Femoral Deficiency, Fibular Aplasia, Tibial
The Egyptian Journal of Medical Human Genetics (2014) 15, 299–303 Ain Shams University The Egyptian Journal of Medical Human Genetics www.ejmhg.eg.net www.sciencedirect.com CASE REPORT Unilateral proximal focal femoral deficiency, fibular aplasia, tibial campomelia and oligosyndactyly in an Egyptian child – Probable FFU syndrome Rabah M. Shawky a,*, Heba Salah Abd Elkhalek a, Shaimaa Gad a, Shaimaa Abdelsattar Mohammad b a Pediatric Department, Genetics Unit, Ain Shams University, Egypt b Radio Diagnosis Department, Ain Shams University, Egypt Received 2 March 2014; accepted 18 March 2014 Available online 30 April 2014 KEYWORDS Abstract We report a fifteen month old Egyptian male child, the third in order of birth of healthy Short femur; non consanguineous parents, who has normal mentality, normal upper limbs and left lower limb. Limb anomaly; The right lower limb has short femur, and tibia with anterior bowing, and an overlying skin dimple. FFU syndrome; The right foot has also oligosyndactyly (three toes), and the foot is in vulgus position. There is lim- Proximal focal femoral ited abduction at the hip joint, full flexion and extension at the knee, limited dorsiflexion and plan- deficiency; tar flexion at the ankle joint. The X-ray of the lower limb and pelvis shows proximal focal femoral Fibular aplasia; deficiency, absent right fibula with shortening of the right tibia and anterior bowing of its distal Tibial campomelia; third. The acetabulum is shallow. He has a family history of congenital cyanotic heart disease. Oligosyndactyly Our patient represents most probably the first case of femur fibula ulna syndrome (FFU) in Egypt with unilateral right leg affection. -

Multiple Hereditary Exostoses
Multiple Hereditary Exostoses Dror Paley MD, FRCSC Medical Director, Paley Orthopedic and spine Institute, St. Mary’s Medical Center, West palm Beach, FL David Feldman, MD Director, Spinal deformity center, Paley Orthopedic and spine Institute, St. Mary’s Medical Center, West palm Beach, FL Multiple hereditary exostoses (MHE), also known as multiple osteochondromas (MO), is an autosomal dominant skeletal disorder. Approximately 10–20% of individuals are a result of a spontaneous mutation while the rest are familial. The prevalence of MHE/MO is 1/50 000. There are two known genes found to cause MHE/MO, EXT1 located on chromosome 8q23-q24 and EXT2 located on chromosome 11p11-p12. In 10–15% of the patients, no mutation can be located by current methods of genetic testing.1–7 These mutations are scattered across both genes. EXT1/EXT2 is essential for the biosynthesis of heparan sulfate (HS). HS production in patients’ cells is reduced by 50% or more.8–19 MHE/MO is associated with characteristic progressive skeletal deformities of the extremities and shortening of one or both the sides, leading to limb length discrepancy (LLD) and short stature.20–28 Two bone segments, such as the lower leg or forearm, are at greater risk of problems due to either osteochondromas (OCs) from one or both bones impinging on or deforming the other bone or a primary issue of altered growth causing one bone to grow at a faster or slower rate. OCs can also affect joint motion due to impingement of an OC with the opposite side of the joint or subluxation/dislocation related to deformity, impingement, and incongruity.20,24,26,29,30 OCs can also cause nerve or vessel entrapment and/or compression, including the spinal cord and nerve roots. -

GUIDE to ADAPTED SWIMMING CLASSIFICATIONS Swimming Is
GUIDE TO ADAPTED SWIMMING CLASSIFICATIONS Swimming is the only sport that combines the conditions of limb loss, cerebral palsy (coordination and movement restrictions), spinal cord injury (weakness or paralysis involving any combination of the limbs) and other disabilities (such as Dwarfism (little people); major joint restriction conditions) across classes. Classes 1-10 – are allocated to swimmers with a physical disability Classes 11-13 – are allocated to swimmers with a visual disability Class 14 – is allocated to swimmers with an intellectual disability The Prefix S to the Class denotes the class for Freestyle, Backstroke and Butterfly The Prefix SB to the class denotes the class for Breaststroke The Prefix SM to the class denotes the class for Individual Medley. The range is from the swimmers with severe disability (S1, SB1, SM1) to those with the minimal disability (S10, SB9, SM10) In any one class some swimmers may start with a dive or in the water depending on their condition. This is factored in when classifying the athlete. The examples are only a guide – some conditions not mentioned may also fit the following classes. Locomotor Impaired (S1-S10): S1: Generally persons with complete spinal cord injuries below C4-C5 or cerebral palsy characterized by severe quadriplegia. Unable to catch the water. Severely limited propulsion from the arms due to muscle weakness, restricted range of motion or uncoordinated movements. No trunk control. No functional leg movements and significant leg drag. Assisted water start. Ordinarily uses the backstroke because of an inability to turn the head to breathe when swimming freestyle. S2: Generally persons with complete spinal cord injuries below C6-C7 or similar musculoskeletal impairment or cerebral palsy characterized by severe quadriplegia. -

Polydactyly of the Hand
A Review Paper Polydactyly of the Hand Katherine C. Faust, MD, Tara Kimbrough, BS, Jean Evans Oakes, MD, J. Ollie Edmunds, MD, and Donald C. Faust, MD cleft lip/palate, and spina bifida. Thumb duplication occurs in Abstract 0.08 to 1.4 per 1000 live births and is more common in Ameri- Polydactyly is considered either the most or second can Indians and Asians than in other races.5,10 It occurs in a most (after syndactyly) common congenital hand ab- male-to-female ratio of 2.5 to 1 and is most often unilateral.5 normality. Polydactyly is not simply a duplication; the Postaxial polydactyly is predominant in black infants; it is most anatomy is abnormal with hypoplastic structures, ab- often inherited in an autosomal dominant fashion, if isolated, 1 normally contoured joints, and anomalous tendon and or in an autosomal recessive pattern, if syndromic. A prospec- ligament insertions. There are many ways to classify tive San Diego study of 11,161 newborns found postaxial type polydactyly, and surgical options range from simple B polydactyly in 1 per 531 live births (1 per 143 black infants, excision to complicated bone, ligament, and tendon 1 per 1339 white infants); 76% of cases were bilateral, and 3 realignments. The prevalence of polydactyly makes it 86% had a positive family history. In patients of non-African descent, it is associated with anomalies in other organs. Central important for orthopedic surgeons to understand the duplication is rare and often autosomal dominant.5,10 basic tenets of the abnormality. Genetics and Development As early as 1896, the heritability of polydactyly was noted.11 As olydactyly is the presence of extra digits. -

Management of Fibular Hemimelia (Congenital Absence of Fibula) Using Ilizarov Method in Sulaimani
European Scientific Journal October 2015 edition vol.11, No.30 ISSN: 1857 – 7881 (Print) e - ISSN 1857- 7431 MANAGEMENT OF FIBULAR HEMIMELIA (CONGENITAL ABSENCE OF FIBULA) USING ILIZAROV METHOD IN SULAIMANI Ass. Prof. Dr. Omer Ali Rafiq Barawi, Ass. Lecturer Zmnako J. Amen School of Medicine, University of Sulaimani, Kurdistan Region, Iraq Abstract Background: Fibular hemimelia is the most common congenital deficiency of long bones. Therefore, it is characterized by a wide spectrum of manifestations ranging from mild limb length inequality to sever shortening with foot and ankle deformities and associated anomalies. Objectives: To evaluate the results of ankle and foot reconstruction and limb length equalization in patients with Fibular Hemimelia. Patients and Methods: A prospective study was carried out on 40 limbs in 32 patients with fibular hemimelia during the periods of March 2010 to January 2014. Male to female ratio was 24:8. Their age ranged at an average between 2-16 years (9 years). The reconstruction of ankle and foot was done. Also, the equalization of the limb was done also using Ilizarov frame. Results: The result of this study was assessed using the Association for the Study of Applications of Methods of Ilizarov (ASAMI) scoring system. Therefore, the final results were: Failure rate with 2 limbs 5%, Poor with 2 limbs 5%, Fair with 2 limbs 5%, Good with 8 limbs 20%, and Excellent with 26 limbs 65%. Conclusion: In conclusion, the Ilizarov method is an attractive alternative method used for the management of selected fibular hemimelic patients having three or more toes who are refusing amputation. -

Familial Poland Anomaly
J Med Genet: first published as 10.1136/jmg.19.4.293 on 1 August 1982. Downloaded from Journal ofMedical Genetics, 1982, 19, 293-296 Familial Poland anomaly T J DAVID From the Department of Child Health, University of Manchester, Booth Hall Children's Hospital, Manchester SUMMARY The Poland anomaly is usually a non-genetic malformation syndrome. This paper reports two second cousins who both had a typical left sided Poland anomaly, and this constitutes the first recorded case of this condition affecting more than one member of a family. Despite this, for the purposes of genetic counselling, the Poland anomaly can be regarded as a sporadic condition with an extremely low recurrence risk. The Poland anomaly comprises congenital unilateral slightly reduced. The hands were normal. Another absence of part of the pectoralis major muscle in son (Greif himself) said that his own left pectoralis combination with a widely varying spectrum of major was weaker than the right. "Although the ipsilateral upper limb defects.'-4 There are, in difference is obvious, the author still had to carry addition, patients with absence of the pectoralis out his military duties"! major in whom the upper limbs are normal, and Trosev and colleagues9 have been widely quoted as much confusion has been caused by the careless reporting familial cases of the Poland anomaly. labelling of this isolated defect as the Poland However, this is untrue. They described a mother anomaly. It is possible that the two disorders are and child with autosomal dominant radial sided part of a single spectrum, though this has never been upper limb defects.