THE ANATOMY of the SYMPATHETHIC TRUNKS in MAN by MARTIN WRETE Histological Department, the University of Uppsala, Sweden
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Variations of Thoracic Splanchnic Nerves and Its Clinical Implications
Int. J. Morphol., 23(3):247-251, 2005. Variations of Thoracic Splanchnic Nerves and its Clinical Implications Variaciones de los Nervios Esplácnicos Torácicos y sus Implicancias Clínicas *Tony George Jacob; ** Surbhi Wadhwa; ***Shipra Paul & ****Srijit Das JACOB, G. T.; WADHWA, S.; PAUL, S. & DAS, S. Variations of thoracic splanchnic nerves and its clinical implications. Int. J. Morphol., 23(3):247-251, 2005. SUMMARY:The present study reports an anomalous branching pattern of the thoracic sympathetic chain. At the level of T3 ganglion, an anomalous branch i.e accessory sympathetic chain (ASC) descended anteromedial to the main sympathetic chain (MSC). The MSC and the ASC communicated with each other at the level of T9, T10 and T11 ganglion, indicating the absence of classical pattern of greater, lesser and least splanchnic nerves on the right side. However, on the left side, the sympathetic chain displayed normal branching pattern. We opine that the ASC may be representing a higher origin of greater splanchnic nerve at the level of T3 ganglion and the branches from MSC at T9, T10 and T11 ganglion may be the lesser and least splanchnic nerves, which further joined the ASC (i.e presumably the greater splanchnic nerve) to form a common trunk. This common trunk pierced the right crus of diaphragm to reach the right suprarenal plexus after giving few branches to the celiac plexus. Awareness and knowledge of such anatomical variants of thoracic sympathetic chain may be helpful to surgeons in avoiding any incomplete denervation or preventing any inadvertent injury during thoracic sympathectomy. KEY WORDS: Splanchnic nerves; Sympathetic chain; Trunk thoracic; Ganglion. -

Autonomic Nervous System
AUTONOMIC NERVOUS SYSTEM PAGE 1 AUTONOMIC NERVOUS SYSTEM PAGE 2 AUTONOMIC NERVOUS SYSTEM PAGE 3 AUTONOMIC NERVOUS SYSTEM PAGE 4 AUTONOMIC NERVOUS SYSTEM PAGE 5 AUTONOMIC NERVOUS SYSTEM PAGE 6 AUTONOMIC NERVOUS SYSTEM PAGE 7 AUTONOMIC NERVOUS SYSTEM PAGE 8 AUTONOMIC NERVOUS SYSTEM PAGE 9 REVIEW QUESTIONS 1. The autonomic nervous system controls the activity of _?_. (a) smooth muscle (b) cardiac muscle (c) glands (d) all of these (e) none of these 2. All preganglionic and postganglionic autonomic neurons are _?_ neurons. (a) somatic efferent (b) visceral efferent (c) somatic afferent (d) visceral afferent (e) association neurons 3. Which neurotransmitter is released at the synapses between preganglionic and postganglionic autonomic neurons ? (a) epinephrine (b) norepinephrine (c) acetylcholine (d) serotonin (e) oxytocin 4. All preganglionic sympathetic neurons are located in: (a) the lateral horn of the spinal cord of spinal cord segments T1-L2 (b) brainstem nuclei (c) intramural (terminal) ganglia (d) paravertebral ganglia of the sympathetic chains (e) prevertebral ganglia 5. All preganglionic parasympathetic neurons are located in _?_. (a) prevertebral ganglia (b) the lateral horn of spinal cord segments T1-L2 (c) sympathetic chain ganglia (d) intramural ganglia (e) brainstem nuclei and spinal cord segments S2-S4 6. Prevertebral and paravertebral ganglia contain _?_. (a) preganglionic sympathetic neurons (b) preganglionic parasympathetic neurons (c) postganglionic sympathetic neurons (d) postganglionic parasympathetic neurons (e) all of these 7. The otic, ciliary, submandibular and pterygopalatine ganglia are located in the head region and contain _?_. (a) preganglionic sympathetic neurons (b) preganglionic parasympathetic neurons (c) postganglionic sympathetic neurons (d) postganglionic parasympathetic neurons (e) none of these 8. -

Of the Pediatric Mediastinum
MRI of the Pediatric Mediastinum Dianna M. E. Bardo, MD Director of Body MR & Co-Director of the 3D Innovation Lab Disclosures Consultant & Speakers Bureau – honoraria Koninklijke Philips Healthcare N V Author – royalties Thieme Publishing Springer Publishing Mediastinum - Anatomy Superior Mediastinum thoracic inlet to thoracic plane thoracic plane to diaphragm Inferior Mediastinum lateral – pleural surface anterior – sternum posterior – vertebral bodies Mediastinum - Anatomy Anterior T4 Mediastinum pericardium to sternum Middle Mediastinum pericardial sac Posterior Mediastinum vertebral bodies to pericardium lateral – pleural surface superior – thoracic inlet inferior - diaphragm Mediastinum – MR Challenges Motion Cardiac ECG – gating/triggering Breathing Respiratory navigation Artifacts Intubation – LMA Surgical / Interventional materials Mediastinum – MR Sequences ECG gated/triggered sequences SSFP – black blood SE – IR – GRE Non- ECG gated/triggered sequences mDIXON (W, F, IP, OP), eTHRIVE, turbo SE, STIR, DWI Respiratory – triggered, radially acquired T2W MultiVane, BLADE, PROPELLER Mediastinum – MR Sequences MRA / MRV REACT – non Gd enhanced Gd enhanced sequences THRIVE, mDIXON, mDIXON XD Mediastinum – Contents Superior Mediastinum PVT Left BATTLE: Phrenic nerve Vagus nerve Structures at the level of the sternal angle Thoracic duct Left recurrent laryngeal nerve (not the right) CLAPTRAP Brachiocephalic veins Cardiac plexus Aortic arch (and its 3 branches) Ligamentum arteriosum Thymus Aortic arch (inner concavity) Trachea Pulmonary -

The Sympathetic and the Parasympathetic Nervous System
The sympathetic and the parasympathetic nervous system Zsuzsanna Tóth, PhD Institute of Anatomy, Histology and Embryology Semmelweis University The role of the autonomic nervous system Claude Bernard • „milieu intérieur” concept; every organism lives in its internal environment that is constant and independent form the external environment Walter Bradford Cannon homeostasis; • an extension of the “milieu interieur” concept • consistence in an open system requires mechanisms that act to maintain that consistency • steady-state conditions require that any tendency toward change automatically meets with factors that resist that change • regulating systems that determine the homeostatic state : o autonomic nervous system ( sympathetic, parasympathetic, enteral) o endocrine system General structure of the autonomic nervous system craniosacral thoracolumbar Anatomy Neurotransmittersof the gut autonomic nervous system. symp. gangl pregangl. fiber pregangl. postgangl. fiber fiber (PoR) PoR enteral ganglion PoR PoR smooth muscle smooth muscle Kuratani S Development 2009;136:1585-1589 Sympathetic activation: Fight or flight reaction • energy mobilization • preparation for escape, or fight vasoconstriction • generalized Parasympathetic activation: adrenal • energy saving and restoring • „rest and digest” system • more localized vasoconstriction Paravertebral ganglia and the sympathetic chains pars cervicalis superius ganglion medium cervicale stellatum pars vertebrae • from the base of the skull to the caudal end thoracalis thoracalis of the sacrum • paravertebral ganglia (ganglia trunci sympathici) • rami interganglionares pars vertebrae • the two chains fuses at the ganglion impar abdominalis lumbalis sacrum pars pelvina foramen sacralia anteriora ganglion impar Anatomy of the cervical part of the sympathetic trunk superior cervical ganglion • behind the seath of the carotid, fusiform ggl. cervicale superius • IML T1-3 vegetative motoneurons- preganglionic fibers truncus symp. -
Nervous System Central Nervous System Peripheral Nervous System Brain Spinal Cord Sensory Division Motor Division Somatic Nervou
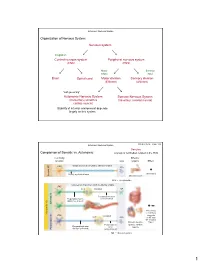
Autonomic Nervous System Organization of Nervous System: Nervous system Integration Central nervous system Peripheral nervous system (CNS) (PNS) Motor Sensory output input Brain Spinal cord Motor division Sensory division (Efferent) (Afferent) “self governing” Autonomic Nervous System Somatic Nervous System (Involuntary; smooth & (Voluntary; skeletal muscle) cardiac muscle) Stability of internal environment depends largely on this system Marieb & Hoehn – Figure 14.2 Autonomic Nervous System Ganglion: Comparison of Somatic vs. Autonomic: A group of cell bodies located in the PNS Cell body Effector location NTs organs Effect CNS Single neuron from CNS to effector organs ACh + Stimulatory Heavily myelinated axon Somatic NS Somatic Skeletal muscle ACh = Acetylcholine Two-neuron chain from CNS to effector organs CNS ACh Ganglion NE Postganglionic axon Preganglionic axon (unmyelinated) (lightly myelinated) Sympathetic + Stimulatory Autonomic NS Autonomic or inhibitory CNS Ganglion (depends ACh ACh on NT and NT receptor Smooth muscle, Type) Postganglionic glands, cardiac Preganglionic axon axon muscle Parasympathetic (lightly myelinated) (unmyelinated) NE = Norepinephrine 1 Autonomic Nervous System Organization of Nervous System: Nervous system Integration Central nervous system Peripheral nervous system (CNS) (PNS) Motor Sensory output input Brain Spinal cord Motor division Sensory division (Efferent) (Afferent) Autonomic Nervous System Somatic Nervous System (Involuntary; smooth & (Voluntary; skeletal muscle) cardiac muscle) Sympathetic division -

The Neuroanatomy of Female Pelvic Pain
Chapter 2 The Neuroanatomy of Female Pelvic Pain Frank H. Willard and Mark D. Schuenke Introduction The female pelvis is innervated through primary afferent fi bers that course in nerves related to both the somatic and autonomic nervous systems. The somatic pelvis includes the bony pelvis, its ligaments, and its surrounding skeletal muscle of the urogenital and anal triangles, whereas the visceral pelvis includes the endopelvic fascial lining of the levator ani and the organ systems that it surrounds such as the rectum, reproductive organs, and urinary bladder. Uncovering the origin of pelvic pain patterns created by the convergence of these two separate primary afferent fi ber systems – somatic and visceral – on common neuronal circuitry in the sacral and thoracolumbar spinal cord can be a very dif fi cult process. Diagnosing these blended somatovisceral pelvic pain patterns in the female is further complicated by the strong descending signals from the cerebrum and brainstem to the dorsal horn neurons that can signi fi cantly modulate the perception of pain. These descending systems are themselves signi fi cantly in fl uenced by both the physiological (such as hormonal) and psychological (such as emotional) states of the individual further distorting the intensity, quality, and localization of pain from the pelvis. The interpretation of pelvic pain patterns requires a sound knowledge of the innervation of somatic and visceral pelvic structures coupled with an understand- ing of the interactions occurring in the dorsal horn of the lower spinal cord as well as in the brainstem and forebrain. This review will examine the somatic and vis- ceral innervation of the major structures and organ systems in and around the female pelvis. -

Sympathetic Nervous System
Prof. Ahmed Fathalla Ibrahim Professor of Anatomy College of Medicine King Saud University E-mail: [email protected] OBJECTIVES At the end of the lecture, students should: . Define the autonomic nervous system. Describe the structure of autonomic nervous system . Trace the preganglionic & postganglionic neurons in both sympathetic & parasympathetic nervous system. Enumerate in brief the main effects of sympathetic & parasympathetic system DEFINITION Nerve cells located in both central & peripheral nervous system that are concerned with innervation of involuntary structures: viscera, smooth & cardiac muscles, glands. Function: maintains homeostasis of internal environment. Regulation: by hypothalamus. STRUCTURE OF AUTONOMIC NERVOUS SYSTEM SYMPATHETIC NERVOUS SYSTEM Cells of lateral horn of spinal cord (T1 – L3) Short axon .Cells of sympathetic chain .Cells of plexuses surrounding abdominal aorta (Coeliac, superior & inferior mesenteric) Long axon SYMPATHETIC NERVOUS SYSTEM SYMPATHETIC NERVOUS SYSTEM SYMPATHETIC NERVOUS SYSTEM Preganglionic sympathetic neurons: cells of the lateral horn of spinal cord in all thoracic + upper 3 lumbar segments. Preganglionic axons leave the spinal cord, join corresponding spinal nerves & reach the sympathetic chain (via the white ramus communicans). They either: 1. Synapse with cells of paravertebral ganglia located in sympathetic chain (postganglionic neurons are cells of paravertebral ganglia: postganglionic axons leave the sympathetic chain & join again the spinal nerve (via grey ramus communicans) to supply structures in head & thorax + blood vessels & sweat glands . SYMPATHETIC NERVOUS SYSTEM 2. Leave the sympathetic chain (without synapse) to reach coeliac & mesenteric plexuses (around branches of abdominal aorta) to synapse with their cells. Postganglionic neurons are cells of coeliac & mesenteric plexuses. Postganglionic axons supply abdominal & pelvic viscera. PARAVERTEBRAL GANGLIA They are interconnected to form 2 sympathetic chains, one on each side of vertebral column. -

Thoracic Anatomy Autonomic Nervous System
Thoracic anatomy Autonomic nervous system Thoracic Anatomy 3.G.1.1 James Mitchell (December 24, 2003) Autonomic nervous system Division by direction Visceral efferent Preganglionic myelinated, postganglionic unmyelinated Synapse in ganglia Visceral afferent Similar to somatic afferent Cell body in CNS, peripheral processes travel with autonomic and somatic fibres Division by outflow Sympathetic Thoracolumbar outflow: T1-L3 Synapse in sympathetic trunk ganglia or other ganglia near CNS Preganglionic cholinergic, postganglionic predominantly noradrenergic (also adrenergic, cholinergic sudomotor and purinergic) Parasympathetic Craniosacral outflow: III, VII, IX, X, S2-4 Synapse adjacent to end-organs Cranial nerve parasympathetic ganglia are traversed by other fibres but contain only parasympathetic synapses Parasympathetic anatomy III Edinger-Westphal nuclei → oculomotor n. → n. to inferior oblique → ciliary ganglion → short ciliary nn. → ciliary muscle and sphincter pupillae VII Superior salivatory nucleus → nervus intermedius → facial n. → chorda tympani → lingual n. → submandibular ganglion → submandibular and sublingual glands Geniculate ganglion → greater petrosal n. → pterygopalatine ganglion → zygomatic and lacrimal nerves to lacrimal gland and nasal and palatine branches to nasal mucosa XI Inferior salivatory nucleus → glossopharyngeal nerve → tympanic plexus → lesser petrosal n. → otic ganglion → auriculotemporal n. → parotid gland and oral mucosa X Dorsal nucleus of vagus → vagus n. → minute ganglia in respiratory tract, heart, -

Review of Sympathetic Blocks Anatomy, Sonoanatomy, Evidence, and Techniques
CHRONIC AND INTERVENTIONAL PAIN REVIEW ARTICLE Review of Sympathetic Blocks Anatomy, Sonoanatomy, Evidence, and Techniques Samir Baig, MD,* Jee Youn Moon, MD, PhD,† and Hariharan Shankar, MBBS*‡ Search Strategy Abstract: The autonomic nervous system is composed of the sympa- thetic and parasympathetic nervous systems. The sympathetic nervous sys- We performed a PubMed and MEDLINE search of all arti- tem is implicated in situations involving emergent action by the body and cles published in English from the years 1916 to 2015 using the “ ”“ ”“ additionally plays a role in mediating pain states and pathologies in the key words ultrasound, ultrasound guided, sympathetic block- ”“ ”“ body. Painful conditions thought to have a sympathetically mediated com- ade, sympathetically mediated pain, stellate ganglion block- ”“ ” “ ” ponent may respond to blockade of the corresponding sympathetic fibers. ade, celiac plexus blockade, , lumbar sympathetic blockade, “ ” “ ” The paravertebral sympathetic chain has been targeted for various painful hypogastric plexus blockade, and ganglion impar blockade. conditions. Although initially injected using landmark-based techniques, In order to capture the breadth of available evidence, because there fluoroscopy and more recently ultrasound imaging have allowed greater were only a few controlled trials, case reports were also included. visualization and facilitated injections of these structures. In addition to There were an insufficient number of reports to perform a system- treating painful conditions, sympathetic blockade has been used to improve atic review. Hence, we elected to perform a narrative review. perfusion, treat angina, and even suppress posttraumatic stress disorder symptoms. This review explores the anatomy, sonoanatomy, and evidence DISCUSSION supporting these injections and focuses on ultrasound-guided/assisted tech- nique for the performance of these blocks. -

Autonomic Nervous System ANS 1 Introduction
Autonomic Nervous System ANS 1 Introduction Control the visceral function = arterial pressure = gastrointestinal motility and secretion = urinary bladder emptying = sweating = body temperature Sympathetic • Divisions of ANS : Division Parasympathetic Division ANS: Preganglionic fibers Postganglionic fibers The Autonomic nervous system Activated by centers located in: • -the spinal cord • - brain stem • - hypothalamus • - the limbic cortex • - The Autonomic nervous system operates by means of visceral reflexes - The efferent Autonomic signals are transmitted to the body through two major subdivisions called - The sympathetic nervous system . - The parasympathetic nervous system. Sympathetic Division Physiological Anatomy of the sympathetic nervous system - two para vertebral sympathetic chains of ganglia in sides of the spinal column - two pre vertebral ganglia inside the abdomen and nervous extending from the ganglia to the different internal organs - the sympathetic nervous originate in the spinal cord between the segments T1 - L2 and pass from here first in to the sympathetic chain and then to the tissues and organs The cell body of each pre ganglion nervous lies in the inter media lateral from of the spinal cord , and its fibers passes through an anterior root of the cord and the spinal nerve. The pre ganglion sympathetic fibers leave the nerve and pass into one of the ganglia of the sympathetic chain Sympathetic Ganglia: A - Paravertebral or Sympathetic chain ganglia B - Prevertebral or Collateral ganglia C - Terminal or Peripheral -

THE MAIN PERIPHERAL CONNECTIONS of the HUMAN SYMPATHETIC NERVOUS SYSTEM by T
THE MAIN PERIPHERAL CONNECTIONS OF THE HUMAN SYMPATHETIC NERVOUS SYSTEM By T. K. POTTS, M.B., CH.M. (SYDNEY)1 BIIE recent investigation (5,7) of the functional significance of the sympathetic system by 1)r N. D). itoyle and Professor J. I. Hunter has revealed the necessity for a re-examination of the anatomy of the human sympathetic system. Ini particular the operations of ramisectioni (7, 8) devised by Dr Royle, in collabora- tion with Professor Hunter, call for a more exact determination of the precise position and topographical relations of the sympathetic cord and its ram? cotitnunicantes than at present is available. The dissection described ill this note was undertaken primarily to provide the surgeon with this guidance. In this matter, two regions stand out as having assumed an added interest ill the light of recent research. I refer to those regions associated with the operations known as cervical, and lumbar sympathetic ramisection, which are performed to remove the rigidity of the musculature of the extremities ill spastic paralysis (2,3,4,5, 7, 8, 9,10). As a description of the rari commnunicantes necessarily involves some mention of the arrangement of corresponding ganglia, this will be done in considering the various regions. To facilitate demonstration, the services of Miss D. Harrison were procured and, under my guidance, faithful repro- dluetions of the dissection were made by her. The dissection has been mounted, and placed in the Wilson. Museum of Anatomy, at the Medical School, Uni- versity of Sydney. The cervical portion of the sympathetic is characterized by the absence of segmental ganglia, and of white rami comnimunicantes. -

Sympathetic Tales: Subdivisons of the Autonomic Nervous System and the Impact of Developmental Studies Uwe Ernsberger* and Hermann Rohrer
Ernsberger and Rohrer Neural Development (2018) 13:20 https://doi.org/10.1186/s13064-018-0117-6 REVIEW Open Access Sympathetic tales: subdivisons of the autonomic nervous system and the impact of developmental studies Uwe Ernsberger* and Hermann Rohrer Abstract Remarkable progress in a range of biomedical disciplines has promoted the understanding of the cellular components of the autonomic nervous system and their differentiation during development to a critical level. Characterization of the gene expression fingerprints of individual neurons and identification of the key regulators of autonomic neuron differentiation enables us to comprehend the development of different sets of autonomic neurons. Their individual functional properties emerge as a consequence of differential gene expression initiated by the action of specific developmental regulators. In this review, we delineate the anatomical and physiological observations that led to the subdivision into sympathetic and parasympathetic domains and analyze how the recent molecular insights melt into and challenge the classical description of the autonomic nervous system. Keywords: Sympathetic, Parasympathetic, Transcription factor, Preganglionic, Postganglionic, Autonomic nervous system, Sacral, Pelvic ganglion, Heart Background interplay of nervous and hormonal control in particular The “great sympathetic”... “was the principal means of mediated by the sympathetic nervous system and the ad- bringing about the sympathies of the body”. With these renal gland in adapting the internal