Free Flap in Diabetic Foot Reconstruction
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

The Gracilis Musculocutaneous Flap As a Method of Closure of Ischial Pressure Sores: Preliminary Report
Paraplegia 20 (1982) 217-226 0031-1758/82/00010217 $02.00 © 1982 Internationalivledical Society of Paraplegia THE GRACILIS MUSCULOCUTANEOUS FLAP AS A METHOD OF CLOSURE OF ISCHIAL PRESSURE SORES: PRELIMINARY REPORT By JOHN C. MCGREGOR, F.R.C.S. Edenhall Hospital, Musselburgh and Bangour General Hospital, West Lothian, Scotland Abstract. Ischial pressure sores were treated by excision and repair with a gracilis musculocutaneous flap. The operative technique and results are discussed. Key words: Ischial pressure sore; Gracilis musculocutaneous flap. Introduction WHILE the majority of ischial pressure sores can be excised and closed directly, this is not invariably so as when they are large or when previous operations have failed. Conservative and non-operative measures can be employed but take time, and scarred tissue is less durable to further trauma (Conway & Griffith, I956). These authors recommended ischiectomy, biceps femoris muscle flap turned into the defect and a medially based thigh rotation flap. With the realisation of the potential value of incorporating muscle and overlying skin as a musculo- or myo-cutaneous flap in the last few years (McCraw et al., I977) it was not long before musculo cutaneous flap repair of ischial defects was described. Various muscles have been used in these flaps including gluteus maximus (Minami et al., 1977), biceps femoris (James & Moir, I980), hamstring muscles (Hagerty et al., 1980), and the gracilis muscle (McCraw et al., 1977; Bostwick et al., 1979; Labandter, 1980). The gracilis muscle is a flat, thin, accessory adductor of the thigh which is expendable, even in the non-paraplegic. It is situated superficially on the medial FIG. -

Thigh Muscles
Lecture 14 THIGH MUSCLES ANTERIOR and Medial COMPARTMENT BY Dr Farooq Khan Aurakzai PMC Dated: 03.08.2021 INTRODUCTION What are the muscle compartments? The limbs can be divided into segments. If these segments are cut transversely, it is apparent that they are divided into multiple sections. These are called fascial compartments, and are formed by tough connective tissue septa. Compartments are groupings of muscles, nerves, and blood vessels in your arms and legs. INTRODUCTION to the thigh Muscles The musculature of the thigh can be split into three sections by intermuscular septas in to; Anterior compartment Medial compartment and Posterior compartment. Each compartment has a distinct innervation and function. • The Anterior compartment muscle are the flexors of hip and extensors of knee. • The Medial compartment muscle are adductors of thigh. • The Posterior compartment muscle are extensor of hip and flexors of knee. Anterior Muscles of thigh The muscles in the anterior compartment of the thigh are innervated by the femoral nerve (L2-L4), and as a general rule, act to extend the leg at the knee joint. There are three major muscles in the anterior thigh –: • The pectineus, • Sartorius and • Quadriceps femoris. In addition to these, the end of the iliopsoas muscle passes into the anterior compartment. ANTERIOR COMPARTMENT MUSCLE 1. SARTORIUS Is a long strap like and the most superficial muscle of the thigh descends obliquely Is making one of the tendon of Pes anserinus . In the upper 1/3 of the thigh the med margin of it makes the lat margin of Femoral triangle. Origin: Anterior superior iliac spine. -

Complex Reconstructive Surgery for a Recurrent Ischial Pressure Ulcer with Contralateral Muscle
Weber et al. Plast Aesthet Res 2017;4:190-4 DOI: 10.20517/2347-9264.2017.73 Plastic and Aesthetic Research www.parjournal.net Case Report Open Access Complex reconstructive surgery for a recurrent ischial pressure ulcer with contralateral muscle Erin L. Weber1, Salah Rubayi1,2 1Division of Plastic and Reconstructive Surgery, Keck School of Medicine of the University of Southern California, Los Angeles, CA 90033, USA. 2Rancho Los Amigos National Rehabilitation Center, Downey, CA 90242, USA. Correspondence to: Dr. Salah Rubayi, Rancho Los Amigos National Rehabilitation Center, 7601 East Imperial Highway, Downey, CA 90242, USA. E-mail: [email protected] How to cite this article: Weber EL, Rubayi S. Complex reconstructive surgery for a recurrent ischial pressure ulcer with contralateral muscle. Plast Aesthet Res 2017;4:190-4. ABSTRACT Article history: The management of recurrent pressure ulcers is a frequent problem in patients with spinal Received: 19 Sep 2017 cord injuries. Many local muscle and fasciocutaneous flaps can be used to cover ulcers of all Accepted: 18 Oct 2017 sizes. However, when a recurrent pressure ulcer has been repeatedly addressed, the number of Published: 31 Oct 2017 available flaps becomes quite limited. Contralateral muscles, such as the gracilis, can be used to cover recurrent ischioperineal ulcers and should be employed before last resort surgeries, Key words: such as hip disarticulation and the total thigh flap. Pressure ulcer, recurrent, gracilis, muscle, contralateral INTRODUCTION risk of serious infection or sepsis. Therefore, pressure ulcers, and the constant attention required to prevent Spinal cord injury predisposes patients to additional them, represent a significant lifetime burden for patients medical complications. -

Lower Gluteal Muscle Flap and Buttock Fascio-Cutaneous Rotation Flap For
PRAS3334_proof ■ 31 July 2012 ■ 1/6 + MODEL Journal of Plastic, Reconstructive & Aesthetic Surgery (2012) xx,1e6 1 63 2 64 3 65 4 66 5 67 6 68 7 69 8 70 9 71 10 72 11 73 12 Lower gluteal muscle flap and buttock 74 13 75 14 fascio-cutaneous rotation flap for reconstruction 76 15 77 16 78 17 of perineal defects after abdomino-perineal 79 18 80 19 resections 81 20 82 21 83 a, a a b 22 Q2 B.K. Tan *, Goh Terence , C.H. Wong , Sim Richard 84 23 85 24 86 25 a Department of Plastic, Reconstructive and Aesthetic Surgery, Singapore General Hospital, Outram Road, Singapore, 87 26 Singapore 88 27 b Department of General Surgery, Tan Tock Seng Hospital, Singapore, Singapore 89 28 90 29 91 30 Received 10 October 2011; accepted 17 July 2012 92 31 93 32 94 33 95 34 96 35 KEYWORDS Summary Background: Abdomino-perineal resection (APR) in the treatment of anal and low 97 36 Abdomino-perineal; rectal cancers is associated with perineal wound problems, especially after pre-operative 98 37 APR; radiotherapy. Immediate reconstruction of defects after APR with flaps has been shown to 99 38 Gluteus maximus; reduce postoperative morbidity. The combined gluteal muscle and buttock fascio-cutaneous 100 39 Reconstruction rotation flap is useful for this purpose. The dual blood supply of the gluteus maximus muscle 101 40 allows it to be split into superior and inferior halves. The inferior fibres are used to fill the 102 41 pelvic cavity, whilst the superior fibres are preserved to maintain hip function. -

Snapping Pes Anserinus Caused by Gracilis Tendon: a New Mechanism
J Korean Soc Radiol 2019;80(5):969-974 Case Report https://doi.org/10.3348/jksr.2019.80.5.969 pISSN 1738-2637 / eISSN 2288-2928 Received July 19, 2018 Revised October 4, 2018 Accepted December 19, 2018 Snapping Pes Anserinus *Corresponding author Tae Eun Kim, MD Department of Radiology, Daegu Fatima Hospital, Caused By Gracilis Tendon: 99 Ayang-ro, Dong-gu, Daegu 41199, Korea. A New Mechanism Proposed Tel 82-53-940-7161 Fax 82-53-954-7417 by Dynamic Knee E-mail [email protected] This is an Open Access article distributed under the terms of the Creative Commons Attribu- Ultrasonography tion Non-Commercial License 두덩정강건에 의해서 발생하는 거위발 근육의 퉁김현상: (https://creativecommons.org/ licenses/by-nc/4.0) which permits 역동적 무릎 초음파 검사에 근거한 새로운 기전 unrestricted non-commercial use, distribution, and reproduc- tion in any medium, provided the Hyun Seok Oh, MD , Tae Eun Kim, MD* original work is properly cited. Department of Radiology, Daegu Fatima Hospital, Daegu, Korea ORCID iDs Tae Eun Kim https:// Snapping pes anserinus is the main extra-articular cause of snapping on the medial side of the orcid.org/0000-0002-9874-0247 Hyun Seok Oh knee. There are limited articles that describe the mechanism of the condition, especially only https:// when flexion of the knee. We report a case of snapping pes anserinus in a 23-year-old skier, which orcid.org/0000-0003-0036-2792 was reproduced on only active flexion of both knees in the posteromedial aspect of the tibia, with pain for 6 years, diagnosed using dynamic ultrasonography for elucidating a new mecha- nism of the gracilis tendon. -

Download PDF File
Folia Morphol. Vol. 77, No. 1, pp. 138–143 DOI: 10.5603/FM.a2017.0069 O R I G I N A L A R T I C L E Copyright © 2018 Via Medica ISSN 0015–5659 www.fm.viamedica.pl Anatomy and morphometry of the distal gracilis muscle tendon in adults and foetuses D.W. Dziedzic, U. Bogacka, I. Komarniţki, B. Ciszek Department of Descriptive and Clinical Anatomy, Centre of Biostructure Research, Medical University of Warsaw, Poland [Received: 18 January 2017; Accepted: 27 April 2017] Ten human gracilis muscles obtained from adults and ten gracilis muscles col- lected from human foetuses between the 15th and 21st week of gestation were examined. The results of this preparatory study show that the gracilis muscle in adults is narrow and long — 482 mm on average. The distal tendon of gracilis muscle is long, 294 mm on average. It can be divided into two sections — external part, outside the muscle belly, and internal, intramuscular, part. The latter one is partially covered by muscle fibres and some of it is completely hidden inside the muscle belly, which is on average 76 mm long. Presence of an intramuscular part of the distal tendon was also demonstrated in the foetal material. Moreover, very strong correlations between particular muscle lengths were noted in foetuses. (Folia Morphol 2018; 77, 1: 138–143) Key words: gracilis, pes anserinus, foetal muscle, tendon INTRODUCTION Several accessory bundles, usually 3–5, may The gracilis muscle is located on the medial side emerge from the tendon at the distal end. They may of the thigh. -
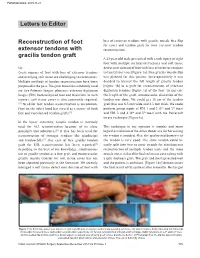
Reconstruction of Foot Extensor Tendons with Gracilis Tendon Graft Letters to Editor
Published online: 2019-11-21 Letters to Editor loss of extensor tendons with gracilis muscle free flap Reconstruction of foot for cover and tendon graft for foot extensor tendon extensor tendons with reconstruction. gracilis tendon graft A 22-year-old male presented with crush injury of right foot with multiple metatarsal fractures and soft tissue Sir, defect over dorsum of foot with loss of extensor tendons Crush injuries of foot with loss of extensor tendons to lateral four toes [Figure 1a]. Free gracilis muscle flap and overlying soft tissue are challenging to reconstruct. was planned for this patient. Intra-operatively it was Multiple methods of tendon reconstruction have been decided to harvest the full length of gracilis tendon proposed in the past. The graft materials commonly used [Figure 1b] as a graft for reconstruction of extensor are free Palmaris longus, plantaris, extensor digitorum digitorum tendons [Figure 1c] of the foot. To increase longus (EDL) from uninjured foot and fascia lata. In such the length of the graft, intramuscular dissection of the injuries, soft tissue cover is also commonly required. tendon was done. We could get 16 cm of the tendon [1,2] Need for foot tendon reconstruction is uncommon. graft that was 6.5 mm wide and 2.5 mm thick. We could Foot on the other hand has served as a source of both perform group repair of EDL 1 and 2 (2nd and 3rd toes) free and vascularised tendon grafts.[3] and EDL 3 and 4 (4th and 5th toes) with the Pulvertuft weave technique [Figure1c]. In the lower extremity, Gracilis tendon is routinely used for ACL reconstruction because of its close This technique in our openion is simpler and more proximity and robustness.[4] It also has been used for logical as violation of the other donor site for harvesting reconstruction of stronger tendons like quadriceps the tendon is avoided. -
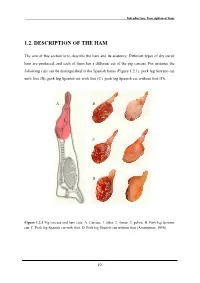
1.2. Description of the Ham
Introduction: Description of ham 1.2. DESCRIPTION OF THE HAM The aim of this section is to describe the ham and its anatomy. Different types of dry cured ham are produced, and each of them has a different cut of the pig carcass. For instance the following cuts can be distinguished in the Spanish hams (Figure 1.2.1): pork leg Serrano cut with foot (B), pork leg Spanish cut with foot (C), pork leg Spanish cut without foot (D). A B 1 2 C 3 D Figure 1.2.1 Pig carcass and ham cuts. A. Carcass. 1. tibia. 2. femur. 3. pelvis. B. Pork leg Serrano cut. C. Pork leg Spanish cut with foot. D. Pork leg Spanish cut without foot (Anomymus, 1996). 10 Introduction: Description of ham The ham can be divided in the muscular part, the bones and the skin. None of this parts are removed for the processing of the traditional dry-cured ham. The following muscles can be distinguished (Figure 1.2.2): The Gracilis muscle is a thin sheet of muscle spread over the medial face of the hindlimb. The Quadriceps femoris muscles form a group of four large muscles that pull on the patella when the leg is extended. The Vastus medialis is medial, the Vastus lateralis is lateral and the Vastus intermedius that covers the anterior face of the femur. The Recturs femoris covers the Vastus intermedius. The Biceps femoris is a single large muscle on the lateral face of the hindlimb. The Semitendinosus and Semimebranosus are two large muscles located on the posterior face of the hindlimb. -

Use of Gracilis Muscle Free Flap for Reconstruction of Chronic Osteomyelitis of Foot and Ankle
USE OF GRACILIS MUSCLE FREE FLAP FOR RECONSTRUCTION OF CHRONIC OSTEOMYELITIS OF FOOT AND ANKLE P. LORÉA, N. VERCRUYSSE, B. C. COESSENS Despite low donor-site morbidity and a straight- Mots-clés : gracilis ; ostéomyélite ; cheville ; pied ; forward dissection, the gracilis muscle flap is still for lambeau libre. many surgeons a second choice in microsurgical reconstruction of the lower extremity in cases of osteomyelitis. They underscore the difficulty of the procedure, and the problems of insufficient muscle INTRODUCTION volume and a small sized vascular pedicle. The aim of this study was to assess the reliability of the gracilis Free-tissue transfer has greatly increased our muscle free flap in the treatment of osteomyelitis of the foot and ankle. ability to cover all soft tissue defects and to sterili- Between 1992 and 1999, 12 consecutive cases (age 9 ze septic bone cavities, but some debate continues to 71 years) of osteomyelitis of the foot and ankle between the proponents of skin flaps (19, 26, 29) were treated using a skin-grafted gracilis free muscle and skin-grafted muscle flaps (18, 21, 30) for the flap. Criteria for osteomyelitis were the presence of weight-bearing area. Free muscle flaps are an exposed bone, positive cultures and bone scans. The effective method for the reconstruction of deep wound defect surface ranged from 9 to 90 cm2 (mean three-dimensional defects, especially in cases 50.5 cm2). Six flaps were applied on the weight bear- where there is evidence of chronic osteomye- ing area of the foot. Flap harvesting time never litis (7). Among skin-grafted muscle flaps, the latis- exceeded 30 minutes. -
Gracilis Muscle Transplant (Free Flap)
FACIAL REANIMATION: GRACILIS MUSCLE TRANSPLANT (FREE FLAP) Thank you for choosing the Johns Hopkins Facial Plastic and Reconstructive Surgery Center for your upcoming surgery. We want you to have the best and safest experience possible. If you have any questions or concerns, please do not hesitate to contact our office. We look forward to helping you achieve your goals! Important Phone Numbers Office/Appointments: (877) 546-4530 or (410) 464-6713 Lou Ellen Michel, R.N.: (410) 583-7183 Evenings/Weekends Emergency: (410) 955-5000 – please ask for the ENT resident on-call General Information Chronic Facial Paralysis: In patients with long-term facial paralysis (more than 1-2 years), the native muscles in the face unfortunately irreversibly lose their function. Therefore, a new muscle must be used in order to restore smile and lower face movement. Gracilis Muscle Transplant (Free Flap): The gracilis muscle is located in the inner aspect of the thigh. A small portion of this muscle – with its blood supply (artery and vein) and nerve – can be transplanted in the face to replace the facial muscles that allow you to smile. Using highly specialized microsurgical techniques, the gracilis muscle’s artery and vein are attached to an artery and vein in the head/neck region. This connection is critical for the muscle to survive in its new environment in the face. The nerve that moves the gracilis muscle (obturator nerve) must then be attached to a new nerve supply in the face, in order to power the muscle to move. Nerve Options to Power the Gracilis Muscle: The three most common options are described below. -

Minimally Invasive Medial Hip Approach
Orthopaedics & Traumatology: Surgery & Research 100 (2014) 687–689 View metadata, citation and similar papers at core.ac.uk brought to you by CORE provided by Elsevier - Publisher Connector Available online at ScienceDirect www.sciencedirect.com Technical note Minimally invasive medial hip approach ∗ P. Chiron , J. Murgier , E. Cavaignac , R. Pailhé , N. Reina Service d’orthopédie-traumatologie, institut de l’appareil locomoteur, cinquième étage, hôpital Pierre-Paul-Riquet, 308, avenue de Grande-Bretagne, 31059 Toulouse, France a r t i c l e i n f o a b s t r a c t Article history: The medial approach to the hip via the adductors, as described by Ludloff or Ferguson, provides restricted Accepted 12 June 2014 visualization and incurs a risk of neurovascular lesion. We describe a minimally invasive medial hip approach providing broader exposure of extra- and intra-articular elements in a space free of neurovas- Keywords: cular structures. With the lower limb in a “frog-leg” position, the skin incision follows the adductor longus Minimally invasive surgery for 6 cm and then the aponeurosis is incised. A slide plane between all the adductors and the aponeurosis Hip approach is easily released by blunt dissection, with no interposed neurovascular elements. This gives access to Adductors the lesser trochanter, psoas tendon and inferior sides of the femoral neck and head, anterior wall of the Iliopsoas acetabulum and labrum. We report a series of 56 cases, with no major complications: this approach allows Fracture treatment of iliopsoas muscle lesions and resection or filling of benign tumors of the cervical region and Foreign body Tumor enables intra-articular surgery (arthrolysis, resection of osteophytes or foreign bodies, labral suture). -

Obturator Sling
132 Whiteside J1, Walters M1 1. The Cleveland Clinic Foundation ANATOMY OF THE OBTURATOR REGION: RELATIONS TO A TRANS- OBTURATOR SLING Aims of Study Recently a new anti-incontinence procedure has been introduced that approaches placement of a mid-urethral polypropylene tape via the obturator foramen. The anticipated advantages of this new approach are lessened bowel, vascular, and bladder injury relative to either the “top-down” or traditional “bottom-up” tape placement techniques that both pass through the space of Retzius. As has been demonstrated with the Tension Free Vaginal Tape (TVT), understanding of the relevant anatomy is paramount to avoidance of operative injury; knowledge of the anatomy of the obturator region likewise should be understood. Given the paucity of information on the anatomy of the obturator region, particularly approached from the perineum, we sought to better define this anatomy with particular emphasis on describing the course of any device passed through the obturator foramen to treat urinary incontinence. Methods Five fresh frozen cadavers were dissected bilaterally in the dorsal supine lithotomy position. Dissection was performed from both an abdominal approach and a perineal approach exposing the space of Retzius abdominally and the thigh musculature. Careful identification of all relevant vascular and nerve structures was done with measurements made from these structures and established soft tissue and bony landmarks. A curved needle was passed from the inner thigh through the obturator foramen to the lateral vagina at the level of the mid- urethra. Measurements were done between the needle and important nerve and vascular structures. Summary statistics were done. Photographs and drawings demonstrated important relationships.