(2) October 2011\Protocol Book\Program-Speaker Page-Oc
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Program Md Dermatology
PROGRAM MD DERMATOLOGY (Revised with effect from 2015-2016 onwards) MD Dermatology 1 Contents Goal ....................................................................................................................................... 3 Objectives to be achieved by an individual at the end of 3 years of training ........................ 3 Programme outcomes ............................................................................................................ 4 Programme specific outcomes ............................................................................................... 5 Tentative schedule for three years of md training ................................................................. 5 Topics related to allied basic sciences ................................................................................... 7 Assessments/ examinations ................................................................................................. 12 Final examination ................................................................................................................ 12 Theory syllabus .................................................................................................................... 13 Fundamentals of cutaneous diagnosis- ................................................................................ 13 Tumours ............................................................................................................................... 14 Disorders of pigmentation .................................................................................................. -

Clinical Dermatology Notice
This page intentionally left blank Clinical Dermatology Notice Medicine is an ever-changing science. As new research and clinical experience broaden our knowledge, changes in treatment and drug therapy are required. The editors and the publisher of this work have checked with sources believed to be reliable in their efforts to provide information that is complete and generally in accord with the standards accepted at the time of publication. However, in view of the possibility of human error or changes in medical sciences, neither the editors nor the publisher nor any other party who has been involved in the preparation or publication of this work warrants that the information contained herein is in every respect accurate or complete, and they disclaim all responsibility for any errors or omissions or for the results obtained from use of such information contained in this work. Readers are encouraged to confirm the information contained herein with other sources. For example and in particular, readers are advised to check the product information sheet included in the package of each drug they plan to administer to be certain that the information contained in this work is accurate and that changes have not been made in the recommended dose or in the contraindications for administration. This recommendation is of particular importance in connection with new or infrequently used drugs. a LANGE medical book Clinical Dermatology Carol Soutor, MD Clinical Professor Department of Dermatology University of Minnesota Medical School Minneapolis, Minnesota Maria K. Hordinsky, MD Chair and Professor Department of Dermatology University of Minnesota Medical School Minneapolis, Minnesota New York Chicago San Francisco Lisbon London Madrid Mexico City Milan New Delhi San Juan Seoul Singapore Sydney Toronto Copyright © 2013 by McGraw-Hill Education, LLC. -

Discrete Papular Dermal Mucinosis with Hashimoto Thyroiditis: a Case Report
Discrete Papular Dermal Mucinosis With Hashimoto Thyroiditis: A Case Report Ilgen Ertam, MD; Nezih Karaca, MD; Can Ceylan, MD; Alican Kazandi, MD; Sibel Alper, MD The cutaneous focal mucinoses are a group of neck. During this time, the patient was being followed connective tissue disorders characterized by by the rheumatology department for fibromyalgia and deposition of mucin found either focally or dif- connective tissue disorder. Because of the cutaneous fusely in the dermis. A 47-year-old woman pre- lesions, she was sent for dermatologic evaluation. sented with asymptomatic flesh-colored papules There was no history of preceding trauma or insect on the neck, inguinal area, intergluteal area, bites. The patient had undergone a subtotal thyroid- vulvar area, and extremities of 5 months’ dura- ectomy 21 years prior but had not used any thyroid tion. There was no history of preceding trauma or medication before she was referred to our clinic. insect bites. The patient had undergone a subto- During dermatologic examination, we found flesh- tal thyroidectomy 21 years prior but had not used colored, well-defined, smooth papules that measured any thyroid medication before she was referred to approximately 1.531 cm in size on the genital region, our clinic. Thyroid ultrasonographyCUTIS was consistent fingers, face, and scalp. The lesions extended from with Hashimoto thyroiditis. During dermatologic the labium majus and labium minus to the interglu- examination, flesh-colored, well-defined, smooth teal and coccygeal region (Figures 1–3). They also papules that measured approximately 1.531 cm appeared symmetrically at the level of the anterior in size on the genital region, fingers, face, and femoral region and on the dorsal and palmar areas of scalp were seen. -

Cutaneous Manifestations of Systemic Disease
Cutaneous Manifestations of Systemic Disease Dr. Lloyd J. Cleaver D.O. FAOCD FAAD Northeast Regional Medical Center A.T.Still University/KCOM Assistant Vice President/Professor ACOI Board Review Disclosure I have no financial relationships to disclose I will not discuss off label use and/or investigational use in my presentation I do not have direct knowledge of AOBIM questions I have been granted approvial by the AOA to do this board review Dermatology on the AOBIM ”1-4%” of exam is Dermatology Table of Test Specifications is unavailable Review Syllabus for Internal Medicine Large amount of information Cutaneous Multisystem Cutaneous Connective Tissue Conditions Connective Tissue Diease Discoid Lupus Erythematosus Subacute Cutaneous LE Systemic Lupus Erythematosus Scleroderma CREST Syndrome Dermatomyositis Lupus Erythematosus Spectrum from cutaneous to severe systemic involvement Discoid LE (DLE) / Chronic Cutaneous Subacute Cutaneous LE (SCLE) Systemic LE (SLE) Cutaneous findings common in all forms Related to autoimmunity Discoid LE (Chronic Cutaneous LE) Primarily cutaneous Scaly, erythematous, atrophic plaques with sharp margins, telangiectasias and follicular plugging Possible elevated ESR, anemia or leukopenia Progression to SLE only 1-2% Heals with scarring, atrophy and dyspigmentation 5% ANA positive Discoid LE (Chronic Cutaneous LE) Scaly, atrophic plaques with defined margins Discoid LE (Chronic Cutaneous LE) Scaly, erythematous plaques with scarring, atrophy, dyspigmentation DISCOID LUPUS Subacute Cutaneous -
Copyrighted Material
1 Index Note: Page numbers in italics refer to figures, those in bold refer to tables and boxes. References are to pages within chapters, thus 58.10 is page 10 of Chapter 58. A definition 87.2 congenital ichthyoses 65.38–9 differential diagnosis 90.62 A fibres 85.1, 85.2 dermatomyositis association 88.21 discoid lupus erythematosus occupational 90.56–9 α-adrenoceptor agonists 106.8 differential diagnosis 87.5 treatment 89.41 chemical origin 130.10–12 abacavir disease course 87.5 hand eczema treatment 39.18 clinical features 90.58 drug eruptions 31.18 drug-induced 87.4 hidradenitis suppurativa management definition 90.56 HLA allele association 12.5 endocrine disorder skin signs 149.10, 92.10 differential diagnosis 90.57 hypersensitivity 119.6 149.11 keratitis–ichthyosis–deafness syndrome epidemiology 90.58 pharmacological hypersensitivity 31.10– epidemiology 87.3 treatment 65.32 investigations 90.58–9 11 familial 87.4 keratoacanthoma treatment 142.36 management 90.59 ABCA12 gene mutations 65.7 familial partial lipodystrophy neutral lipid storage disease with papular elastorrhexis differential ABCC6 gene mutations 72.27, 72.30 association 74.2 ichthyosis treatment 65.33 diagnosis 96.30 ABCC11 gene mutations 94.16 generalized 87.4 pityriasis rubra pilaris treatment 36.5, penile 111.19 abdominal wall, lymphoedema 105.20–1 genital 111.27 36.6 photodynamic therapy 22.7 ABHD5 gene mutations 65.32 HIV infection 31.12 psoriasis pomade 90.17 abrasions, sports injuries 123.16 investigations 87.5 generalized pustular 35.37 prepubertal 90.59–64 Abrikossoff -

Self-Assessment Answers Cases 1 - 15
Self-Assessment Answers Cases 1 - 15 Chairs: Richard Carr (UK) Rossitza Lazova (USA) Self Assessment Preçis XXXVIII Symposium of the International Society of Dermatopathology, Glasgow, 28-30 September 2017 Self-Assessment Answers Part 1 – Friday 29th September 2017 No Time First Name Surname Country Selected Cases Page 1 16:20 Mona Abdel-Halim Egypt Fluoroscopy: radiodermatitis 3 2 16:26 Asha Kubba India Papulonecrotic tuberculid 5 3 16:32 Doina Ivan USA Crystaloglobulinemia 6 4 16:38 Francisco Bravo Peru Gnathosmiasis 7 5 16:44 Jose Cardoso Portugal Acral persistent papular mucinosis 9 6 16:50 Agnes Carlotti France Anaplastic Kaposi's Sarcoma 11 7 16:56 Benedicte Cavalier-Balloy France Acantholytic extrammary genital Pagets disease 12 8 17:02 Heung Chong UK Plaque like myofibroblastic tumour of infancy 14 9 17:08 David Cassarino USA Mycoplasma induced rash & mucositis syndrome 15 (EM-like) 10 17:14 Reem El Bahtimi Dubai Cutaneous lymphadenoma 16 11 17:20 Lydia Essary USA Primary cutaneous coccidiodomycosis 18 12 17:26 Maxwell Fung USA Sclerodermoid GVHD w cutaneous amyloid 19 13 17:32 Anjela Galan USA Granuloma-annulare-like mets. Breast 20 14 17:38 Joerg Schaller Germany Randalls disease (non-amyloid light chains) 22 15 17:44 Katrin Kerl Switzerland Lavamisol induced occlusive vasculitis 24 2 Self Assessment Preçis XXXVIII Symposium of the International Society of Dermatopathology, Glasgow, 28-30 September 2017 Case 1 Mona R.E. Abdel-Halim, MD, Dip Dermpath (ICDP-UEMS) DIAGNOSIS FLOUROSCOPY INDUCED CHRONIC RADIODERMATITIS Clinical Summary: A 66-year-old male patient presented with a well defined square shaped indurated/sclerotic focally ulcerated plaque with atrophic areas on the right sub-scapular area of 2 years duration. -

Reticular Erythematous Mucinosis: a Rare Cutaneous Mucinosis Amer Ali Almohssen1, Ragha Vasantha Suresh2,Robert A
Acta Dermatovenerol Croat 2019;27(1):16-21 REVIEW Reticular Erythematous Mucinosis: A Rare Cutaneous Mucinosis Amer Ali Almohssen1, Ragha Vasantha Suresh2,Robert A. Schwartz2 1Dermatopathology, State University of New York Downstate Medical School & The Ackerman Academy of Dermatopathology New York City, NY, USA; 2Dermatology and Pathology, Rutgers New Jersey Medical School, Newark, New Jersey, USA Corresponding Author ABSTracT Reticular erythematous mucinosis (REM) is a rare form of pri- Amer Ali Almohssen, MD mary cutaneous mucinosis, most often involving the midline of the upper chest or back in middle-aged women. REM bears clinical and histopatho- Dermatopathology Fellow, State University logic resemblance to lupus erythematosus tumidus (LET), dermatomyosi- of New York tis, scleredema, and lichen myxedematosus. Early recognition and diagno- Downstate Medical School & The Ackerman sis of REM is particularly relevant to exclude the abovementioned diseases, as REM is more benign and has fewer systemic consequences. Academy of Dermatopathology New York City KEY WORDS: reticular erythematous mucinosis, lupus erythematous tu- New York midus, scleredema, dermatomyositis, lichen myxedematosus, papular mu- USA cinosis [email protected] Received: December 27, 2017 Accepted: February 9, 2019 INTRODUCTION The cutaneous mucinoses are a diverse group of pathologic resemblance to lupus erythematosus tu- disorders in which elevated levels of mucin are found midus (LET), dermatomyositis, scleredema, and pap- in the skin, predominantly in the dermis (1). The pri- ular mucinosis. However, recent evidence supports mary cutaneous mucinoses are characterized by mu- the recognition of REM as a distinct entity, based on cin deposition as the major histological feature, and its distinctive clinical and histologic features of this include scleromyxedema, scleredema, and lichen disorder. -

Discrete Papular Mucinosis: a Rare Subtype of Lichen Myxedematosus Wongsiya Viarasilpa MD, Wareeporn Disphanurat MD
198 Case report Thai J Dermatol, October-December, 2019 Discrete papular mucinosis: A rare subtype of lichen myxedematosus Wongsiya Viarasilpa MD, Wareeporn Disphanurat MD. ABSTRACT: VIARASILPA W, DISPHANURAT W. DISCRETE PAPULAR MUCINOSIS: A RARE SUBTYPE OF LICHEN MYXEDEMATOSUS. THAI J DERMATOL 2019; 35: 198-205. DIVISION OF DERMATOLOGY, DEPARTMENT OF MEDICINE, FACULTY OF MEDICINE, THAMMASAT UNIVERSITY, PATHUMTHANI, THAILAND. Lichen myxedematosus is a chronic, progressive idiopathic cutaneous mucinosis characterized by localized or generalized papular eruption of unknown etiology in which mucin deposition in the dermis is the distinctive histologic feature. The classification system was revised into three clinicopathological subsets, localized lichen myxedematosus, scleromyxedema and atypical forms of lichen myxedematosus. We report a rare subtype of lichen myxedematosus, discrete papular subtype, presented with papular eruption on the back, chest, face and neck. Histopathology showed focal mucin accumulation in upper and mid reticular dermis with scattered stellate fibroblasts among mucinous material, confirmed by Alcian blue staining. Her serum protein electrophoresis showed polyclonal immunoglobulin, serology for hepatitis C and HIV were negative and her thyroid function test was normal. She was diagnosed with localized forms of lichen myxedematosus, discrete papular subtype and was treated with an excellent response to topical corticosteroids and oral hydroxychloroquine combination therapy. Key words: lichen myxedematosus, papular mucinosis, skin-colored papules From: Division of dermatology, Department of Medicine, Faculty of Medicine, Thammasat University, Pathumthani, Thailand Corresponding author: Wareeporn Disphanurat MD, email: [email protected] Received: 2 April 2019 Revised: 23 September 2019 Accepted: 6 November 2019 Vol.35 No.4 Viarasilpa W and Disphanurat W 199 myxedematosus is a rare entity and has less prevalence than scleromyxedema4, 6-12. -
Dermatological Indications of Disease - Part II This Patient on Dialysis Is Showing: A
“Cutaneous Manifestations of Disease” ACOI - Las Vegas FR Darrow, DO, MACOI Burrell College of Osteopathic Medicine This 56 year old man has a history of headaches, jaw claudication and recent onset of blindness in his left eye. Sed rate is 110. He has: A. Ergot poisoning. B. Cholesterol emboli. C. Temporal arteritis. D. Scleroderma. E. Mucormycosis. Varicella associated. GCA complex = Cranial arteritis; Aortic arch syndrome; Fever/wasting syndrome (FUO); Polymyalgia rheumatica. This patient missed his vaccine due at age: A. 45 B. 50 C. 55 D. 60 E. 65 He must see a (an): A. neurologist. B. opthalmologist. C. cardiologist. D. gastroenterologist. E. surgeon. Medscape This 60 y/o male patient would most likely have which of the following as a pathogen? A. Pseudomonas B. Group B streptococcus* C. Listeria D. Pneumococcus E. Staphylococcus epidermidis This skin condition, erysipelas, may rarely lead to septicemia, thrombophlebitis, septic arthritis, osteomyelitis, and endocarditis. Involves the lymphatics with scarring and chronic lymphedema. *more likely pyogenes/beta hemolytic Streptococcus This patient is susceptible to: A. psoriasis. B. rheumatic fever. C. vasculitis. D. Celiac disease E. membranoproliferative glomerulonephritis. Also susceptible to PSGN and scarlet fever and reactive arthritis. Culture if MRSA suspected. This patient has antithyroid antibodies. This is: • A. alopecia areata. • B. psoriasis. • C. tinea. • D. lichen planus. • E. syphilis. Search for Hashimoto’s or Addison’s or other B8, Q2, Q3, DRB1, DR3, DR4, DR8 diseases. This patient who works in the electronics industry presents with paresthesias, abdominal pain, fingernail changes, and the below findings. He may well have poisoning from : A. lead. B. -

Flesh-Colored Papular Eruption
DERMATOPATHOLOGY DIAGNOSIS CLOSE ENCOUNTERS WITH THE ENVIRONMENT Flesh-Colored Papular Eruption Vanessa B. Voss, MD; Claudia I. Vidal, MD, PhD Eligible for 1 MOC SA Credit From the ABD This Dermatopathology Diagnosis article in our print edition is eligible for 1 self-assessment credit for Maintenance of Certification from the American Board of Dermatology (ABD). After completing this activity, diplomates can visit the ABD website (http://www.abderm.org) to self-report the credits under the activity title “Cutis Dermatopathology Diagnosis.” You may report the credit after each activity is completed or after accumu- lating multiple credits. A 48-year-old black man presented with a rash of 7 months’ duration that started on the face and spread to the body. He had extreme pruritus, increased stiffness in the hands and joints,copy and paresthesia. Physical examination revealed an eruption of 2- to 4-mm, flesh-colored papules with follicu- lar accentuation on the face, neck, bilateral uppernot extremities, back, and thighs. Do H&E, original magnification ×100. The best diagnosis is: a. infundibulofolliculitis b. interstitial granulomaCUTIS annulare c. papular mucinosis/scleromyxedema d. reticular erythematous mucinosis e. scleredema PLEASE TURN TO PAGE 362 FOR DERMATOPATHOLOGY DIAGNOSIS DISCUSSION From Saint Louis University, Missouri. Dr. Voss is from the School of Medicine. Dr. Vidal is from the Department of Dermatology. The authors report no conflict of interest. Correspondence: Claudia I. Vidal, MD, PhD, Department of Dermatology, Anheuser-Busch Institute, 4th Floor, Room 402, 1755 S Grand Blvd, St Louis, MO 63104 ([email protected]). WWW.CUTIS.COM VOLUME 98, DECEMBER 2016 361 Copyright Cutis 2016. -
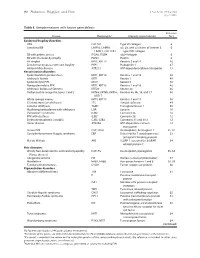

Table I. Genodermatoses with Known Gene Defects 92 Pulkkinen
92 Pulkkinen, Ringpfeil, and Uitto JAM ACAD DERMATOL JULY 2002 Table I. Genodermatoses with known gene defects Reference Disease Mutated gene* Affected protein/function No.† Epidermal fragility disorders DEB COL7A1 Type VII collagen 6 Junctional EB LAMA3, LAMB3, ␣3, 3, and ␥2 chains of laminin 5, 6 LAMC2, COL17A1 type XVII collagen EB with pyloric atresia ITGA6, ITGB4 ␣64 Integrin 6 EB with muscular dystrophy PLEC1 Plectin 6 EB simplex KRT5, KRT14 Keratins 5 and 14 46 Ectodermal dysplasia with skin fragility PKP1 Plakophilin 1 47 Hailey-Hailey disease ATP2C1 ATP-dependent calcium transporter 13 Keratinization disorders Epidermolytic hyperkeratosis KRT1, KRT10 Keratins 1 and 10 46 Ichthyosis hystrix KRT1 Keratin 1 48 Epidermolytic PPK KRT9 Keratin 9 46 Nonepidermolytic PPK KRT1, KRT16 Keratins 1 and 16 46 Ichthyosis bullosa of Siemens KRT2e Keratin 2e 46 Pachyonychia congenita, types 1 and 2 KRT6a, KRT6b, KRT16, Keratins 6a, 6b, 16, and 17 46 KRT17 White sponge naevus KRT4, KRT13 Keratins 4 and 13 46 X-linked recessive ichthyosis STS Steroid sulfatase 49 Lamellar ichthyosis TGM1 Transglutaminase 1 50 Mutilating keratoderma with ichthyosis LOR Loricrin 10 Vohwinkel’s syndrome GJB2 Connexin 26 12 PPK with deafness GJB2 Connexin 26 12 Erythrokeratodermia variabilis GJB3, GJB4 Connexins 31 and 30.3 12 Darier disease ATP2A2 ATP-dependent calcium 14 transporter Striate PPK DSP, DSG1 Desmoplakin, desmoglein 1 51, 52 Conradi-Hu¨nermann-Happle syndrome EBP Delta 8-delta 7 sterol isomerase 53 (emopamil binding protein) Mal de Meleda ARS SLURP-1 -

Acral Persistent Papular Mucinosis
Journal of Pakistan Association of Dermatologists 2004; 14: 253-256. Case Report Acral persistent papular mucinosis: A rare variant of cutaneous mucinosis Arfan ul Bari, Muhammad Rashid*, Simeen ber Rahman** Dermatology Department, PAF Hospital Sargodha *ENT Department, PAF Hospital Sargodha ** Dermatology Department, Military Hospital, Rawalpindi, Pakistan Abstract Acral persistent papular mucinosis (APPM) is a distinctive form of dermal mucinosis not associated with systemic diseases. We report such a case in a sixty years old male who presented with few small papular lesions over both of his ears. These were managed successfully with excision and cryosurgery. Key words Papular mucinosis, acral persistent papular mucinosis, scleromyxedema, lichen myxedematosus Introduction rare, affects adults of both sexes equally and appears between ages 30 and 80. It is Papular mucinosis is one of the cutaneous chronic and may be progressive. The deposit diseases that presents as flesh- primary lesions are waxy, 2-to-4-mm, colored dermal papules mostly on the acral dome-shaped or flat-topped papules. parts of the body. There is confusion with Frequently, they may coalesce into regard to the terminology of this entity in plaques or appear in a linear array. Less the literature. Localized form of the frequently, urticarial, nodular, or disease has been called papular mucinosis sometimes annular lesions may be or lichen myxedematosus and generalized, appreciated. The dorsal aspect of the confluent papular forms with sclerosis are hands, face, elbows, and extensor portions known as scleromyxedema.1,2 Although of the extremities are most frequently papular mucinosis is frequently used as a affected. Mucosal lesions are absent.