Scrotal Granular Cell Tumor: a Case Report
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Glossary for Narrative Writing
Periodontal Assessment and Treatment Planning Gingival description Color: o pink o erythematous o cyanotic o racial pigmentation o metallic pigmentation o uniformity Contour: o recession o clefts o enlarged papillae o cratered papillae o blunted papillae o highly rolled o bulbous o knife-edged o scalloped o stippled Consistency: o firm o edematous o hyperplastic o fibrotic Band of gingiva: o amount o quality o location o treatability Bleeding tendency: o sulcus base, lining o gingival margins Suppuration Sinus tract formation Pocket depths Pseudopockets Frena Pain Other pathology Dental Description Defective restorations: o overhangs o open contacts o poor contours Fractured cusps 1 ww.links2success.biz [email protected] 914-303-6464 Caries Deposits: o Type . plaque . calculus . stain . matera alba o Location . supragingival . subgingival o Severity . mild . moderate . severe Wear facets Percussion sensitivity Tooth vitality Attrition, erosion, abrasion Occlusal plane level Occlusion findings Furcations Mobility Fremitus Radiographic findings Film dates Crown:root ratio Amount of bone loss o horizontal; vertical o localized; generalized Root length and shape Overhangs Bulbous crowns Fenestrations Dehiscences Tooth resorption Retained root tips Impacted teeth Root proximities Tilted teeth Radiolucencies/opacities Etiologic factors Local: o plaque o calculus o overhangs 2 ww.links2success.biz [email protected] 914-303-6464 o orthodontic apparatus o open margins o open contacts o improper -

Rush University Medical Center, May 2005
TABLE OF CONTENTS Case # Title Page 1. Malignant Spitz’s Nevus 1 2. Giant Congenital Nevus 4 3. Methotrexate Nodulosis 7 4. Apthae with Trisomy 8–positive Myelodysplastic Syndrome 10 5. Kwashiorkor 13 6. “Unknown” 16 7. Gangrenous Cellulitis 17 8. Parry-Romberg Syndrome 21 9. Wegener’s Granulomatosis 24 10. Pediatric CTCL 27 11. Hypopigmented Mycosis Fungoides 30 12. Fabry’s Disease 33 13. Cicatricial Alopecia, Unclassified 37 14. Mastocytoma 40 15. Cutaneous Piloleiomyomas 42 16. Granular Cell Tumor 44 17. Disseminated Blastomycoses 46 18. Neonatal Lupus 49 19. Multiple Lipomas 52 20. Acroangiodermatitis of Mali 54 21. Pigmented Basal Cell Carcinoma (BCC) 57 Page 1 Case #1 CHICAGO DERMATOLOGICAL SOCIETY RUSH UNIVERSITY MEDICAL CENTER CHICAGO, ILLINOIS MAY 18, 2005 CASE PRESENTED BY: Michael D. Tharp, M.D. Lady Dy, M.D., and Darrell W. Gonzales, M.D. History: This 2 year-old white female presented with a one year history of an expanding lesion on her left cheek. There was no history of preceding trauma. The review of systems was normal. Initially the lesion was thought to be a pyogenic granuloma and treated with two courses of pulse dye laser. After no response to treatment, a shave biopsy was performed. Because the histopathology was interpreted as an atypical melanocytic proliferation with Spitzoid features, a conservative, but complete excision with margins was performed. The pathology of this excision was interpreted as malignant melanoma measuring 4.0 mm in thickness. A sentinel lymph node biopsy was subsequently performed and demonstrated focal spindle cells within the subcapsular sinus of a left preauricular lymph node. -

A Single Case Report of Granular Cell Tumor of the Tongue Successfully Treated Through 445 Nm Diode Laser
healthcare Case Report A Single Case Report of Granular Cell Tumor of the Tongue Successfully Treated through 445 nm Diode Laser Maria Vittoria Viani 1,*, Luigi Corcione 1, Chiara Di Blasio 2, Ronell Bologna-Molina 3 , Paolo Vescovi 1 and Marco Meleti 1 1 Department of Medicine and Surgery, University of Parma, 43126 Parma, Italy; [email protected] (L.C.); [email protected] (P.V.); [email protected] (M.M.) 2 Private practice, Centro Medico Di Blasio, 43121 Parma; Italy; [email protected] 3 Faculty of Dentistry, University of the Republic, 14600 Montevideo, Uruguay; [email protected] * Correspondence: [email protected] Received: 10 June 2020; Accepted: 11 August 2020; Published: 13 August 2020 Abstract: Oral granular cell tumor (GCT) is a relatively rare, benign lesion that can easily be misdiagnosed. Particularly, the presence of pseudoepitheliomatous hyperplasia might, in some cases, lead to the hypothesis of squamous cell carcinoma. Surgical excision is the treatment of choice. Recurrence has been reported in up to 15% of cases treated with conventional surgery. Here, we reported a case of GCT of the tongue in a young female patient, which was successfully treated through 445 nm diode laser excision. Laser surgery might reduce bleeding and postoperative pain and may be associated with more rapid healing. Particularly, the vaporization effect on remnant tissues could eliminate GCT cells on the surgical bed, thus hypothetically leading to a lower rate of recurrence. In the present case, complete healing occurred in 1 week, and no recurrence was observed after 6 months. Laser surgery also allows the possibility to obtain second intention healing. -

Network Scan Data
CTEP Protocol No: T-99-0090 CC Protocol No: 01-C-0222 Amendment: J Revised: 4/21/09 IRB Approval Date: A Phase II Randomized, Cross-Over, Double-Blinded, Placebo-Controlled Trial of the Farnesyltransferase Inhibitor R115777 in Pediatric Patients with Neurofibromatosis Type 1 and Progressive Plexiform Neurofibromas Coordinating Center: Pediatric Oncology Branch, NCI Principal Investigator: Brigitte Widemann, M.D.* (POB, NCI) NIH Associate Investigators: Frank M. Balis, M.D. (POB, NCI) Beth Fox, M.D. (POB, NCI) Kathy Warren, M.D. (NOB, NCI) Andy Gillespie, R.N. (ND, CC) Eva Dombi, MD (POB, NCI)** Nalini Jayaprakash, (POB, NCI) Diane Cole, (POB, NCI) Seth Steinberg, Ph.D. (BDMB, DCS, NCI) Nicholas Patronas, M.D. (DR, CC)** Maria Tsokos, M.D., (Laboratory of Pathology, NCI)** Pamela Wolters, Ph.D. (HAMB, NCI) Staci Martin, Ph.D. (HAMB, NCI) Jeffrey Solomon, (NIH and Sensor Systems, Inc.) Non-NIH Associate Investigators: Wanda Salzer, M.D. ** Keesler Air Force Base, Biloxi, Mississippi) 81st MDOS/SGOC 301 Fisher Street, Room 1A132 Keesler AFB, MS 39534-2519 Phone: 228-377-6524 E-mail: [email protected] Bruce R. Korf, M.D., Ph.D. ** Chair, Department of Genetics Univeristy of Alabama at Birmingham 1530 3rd Ave. S. Birmingham, AL 35294 Phone: (205)-934-9411, Fax: (205)-934-9488 E-mail: [email protected] David H. Gutmann, M.D., Ph.D. ** Department of Neurology Washington University School of Medicine St. Louis Children’s Hospital Box 8111, 660 S. Euclid Avenue St. Louis, MO 63110 Phone: (314)-632-7149, Fax: (314)-362-9462 E-mail: [email protected] 1 4/21/2009 T-99-0090, 01-C-0222 Arie Perry, M.D. -

Growing Papule on the Right Shoulder of an Elderly Man
DERMATOPATHOLOGY DIAGNOSIS CLOSE ENCOUNTERS WITH THE ENVIRONMENT Growing Papule on the Right Shoulder of an Elderly Man Campbell L. Stewart, MD; Karolyn A. Wanat, MD; Adam I. Rubin, MD copy A not B H&E, original magnification ×20. H&E, original magnification ×400. Do The best diagnosis is: a. desmoplastic trichilemmoma b. granular cell basal cell carcinoma c. granular cell tumor d. sebaceous adenoma CUTIS e. xanthogranuloma PLEASE TURN TO PAGE 392 FOR DERMATOPATHOLOGY DIAGNOSIS DISCUSSION Dr. Stewart is from the University of Washington, Seattle. Dr. Wanat is from the University of Iowa, Iowa City. Dr. Rubin is from the University of Pennsylvania, Philadelphia. The authors report no conflict of interest. Correspondence: Adam I. Rubin, MD, University of Pennsylvania, 2 Maloney Bldg, 3600 Spruce St, Philadelphia, PA 19104 ([email protected]). WWW.CUTIS.COM VOLUME 97, JUNE 2016 391 Copyright Cutis 2016. No part of this publication may be reproduced, stored, or transmitted without the prior written permission of the Publisher. Dermatopathology Diagnosis Discussion Granular Cell Basal Cell Carcinoma asal cell carcinoma (BCC) is the most com- The granules in GBCC generally are positive on peri- mon human epithelial malignancy. There are odic acid–Schiff staining.1-4 several histologic variants, the rarest being The histologic differential diagnosis for GBCC B 1 granular cell BCC (GBCC). Granular cell BCC is includes granular cell tumor as well as other tumors reported most commonly in men with a mean age that can present with granular cell changes such as of 63 years. Sixty-four percent of cases develop on ameloblastoma, leiomyoma, leiomyosarcoma, angio- the face, with the remainder arising on the chest sarcoma, malignant peripheral nerve sheath tumor, or trunk. -

Depo-Provera
PRODUCT MONOGRAPH INCLUDING PATIENT MEDICATION INFORMATION PR ® DEPO-PROVERA medroxyprogesterone acetate injectable suspension, USP Sterile Aqueous Suspension 50 mg/mL and 150 mg/mL Progestogen Pfizer Canada Inc. Date of Revision: 17,300 Trans-Canada Highway February 13, 2018 Kirkland, Quebec H9J 2M5 Submission Control No: 210121 ® Pharmacia & Upjohn Company LLC Pfizer Canada Inc., Licensee © Pfizer Canada Inc., 2018 Table of Contents PART I: HEALTH PROFESSIONAL INFORMATION......................................................... 3 SUMMARY PRODUCT INFORMATION ........................................................................ 3 INDICATIONS AND CLINICAL USE .............................................................................. 3 CONTRAINDICATIONS ................................................................................................... 4 WARNINGS AND PRECAUTIONS: ................................................................................ 5 ADVERSE REACTIONS ................................................................................................. 18 DRUG INTERACTIONS .................................................................................................. 27 DOSAGE AND ADMINISTRATION .............................................................................. 28 OVERDOSAGE ................................................................................................................ 30 ACTION AND CLINICAL PHARMACOLOGY ............................................................ 30 STORAGE AND -

Cutaneous Neurofibromas: Clinical Definitions Current Treatment Is Limited to Surgical Removal Or Physical Or Descriptors Destruction
ARTICLE OPEN ACCESS Cutaneous neurofibromas Current clinical and pathologic issues Nicolas Ortonne, MD, PhD,* Pierre Wolkenstein, MD, PhD,* Jaishri O. Blakeley, MD, Bruce Korf, MD, PhD, Correspondence Scott R. Plotkin, MD, PhD, Vincent M. Riccardi, MD, MBA, Douglas C. Miller, MD, PhD, Susan Huson, MD, Dr. Wolkenstein Juha Peltonen, MD, PhD, Andrew Rosenberg, MD, Steven L. Carroll, MD, PhD, Sharad K. Verma, PhD, [email protected] Victor Mautner, MD, Meena Upadhyaya, PhD, and Anat Stemmer-Rachamimov, MD Neurology® 2018;91 (Suppl 1):S5-S13. doi:10.1212/WNL.0000000000005792 Abstract RELATED ARTICLES Objective Creating a comprehensive To present the current terminology and natural history of neurofibromatosis 1 (NF1) cuta- research strategy for neous neurofibromas (cNF). cutaneous neurofibromas Page S1 Methods NF1 experts from various research and clinical backgrounds reviewed the terms currently in use The biology of cutaneous fi for cNF as well as the clinical, histologic, and radiographic features of these tumors using neuro bromas: Consensus published and unpublished data. recommendations for setting research priorities Results Page S14 Neurofibromas develop within nerves, soft tissue, and skin. The primary distinction between fi fi Considerations for cNF and other neuro bromas is that cNF are limited to the skin whereas other neuro bromas development of therapies may involve the skin, but are not limited to the skin. There are important cellular, molecular, for cutaneous histologic, and clinical features of cNF. Each of these factors is discussed in consideration of neurofibroma a clinicopathologic framework for cNF. Page S21 Conclusion Clinical trial design for The development of effective therapies for cNF requires formulation of diagnostic criteria that cutaneous neurofibromas encompass the clinical and histologic features of these tumors. -

9Th Clinical Dermatology Congress Psoriasis, Psoriatic Arthritis & Skin
conferenceseries.com Joint Conference Mi Hye Lee et al., J Clin Exp Dermatol Res 2017, 8:6 (Suppl) DOI: 10.4172/2155-9554-C1-066 9th Clinical Dermatology Congress & 2nd International Conference on Psoriasis, Psoriatic arthritis & Skin infections October 16-18, 2017 New York, USA Nonsurgical treatment using micro-insulated needle on neurofibroma Mi Hye Lee, Hak Tae Kim, Woo Jin Lee, Chong Hyun Won, Sung Eun Chang, Mi Woo Lee and Jee Ho Choi University of Ulsan, Korea any studies have investigated the application of micro-insulated needles with radiofrequency (RF) for acne treatment or skin Mrejuvenation. However, there is no study investigating the effects of using micro-insulated needles with RF to treat multiple neurofibroma (NF) lesions. Many patients with multiple neurofibromas usually hesitate to remove all the lesions surgically due to cosmetic concerns. The aim of this study was to evaluate the clinicopathologic outcome, including efficacy and side effects after treatment, using newly developed micro-insulated needles with RF treatment. In this study, two human volunteers received multiple sessions of the micro-insulated needle RF treatment to multiple lesions. Seven to 40 shots were performed on each lesion. The treatment settings were as follows: microneedle penetrating depth of 5.0 mm; insulated 1.0 mm; power 16~46 (level 12~25); and a RF exposure time of 180~400 milliseconds. Skin biopsies were performed before and after the treatment. Outcome assessments included standardized photography, objective measurements of lesion size, histopathologic comparison between before and after the treatment, a physician’s global assessment, and patient satisfaction scores. RF energy could be delivered to the lesions without epidermal damage because the micro-insulation on the needle protects the epidermis from skin burns. -

Clinical Guideline Treatment and Removal of Benign Skin Lesions
Clinical Guideline Guideline Number: CG015, Ver. 5 Treatment and Removal of Benign Skin Lesions Disclaimer Clinical guidelines are developed and adopted to establish evidence-based clinical criteria for utilization management decisions. Oscar may delegate utilization management decisions of certain services to third-party delegates, who may develop and adopt their own clinical criteria. Clinical guidelines are applicable to certain plans. Clinical guidelines are applicable to members enrolled in Medicare Advantage plans only if there are no criteria established for the specified service in a Centers for Medicare & Medicaid Services (CMS) national coverage determination (NCD) or local coverage determination (LCD) on the date of a prior authorization request. Services are subject to the terms, conditions, limitations of a member’s policy and applicable state and federal law. Please reference the member’s policy documents (e.g., Certificate/Evidence of Coverage, Schedule of Benefits) or contact Oscar at 855-672-2755 to confirm coverage and benefit conditions. Summary The integumentary system is comprised of the skin, hair, and nails. The skin is divided into two layers: the dermis and epidermis; diseases of these protective outer layers are among the most common conditions worldwide. Lesions of the skin can be either benign (non-malignant), pre-malignant (potential for evolving into malignancy), or malignant (cancerous). Such lesions arise from congenital malformations or are acquired, often due to extensive UV exposure or underlying illness. Diagnosis is primarily through history, clinical exam, and the appearance of the lesion(s). While the vast majority of benign lesions require no intervention, some cases may necessitate intervention due to bothersome symptoms, for definitive diagnosis, or for exclusion of malignant features. -

Supermicar Data Entry Instructions, 2007 363 Pp. Pdf Icon[PDF
SUPERMICAR TABLE OF CONTENTS Chapter I - Introduction to SuperMICAR ........................................... 1 A. History and Background .............................................. 1 Chapter II – The Death Certificate ..................................................... 3 Exercise 1 – Reading Death Certificate ........................... 7 Chapter III Basic Data Entry Instructions ....................................... 12 A. Creating a SuperMICAR File ....................................... 14 B. Entering and Saving Certificate Data........................... 18 C. Adding Certificates using SuperMICAR....................... 19 1. Opening a file........................................................ 19 2. Certificate.............................................................. 19 3. Sex........................................................................ 20 4. Date of Death........................................................ 20 5. Age: Number of Units ........................................... 20 6. Age: Unit............................................................... 20 7. Part I, Cause of Death .......................................... 21 8. Duration ................................................................ 22 9. Part II, Cause of Death ......................................... 22 10. Was Autopsy Performed....................................... 23 11. Were Autopsy Findings Available ......................... 23 12. Tobacco................................................................ 24 13. Pregnancy............................................................ -

New Jersey State Cancer Registry List of Reportable Diseases and Conditions Effective Date March 10, 2011; Revised March 2019
New Jersey State Cancer Registry List of reportable diseases and conditions Effective date March 10, 2011; Revised March 2019 General Rules for Reportability (a) If a diagnosis includes any of the following words, every New Jersey health care facility, physician, dentist, other health care provider or independent clinical laboratory shall report the case to the Department in accordance with the provisions of N.J.A.C. 8:57A. Cancer; Carcinoma; Adenocarcinoma; Carcinoid tumor; Leukemia; Lymphoma; Malignant; and/or Sarcoma (b) Every New Jersey health care facility, physician, dentist, other health care provider or independent clinical laboratory shall report any case having a diagnosis listed at (g) below and which contains any of the following terms in the final diagnosis to the Department in accordance with the provisions of N.J.A.C. 8:57A. Apparent(ly); Appears; Compatible/Compatible with; Consistent with; Favors; Malignant appearing; Most likely; Presumed; Probable; Suspect(ed); Suspicious (for); and/or Typical (of) (c) Basal cell carcinomas and squamous cell carcinomas of the skin are NOT reportable, except when they are diagnosed in the labia, clitoris, vulva, prepuce, penis or scrotum. (d) Carcinoma in situ of the cervix and/or cervical squamous intraepithelial neoplasia III (CIN III) are NOT reportable. (e) Insofar as soft tissue tumors can arise in almost any body site, the primary site of the soft tissue tumor shall also be examined for any questionable neoplasm. NJSCR REPORTABILITY LIST – 2019 1 (f) If any uncertainty regarding the reporting of a particular case exists, the health care facility, physician, dentist, other health care provider or independent clinical laboratory shall contact the Department for guidance at (609) 633‐0500 or view information on the following website http://www.nj.gov/health/ces/njscr.shtml. -
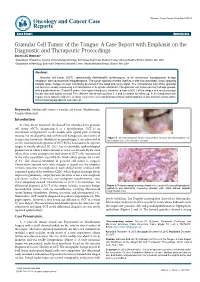
Granular Cell Tumor of the Tongue: a Case Report with Emphasis on The
ancer C C as & e y Ottoman, Oncol Cancer Case Rep 2015,1:1 g R o e l p o o c r t n Oncology and Cancer Case O ISSN: 2471-8556 Reports ResearchCase Report Article OpenOpen Access Access Granular Cell Tumor of the Tongue: A Case Report with Emphasis on the Diagnostic and Therapeutic Proceedings Bacem AE Ottoman* 1Department of Medicine, Division of Hematology/Oncology, Beth Israel Deaconess Medical Center, Harvard Medical School, Boston, MA, USA 2Department of Pathology, Beth Israel Deaconess Medical Center, Harvard Medical School, Boston, MA, USA Abstract Granular cell tumor (GCT), eponymically Abrikossoff’s myoblastoma, is an uncommon asymptomatic benign neoplasm with controversial etiopathogenia. The tumor typically reveals itself as a well-circumscribed, slowly growing nodular mass. Tongue is most commonly preferred in the head and neck region. The conventional size of the granular cell tumor is usually measuring 2-3 centimeters in its greater diameter. The granular cell tumor can taint all age groups, with a peak between 40 and 60 years. This report introduces, however, a case of GCT of the tongue in a much younger female that was totally excised. The clientele has shown up after 1, 3 and 6 months for follow-up. In the head and neck region, there was no evidence of either recurrence or metachronous clinical manifestations of any similar lesions; at the clinical and sonographical assessment. Keywords: Abrikossoff’s tumor; Granular cell tumor; Myoblastoma; Tongue ultrasound Introduction In 1926, Alexei Ivanovich Abrikossoff has introduced the granular cell tumor (GCT), designating it as a myoblastoma. GCT is an uncommon asymptomatic sessile nodule with typical pink overlying mucosa.