Rush University Medical Center, May 2005
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Glossary for Narrative Writing
Periodontal Assessment and Treatment Planning Gingival description Color: o pink o erythematous o cyanotic o racial pigmentation o metallic pigmentation o uniformity Contour: o recession o clefts o enlarged papillae o cratered papillae o blunted papillae o highly rolled o bulbous o knife-edged o scalloped o stippled Consistency: o firm o edematous o hyperplastic o fibrotic Band of gingiva: o amount o quality o location o treatability Bleeding tendency: o sulcus base, lining o gingival margins Suppuration Sinus tract formation Pocket depths Pseudopockets Frena Pain Other pathology Dental Description Defective restorations: o overhangs o open contacts o poor contours Fractured cusps 1 ww.links2success.biz [email protected] 914-303-6464 Caries Deposits: o Type . plaque . calculus . stain . matera alba o Location . supragingival . subgingival o Severity . mild . moderate . severe Wear facets Percussion sensitivity Tooth vitality Attrition, erosion, abrasion Occlusal plane level Occlusion findings Furcations Mobility Fremitus Radiographic findings Film dates Crown:root ratio Amount of bone loss o horizontal; vertical o localized; generalized Root length and shape Overhangs Bulbous crowns Fenestrations Dehiscences Tooth resorption Retained root tips Impacted teeth Root proximities Tilted teeth Radiolucencies/opacities Etiologic factors Local: o plaque o calculus o overhangs 2 ww.links2success.biz [email protected] 914-303-6464 o orthodontic apparatus o open margins o open contacts o improper -

Comorbidities in Mycosis Fungoides and Racial Differences In
medicines Article Comorbidities in Mycosis Fungoides and Racial Differences in Co-Existent Lymphomatoid Papulosis: A Cross-Sectional Study of 580 Patients in an Urban Tertiary Care Center Subuhi Kaul 1,*, Micah Belzberg 2, John-Douglas Matthew Hughes 3, Varun Mahadevan 2 , Raveena Khanna 2, Pegah R. Bakhshi 2, Michael S. Hong 2, Kyle A. Williams 2, 2 2, 2, Annie L. Grossberg , Shawn G. Kwatra y and Ronald J. Sweren y 1 Department of Medicine, John H. Stroger Hospital of Cook County, Chicago, IL 60612, USA 2 Department of Dermatology, Johns Hopkins University School of Medicine, Baltimore, MD 21287, USA; [email protected] (M.B.); [email protected] (V.M.); [email protected] (R.K.); [email protected] (P.R.B.); [email protected] (M.S.H.); [email protected] (K.A.W.); [email protected] (A.L.G.); [email protected] (S.G.K.); [email protected] (R.J.S.) 3 Section of Dermatology, University of Calgary, Alberta, AB T2N 1N4, Canada; [email protected] * Correspondence: [email protected]; Tel.: +1-312-864-7000 Considered co-senior authors. y Received: 26 October 2019; Accepted: 24 December 2019; Published: 26 December 2019 Abstract: Background: Mycosis fungoides (MF) is a cutaneous T-cell lymphoma. Previous reports have suggested MF is associated with inflammatory conditions such as psoriasis, increased cardiovascular risk factors as well as secondary neoplasms. Methods: A cross-sectional study of MF patients seen from 2013 to 2019 was performed. Comorbidities were selected based on the 2015 Medicare report highlighting the most common chronic medical illnesses in the United States. -

A Single Case Report of Granular Cell Tumor of the Tongue Successfully Treated Through 445 Nm Diode Laser
healthcare Case Report A Single Case Report of Granular Cell Tumor of the Tongue Successfully Treated through 445 nm Diode Laser Maria Vittoria Viani 1,*, Luigi Corcione 1, Chiara Di Blasio 2, Ronell Bologna-Molina 3 , Paolo Vescovi 1 and Marco Meleti 1 1 Department of Medicine and Surgery, University of Parma, 43126 Parma, Italy; [email protected] (L.C.); [email protected] (P.V.); [email protected] (M.M.) 2 Private practice, Centro Medico Di Blasio, 43121 Parma; Italy; [email protected] 3 Faculty of Dentistry, University of the Republic, 14600 Montevideo, Uruguay; [email protected] * Correspondence: [email protected] Received: 10 June 2020; Accepted: 11 August 2020; Published: 13 August 2020 Abstract: Oral granular cell tumor (GCT) is a relatively rare, benign lesion that can easily be misdiagnosed. Particularly, the presence of pseudoepitheliomatous hyperplasia might, in some cases, lead to the hypothesis of squamous cell carcinoma. Surgical excision is the treatment of choice. Recurrence has been reported in up to 15% of cases treated with conventional surgery. Here, we reported a case of GCT of the tongue in a young female patient, which was successfully treated through 445 nm diode laser excision. Laser surgery might reduce bleeding and postoperative pain and may be associated with more rapid healing. Particularly, the vaporization effect on remnant tissues could eliminate GCT cells on the surgical bed, thus hypothetically leading to a lower rate of recurrence. In the present case, complete healing occurred in 1 week, and no recurrence was observed after 6 months. Laser surgery also allows the possibility to obtain second intention healing. -

Growing Papule on the Right Shoulder of an Elderly Man
DERMATOPATHOLOGY DIAGNOSIS CLOSE ENCOUNTERS WITH THE ENVIRONMENT Growing Papule on the Right Shoulder of an Elderly Man Campbell L. Stewart, MD; Karolyn A. Wanat, MD; Adam I. Rubin, MD copy A not B H&E, original magnification ×20. H&E, original magnification ×400. Do The best diagnosis is: a. desmoplastic trichilemmoma b. granular cell basal cell carcinoma c. granular cell tumor d. sebaceous adenoma CUTIS e. xanthogranuloma PLEASE TURN TO PAGE 392 FOR DERMATOPATHOLOGY DIAGNOSIS DISCUSSION Dr. Stewart is from the University of Washington, Seattle. Dr. Wanat is from the University of Iowa, Iowa City. Dr. Rubin is from the University of Pennsylvania, Philadelphia. The authors report no conflict of interest. Correspondence: Adam I. Rubin, MD, University of Pennsylvania, 2 Maloney Bldg, 3600 Spruce St, Philadelphia, PA 19104 ([email protected]). WWW.CUTIS.COM VOLUME 97, JUNE 2016 391 Copyright Cutis 2016. No part of this publication may be reproduced, stored, or transmitted without the prior written permission of the Publisher. Dermatopathology Diagnosis Discussion Granular Cell Basal Cell Carcinoma asal cell carcinoma (BCC) is the most com- The granules in GBCC generally are positive on peri- mon human epithelial malignancy. There are odic acid–Schiff staining.1-4 several histologic variants, the rarest being The histologic differential diagnosis for GBCC B 1 granular cell BCC (GBCC). Granular cell BCC is includes granular cell tumor as well as other tumors reported most commonly in men with a mean age that can present with granular cell changes such as of 63 years. Sixty-four percent of cases develop on ameloblastoma, leiomyoma, leiomyosarcoma, angio- the face, with the remainder arising on the chest sarcoma, malignant peripheral nerve sheath tumor, or trunk. -

Utility of CD123 Immunohistochemistry in Differentiating Lupus Erythematosus from Cutaneous T-Cell Lymphoma
DR PAUL WILLIAM HARMS (Orcid ID : 0000-0002-0802-2883) DR MAY P. CHAN (Orcid ID : 0000-0002-0650-1266) Article type : Original Article Utility of CD123 immunohistochemistry in differentiating lupus erythematosus from cutaneous T-cell lymphoma (Running title: CD123 in lupus and cutaneous T-cell lymphoma) Stephanie J. T. Chen1,2, Julie Y. Tse3, Paul W. Harms1,4, Alexandra C. Hristov1,4, May P. Chan1,4 1Department of Pathology, University of Michigan, Ann Arbor, MI 2Department of Pathology, University of Iowa, Iowa City, IA 3Department of Pathology, Tufts Medical Center, Boston, MA 4Department of Dermatology, University of Michigan, Ann Arbor, MI Corresponding author: May P. Chan, MD University of Michigan Author Manuscript NCRC Building 35 This is the author manuscript accepted for publication and has undergone full peer review but has not been through the copyediting, typesetting, pagination and proofreading process, which may lead to differences between this version and the Version of Record. Please cite this article as doi: 10.1111/HIS.13817 This article is protected by copyright. All rights reserved 2800 Plymouth Road Ann Arbor, MI 48109 Phone: (734)764-4460 Fax: (734)764-4690 Email: [email protected] The authors report no conflict of interest. Abstract: 250 words Manuscript: 2496 words Figures: 3 Tables: 2 Abstract Aims: Histopathologic overlap between lupus erythematosus and certain types of cutaneous T- cell lymphoma (CTCL) is well documented. CD123+ plasmacytoid dendritic cells (PDCs) are typically increased in lupus erythematosus, but have not been well studied in CTCL. We aimed to compare CD123 immunostaining and histopathologic features in these conditions. -

Evaluation of Melanocyte Loss in Mycosis Fungoides Using SOX10 Immunohistochemistry
Article Evaluation of Melanocyte Loss in Mycosis Fungoides Using SOX10 Immunohistochemistry Cynthia Reyes Barron and Bruce R. Smoller * Department of Pathology and Laboratory Medicine, University of Rochester Medical Center, Rochester, NY 14642, USA; [email protected] * Correspondence: [email protected] Abstract: Mycosis fungoides (MF) is a subtype of primary cutaneous T-cell lymphoma (CTCL) with an indolent course that rarely progresses. Histologically, the lesions display a superficial lymphocytic infiltrate with epidermotropism of neoplastic T-cells. Hypopigmented MF is a rare variant that presents with hypopigmented lesions and is more likely to affect young patients. The etiology of the hypopigmentation is unclear. The aim of this study was to assess melanocyte loss in MF through immunohistochemistry (IHC) with SOX10. Twenty cases were evaluated, including seven of the hypopigmented subtype. The neoplastic epidermotropic infiltrate consisted predominantly of CD4+ T-cells in 65% of cases; CD8+ T-cells were present in moderate to abundant numbers in most cases. SOX10 IHC showed a decrease or focal complete loss of melanocytes in 50% of the cases. The predominant neoplastic cell type (CD4+/CD8+), age, race, gender, histologic features, and reported clinical pigmentation of the lesions were not predictive of melanocyte loss. A significant loss of melanocytes was observed in 43% of hypopigmented cases and 54% of conventional cases. Additional studies will increase our understanding of the relationship between observed pigmentation and the loss of melanocytes in MF. Citation: Barron, C.R.; Smoller, B.R. Evaluation of Melanocyte Loss in Keywords: mycosis fungoides; hypopigmented mycosis fungoides; SOX10; cutaneous T-cell lymphoma Mycosis Fungoides Using SOX10 Immunohistochemistry. -

Granulomatous Mycosis Fungoides, a Rare Subtype of Cutaneous T-Cell Lymphoma
CASE REPORT Granulomatous mycosis fungoides, a rare subtype of cutaneous T-cell lymphoma Marta Kogut, MD,a Eva Hadaschik, MD,a Stephan Grabbe, MD,b Mindaugas Andrulis, MD,c Alexander Enk, MD,a and Wolfgang Hartschuh, MDa Heidelberg and Mainz, Germany Key words: Granulomatous dermatitis; granulomatous mycosis fungoides; T-cell receptor gamma gene. ranulomatous mycosis fungoides (GMF) is an unusual histologic subtype of cutaneous Abbreviations used: T-cell lymphoma.1 The diagnosis of GMF is GMF: granulomatous mycosis fungoides G INF-a: interferon alfa usually established after observation of a granulo- MF: mycosis fungoides matous inflammatory reaction associated with a TCR: T-cell receptor malignant lymphoid infiltrate. Epidermotropism, a clue to diagnosis in classical mycosis fungoides (MF) 2 may be absent in about 47% of cases of GMF. In ear, Mycobacterium gordonae grew in a culture; some instances, the granulomatous component may however, polymerase chain reaction results were be intense and obscures the lymphomatous compo- negative. The etiologic relevance was considered nent of the infiltrate.1 There are no distinctive clinical 1,3 questionable, and the appropriate systemic antibi- patterns associated with GMF. otic therapy did not show any effects. The histopathologic evaluation of biopsy speci- CASE REPORT mens from the ear and forearm found a lympho- In 1998 a 28 year-old male patient presented with histiocytic, lichenoid inflammatory infiltrate with desquamating erythema on his left auricle (Fig 1, A). epitheloid giant cell granulomas (Fig 3, A and B). On exam he also had erythematous scaly plaques on On the basis of the clinical findings of a chronic his forearms and trunk associated with surrounding ulceration and histologic evidence of granulomas, we alopecia (Fig 2, A). -

Histologic Findings in Cutaneous Lupus Erythematosus 299
CHAPTER 21 Histologic Findings in Cutaneous Lupus 21 Erythematosus Christian A. Sander, Amir S. Yazdi, Michael J. Flaig, Peter Kind Lupus erythematosus (LE) is a chronic inflammatory disease that can be clinically divided into three major categories: chronic cutaneous LE (CCLE), subacute cuta- neous LE (SCLE), and systemic LE (SLE). In general, LE represents a spectrum of dis- ease with some overlap of these categories. Classification is based on clinical, histo- logic, serologic, and immunofluorescent (see Chap. 22) features. Consequently, histologic findings alone may not be sufficient for correct classification. In addition, these categories can be subdivided into numerous variants affecting different levels of the skin and subcutaneous tissue. Chronic Cutaneous Lupus Erythematosus Discoid Lupus Erythematosus Discoid LE (DLE) is the most common form of LE. Clinically, the head and neck region is affected in most cases. On the face, there may be a butterfly distribution. However, in some cases, the trunk and upper extremities can be also involved. Lesions consist of erythematous scaly patches and plaques. Histologically, in DLE the epidermis and dermis are affected, and the subcuta- neous tissue is usually spared. However, patchy infiltrates may be present. Character- istic microscopic features are hyperkeratosis with follicular plugging, thinning, and flattening of the epithelium and hydropic degeneration of the basal layer (liquefac- tion degeneration) (Fig. 21.1). In addition, there are scattered apoptotic keratinocytes (Civatte bodies) in the basal layer or in the epithelium. Particularly in older lesions, thickening of the basement membrane becomes obvious in the periodic acid-Schiff stain. In the dermis, there is a lichenoid or patchy lymphocytic infiltrate with accen- tuation of the pilosebaceous follicles. -

New Jersey State Cancer Registry List of Reportable Diseases and Conditions Effective Date March 10, 2011; Revised March 2019
New Jersey State Cancer Registry List of reportable diseases and conditions Effective date March 10, 2011; Revised March 2019 General Rules for Reportability (a) If a diagnosis includes any of the following words, every New Jersey health care facility, physician, dentist, other health care provider or independent clinical laboratory shall report the case to the Department in accordance with the provisions of N.J.A.C. 8:57A. Cancer; Carcinoma; Adenocarcinoma; Carcinoid tumor; Leukemia; Lymphoma; Malignant; and/or Sarcoma (b) Every New Jersey health care facility, physician, dentist, other health care provider or independent clinical laboratory shall report any case having a diagnosis listed at (g) below and which contains any of the following terms in the final diagnosis to the Department in accordance with the provisions of N.J.A.C. 8:57A. Apparent(ly); Appears; Compatible/Compatible with; Consistent with; Favors; Malignant appearing; Most likely; Presumed; Probable; Suspect(ed); Suspicious (for); and/or Typical (of) (c) Basal cell carcinomas and squamous cell carcinomas of the skin are NOT reportable, except when they are diagnosed in the labia, clitoris, vulva, prepuce, penis or scrotum. (d) Carcinoma in situ of the cervix and/or cervical squamous intraepithelial neoplasia III (CIN III) are NOT reportable. (e) Insofar as soft tissue tumors can arise in almost any body site, the primary site of the soft tissue tumor shall also be examined for any questionable neoplasm. NJSCR REPORTABILITY LIST – 2019 1 (f) If any uncertainty regarding the reporting of a particular case exists, the health care facility, physician, dentist, other health care provider or independent clinical laboratory shall contact the Department for guidance at (609) 633‐0500 or view information on the following website http://www.nj.gov/health/ces/njscr.shtml. -
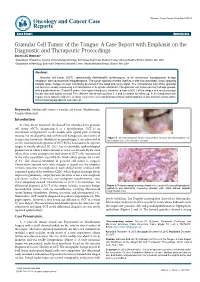
Granular Cell Tumor of the Tongue: a Case Report with Emphasis on The
ancer C C as & e y Ottoman, Oncol Cancer Case Rep 2015,1:1 g R o e l p o o c r t n Oncology and Cancer Case O ISSN: 2471-8556 Reports ResearchCase Report Article OpenOpen Access Access Granular Cell Tumor of the Tongue: A Case Report with Emphasis on the Diagnostic and Therapeutic Proceedings Bacem AE Ottoman* 1Department of Medicine, Division of Hematology/Oncology, Beth Israel Deaconess Medical Center, Harvard Medical School, Boston, MA, USA 2Department of Pathology, Beth Israel Deaconess Medical Center, Harvard Medical School, Boston, MA, USA Abstract Granular cell tumor (GCT), eponymically Abrikossoff’s myoblastoma, is an uncommon asymptomatic benign neoplasm with controversial etiopathogenia. The tumor typically reveals itself as a well-circumscribed, slowly growing nodular mass. Tongue is most commonly preferred in the head and neck region. The conventional size of the granular cell tumor is usually measuring 2-3 centimeters in its greater diameter. The granular cell tumor can taint all age groups, with a peak between 40 and 60 years. This report introduces, however, a case of GCT of the tongue in a much younger female that was totally excised. The clientele has shown up after 1, 3 and 6 months for follow-up. In the head and neck region, there was no evidence of either recurrence or metachronous clinical manifestations of any similar lesions; at the clinical and sonographical assessment. Keywords: Abrikossoff’s tumor; Granular cell tumor; Myoblastoma; Tongue ultrasound Introduction In 1926, Alexei Ivanovich Abrikossoff has introduced the granular cell tumor (GCT), designating it as a myoblastoma. GCT is an uncommon asymptomatic sessile nodule with typical pink overlying mucosa. -

Cutaneous T-Cell Lymphoma: Mycosis Fungoides/Se´Zary Syndrome: Part 1
FEATURE ARTICLE Cutaneous T-Cell Lymphoma: Mycosis Fungoides/Se´zary Syndrome: Part 1 Susan Booher, MS, RN, Sue Ann McCann, MSN, RN, DNC, Marianne C. Tawa, RN, MSN, ANP INTRODUCTION (Lutzner et al., 1975). The term CTCL should not be used Cutaneous T-cell lymphoma (CTCL) represents a category interchangeably with MF and SS; rather, it should be used of complex and diverse disease states that involve the skin only to describe the complete spectrum of cutaneous lym- as the primary site of malignant T-lymphocyte proliferation phomas of T-cell origin. and is a type of non-Hodgkin lymphoma. These malignant The World Health Organization and the European CD4+ T cells (lymphocytes) also can invade the lymphatic Organisation for Research and Treatment of Cancer met nodes, blood, and visceral organs. Mycosis fungoides (MF) in 2003 and 2004 to organize and define the cutaneous and its leukemic variant, Se´zary syndrome (SS), are the lymphomas and to separate them from systemic lymphomas most common types of CTCL. These chronic diseases are with similar histology (Willemze et al., 2005). Lymphomas rare and have considerable variation in cutaneous presen- are now classified as either T-cell or B-cell lymphoma with tation, histologic appearance, degree of blood involvement, indolent, intermediate, or aggressive clinical behavior, al- immunophenotypic profile, and prognosis. lowing for more consistent diagnosis and treatment regi- Historically, the French were pioneers in the discovery of mens (see Figure 4-1). CTCL. Approximately 200 years ago, Jean Louise Alibert published an article describing the appearance of tumors on EPIDEMIOLOGY the skin similar to that of a mushroom and coined the term MF and SS are rare diseases despite evidence that their mycosis fungoides (Alibert, 1806). -

Erythema Annulare Centrifugum Associated with Mantle B-Cell Non-Hodgkin’S Lymphoma
Letters to the Editor 319 Erythema Annulare Centrifugum Associated with Mantle B-cell Non-Hodgkin’s Lymphoma Marta Carlesimo1, Laura Fidanza1, Elena Mari1*, Guglielmo Pranteda1, Claudio Cacchi2, Barbara Veggia3, Maria Cristina Cox1 and Germana Camplone1 1UOC Dermatology, 2UOC Histopathology and 3UOC Haematolohy, II Unit University of Rome Sapienza Via di Grottarossa, 1039, IT-00189 Rome, Italy. *E-mail: [email protected] Accepted September 25, 2008. Sir, superficial type (Fig. 2). Previous investigations were Figurate erythemas are classified as erythema annulare normal, but as the lesions persisted further investi- centrifugum (EAC), erythema gyratum repens, erythema gations were carried out. Hepatic, pancreatic, renal migrans and necrolytic migratory erythema. Differential function and blood pictures were normal. The lymph diagnoses are mycosis fungoides, urticaria, granuloma nodes on the left side of his neck were approximately annulare and pseudolymphoma. 4.5 cm in diameter. EAC consists of recurrent and persistent erythematous A lymph node biopsy revealed a small B-cell non- eruptions or urticarial papules forming annular or serpen- Hodgkin’s lymphoma. The neoplastic cells were tiginous patterns with an advancing macular or raised positive for CD20/79a and cyclin d1. A bone marrow border and scaling on the inner aspect of the border. investigation showed scattered CD20/79apositive EAC was first described by Darier in 1916, and classi lymphocytes. GeneScan analysis and heteroduplex on fied in 1978 by Ackerman into a superficial and a deep polyacrylamide gel analysis showed a monoclonal B type (1, 2). EAC can be associated with a wide variety lymphocyte population. of triggers including infections, food and drug ingestion, endocrinological conditions and as a paraneoplastic sign.