MRSA Ophthalmic Infection, Part 2: Focus on Orbital Cellulitis
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Differentiate Red Eye Disorders
Introduction DIFFERENTIATE RED EYE DISORDERS • Needs immediate treatment • Needs treatment within a few days • Does not require treatment Introduction SUBJECTIVE EYE COMPLAINTS • Decreased vision • Pain • Redness Characterize the complaint through history and exam. Introduction TYPES OF RED EYE DISORDERS • Mechanical trauma • Chemical trauma • Inflammation/infection Introduction ETIOLOGIES OF RED EYE 1. Chemical injury 2. Angle-closure glaucoma 3. Ocular foreign body 4. Corneal abrasion 5. Uveitis 6. Conjunctivitis 7. Ocular surface disease 8. Subconjunctival hemorrhage Evaluation RED EYE: POSSIBLE CAUSES • Trauma • Chemicals • Infection • Allergy • Systemic conditions Evaluation RED EYE: CAUSE AND EFFECT Symptom Cause Itching Allergy Burning Lid disorders, dry eye Foreign body sensation Foreign body, corneal abrasion Localized lid tenderness Hordeolum, chalazion Evaluation RED EYE: CAUSE AND EFFECT (Continued) Symptom Cause Deep, intense pain Corneal abrasions, scleritis, iritis, acute glaucoma, sinusitis, etc. Photophobia Corneal abrasions, iritis, acute glaucoma Halo vision Corneal edema (acute glaucoma, uveitis) Evaluation Equipment needed to evaluate red eye Evaluation Refer red eye with vision loss to ophthalmologist for evaluation Evaluation RED EYE DISORDERS: AN ANATOMIC APPROACH • Face • Adnexa – Orbital area – Lids – Ocular movements • Globe – Conjunctiva, sclera – Anterior chamber (using slit lamp if possible) – Intraocular pressure Disorders of the Ocular Adnexa Disorders of the Ocular Adnexa Hordeolum Disorders of the Ocular -

A Description of the Clinical Features of Brimonidine- Associated Uveitis Alyssa Louie Primary Care Resident, San Francisco VA
Drug-induced intraocular inflammation: A description of the clinical features of brimonidine- associated uveitis Alyssa Louie Primary Care Resident, San Francisco VA Abstract: A description of the clinical features, diagnostic work-up, and management of acute anterior uveitis caused by brimonidine, a widely used glaucoma medication. I. Case History a. Patient demographics: 74 year-old white male b. Chief complaint: eye pain, redness, irritation for last 2 weeks c. Ocular and medical history: i. Ocular history 1. Primary open angle glaucoma OU, diagnosed 8 years ago 2. Senile cataracts OU, not visually significant 3. Type 2 Diabetes without retinopathy OU 4. No prior history of uveitis ii. Medical history: Diabetes Mellitus Type 2 iii. No known drug allergies d. Medications i. Ocular: dorzolamide BID OU (1.5 years), brimonidine BID OU (11 months), travatan QHS OU (5.5 years) ii. Medical: metformin 500mg tab BID PO II. Pertinent Findings a. Clinical exam i. Visual acuities: OD 20/20-, OS 20/20- ii. Goldmann applanation tonometry: 13 mm Hg OD, 13 mm Hg OS iii. Anterior segment 1. OU: 3+ diffuse conjunctival injection 2. OU: central and inferior granulomatous keratic precipitates 3. OU: Grade 1+ cell, 1+ flare 4. OU: No synechiae or iris changes were present iv. Posterior segment 1. Optic Nerve a. OD: Cup-to-disc ratio 0.70H/V, distinct margins b. OS: Cup-to-disc ratio 0.75H/V, distinct margins 2. Posterior pole, periphery, vitreous: unremarkable OU b. Laboratory Studies i. ACE, Lysozyme, FTA-ABS, VDRL, HLA-B27, Rheumatoid Factor, ANA, PPD, Chest X- ray: all negative/unreactive III. -

Adult Patients Common Eye Infections
Common Eye Dermatitis: HZV and HSV Infections: Adult • Redness of periocular skin can be allergic Patients (if associated with prominent itching) or bacterial (if associated with open sores/wounds) Julie D. Meier, MD Assistant Professor of Ophthalmology • Both HZV and HSV can have devastating ocular sequelae if not treated promptly OSU Eye and Ear Institute General Categories of Herpes Zoster Eye Infections Ophthalmicus • Symptoms: Skin rash and pain, may be • Dermatitis of Lids (HZV, HSV) preceded by headache, fever, eye pain or • Cellulitis of Lids (pre- vs post-septal) blurred vision • Blepharitis • Signs: Vesicular skin rash involving CN V • Conjunctivitis distribution; Involvement of tip of nose can predict higher rate of ocular involvement • Keratitis 1 Herpes Zoster Herpes Simplex Virus Ophthalmicus • Symptoms: • Work-up 9 Duration of rash; Immunocompromised? 9 Red eye, pain, light sensitivity, skin rash 9 Complete ocular exam, including slit 9 Fever, flu-like symptoms lamp, IOP, and dilated exam • Signs: • Can have conjunctival or corneal involvement, elevated IOP, anterior 9 Skin rash: Clear vesicles on chamber inflammation, scleritis, or erythematous base that progress to even involvement of retina and optic crusting nerve. Herpes Zoster Herpes Simplex Virus Ophthalmicus • Work-up: • Treatment: 9 Previous episodes? 9 If present within 3 days of rash’s 9 Previous nasal, oral or genital sores? appearance: oral Acyclovir/ Valacyclovir 9 Recurrences can be triggered by fever, stress, trauma, UV exposure 9 Bacitracin ointment to skin lesions 9 External exam: More suggestive of HSV 9 Warm compresses if lesions centered around eye and no involvement of forehead/scalp 9 TOPICAL ANTIVIRALS (e.g. -

Common Eye Condition Management
Common eye condition management Introduction by Moorfields’ medical director Thank you for taking the time to read this concise advice booklet about common eye conditions. It has been produced by clinicians and other staff CONTENTS at Moorfields to help you to make informed clinical decisions about your Introduction by Moorfields’ patients’ eye conditions locally, and medical director ......................... 3 avoid them having to attend hospital unnecessarily. Schematic diagram of the human eye ........................ 4 For each of the most common conditions you might see in your practice, we have listed signs and symptoms, General information Equipment and drugs to keep the equipment you will need to examine the patient, and at hand in the surgery ............ 4 the procedure to follow in undertaking that examination. General good practice advice ..................................... 5 Towards the end of the booklet, we have included a Eye examination .................... 5 table divided into four levels of urgency for onward referral – immediate, within 24 hours, within one week Care pathways for common and routine – with a list of relevant circumstances and eye conditions: conditions for each. Conjuntivitis ........................... 6 Dry eyes ............................... 7 We have also provided a table of the several locations Blepharitis ............................. 8 in which Moorfields provides care in and around Chalazion (meibomian cyst) ...10 London, and the sub-specialty services we offer in Stye .......................................11 each place. Corneal abrasion ....................12 Corneal foreign body ..............13 Subtarsal foreign body ..........14 I hope you find this guide helpful, and welcome your Subconjunctival views on how we might improve future editions. Please haemorrhage .........................15 contact our GP liaison manager on 020 7253 3411, Episcleritis .............................16 ext 3101 or by email to [email protected] with your comments. -

STYES and CHALAZION
TRE ATM ENT TRE ATM ENT FOR STYES FOR CHALAZION While most styes will drain on their The primary treatment for chalazion is own, the application of a hot or warm application of warm compresses for 10 compress are the most effective to 20 minutes at least 4 times a day. means of accelerating This may soften the hardened oils STYES drainage. The blocking the duct and promote drain- warmth and damp- age and healing. ness encourages the stye to drain. Just like any infection try not to touch it with your fingers. A Chalazion may be treated with compress can be made by putting hot any one or a combination of (not boiling) water on a wash cloth, or antibiotic or steroid drops pre- by using room temperature water and scribed by your healthcare a plastic heat pack. Warm compress- provider. es should be applied for 10—20 and minutes, four (4) times a day. There are occasions when sur- There is also a specialized topical gical drainage is required. ointment for styes, that may be pre- scribed. “Do not use eye makeup Styes may also cause a bruised feel- or wear contact lenses ing around the eye which is treated by application of a warm cloth to the eye. until the stye or chalazion CHALAZION With treatment, styes typically resolve have healed.” within one week. Lancing of a stye is not recommended. Revised: August 2011 WHAT ARE THEY? Signs and Symptoms Signs & Symptoms O f S t ye s of Chalazions The first signs of a stye are: A stye is an infection of the The symptoms of chalazions differ from tenderness, sebaceous glands at the base of the styes as they are usually painless. -

Chronic Conjunctivitis
9/8/2017 Allergan Pharmaceuticals Speaker’s Bureau Bio-Tissue BioDLogics, LLC Katena/IOP Seed Biotech COA Monterey Symposium 2017 Johnson and Johnson Vision Care, Inc. Shire Pharmaceuticals Nicholas Colatrella, OD, FAAO, Dipl AAO, ABO, ABCMO Jeffrey R. Varanelli, OD, FAAO, Dipl ABO, ABCMO Text NICHOLASCOLA090 to 22333 to join Live Text Poll Nicholas Colatrella, OD, FAAO, Dipl AAO, Jeffrey Varanelli, OD, FAAO, Dipl ABO, ABO, ABCMO ABCMO Text NICHOLASCOLA090 to 22333 once to join Then text A, B, C, D, E or write in your answer Live Immediate Accurate Chronic conjunctivitis is one of the most frustrating reasons that patients present to the office (1) Time course Often times patients will seek multiple providers searching for a solution The chronicity of their symptoms is extremely frustrating to the (2) Morphology patient and treating physician alike Some conditions can seriously affect vision and create ocular morbidity (3) Localization of disease process Many of these diseases do not respond to commonly used topical antibiotics, topical steroids, artificial tears, and other treatments for external ocular disease (4) Type of discharge or exudate Our hope during this one-hour lecture is to present a process to help aid in the diagnosis of chronic conjunctivitis help you determine the most likely etiology 1 9/8/2017 Three weeks is the dividing point as it is the upper limit for cases of viral infection and most bacterial infections to resolve without treatment. Acute Conjunctivitis Conjunctivitis that has been present for less than 3 weeks -

Eye Infections
CLINICAL Approach Taking a Look at Common Eye Infections John T. Huang, MD, FRCSC and Peter T. Huang, MD, FRCSC he acutely red eye is often seen first by the primary-care physician. The exact Tcause may be difficult to determine and may cause some concern that a serious ocular condition has been missed. Thorough history and clinical examination will help delineate the final diagnosis. When there are doubts, prompt referral to an oph- thalmologist can prevent serious consequences. Often, the most likely diagnosis of an acutely red eye is acute conjunctivitis. In the first day, an acute bacterial infection may be hard to differentiate from viral, chlamydial and noninfectious conjunctivitis and from episcleritis or scleritis. Below is a review of the most commonly seen forms of eye infections and treat- ments. Failure to improve after three to five days should lead to a re-evaluation of the patient and appropriate referral where necessary. CHRONIC BLEPHARITIS Clinical: Gritty burning sensation, mattering, lid margin swelling and/or scaly, flaky debris, mild hyperemia of conjunctiva; may have acne rosacea or hyperkeratotic dermatitis (Figure 1). Anterior: Staphylococcus aureus (follicles, accessory glands); posterior (meibomian glands). Treatment: • Lid scrubs (baby shampoo, lid-care towellettes, warm compresses). Figure 1. Chronic blepharitis. There may be localized sensitivity to the shampoo or the components of the solution in the towellettes (e.g., benzyl alcohol). • Hygiene is important for the treatment and management of chronic blepharitis. Topical antibiotic-corticosteroid combinations (e.g., tobramycin drops, tobramycin/dexamethasone or sulfacetamide sodium-prednisolone acetate). Usage of these medications is effective in providing symptomatic relief, as the inflammatory component of the problem is more effectively dealt with. -

Oral Contraception and Eye Disease: findings in Two Large Cohort Studies
538 Br J Ophthalmol 1998;82:538–542 Oral contraception and eye disease: findings in two large cohort studies M P Vessey, P Hannaford, J Mant, R Painter, P Frith, D Chappel Abstract over.4 Given the sparsity of the epidemiological Aim—To investigate the relation between evidence available, we have undertaken an oral contraceptive use and certain eye dis- analysis of the data on eye disease in the two eases. large British cohort studies of the benefits and Methods—Abstraction of the relevant data risks of oral contraception—namely, the Royal from the two large British cohort studies College of General Practitioners’ (RCGP) Oral of the eVects of oral contraception, the Contraception Study5 and the Oxford-Family Royal College of General Practitioners’ Planning Association (Oxford-FPA) contra- (RCGP) Oral Contraception Study and ceptive study.6 We summarise our findings the Oxford-Family Planning Association here. (Oxford-FPA) Contraceptive Study. Both cohort studies commenced in 1968 and were organised on a national basis. Be- Material and methods tween them they have accumulated over ROYAL COLLEGE OF GENERAL PRACTITIONERS’ 850 000 person years of observation in- ORAL CONTRACEPTION STUDY volving 63 000 women. During a 14 month period beginning in May 1968, 1400 British general practitioners re- Results—The conditions considered in the analysis were conjunctivitis, keratitis, iri- cruited 23 000 women using oral contracep- tives and a similar number who had never done tis, lacrimal disease, strabismus, cataract, 5 glaucoma, retinal detachment, and retinal so. The two groups were of similar age and all vascular lesions. With the exception of subjects were married or living as married. -

Stye (Hordeolum) N
n Stye (Hordeolum) n What puts your child at risk A stye is an infection causing a red, swollen bump on the eyelid. It occurs when the glands of a stye? under the skin of the eyelid become infected. Anything that irritates the eye, including frequent rub- Treatment, possibly including antibiotics, is impor- bing, eye makeup, or contact lenses, may increase the tant to prevent the infection from spreading. risk of infection. However, most styes occur without such risk factors. Other infections of the eyelid (such as blepharitis) may What is a stye? increase the risk of styes. A stye is an infection of the glands under the skin of the Can styes be prevented? eyelid, at the base of the eyelashes. The medical term is “hordeolum.” Styes can be quite irritating, and there is a Good hygiene, including regular washing of the face and risk that the infection will spread. hands, may reduce the risk of styes. Treatment usually consists of frequent soaks with a warm washcloth. Your doctor may recommend an antibiotic oint- ment as well. If the stye doesn’t go away within a few days, How are styes treated? or if it seems to be getting worse, call our office. Warm soaks. Soak a washcloth in warm water and place it over the eye. Keep the warm washcloth on the eye for 10 minutes or so, a few times per day. This will reduce What does it look like? pain and help the stye to heal faster. A red, tender, swollen bump on the edge of the eyelid. -

The Eyes Have It! Update on Common Conditions Affecting the Eye
Pharmacy Tech Topics™ VOLUME 22 NO. 2 | APRIL 2017 The Eyes Have It! Update on Common Conditions Affecting the Eye AUTHORS: Steven R. Abel, BS Pharm, PharmD, FASHP Kirk Evoy, PharmD, BCACP, BC-ADM, TTS PEER REVIEWERS: Sami Labib, RPh Rita Edwards, CPhT EDITOR: Patricia M. Wegner, BS Pharm, PharmD, FASHP DESIGN EDITOR: Leann Nelson Pharmacy Tech Topics™ (USPS No. 014-766) is published quarterly for $50 per year by the Illinois Council of Health-System Pharmacists, 4055 N. Perryville Road, Loves Park, IL 61111-8653. Phone 815-227-9292. Periodicals Postage Paid at Rockford, IL and additional mailing offices. POSTMASTER: Send address changes to: Pharmacy Tech Topics™, c/o ICHP, 4055 N. Perryville Road, Loves Park, IL 61111-8653 COPYRIGHT ©2017 by the Illinois Council of Health-System Pharmacists unless otherwise noted. All rights reserved. Pharmacy Tech Topics™ is a trademark of the Illinois Council of Health-System Pharmacists. This module is accredited for 2.5 contact hours of continuing pharmacy education and is recognized by the Pharmacy Technician Certification Board (PTCB). Cover image property of ©2017 Adobe Stock. LEARNING OBJECTIVES Upon completion of this module, the subscriber will be able to: 1. Identify the parts of the eye and the function of each part. 2. Summarize various eye disorders including ocular hypertension, glaucoma, infections, dry eyes, conjunctivitis, age-related macular degeneration, macular edema following retinal vein occlusion, and diabetic macular edema. 3. Discuss brand/generic substitutions, possible side effects, and proper administration of ophthalmic medications. 4. Describe the roles of various ophthalmic agents including those used to treat the following conditions: ocular hypertension, glaucoma, infections, dry eyes, conjunctivitis, age-related macular degeneration, macular edema following retinal vein occlusion, and diabetic macular edema. -

Ophthalmology Ophthalomolgy
Ophthalmology Ophthalomolgy Description ICD10-CM Documentation Tips Description ICD10-CM Documentation Tips Cataracts Code Tip Glaucoma Code Tip Cortical age-related cataract, right eye H25.011 Right, left, or bilateral; Presenile, Open angle with borderline H40.011 Suspect, Open angle, Primary senile, traumatic, complicated; findings, low risk, right eye angle closure; type; acute vs., specific type (cortical, anterior or chronic; mild, moderate, severe, Cortical age-related cataract, left eye H25.012 Open angle with borderline H40.012 posterior subcapsular polar, etc) indeterminate findings, low risk, left eye Cortical age-related cataract, bilateral eye H25.013 Open angle with borderline H40.013 findings, low risk, bilateral eye Anterior subcapsular polar age-related H25.031 Anatomical narrow angle, right H40.031 cataract,right eye eye Anterior subcapsular polar age-related H25.032 Anatomical narrow angle, right H40.032 cataract, left eye eye Anterior subcapsular polar age-related H25.033 Anatomical narrow angle, H40.033 cataract, bilateral bilateral Age-related nuclear cataract, right eye H25.11 Primary open-angle H40.11x2 glaucoma, moderate stage Age-related nuclear cataract, left eye H25.12 Globe Rupture Code Tip Age-related nuclear cataract, bilateral eye H25.13 Penetrating wound without S05.62xS Contusion vs. laceration; If foreign body of left eyeball, laceration, with or without sequela prolapsed or loss of intraocular tissue; penetrating wound, with or Combined forms of age-related cataract, H25.811 Contusion of eyeball and -
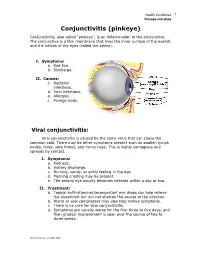
Pinkeye and Styes Conjunctivitis (Pinkeye) Conjunctivitis, Also Called “Pinkeye”, Is an Inflammation of the Conjunctiva
Health Guidelines 1 Pinkeye and styes Conjunctivitis (pinkeye) Conjunctivitis, also called “pinkeye”, is an inflammation of the conjunctiva. The conjunctiva is a thin membrane that lines the inner surface of the eyelids and the whites of the eyes (called the sclera). I. Symptoms: a. Red Eye. b. Discharge. II. Causes: c. Bacterial infections. d. Viral infections. e. Allergies. f. Foreign body. Viral conjunctivitis: Viral conjunctivitis is caused by the same virus that can cause the common cold. There may be other symptoms present such as swollen lymph nodes, fever, sore throat, and runny nose. This is highly contagious and spreads by contact. I. Symptoms: a. Redness. b. Watery discharge. c. Burning, sandy, or gritty feeling in the eye. d. Morning crusting may be present. e. The second eye usually becomes infected within a day or two. II. Treatment: a. Topical antihistamine/decongestant eye drops can help relieve the discomfort but will not shorten the course of the infection. b. Warm or cool compresses may also help relieve symptoms. c. There is no cure for viral conjunctivitis. d. Symptoms are usually worse for the first three to five days, and then gradual improvement is seen over the course of two to three weeks. 2013, 8-28 JJustad, MD, DDP Health Guidelines 2 Pinkeye and styes Bacterial conjunctivitis: Bacterial conjunctivitis is highly contagious and spread by contact. I. Symptoms: a. Redness and thick discharge from one eye. b. Both eyes can become infected. c. The discharge is usually yellow, white, or green. d. There is discharge throughout the day. e. The eye may be “stuck shut” in the mornings.