Every Red Eye Deserves an Antibiotic
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-
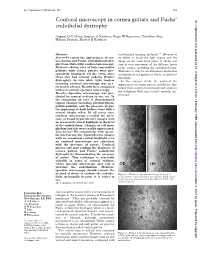
Confocal Microscopy in Cornea Guttata and Fuchs' Endothelial Dystrophy
Br J Ophthalmol 1999;83:185–189 185 Confocal microscopy in cornea guttata and Fuchs’ Br J Ophthalmol: first published as 10.1136/bjo.83.2.185 on 1 February 1999. Downloaded from endothelial dystrophy Auguste G-Y Chiou, Stephen C Kaufman, Roger W Beuerman, Toshihiko Ohta, Hisham Soliman, Herbert E Kaufman Abstract conventional imaging methods.3–13 Because of Aims—To report the appearances of cor- its ability to focus the light source and the nea guttata and Fuchs’ endothelial dystro- image on the same focal plane, it allows real phy from white light confocal microscopy. time in vivo assessment of the diVerent layers Methods—Seven eyes of four consecutive of the cornea, including the endothelial layer. patients with cornea guttata were pro- Therefore, it may be an alternative method in spectively examined. Of the seven eyes, evaluating cornea guttata or Fuchs’ endothelial three also had corneal oedema (Fuchs’ dystrophy. dystrophy). In vivo white light tandem In the current study, we analysed the scanning confocal microscopy was per- appearances of cornea guttata and Fuchs’ dys- formed in all eyes. Results were compared trophy from confocal microscopy and compare with non-contact specular microscopy. the technique with non-contact specular mi- Results—Specular microscopy was pre- croscopy. cluded by corneal oedema in one eye. In the remaining six eyes, it demonstrated typical changes including pleomorphism, polymegathism, and the presence of gut- tae appearing as dark bodies, some with a central bright reflex. In all seven eyes, confocal microscopy revealed the pres- ence of round hyporeflective images with an occasional central highlight at the level of the endothelium. -

Differentiate Red Eye Disorders
Introduction DIFFERENTIATE RED EYE DISORDERS • Needs immediate treatment • Needs treatment within a few days • Does not require treatment Introduction SUBJECTIVE EYE COMPLAINTS • Decreased vision • Pain • Redness Characterize the complaint through history and exam. Introduction TYPES OF RED EYE DISORDERS • Mechanical trauma • Chemical trauma • Inflammation/infection Introduction ETIOLOGIES OF RED EYE 1. Chemical injury 2. Angle-closure glaucoma 3. Ocular foreign body 4. Corneal abrasion 5. Uveitis 6. Conjunctivitis 7. Ocular surface disease 8. Subconjunctival hemorrhage Evaluation RED EYE: POSSIBLE CAUSES • Trauma • Chemicals • Infection • Allergy • Systemic conditions Evaluation RED EYE: CAUSE AND EFFECT Symptom Cause Itching Allergy Burning Lid disorders, dry eye Foreign body sensation Foreign body, corneal abrasion Localized lid tenderness Hordeolum, chalazion Evaluation RED EYE: CAUSE AND EFFECT (Continued) Symptom Cause Deep, intense pain Corneal abrasions, scleritis, iritis, acute glaucoma, sinusitis, etc. Photophobia Corneal abrasions, iritis, acute glaucoma Halo vision Corneal edema (acute glaucoma, uveitis) Evaluation Equipment needed to evaluate red eye Evaluation Refer red eye with vision loss to ophthalmologist for evaluation Evaluation RED EYE DISORDERS: AN ANATOMIC APPROACH • Face • Adnexa – Orbital area – Lids – Ocular movements • Globe – Conjunctiva, sclera – Anterior chamber (using slit lamp if possible) – Intraocular pressure Disorders of the Ocular Adnexa Disorders of the Ocular Adnexa Hordeolum Disorders of the Ocular -

MRSA Ophthalmic Infection, Part 2: Focus on Orbital Cellulitis
Clinical Update COMPREHENSIVE MRSA Ophthalmic Infection, Part 2: Focus on Orbital Cellulitis by gabrielle weiner, contributing writer interviewing preston h. blomquist, md, vikram d. durairaj, md, and david g. hwang, md rbital cellulitis is a poten- Acute MRSA Cellulitis tially sight- and life-threat- ening disease that tops the 1A 1B ophthalmology worry list. Add methicillin-resistant OStaphylococcus aureus (MRSA) to the mix of potential causative bacteria, and the level of concern rises even higher. MRSA has become a relatively prevalent cause of ophthalmic infec- tions; for example, one study showed that 89 percent of preseptal cellulitis S. aureus isolates are MRSA.1 And (1A) This 19-month-old boy presented with left periorbital edema and erythema preseptal cellulitis can rapidly develop five days after having been diagnosed in an ER with conjunctivitis and treated into the more worrisome condition of with oral and topical antibiotics. (1B) Axial CT image of the orbits with contrast orbital cellulitis if not treated promptly shows lacrimal gland abscess and globe displacement. and effectively. Moreover, the community-associ- and Hospital System in Dallas, 86 per- When to Suspect ated form of MRSA (CA-MRSA) now cent of those with preseptal cellulitis MRSA Orbital Cellulitis accounts for a larger proportion of and/or lid abscesses had CA-MRSA. Patients with orbital cellulitis com- ophthalmic cases than health care– These studies also found that preseptal monly complain of pain when moving associated MRSA (HA-MRSA). Thus, cellulitis was the most common oph- the eye, decreased vision, and limited many patients do not have the risk fac- thalmic MRSA presentation from 2000 eye movement. -

Adult Patients Common Eye Infections
Common Eye Dermatitis: HZV and HSV Infections: Adult • Redness of periocular skin can be allergic Patients (if associated with prominent itching) or bacterial (if associated with open sores/wounds) Julie D. Meier, MD Assistant Professor of Ophthalmology • Both HZV and HSV can have devastating ocular sequelae if not treated promptly OSU Eye and Ear Institute General Categories of Herpes Zoster Eye Infections Ophthalmicus • Symptoms: Skin rash and pain, may be • Dermatitis of Lids (HZV, HSV) preceded by headache, fever, eye pain or • Cellulitis of Lids (pre- vs post-septal) blurred vision • Blepharitis • Signs: Vesicular skin rash involving CN V • Conjunctivitis distribution; Involvement of tip of nose can predict higher rate of ocular involvement • Keratitis 1 Herpes Zoster Herpes Simplex Virus Ophthalmicus • Symptoms: • Work-up 9 Duration of rash; Immunocompromised? 9 Red eye, pain, light sensitivity, skin rash 9 Complete ocular exam, including slit 9 Fever, flu-like symptoms lamp, IOP, and dilated exam • Signs: • Can have conjunctival or corneal involvement, elevated IOP, anterior 9 Skin rash: Clear vesicles on chamber inflammation, scleritis, or erythematous base that progress to even involvement of retina and optic crusting nerve. Herpes Zoster Herpes Simplex Virus Ophthalmicus • Work-up: • Treatment: 9 Previous episodes? 9 If present within 3 days of rash’s 9 Previous nasal, oral or genital sores? appearance: oral Acyclovir/ Valacyclovir 9 Recurrences can be triggered by fever, stress, trauma, UV exposure 9 Bacitracin ointment to skin lesions 9 External exam: More suggestive of HSV 9 Warm compresses if lesions centered around eye and no involvement of forehead/scalp 9 TOPICAL ANTIVIRALS (e.g. -

Common Eye Condition Management
Common eye condition management Introduction by Moorfields’ medical director Thank you for taking the time to read this concise advice booklet about common eye conditions. It has been produced by clinicians and other staff CONTENTS at Moorfields to help you to make informed clinical decisions about your Introduction by Moorfields’ patients’ eye conditions locally, and medical director ......................... 3 avoid them having to attend hospital unnecessarily. Schematic diagram of the human eye ........................ 4 For each of the most common conditions you might see in your practice, we have listed signs and symptoms, General information Equipment and drugs to keep the equipment you will need to examine the patient, and at hand in the surgery ............ 4 the procedure to follow in undertaking that examination. General good practice advice ..................................... 5 Towards the end of the booklet, we have included a Eye examination .................... 5 table divided into four levels of urgency for onward referral – immediate, within 24 hours, within one week Care pathways for common and routine – with a list of relevant circumstances and eye conditions: conditions for each. Conjuntivitis ........................... 6 Dry eyes ............................... 7 We have also provided a table of the several locations Blepharitis ............................. 8 in which Moorfields provides care in and around Chalazion (meibomian cyst) ...10 London, and the sub-specialty services we offer in Stye .......................................11 each place. Corneal abrasion ....................12 Corneal foreign body ..............13 Subtarsal foreign body ..........14 I hope you find this guide helpful, and welcome your Subconjunctival views on how we might improve future editions. Please haemorrhage .........................15 contact our GP liaison manager on 020 7253 3411, Episcleritis .............................16 ext 3101 or by email to [email protected] with your comments. -

STYES and CHALAZION
TRE ATM ENT TRE ATM ENT FOR STYES FOR CHALAZION While most styes will drain on their The primary treatment for chalazion is own, the application of a hot or warm application of warm compresses for 10 compress are the most effective to 20 minutes at least 4 times a day. means of accelerating This may soften the hardened oils STYES drainage. The blocking the duct and promote drain- warmth and damp- age and healing. ness encourages the stye to drain. Just like any infection try not to touch it with your fingers. A Chalazion may be treated with compress can be made by putting hot any one or a combination of (not boiling) water on a wash cloth, or antibiotic or steroid drops pre- by using room temperature water and scribed by your healthcare a plastic heat pack. Warm compress- provider. es should be applied for 10—20 and minutes, four (4) times a day. There are occasions when sur- There is also a specialized topical gical drainage is required. ointment for styes, that may be pre- scribed. “Do not use eye makeup Styes may also cause a bruised feel- or wear contact lenses ing around the eye which is treated by application of a warm cloth to the eye. until the stye or chalazion CHALAZION With treatment, styes typically resolve have healed.” within one week. Lancing of a stye is not recommended. Revised: August 2011 WHAT ARE THEY? Signs and Symptoms Signs & Symptoms O f S t ye s of Chalazions The first signs of a stye are: A stye is an infection of the The symptoms of chalazions differ from tenderness, sebaceous glands at the base of the styes as they are usually painless. -

Eye Infections
CLINICAL Approach Taking a Look at Common Eye Infections John T. Huang, MD, FRCSC and Peter T. Huang, MD, FRCSC he acutely red eye is often seen first by the primary-care physician. The exact Tcause may be difficult to determine and may cause some concern that a serious ocular condition has been missed. Thorough history and clinical examination will help delineate the final diagnosis. When there are doubts, prompt referral to an oph- thalmologist can prevent serious consequences. Often, the most likely diagnosis of an acutely red eye is acute conjunctivitis. In the first day, an acute bacterial infection may be hard to differentiate from viral, chlamydial and noninfectious conjunctivitis and from episcleritis or scleritis. Below is a review of the most commonly seen forms of eye infections and treat- ments. Failure to improve after three to five days should lead to a re-evaluation of the patient and appropriate referral where necessary. CHRONIC BLEPHARITIS Clinical: Gritty burning sensation, mattering, lid margin swelling and/or scaly, flaky debris, mild hyperemia of conjunctiva; may have acne rosacea or hyperkeratotic dermatitis (Figure 1). Anterior: Staphylococcus aureus (follicles, accessory glands); posterior (meibomian glands). Treatment: • Lid scrubs (baby shampoo, lid-care towellettes, warm compresses). Figure 1. Chronic blepharitis. There may be localized sensitivity to the shampoo or the components of the solution in the towellettes (e.g., benzyl alcohol). • Hygiene is important for the treatment and management of chronic blepharitis. Topical antibiotic-corticosteroid combinations (e.g., tobramycin drops, tobramycin/dexamethasone or sulfacetamide sodium-prednisolone acetate). Usage of these medications is effective in providing symptomatic relief, as the inflammatory component of the problem is more effectively dealt with. -

Fusarium Keratitis and Corneal Collagen Cross
FUSARIUM KERATITIS AND SURGERY REFRACTIVE CORNEAL COLLAGEN CROSS-LINKING BY MINAS CORONEO, AO, BSC(MED), MBBS, MSC SYD, MD, MS, UNSW, FRACS, FRANZCO; RAJESH FOGLA, DNB, FRCS(EDIN), MMED(OPHTH); WILLIAM B. TRATTLER, MD; ASHIYANA NARIANI, MD, MPH; COMPLEX CASE MANAGEMENT COMPLEX GARGI KHARE VORA, MD; AND ALAN N. CARLSON, MD CASE PRESENTATION A 42-year-old white man is referred to the Duke University Eye Center Cornea Service for a central corneal ulcer with a hypopyon in his right eye. The patient sustained the ocular injury while mowing the lawn, with debris getting into the eye while he was wearing contact lenses. He was diagnosed with culture-positive Fusarium species by the referring ophthalmologist and was treat- ed with oral voriconazole 200 mg twice daily and frequent topical natamycin 5% and voriconazole 10 mg/mL. The patient under- went epithelium-off corneal collagen cross-linking (CXL) approxi- Figure 1. Initial evaluation of the eye with a Fusarium corneal mately 4 weeks after diagnosis of the ulcer and was treated with infiltrate and hypopyon. a loteprednol steroid taper after the procedure. His condition subsequently progressed, with increasing eye pain, a nonhealing epithelial defect, and a worsening corneal infiltrate. Upon evaluation, the patient has a large corneal infiltrate with necrotic stroma, which is approaching the limbus, and a hypopyon (Figure 1). His UCVA measures 20/70-1. B-scan ultrasound of the right eye shows no evidence of posterior segment involvement. Reculturing of the corneal infiltrate is negative for bacteria, fungus, and Acanthamoeba. Confocal microscopy reveals no evidence of hyphae or cysts. -

A Microbiological Study of Neonatal Conjunctivae and Conjunctivitis
Br J Ophthalmol: first published as 10.1136/bjo.61.9.601 on 1 September 1977. Downloaded from British Journal of Ophthalmology, 1977, 61, 601-607 A microbiological study of neonatal conjunctivae and conjunctivitis M. J. PRENTICE, G. R. HUTCHINSON, AND D. TAYLOR-ROBINSON From the Division of Communicable Diseases, MRC Clinical Research Centre, and Northwick Park Hospital, Watford Road, Harrow, Middlesex SUJMMARY To investigate the importance of chlamydiae, ureaplasmas, Mycoplasma hominis, and anaerobic bacteria in the pathogenesis of neonatal conjunctivitis in the Harrow population con- junctival specimens from 104 infants with conjunctivitis and 104 similar healthy neonates were examined. The incidence of neonatal conjunctivitis was 8 2%, and no case of neomycin-resistant disease occurred during the study. Staphylococcus aureus, viridans Streptococci, and Eschlerichia coli were the only micro-organisms isolated significantly more frequently from affected than from control eyes, which suggests that these bacteria may be a cause of the conjunctivitis. All cultures for chlamydiae, M. hominis, Neisseria gonorrhoeae, and anaerobic bacteria were negative. The mother's race, social status, illness, and obstetric events were found to have no effect on the incidence, time of onset of conjunctivitis, or micro-organisms isolated. The clinical characteristics of conjunc- tivitis were also not related to the micro-organisms isolated. No potential pathogens were isolated from 63-5 % of the eyes showing conjunctivitis. The results suggest that some of these cases may be caused by chemical irritation, and the possibility of an infectious aetiology is also discussed. copyright. Neonatal conjunctivitis is a common disease et al., 1974; Burns et al., 1975), but some cases of affecting between 2-6% (Watson and Gairdner, cervicitis may be caused by this organism (Chiang 1968) and 5 to 8% (Hurley, 1966) of infants born et al., 1968; Hobson et al., 1976). -

Stye (Hordeolum) N
n Stye (Hordeolum) n What puts your child at risk A stye is an infection causing a red, swollen bump on the eyelid. It occurs when the glands of a stye? under the skin of the eyelid become infected. Anything that irritates the eye, including frequent rub- Treatment, possibly including antibiotics, is impor- bing, eye makeup, or contact lenses, may increase the tant to prevent the infection from spreading. risk of infection. However, most styes occur without such risk factors. Other infections of the eyelid (such as blepharitis) may What is a stye? increase the risk of styes. A stye is an infection of the glands under the skin of the Can styes be prevented? eyelid, at the base of the eyelashes. The medical term is “hordeolum.” Styes can be quite irritating, and there is a Good hygiene, including regular washing of the face and risk that the infection will spread. hands, may reduce the risk of styes. Treatment usually consists of frequent soaks with a warm washcloth. Your doctor may recommend an antibiotic oint- ment as well. If the stye doesn’t go away within a few days, How are styes treated? or if it seems to be getting worse, call our office. Warm soaks. Soak a washcloth in warm water and place it over the eye. Keep the warm washcloth on the eye for 10 minutes or so, a few times per day. This will reduce What does it look like? pain and help the stye to heal faster. A red, tender, swollen bump on the edge of the eyelid. -

Infections in & Around The
Starship Children’s Health Clinical Guideline Note: The electronic version of this guideline is the version currently in use. Any printed version can not be assumed to be current. Please remember to read our disclaimer. INFECTIONS IN & AROUND THE EYE Examining the Eyes Herpes Simplex Keratitis Preseptal vs Orbital cellulitis Herpes Zoster Opthalmicus Preseptal (periorbital) cellulitis Non-infectious conditions that may cause Orbital Cellulitis diagnostic confusion Dacryocystitis o Watery & Sticky eyes in the Stye / Hordeolum Newborn Neonatal conjunctivitis o Allergic Conjunctivitis Conjunctivitis (non-neonatal) o Chalazion o Viral conjunctivitis References o Bacterial conjunctivitis Examining the eyes Always assess visual acuity in each eye separately > 6 weeks fixing & following or reaching for objects of interest. >12 months – see and pick up small objects such as hundred-and-thousands > 3 to 4 years – letter or shape matching is usually possible > 5-6 year olds - Snellen chart usually possible (NB: 6/9 means the child can read line 9 at 6 metres) Check pupil responses and for a red reflex, examine the conjunctiva, stain with fluorescein and examine with the BLUE light on the ophthalmoscope (not the green light), check for a foreign body including beneath the upper eyelid by everting the lid over a cotton bud. Preseptal versus Orbital cellulitis It is essential to distinguish between these conditions as they differ considerably in terms of severity of complications, urgency of investigations & management. The orbital septum is a thin membrane that extends from the orbital periosteum & inserts into the tarsal plates of both eyelids. It acts as a physical barrier to infection. Preseptal (periorbital) Cellulitis Infection of the superficial eyelid & periorbital structures anterior to the orbital septum. -

Pseudomonas Aeruginosa Conjunctivitis
Clinical Perinatal/Neonatal Case Presentation nnnnnnnnnnnnnn Bacteremia, Meningitis, and Brain Abscesses in a Hospitalized Infant: Complications of Pseudomonas aeruginosa Conjunctivitis Samir S. Shah, MD dosis. The white blood cell count was 50,900/mm3 with 59% seg- Peter Gloor, MD mented neutrophils and 17% band forms. The platelet count was 3 Patrick G. Gallagher, MD 20,000/mm , and prothrombin and partial thromboplastin times were prolonged at 26.5 seconds and .2 minutes, respectively. Cere- This report describes a preterm infant hospitalized in a neonatal brospinal fluid examination revealed a glucose of 22 mg/dl, a protein 3 3 intensive care unit who developed Pseudomonas aeruginosa of 164 mg/dl, 5/mm erythrocytes, and 387/mm leukocytes. Blood, conjunctivitis associated with bacteremia, meningitis, and multiple urine, endotracheal secretion, and cerebrospinal fluid cultures were brain abscesses. P. aeruginosa conjunctivitis can rapidly progress to an obtained. Cranial ultrasonography was normal. Treatment included invasive eye infection, such as corneal ulceration or endophthalmitis, intravenous fluid boluses, dopamine infusion, mechanical ventila- leading to poor vision or blindness. Progression of this infection may tion, and transfusion with packed red blood cells, fresh frozen plasma, lead to systemic disease. However, as illustrated in this report, P. and platelets. Intravenous ampicillin and ceftriaxone were prescribed. aeruginosa conjunctivitis may be associated with the development of These were subsequently changed to intravenous gentamicin and systemic complications such as bacteremia and meningitis in the ceftazidime when Pseudomonas aeruginosa was isolated from absence of invasive eye disease. P. aeruginosa is a relatively common blood, endotracheal, and conjunctival cultures. Both eyes were treated cause of conjunctivitis in hospitalized preterm and low birth weight with ophthalmic gentamicin ointment.