Time of Quickening Is Associated with the Placental Site and BMI in Nulliparous Women Negin Jaafar 1 Lars Henning Pedersen 2,3,4
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

The Stunted Development of in Vitro Fertilization in the United States, 1975-1992
EMBRYONIC POLICIES: THE STUNTED DEVELOPMENT OF IN VITRO FERTILIZATION IN THE UNITED STATES, 1975-1992 Erin N. McKenna A Thesis Submitted to the Graduate College of Bowling Green State University in partial fulfillment of the requirements for the degree of MASTER OF ARTS May 2006 Committee: Dr. Leigh Ann Wheeler, Advisor Dr. Walter Grunden ii Abstract The federal government’s failure to fund research on in vitro fertilization has had an important legacy and significant consequences in the United States. Due to the dismantling of the Ethics Advisory Board in 1980, no government funding was provided for research for in vitro fertilization (IVF), embryo transfer (ET), and gamete intra-fallopian transfer (GIFT). The lack of government funding, regulation, and involvement has resulted in the false advertising of higher success rates to lure patients into the infertility specialists’ offices. In their desperation to have children, consumers of such medical technologies paid exorbitant fees that often remained uncovered by insurance companies. The federal government enacted legislation in 1992 attempting to alleviate some of the aspects of exploitation of the consumer-patient. The government’s recognition of the importance of such procedures was hit and miss, though, much like the reproductive technology itself. The legacy is one that has resulted in American citizens who now turn to developing countries such as Israel and India, where the treatment is drastically cheaper and often more effective. I attempt to explain the federal government’s response to New Reproductive Technologies (NRTs), beginning with in vitro fertilization, thus exploring why and how this debate has inextricably been linked to the ongoing abortion debate. -

Pregnancy Tracker
Women’sPregnancy WelcomeHealth Specialists Packet #5 Pregnancy Tracker It can be confusing to figure out “how far along” you are. A normal pregnancy is dated most times by a patient’s last menstrual period. If a patient is uncertain of when her last menstrual period occurred than an ultrasound may be used to date the pregnancy. A normal pregnancy lasts 42 weeks and your due date is 40 weeks from your last menstrual period. A full term pregnancy is any pregnancy beyond 37 weeks. What to Expect Each Month of Your Pregnancy Office Hours: Our office hours are 9:00-12:00 and 1:00-4:00 Monday through Friday. We are closed on the weekends. If you need to reach a doctor after hours or on the weekend please dial 770-474-0064 and instructions will be given. Calculating Your Due Date The estimated date of delivery (EDD), also known as your due date, is most often calculated from the first day of your last menstrual period. In order to estimate your due date take the date that your last normal menstrual cycle started, add 7 days and count back 3 months. Pregnancy is assumed to have occurred 2 weeks after your last cycle and therefore 2 weeks are added to the beginning of your pregnancy. Pregnancy actually lasts 10 months (40 weeks) and not 9 months. Most women go into labor within 2 weeks of their due date either before or after their actual EDD. For more information, please visit www.girldocs.com First Month (0-4 weeks) Fetal Growth Your Health Sperm fertilizes the egg in one of the fallopian tubes and During this time it is important you take a multivitamin then 5-7 days later the fertilized egg implants (attaches) supplement that contains folic acid 0.4 milligrams daily. -
Turning Your Breech Baby to a Head-Down Position (External Cephalic Version)
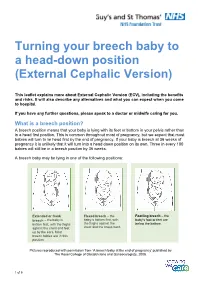
Turning your breech baby to a head-down position (External Cephalic Version) This leaflet explains more about External Cephalic Version (ECV), including the benefits and risks. It will also describe any alternatives and what you can expect when you come to hospital. If you have any further questions, please speak to a doctor or midwife caring for you. What is a breech position? A breech position means that your baby is lying with its feet or bottom in your pelvis rather than in a head first position. This is common throughout most of pregnancy, but we expect that most babies will turn to lie head first by the end of pregnancy. If your baby is breech at 36 weeks of pregnancy it is unlikely that it will turn into a head down position on its own. Three in every 100 babies will still be in a breech position by 36 weeks. A breech baby may be lying in one of the following positions: Extended or frank Flexed breech – the Footling breech – the breech – the baby is baby is bottom first, with baby’s foot or feet are bottom first, with the thighs the thighs against the below the bottom. against the chest and feet chest and the knees bent. up by the ears. Most breech babies are in this position. Pictures reproduced with permission from ‘A breech baby at the end of pregnancy’ published by The Royal College of Obstetricians and Gynaecologists, 2008. 1 of 5 What causes breech? Breech is more common in women who are expecting twins, or in women who have a differently-shaped womb (uterus). -

Maternal Movement and Position Changes to Facilitate Labor Progress Have Been Discussed in the Literature for Decades
ELAINE ZWELLING, PHD, RN, LCCE, FACCE Abstract The benefi ts of maternal movement and position changes to facilitate labor progress have been discussed in the literature for decades. Recent routine interventions such as amniotomy, induction, fetal monitoring, and epidural anesthesia, as well as an increase in maternal obesity, have made position changes during labor challenging. The lack of maternal changes in position throughout labor can contribute to dystocia and increase the risk of cesarean births for failure to progress or descend. This article provides a historical review of the research fi ndings related to the effects of maternal positioning on the labor process and uses six physiological principles as a framework to offer sug- gestions for maternal positioning both before and after epidural anesthesia. Key Words Birth; Childbirth; Labor, fi rst stage; Labor, second stage; Maternity nursing; Obstetrical nursing; Maternal postures; Maternal positioning. Overcoming the Challenges: Maternal Movement 72 volume 35 | number 2 March/April 2010 or centuries laboring women chose to remain dural anesthesia, found that women who were able to mobile and upright, using positions such as change positions regularly or maintain upright positions standing, sitting, kneeling, hands and knees, or during labor were more comfortable and required less Fsquatting (Gupta & Nikodem, 2000; Johnson, pain medication (Atwood, 1976; de Jong et al., 1997; En- Johnson, & Gupta, 1991). Today immobility throughout gelmann, 1977; Johnson et al., 1991). For instance, Ada- the labor process has become a common occurrence for chi, Shimada, and Usul (2003) found in their study of 58 many childbearing women. Increased medical manage- laboring women that a sitting position decreased labor ment, obesity, lack of patient understanding about the pain in contrast with supine positioning. -

Variation in Fetal Presentations and Positions Among Women in Warri, Delta State, Nigeria
World Research Journal of Obstetrics and Gynecology ISSN: 2277-6001, Volume 2, Issue 1, 2013, pp.-10-12. Available online at http://www.bioinfopublication.org/jouarchive.php?opt=&jouid=BPJ0000126 VARIATION IN FETAL PRESENTATIONS AND POSITIONS AMONG WOMEN IN WARRI, DELTA STATE, NIGERIA OLANIYAN O.T.1*, MERAIYEBU A.B.1, ALELE J.Y.1, DARE J.B.2, ATSUKWEI D.1 AND ADELAIYE A.B.1 1Department of Physiology, Bingham University, Karu, Nasarawa, Nigeria. 2Department of Anatomy, Bingham University, Karu, Nasarawa, Nigeria. *Corresponding Author: Email- [email protected] Received: November 21, 2013; Accepted: December 23, 2013 Abstract- This study investigates the various fetal presentations among women in Warri and the various predisposing factors which may have possibly brought about these variations; the major positions considered were cephalic, breech and transverse, with the considered influencing factors being gestational age of the fetus, maternal age, amniotic fluid volume, parity, and method of previous deliveries. A total of 105 ultra- sound fetal biometries with a total of 108 fetuses, between 15-40 weeks of gestational age, and maternal age between 19 and 40 were used for this study. Fetal ultrasound biometry was used to find out information about the fetus including gestational age, amniotic fluid volume, presentation of the fetus and a questionnaire was used to take information about the mother including maternal age, parity, and method of previous delivery (ies). The result showed that a total of 82 fetuses (75.9%) were Cephalic babies, 19 (17.6%) were Breech and 7 (6.5%) are transverse. Out of the 105 women, there were 102 (77.1% cephalic, 18.3% breech, 4.8% transverse) women with adequate amniotic fluid volume and 1 woman (with a cephalic fetus) with average amniotic fluid volume and 2 women (with transverse foetuses) with low amniotic fluid volume. -

FETAL GROWTH and DEVELOPMENT Copyright© 1995 by the South Dakota Department of Health
FETAL GROWTH AND DEVELOPMENT Copyright© 1995 by the South Dakota Department of Health. All rights reserved. The South Dakota Department of Health acknowledges Keith L. Moore, Ph.D., F.I.A.C, F.R.S.M.; T.V.N. Persaud, M.D., Ph.D., F.R.C. Path (Lond): Cynthia Barrett, M.D.; and Kathleen A. Veness-Meehan, M.D.; for their professional assis- tance in reviewing this booklet. Photos on pages 8, 9, 11, 13, 16 and 18 by Lennart Nilsson, of Sweden, A Child is Born, 1986, Dell Publishing and are used by permission. Lennart Nilsson is a pioneer in medical photography, credited with inventing numerous devices and techniques in his field. The photos used in this booklet have been published internationally in scientific periodicals and used in the popular press and television. Illustrations on pp. 5 and 6 by Drs. K.L. Moore, T.V.N. Persaud and K. Shiota, Color Atlas of Clinical Embryology, 1944, Philadelphia: W.B. Saunders, are used by permission. The South Dakota Department of Health also acknowledges the technical assis- tance of the following in development of the booklet: Gary Crum, Ph.D., Ann Kappel and Arlen Pennell of the Ohio Department of Health; Sandra Van Gerpen, M.D. M.P.H., Terry Englemann, R.N., Colleen Winter, R.N., B.S.N., and Nancy Shoup, R.N., B.S.N., of the South Dakota Department of Health; Dennis Stevens, M.D.; Virginia Johnson, M.D.; Brent Lindbloom, D.O.; Dean Madison, M.D.; Buck Williams, M.D.; Roger Martin, R.N., C.N.P., M.S.; Barbara Goddard, B.S., Ph.D.; Laurie Lippert; Vincent Rue, P.h.D.; and Representative Roger Hunt. -

Maternal Perception of Fetal Movements: a Qualitative Description
View metadata, citation and similar papers at core.ac.uk brought to you by CORE provided by ResearchArchive at Victoria University of Wellington MATERNAL PERCEPTION OF FETAL MOVEMENTS: A QUALITATIVE DESCRIPTION BY BILLIE BRADFORD A thesis submitted to the Victoria University of Wellington in fulfilment of the requirements for the degree of Master of Midwifery Victoria University of Wellington 2014 Abstract Background: Maternal perception of decreased fetal movements is a specific indicator of fetal compromise, notably in the context of poor fetal growth. There is currently no agreed numerical definition of decreased fetal movements, with subjective perception of a decrease on the part of the mother being the most significant definition clinically. Both qualitative and quantitative aspects of fetal activity may be important in identifying the compromised fetus.Yet, how pregnant women perceive and describe fetal activity is under-investigated by qualitative means. The aim of this study was to explore normal fetal activity, through first- hand descriptive accounts by pregnant women. Methods: Using qualitative descriptive methodology, interviews were conducted with 19 low-risk women experiencing their first pregnancy, at two timepoints in their third trimester. Interview transcripts were later analysed using qualitative content analysis and patterns of fetal activity identified were then considered along-side the characteristics of the women and their birth outcomes. Results: Fetal activity as described by pregnant women demonstrated a sustained increase in strength, frequency and variation from quickening until 28-32 weeks. Strength of movements continued to increase at term, but variation in movement types reduced. Kicking and jolting movements decreased at term with pushing or stretching movements dominating. -

Fetal Outcome in Pregnant Women with Reduced Fetal Movements. Int J Health Sci Res
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Fetal Outcome in Pregnant Women with Reduced Fetal Movements Syeda.R.M1, Shakuntala.P.N1*, Shubha.R.Rao1, Sharma.S.K1, Claudius. S2 1Department of Obstetrics and Gynaecology, 2Department of Radiology. St.Martha’s Hospital, Nrupathunga Road, Bengaluru-560070, Karnataka, India. *Correspondence Email: [email protected] Received: 03/04//2013 Revised: 07/05/2013 Accepted: 20/05/2013 ABSTRACT Objectives: To analyse the fetal outcome following reduced fetal movements monitored by cardiotocogram and Biophysical Profile Score (BPP) at onset of complaints and before delivery. Material and Methods: Present study was a prospective observational study conducted in the Department of Obstetrics and Gynaecology St. Martha’s Hospital over a period of 13 months from 01/03/2009 to 31/03/2010 It included 50 pregnant women after 32 weeks of gestation and singleton pregnancies with < 12 fetal movements in 24 hours. They underwent a cardiotocogram(CTG) or a non stress test(NST) and biophysical profile test(BPP) and results were analysed statistically. Results: A non -reactive CTG on admission was encountered in 2/50(04%) vs 21/50(42%);(p<0.001) of women with reduced fetal movements at delivery. Majority 20/50(40%) of the caesarean sections were emergency due to non reassuring CTG. Neonatal birth weight <2500 grams was recorded in 25/50(50%) and 10/26(38.46%) had meconium staining of liquor indicating an unfavorable intra uterine environment. When birth weight <2500 and >2500 grams, NRCTG (non reactive CTG) at the time of delivery was 42.30% vs 37.50%;( p value 0.393) respectively and was not significantly related. -

Module Presentation
Module Presentation How to best use the Modules To make the best use of this training we encourage you to complete each Module in order following the format below: 1. Read Module Presentation. Added explanations can be found in the HELPER Guidelines and in the extra information section if there is one. 2. Complete the Extraction/Scenario training exercises. The extraction exercises use de-identified and altered patient medical records. Enter the requested information into the provided section from the Birth Certificate Workbook. The Scenarios are situations you may encounter as you collect information from your patients’ medical records. 3. Check your responses using the answer sheets immediately following the segment completed 4. Complete the Module specific Evaluation, as before the answers are immediately following the Evaluation 5. If not already done, read extra training materials, if available. If you have questions about how to answer any of the requests for information in the NYS Certification of Live Birth Training Modules, please contact Rosemary Varga (585-275-8737). *”Coding” is a convenient although slightly misleading term for entering the needed information in the Statewide Perinatal Data system. True “coding” is the entry of predetermined numbers into a system that can then rate the material. We do not use numbers rather we enter the requested information. Module Three Labor & Delivery Part I Labor & Delivery Fields •Labor & Delivery information is found in the mother’s chart with much of the information on the L & D flowsheet/summary. A copy of this information may also be found in the infant’s chart. 2 Mother Transferred in Antepartum •Only complete these fields if the mother was transferred for medical reasons NYS GUIDELINES 3 Mother’s Weight at Delivery •Mother’s weight at delivery will often be found on the L&D flowsheet If you can’t find mother’s weight at delivery in the L&D information you can use the mother’s weight at her last prenatal visit if the visit was within 2 weeks of delivery. -

Decreased Fetal Movements Policy
Document ID: MATY115 Version: 1.0 Facilitated by: Billie Bradford Last reviewed: June 2019 Approved by: Maternity Quality Committee Review date: June 2022 Management of women with decreased fetal movements Hutt Maternity Policies provide guidance for the midwives and medical staff working in Hutt Maternity Services. Please discuss policies relevant to your care with your Lead Maternity Carer. Purpose Maternal concern about decreased fetal movements (DFM) is common and occurs in 4- 16% of pregnancies. The majority of cases are transient and benign however, DFM is associated with numerous adverse outcomes including small for gestation age (SGA), oligohydramnios, perinatal brain injuries, intrauterine infections, congenital abnormalities, feto-maternal haemorrhage, umbilical cord complications, stillbirths and neonatal deaths.1 Emerging evidence suggests that dissemination of information regarding fetal movements to pregnant women and timely assessment of maternal reports of DFM may reduce adverse outcomes. 2 The purpose of this policy is to ensure timely and appropriate assessment of DFM complaints. Scope This policy is intended to apply to women with otherwise normal pregnancies who present with a concern about fetal movements. For women with identified medical or obstetric conditions, DFM may be considered an additional risk factor for poor outcome. There is a lack of high-quality evidence to guide management of cases of DFM at present, although two large trials are ongoing. Definitions A diagnosis of DFM is made based on the subjective impression of reduced fetal movements by the pregnant woman herself. This decrease may be in frequency and/or strength of movements, or constitute a change in her baby’s normal pattern of movements. -

Images of the Pregnant Body and the Unborn Child in England, 1540–C.1680 Rebecca Whiteley*
Social History of Medicine Vol. 32, No. 2 pp. 241–266 Roy Porter Student Prize Essay Figuring Pictures and Picturing Figures: Images of the Pregnant Body and the Unborn Child in England, 1540–c.1680 Rebecca Whiteley* Summary. Birth figures, or print images of the fetus in the uterus, were immensely popular in mid- wifery and surgical books in Europe in the sixteenth and seventeenth centuries. But despite their central role in the visual culture of pregnancy and childbirth during this period, very little critical attention has been paid to them. This article seeks to address this dearth by examining birth figures in their cultural context and exploring the various ways in which they may have been used and interpreted by early modern viewers. I argue that, through this process of exploring and contextual- ising early modern birth figures, we can gain a richer and more nuanced understanding of the early modern body, how it was visualised, understood and treated. Keywords: midwifery; childbirth; pregnancy; visual culture; print culture An earnest, cherubic toddler floats in what looks like an inverted glass flask. Accompanied by numerous fellows, each figure demonstrates a different acrobatic pos- ture (Figure 1). These images seem strange to a modern eye: while we might suppose they represent a fetus in utero (which indeed they do), we are troubled by their non- naturalistic style, and perhaps by a feeling that they are rich in a symbolism with which we are not familiar. Their first viewers, in England in the 1540s, might also have found them strange, but in a different way, as these images offered to them an entirely new picture of a bodily interior that was largely understood to be both visually inaccessible and inherently mysterious. -

Reducing Alcohol Use During Pregnancy Saves Lives
WICWORKS REDUCING ALCOHOL USE DURING PREGNANCY SAVES LIVES women drink no alcohol at all if pregnant or planning to become pregnant.7 Low-income women, whose children are most at risk for negative health outcomes, are less likely to receive appropriate counseling regarding alcohol use in pregnancy.8.9 The Supplemental Nutrition Program for Women, Infants and Children (WIC) serves more than 9 million low-income participants each month, including more than half of all infants born in the United States.10 Given its reach into a high- risk population during this critical period of the life nfants exposed to alcohol before birth can cycle, WIC can play a major role in reducing alcohol have serious life-long problems. WIC is in consumption during pregnancy. Along with food and Ian excellent position to screen pregnant nutrition education, WIC agencies are mandated by women for alcohol use during pregnancy and federal law to provide individual screening for drug and help women change their drinking behaviors. alcohol use and to make referrals to substance abuse In collaboration with UCLA, the largest local treatment programs when needed.11 The challenge with agency WIC program in the country designed such screening and referral is that only heavy users of and conducted a randomized study of a brief alcohol qualify for substance abuse treatment programs, intervention program to reduce prenatal yet lower levels of alcohol use can also be harmful to the alcohol use among WIC participants. Results developing fetus. Until now, WIC screening has often documented that brief intervention conducted led to recognition of prenatal alcohol use—with no in the WIC setting led to significant reductions accompanying intervention tools available.