Mizuo-Nakamura Phenomenon in Oguchi Disease Due to A
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Retinitis Pigmentosa Precision Panel Overview Indications Clinical
Retinitis Pigmentosa Precision Panel Overview Retinitis Pigmentosa (RP) comprises a complex group of inherited dystrophies characterized by degeneration and dysfunction of the retina, affecting photoreceptor and pigment epithelial function. RP can be an isolated finding or be part of a syndrome that can be inherited in a dominant, recessive or X-linked pattern. This disease presents as progressive loss of night and peripheral vision, leading to a constricted visual field and markedly diminished vision. The clinical presentation of these findings is highly variable, some patients being affected during childhood while others are asymptomatic well into adulthood. There is an increase in mortality rate due to psychiatric comorbidities. The Igenomix Retinitis Pigmentosa Precision Panel can be used to make an accurate and directed diagnosis as well as a differential diagnosis of blindness ultimately leading to a better management and prognosis of the disease. It provides a comprehensive analysis of the genes involved in this disease using next-generation sequencing (NGS) to fully understand the spectrum of relevant genes involved. Indications The Igenomix Retinitis Pigmentosa Precision Panel is indicated for those patients with a clinical suspicion or diagnosis with or without the following manifestations: - Family history of RP - Night blindness - Progressive constriction of the visual field, usually peripheral - Cataracts - Sensation of sparking lights (photopsias) - Headache Clinical Utility The clinical utility of this panel is: - The genetic and molecular confirmation for an accurate clinical diagnosis of a symptomatic patient. - Early initiation of multidisciplinary treatment in the form of medical care with vitamin A and other antioxidants and surgical care for potential cataract extraction or retinal prosthesis. -

Bass – Glaucomatous-Type Field Loss Not Due to Glaucoma
Glaucoma on the Brain! Glaucomatous-Type Yes, we see lots of glaucoma Field Loss Not Due to Not every field that looks like glaucoma is due to glaucoma! Glaucoma If you misdiagnose glaucoma, you could miss other sight-threatening and life-threatening Sherry J. Bass, OD, FAAO disorders SUNY College of Optometry New York, NY Types of Glaucomatous Visual Field Defects Paracentral Defects Nasal Step Defects Arcuate and Bjerrum Defects Altitudinal Defects Peripheral Field Constriction to Tunnel Fields 1 Visual Field Defects in Very Early Glaucoma Paracentral loss Early superior/inferior temporal RNFL and rim loss: short axons Arcuate defects above or below the papillomacular bundle Arcuate field loss in the nasal field close to fixation Superotemporal notch Visual Field Defects in Early Glaucoma Nasal step More widespread RNFL loss and rim loss in the inferior or superior temporal rim tissue : longer axons Loss stops abruptly at the horizontal raphae “Step” pattern 2 Visual Field Defects in Moderate Glaucoma Arcuate scotoma- Bjerrum scotoma Focal notches in the inferior and/or superior rim tissue that reach the edge of the disc Denser field defects Follow an arcuate pattern connected to the blind spot 3 Visual Field Defects in Advanced Glaucoma End-Stage Glaucoma Dense Altitudinal Loss Progressive loss of superior or inferior rim tissue Non-Glaucomatous Etiology of End-Stage Glaucoma Paracentral Field Loss Peripheral constriction Hereditary macular Loss of temporal rim tissue diseases Temporal “islands” Stargardt’s macular due -

Bilateral Acquired Progressive Retinal Nerve Fiber Layer Myelination
Bilateral Acquired Progressive Retinal Nerve Fiber Layer Myelination Abstract We present the multimodal imaging findings of an unusual case of bilateral acquired progressive myelination of the optic disc over a 10-year follow up period, in a hyperopic adolescent patient in the absence of an underlying ocular or systemic abnormality. Myelination of the left optic disc was noted at age 7 and of the right optic disc at age 13 but no other ocular or systemic abnormalities were identified. Cross sectional OCT and en face OCT angiography confirmed the presence of myelination of the retinal nerve fiber layer and excluded other etiologic possibilities including an astrocytic hamartoma. Keywords: Optic Nerve; Optic Fiber Myelination, Acquired, Hyperopia INTRODUCTION Myelination of the retinal nerve fiber layer occurs in 1% of the population and is most frequently congenital and non-progressive. (1) Congenital cases are typically isolated but may be rarely associated with the syndrome of ipsilateral high myopia, strabismus and amblyopia (2,3), although cases have been reported in hyperopic eyes. Reports of acquired and progressive myelination associated with congenital optic nerve disorders such as Arnold-Chiari malformation, hydrocephalus, optic disc drusen, and iatrogenic causes such as optic nerve sheath fenestration, are relatively rare.(4–8) PLEASE ADJUST THE REFERENCE CITATIONS While affected patients are typically asymptomatic, retinal nerve fiber layer myelination can be rarely associated with visual loss. Even more unusual are reports of acquired and progressive myelination of the nerve fiber layer. We present the multimodal imaging findings of such a case in a healthy young patient with a 10-year follow up. -

Optical Coherence Tomography
Eponyms in Ophthalmology: What’s in a Name? What’s in a Name? How do ophthalmic diagnostic findings get their names? Timothy J. Bennett, CRA, OCT-C, FOPS Penn State Hershey Eye Center Hershey, PA SA-5-C What’s in a Name? What’s in a Name? Linnaean Taxonomy: system of Linnaean Taxonomy classification Binomial nomenclature Carl Linnaeus, 1707-1778 What About Human Anatomy? Anatomic Terminology In the late nineteenth century some Nomina Anatomica was the international 50,000 terms for various body parts standard on human anatomic terminology were in use. from 1956 until it was replaced by Terminologia Anatomica in 1998. The same structures were described by different names, depending on the anatomist’s background: school, language, culture, traditions, etc. 1 How About Ophthalmology? Diagnostic Naming Conventions Etymology: origins of words often from Greek or Latin roots Named for anatomic location Descriptive of process or result Descriptive of appearance Acronyms or initials Eponyms: named for first person to identify or describe Etymology Etymology Retinopathy from the Greek “Pathos”: suffering, disease, feeling, passion. Descriptive of Process or Result Descriptive of Process or Result Macular degeneration Vitreo-macular traction Plaquenil toxicity Macular hole 2 Descriptive of Appearance Descriptive of Appearance Literal Synonymous (looks like something else) Pink eye Cherry red spot Floppy lid syndrome Bear tracks Cataract? Ichthyosis Genetic skin disorder characterized by dry, scaly, or flaky skin that resembles -

Central Serous Papillopathy by Optic Nerve Head Drusen
Clinical Ophthalmology Dovepress open access to scientific and medical research Open Access Full Text Article CASE REPORT Central serous papillopathy by optic nerve head drusen Ana Marina Suelves1 Abstract: We report a 38-year-old man with a complaint of blurred vision in his right eye for the Ester Francés-Muñoz1 previous 5 days. He had bilateral optic disc drusen. Fluorescein angiography revealed multiple Roberto Gallego-Pinazo1 hyperfluorescent foci within temporal optic discs and temporal inferior arcade in late phase. Diamar Pardo-Lopez1 Optical coherence tomography showed bilateral peripapillary serous detachment as well as right Jose Luis Mullor2 macular detachment. This is the first reported case of a concurrent peripapillary and macular Jose Fernando Arevalo3 detachment in a patient with central serous papillopathy by optic disc drusen. Central serous papillopathy is an atypical form of central serous chorioretinopathy that should be considered Manuel Díaz-Llopis1,4,5 as a potential cause of acute loss of vision in patients with optic nerve head drusen. 1 Department of Ophthalmology, La Fe Keywords: central serous papillopathy, peripapillary central serous chorioretinopathy, optic University Hospital, Valencia, Spain; For personal use only. 2Instituto de Investigación Sanitaria, nerve head drusen, peripapillary subretinal fluid Fundación para la investigación, La Fe Hospital, Valencia, Spain; 3Retina and vitreous service, Clínica Introduction Oftalmológica Centro Caracas, Optic nerve head drusen (ONHD) are hyaline material calcificated -

Assessing Retinal Structure in Complete Congenital Stationary Night Blindness and Oguchi Disease Pooja Godara Medical College of Wisconsin
Marquette University e-Publications@Marquette Biomedical Engineering Faculty Research and Biomedical Engineering, Department of Publications 12-1-2012 Assessing Retinal Structure In Complete Congenital Stationary Night Blindness and Oguchi Disease Pooja Godara Medical College of Wisconsin Robert F. Cooper Marquette University Panagiotis I. Sergouniotis University College London Melissa A. Diederichs Medical College of Wisconsin Megan R. Streb University of Iowa See next page for additional authors NOTICE: this is the author’s version of a work that was accepted for publication in American Journal of Ophthalmology. Changes resulting from the publishing process, such as peer review, editing, corrections, structural formatting, and other quality control mechanisms may not be reflected in this document. Changes may have been made to this work since it was submitted for publication. A definitive version was subsequently published in American Journal of Ophthalmology, Vol. 154, No. 6 (December 2012): 987–1001. DOI. © Elsevier 2012. Used with permission. Authors Pooja Godara, Robert F. Cooper, Panagiotis I. Sergouniotis, Melissa A. Diederichs, Megan R. Streb, Mohamed Genead, J. Jason McAnany, Andrew R. Webster, Anthony T. Moore, Adam M. Dubis, Maureen Neitz, Alfredo Dubra, Edwin M. Stone, Gerald A. Fishman, Dennis P. Han, Michel Michaelides, and Joseph Carroll This article is available at e-Publications@Marquette: https://epublications.marquette.edu/bioengin_fac/321 NOT THE PUBLISHED VERSION; this is the author’s final, peer-reviewed manuscript. The published version may be accessed by following the link in the citation at the bottom of the page. Assessing Retinal Structure In Complete Congenital Stationary Night Blindness and Oguchi Disease Pooja Godara Department of Ophthalmology, Medical College of Wisconsin Milwaukee, WI Robert F. -

Oguchi Disease with Unusual Findings Associated with A
addition, the duration of treatment to induce retinal re- a golden-yellow discoloration of the fundus that disap- attachment is currently unknown. However, patients with pears after prolonged dark adaptation, called the Mizuo- IH have been treated for several months. Nakamura phenomenon. The International Society for Hemangiomas consist histologically of cavernous and Clinical Electrophysiology of Vision–protocol bright- capillary vascular networks. The mechanism by which flash electroretinograms (ERGs), performed after 30 min- oral propranolol aids in the resolution of exudative reti- utes of dark adaptation, are typically electronegative with nal detachment in DCH associated with Sturge-Weber a severely reduced b-wave and milder reduction of the syndrome is unknown. It is possible that, similar to IH, a-wave.1,2 After 3 to 4 hours of dark adaptation, both am- there is vasoconstriction of the DCH due to decreased plitudes recover to nearly normal, especially the a- release of nitric oxide, blocking of proangiogenic sig- wave.2 However, the recovered rod function is rapidly lost nals including vascular endothelial growth factor and ba- after a short light exposure or a single bright white flash.2,3 sic fibroblast growth factor, and apoptosis in proliferat- We describe a case of Oguchi disease with unusual find- ing endothelial cells with vascular tumor regression.5 ings caused by a putative heterozygous mutation in the To our knowledge, the benefits of propranolol therapy SAG gene. have not been reported in adult hemangioma or for DCH. This is the first reported case of propranolol treatment Report of a Case. A 40-year-old woman with visual acu- in an adult with exudative retinal detachment in DCH ity of 20/20 OU had fundus abnormalities and was re- associated with Sturge-Weber syndrome. -

Neuroradiology for Ophthalmologists
Eye (2020) 34:1027–1038 https://doi.org/10.1038/s41433-019-0753-z REVIEW ARTICLE Neuroradiology for ophthalmologists 1 2 1 1,3,4,5,6,7 Bayan Al Othman ● Jared Raabe ● Ashwini Kini ● Andrew G. Lee Received: 3 June 2019 / Revised: 29 October 2019 / Accepted: 24 November 2019 / Published online: 2 January 2020 © The Author(s), under exclusive licence to The Royal College of Ophthalmologists 2020 Abstract This article will review the best approaches to neuroimaging for specific ophthalmologic conditions and discuss characteristic radiographic findings. A review of the current literature was performed to find recommendations for the best approaches and characteristic radiographic findings for various ophthalmologic conditions. Options for imaging continue to grow with modern advances in technology, and ophthalmologists should stay current on the various radiographic techniques available to them, focusing on their strengths and weaknesses for different clinical scenarios. Introduction Computed tomography (CT) 1234567890();,: 1234567890();,: Modern imaging technology continues to advance the CT imaging reconstructs a three-dimensional image made boundaries and increase the options available to physicians of many conventional x-ray images. The conventional x-ray with respect to neuroradiology. In ophthalmology, the most images are ordered in tomographic slices that have been common studies employed are computed tomography (CT) computerized so a viewer can scroll through the images, and magnetic resonance imaging (MRI). There are several analyzing sequential cross-sections [1]. Density is the pri- different types of protocols that provide unique advantages mary characteristic that determines image appearance on a and disadvantages depending on the clinical scenario. This CT scan. As with traditional x-rays, tissues appear on a grey article endeavours to review those options and discuss how scale ranging from white (i.e., hyperdense tissues such as they are best employed to evaluate a variety of specific bone) to black (i.e., hypodense materials such as air). -
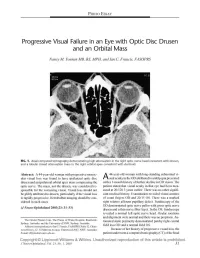
Progressive Visual Failure in an Eye with Optic Disc Drusen and an Orbital Mass
PHOTO ESSAY Progressive Visual Failure in an Eye with Optic Disc Drusen and an Orbital Mass Nancy M. Younan MB, BS, MPH, and Ian C. Francis, FASOPRS FIG. 1. Axial computed tomography demonstrating high attenuation in the right optic nerve head consistent with drusen, and a lobular mixed attenuation mass in the right orbital apex consistent with dermoid. Abstract: A 44-year-old woman with progressive monoc 44-year-old woman with long-standing subnormal vi ular visual loss was found to have ipsilateral optic disc A sual acuity in the OD attributed to amblyopia presented drusen and an ipsilateral orbital apex mass compressing the with a 1-month history of further decline in OD vision. The optic nerve. The mass, not the drusen, was considered re patient stated that visual acuity in that eye had been mea sponsible for the worsening vision. Visual loss should not sured at 20/120 3 years earlier. There was no other signifi be glibly attributed to drusen, particularly if the visual loss cant medical history. Examination revealed visual acuities is rapidly progressive. Retrobulbar imaging should be con of count fingers OD and 20/15 OS. There was a marked sidered in such cases. right relative afferent pupillary defect. Funduscopy of the OD demonstrated optic nerve pallor with gross optic nerve (JNeuro-Ophthalmol 2003;23: 31-33) drusen and a thin nerve fiber layer. In the OS, funduscopy revealed a normal left optic nerve head. Ocular rotations and alignment were normal and there was no proptosis. Au The Ocular Plastics Unit, The Prince of Wales Hospital, Randwick, tomated static perimetry demonstrated patchy right central Sydney, Australia, and the University of NSW, Sydney, Australia. -

Optic Disc Drusen, Glaucoma, Or Could It Be Both?
Title: Where are the defects coming from…Optic Disc Drusen, Glaucoma, or could it be both? Authors: Rachel Goretsky OD, Biana Gekht OD Abstract: Optic disc drusen and glaucoma cause similar retinal nerve fiber layer(RNFL) as well as visual field defects. This paper describes a patient who has both conditions and the management involved. I. Case History: 66 year old African-American male presents for dilation and imaging. Patient has a history of Glaucoma for several years; he is taking Brimonidine bid OU and Latanoprost qhs OU with reported good compliance. Medical & Ocular History: • Hypertension, gout, cholesterol and stents placed in leg and chest. Glaucoma OU. History of peripheral iridotomy OU one year ago. Medications:Amplodipine, clopidogrel, allopurinol II. Pertinent findings: • Maximum pressure history is 17 OD, 19 OS, current visit 16 OD, 19 OS • Anterior chamber : Grade 2 Van Herick Angles OU • Iris: Peripheral Iridotomy, patent at 12 o’clock OD,OS • Optic disc: 0.3r OD, OS small nerves, mild blurry margins indicative of disc drusen • Macula: diffuse epiretinal membrane OU • Pachymetry : 556 OD/ 566 OS • Gonioscopy: open to trabecular meshwork (TM) superiorly, otherwise no structures visible OD, open to TM inferiorly, otherwise no structures visible OS • Spectralis Optical Coherence Tomography(OCT): optic disc drusen with small cups and disc area OU • Visual field exhibited no defects OD, inferior nasal defects OS. III. Differential Diagnosis: • Papilledema, tilted discs, pseudotumor cerebri, myelinated nerve fiber layer IV. Diagnosis and Discussion Optic nerve head drusen are hyaline deposits made of calcium phosphate as well as amino acids, among other materials. -

The Alter Retina: Alternative Splicing of Retinal Genes in Health and Disease
International Journal of Molecular Sciences Review The Alter Retina: Alternative Splicing of Retinal Genes in Health and Disease Izarbe Aísa-Marín 1,2 , Rocío García-Arroyo 1,3 , Serena Mirra 1,2 and Gemma Marfany 1,2,3,* 1 Departament of Genetics, Microbiology and Statistics, Avda. Diagonal 643, Universitat de Barcelona, 08028 Barcelona, Spain; [email protected] (I.A.-M.); [email protected] (R.G.-A.); [email protected] (S.M.) 2 Centro de Investigación Biomédica en Red Enfermedades Raras (CIBERER), Instituto de Salud Carlos III (ISCIII), Universitat de Barcelona, 08028 Barcelona, Spain 3 Institute of Biomedicine (IBUB, IBUB-IRSJD), Universitat de Barcelona, 08028 Barcelona, Spain * Correspondence: [email protected] Abstract: Alternative splicing of mRNA is an essential mechanism to regulate and increase the diversity of the transcriptome and proteome. Alternative splicing frequently occurs in a tissue- or time-specific manner, contributing to differential gene expression between cell types during development. Neural tissues present extremely complex splicing programs and display the highest number of alternative splicing events. As an extension of the central nervous system, the retina constitutes an excellent system to illustrate the high diversity of neural transcripts. The retina expresses retinal specific splicing factors and produces a large number of alternative transcripts, including exclusive tissue-specific exons, which require an exquisite regulation. In fact, a current challenge in the genetic diagnosis of inherited retinal diseases stems from the lack of information regarding alternative splicing of retinal genes, as a considerable percentage of mutations alter splicing Citation: Aísa-Marín, I.; or the relative production of alternative transcripts. Modulation of alternative splicing in the retina García-Arroyo, R.; Mirra, S.; Marfany, is also instrumental in the design of novel therapeutic approaches for retinal dystrophies, since it G. -
Optic Nerve on Sheath:
3/16/2018 < Optic nerve axons of retinal ganglion cells 1.2 million nerve fibers . ON sheath: continuous with the meninges dura、arachnoid and pia mater 1 3/16/2018 optic nerve functions 1.Visual Acuity 2.Color Vision 3.Pupil 4.Contrast sensitivity Ancillary Tests 1.Visual Field 2.Neuro-imaging 3.OCT 4.VEP Etiology:Optic nerve diseases 1.inflammation:optic neuritis 2 . ischemic optic neuropathy 3-Compression 4-Granuloma & infiltration 5-Hereditary 6-Toxic 7-Irradiation 8- Trauma . 2 3/16/2018 Optic Neuritis 3-Neuroretinitis 1-Retrobulbar neuritis 2-Papillitis Papillitis optic disc is normal hyperemia and edema with macular star . in adults common in children. least common type with multiple sclerosis. viral infections Rapid unilateral loss of vision RAPD Loss of color vision Pain in moving the eye Swollen disc with or without peripapillary flame-shaped hemorrhages. 3 3/16/2018 Fig optic neuritis Centrocecal scotoma Bilateral optic neuritis Bilateral Central scotoma 4 3/16/2018 Bilateral hemianopsia MRI demyelinating lesions multiple sclerosis Neuromylitis Optica VF showed non- central scotoma altitudinal VF an ischemic mechanism play a role in ON in NMO patients 5 3/16/2018 Optic Neuritis Follow Up Diffuse and central loss in the affected eye at baseline Follow Up : nerve fiber bundle defects were the predominant localized abnormalities in both the affected and fellow eyes physicians evaluate the characteristics of optic neuritis and other optic neuropathies in the future Ischemic optic neuropathy ( ION) 6 3/16/2018 Anterior ischemic optic neuropathy ( AION ) Arteritic Non- Arteritic GCA - vasculitis hypoperfusion of ONH transient visual loss, temporal sudden painless loss of vision pain, jaw pain, fatigue, weight loss hyperemic disc Pale disc Sectorial, diffuse edema optic disc edema splinter hemorrhages of a chalky white color Subsequent optic atrophy Nonarteritic ischemic optic neuropathy visual field altitudinal field defect 7 3/16/2018 NAION sudden, painless visual loss OS shows AION .