Tendon Transfer for Foot Drop: a Simple Procedure with Effective Outcome Local Experience
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

GBS/CIDP Foundation International
Guillain-Barré Syndrome GBS: An Acute Care Guide For Medical Professionals A publication of the GBS/CIDP Foundation International Guillain-Barré Syndrome: An Acute Care Guide For Medical Professionals A publication of the GBS/CIDP Foundation International 2012 Edition GBS/CIDP Foundation International The Holly Building 104 1/2 Forrest Avenue Narberth, PA 19072 Phone: 610.667.0131 Toll Free: 866.224.3301 Fax: 610.667.7036 [email protected] www.gbs-cidp.org Guillain-Barré Syndrome: An Acute Care Guide For Medical Professionals Contents Page Acknowledgements . i Introduction . 1 Initial Patient Evaluation . 4 Natural History of GBS: Implications for Patient Care . 6 Respiratory Complications . 8 Dysautonomia and Cardiovascular Complications . 12 Bladder, Bowel Dysfunction . 14 Metabolism: Nutrition, Hydration, Electrolytes . 14 Pain . 17 ICU Delirium . 18 Skin . 18 Musculo-Skeletal Issues, Occupational and Physical Therapy . 19 Infection . 22 Disorder Specific Treatments . 22 Appendix A. Checklist of Patient Issues to Monitor . 24 B. Diagnostic Criteria for GBS . 25 C. Prognosis . 26 References . 27 This pamphlet is provided as a service of the GBS/CIDP Foundation International Serving the medical community and patients with Guillain-Barré syndrome and related acute and chronic paralyzing disorders of the peripheral nerves. Acknowledgements Guillain-Barré syndrome (GBS) is a rare disorder. Some health professionals may not be familiar with treating it. A beautiful video by Tanya Ooraikul chronicled the superb care provided to her husband Kit during his recovery from GBS. His care at Gray Nuns Community Hospital in Edmonton, Alberta, Canada included 86 days in the intensive care unit. The video handsomely demonstrates the high quality of care that can be provided for this rare and complicated disorder in a community hospital. -
Unilateral Foot Drop: an Unusual Presentation of a More Common
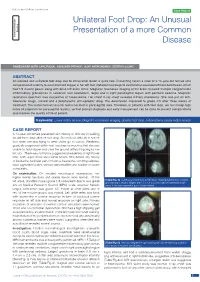
DOI: 10.7860/JCDR/2017/26249.10738 Case Report Unilateral Foot Drop: An Unusual Section Presentation of a more Common Internal Medicine Disease RAMESHWAR NATH CHAURASIA1, ABHISHEK PathaK2, VIJAY nath MISHRA3, DEEPIKA JOSHI4 ABSTRACT An isolated and unilateral foot drop due to intracranial lesion is quite rare. Presenting herein a case of a 14-year-old female who complained of inability to wear and hold slipper in her left foot. Detailed neurological examination revealed left foot dorsiflexion which had 1/5 muscle power along with brisk left ankle reflex. Magnetic resonance imaging of the brain revealed multiple conglomerate inflammatory granulomas in cerebrum and cerebellum, larger one in right parasagittal region with perifocal oedema. Magnetic resonance spectrum was suggestive of tuberculoma. Her chest X-ray chest revealed milliary shadowing. She was put on anti- tubercular drugs, steroid and a prophylactic anti-epileptic drug. The dorsiflexion improved to grade 4/5 after three weeks of treatment. The motor homunculus for foot is located in parasagittal area. Therefore, in patients with foot drop, we must keep high index of suspicion for parasagittal lesions, so that prompt diagnosis and early management can be done to prevent complications and improve the quality of life of patient. Keywords: Lower motor neuron, Magnetic resonance imaging, Spastic foot drop, Tuberculoma, Upper motor neuron CASE REPORT A 14-year-old female presented with history of difficulty in walking for last three days after left foot drop. She noticed difficulty in her left foot when she was trying to wear shoes go to school. Weakness gradually progressed within next two days so much so that she was unable to hold slipper and clear the ground without tripping by her left foot. -
Physical Therapy & FSHD
Physical Therapy & FSHD Facioscapulohumeral Muscular Dystrophy A Guide for Patients & Physical Therapists Authors: Wendy M. King, P.T., Assistant Professor, Neurology & Shree Pandya, P.T., M.S., Assistant Professor, Neurology & Physical Medicine and Rehabilitation A publication of the FSH Society, Inc. www.fshsociety.org Table of Contents Introduction ...............................................................................4 Facioscapulohumeral Dystrophy (FSHD) .....................5 Manifestations of Impairments Related to FSHD ......5 Exercise and FSHD ...................................................................7 Hydrotherapy (Water Therapy) and FSHD ..................9 Pain and FSHD ...........................................................................9 Surgical Management of Scapular Problems ............11 Who Are Physical Therapists &What Can You Expect When You See Them? .................................12 To Physical Therapists .......................................................14 Treatment of Pain .................................................................15 Summary ...................................................................................16 References ................................................................................17 About the FSH Society .........................................................18 Contact Information .............................................................19 ‐3‐ Introduction he purpose of this guide is to assist physical T therapists and patients to develop -

Foot Drop Schema Script
CPS Foot Drop Schema Script Hi everyone - my name is Maniraj. I’m excited to narrate this Clinical Problem Solvers schema on foot drop. Foot drop is really a story about a weakness or paralysis in the muscles that dorsiflex the foot. A patient with foot drop will drag their toes while walking. To avoid tripping over their toes while walking, a patient will lift their foot higher off the ground. Since there is no dorsiflexion for a heel strike when bringing their foot down, the patient “overshoots” and slaps their foot on the ground. This is called a steppage gait. What muscles are we talking about? The main dorsiflexor muscles are the tibialis anterior and the extensors of the toes (extensor hallucis longus and extensor digitorum longus). All of these muscles are innervated by the deep peroneal nerve, which is a branch of the common peroneal nerve. The peroneal nerve itself is a terminal branch of the sciatic nerve; the other branch of the sciatic is the tibial nerve. To help anchor the nerve functions we’ll be talking about, I think it’d be beneficial to first review acronyms that can be used to memorize them. The peroneal nerve functions to evert and dorsiflex at the ankle, which can be remembered by the acronym PED. The tibial nerve functions to invert and plantarflex at the ankle, so that becomes TIP. Since the sciatic nerve is really just the bundle of peroneal & tibial nerves, you can remember the sciatic nerve functions as PED + TIP. The sciatic nerve also supplies the hamstrings, which flex the leg at the knee. -

Prescription of Foot and Ankle Orthoses for Children with Charcot–Marie–Tooth Disease: a Review of the Evidence
Narrative Review Prescription of foot and ankle orthoses for children with Charcot–Marie–Tooth disease: a review of the evidence Grant Scheffers1, Claire Hiller1, Kathryn Refshauge1, Joshua Burns1,2 1Faculty of Health Sciences, The University of Sydney, Australia, 2Institute for Neuroscience and Muscle Research, The Children’s Hospital at Westmead, Australia Background: Charcot–Marie–Tooth disease (CMT) is the most common inherited peripheral neuropathy and is associated with debilitating lower limb impairments and activity limitations. These impairments and activity limitations are potentially amendable to the prescription of orthoses, yet there is no universal, literature-based consensus to inform the decision making process of whether or not orthoses are indicated for a particular child with CMT, and if so, what type of device. Objectives: The aims of this paper were to: (1) review the lower limb impairments and activity limitations of children with CMT; (2) review the indications of commonly prescribed foot and ankle orthoses; and (3) formulate a clinical algorithm for the optimal prescription of foot and ankle orthoses for children with CMT. Major findings: We conducted a comprehensive search of the major databases and reference lists of relevant articles and books. In general, in-shoe orthoses are indicated for children with CMT and pes cavus and foot pain and/or mild balance impairments, whilst ankle-foot orthoses are indicated for children with CMT and pes cavus, foot drop, global foot and ankle muscle weakness and/or ankle equinus, and moderate-severe balance impairments and/or difficulty walking. Conclusions: A clinical algorithm is proposed to guide the prescription of foot and ankle orthoses for children with CMT. -

Diagnosis and Treatment of Facioscapulohumeral Muscular Dystrophy: 2015 Guidelines Steven Karceski Neurology 2015;85;E41-E43 DOI 10.1212/WNL.0000000000001865
PATIENT PAGE Section Editors Diagnosis and treatment of DavidC.Spencer,MD Steven Karceski, MD facioscapulohumeral muscular dystrophy 2015 guidelines Steven Karceski, MD WHAT DID THE AUTHORS STUDY? Dr. Tawil led a in people with FSHD. However, a person with committee of doctors who specialize in diagnosing FSHD could develop heart problems unrelated to and treating facioscapulohumeral muscular dystrophy FSHD. If a person with FSHD developed heart prob- (FSHD). Together, they reviewed published articles lems, he or she would need to see a doctor for an eval- and research in FSHD and similar muscular dystro- uation and treatment. phies. They assembled detailed recommendations Although rare, patients with a low number of about the diagnosis and treatment of people with copies of D4Z4 may develop problems with their FSHD.1 vision. They develop Coats disease, which can be de- tected by an ophthalmologist using special equip- HOW IS FSHD DIAGNOSED? The initial step to the ment called indirect ophthalmoscopy. In short, a diagnosis of FSHD is taking a careful medical history. person who has a low number of copies should be This starts in the doctor’s office. The doctor will ask screened and evaluated for this possibility by a many questions about the person’s weakness: how it trained eye specialist. started, where it is most noticeable, how quickly it is Pain is common in people with FSHD. The pain worsening, and whether there is a family history of occurs in the muscles and bones. It often responds to the same kind of problem. If there is a family history several medications and physical therapy. -

Dissociated Leg Muscle Atrophy in Amyotrophic Lateral
www.nature.com/scientificreports OPEN Dissociated leg muscle atrophy in amyotrophic lateral sclerosis/ motor neuron disease: the ‘split‑leg’ sign Young Gi Min1,4, Seok‑Jin Choi2,4, Yoon‑Ho Hong3, Sung‑Min Kim1, Je‑Young Shin1 & Jung‑Joon Sung1* Disproportionate muscle atrophy is a distinct phenomenon in amyotrophic lateral sclerosis (ALS); however, preferentially afected leg muscles remain unknown. We aimed to identify this split‑leg phenomenon in ALS and determine its pathophysiology. Patients with ALS (n = 143), progressive muscular atrophy (PMA, n = 36), and age‑matched healthy controls (HC, n = 53) were retrospectively identifed from our motor neuron disease registry. We analyzed their disease duration, onset region, ALS Functional Rating Scale‑Revised Scores, and results of neurological examination. Compound muscle action potential (CMAP) of the extensor digitorum brevis (EDB), abductor hallucis (AH), and tibialis anterior (TA) were reviewed. Defned by CMAPEDB/CMAPAH (SIEDB) and CMAPTA/CMAPAH (SITA), respectively, the values of split‑leg indices (SI) were compared between these groups. SIEDB was signifcantly reduced in ALS (p < 0.0001) and PMA (p < 0.0001) compared to the healthy controls (HCs). SITA reduction was more prominent in PMA (p < 0.05 vs. ALS, p < 0.01 vs. HC), but was not signifcant in ALS compared to the HCs. SI was found to be signifcantly decreased with clinical lower motor neuron signs (SIEDB), while was rather increased with clinical upper motor neuron signs (SITA). Compared to the AH, TA and EDB are more severely afected in ALS and PMA patients. Our fndings help to elucidate the pathophysiology of split‑leg phenomenon. -

Charcot-Marie-Tooth Disease and Other Genetic Polyneuropathies
Review Article 04/25/2018 on mAXWo3ZnzwrcFjDdvMDuzVysskaX4mZb8eYMgWVSPGPJOZ9l+mqFwgfuplwVY+jMyQlPQmIFeWtrhxj7jpeO+505hdQh14PDzV4LwkY42MCrzQCKIlw0d1O4YvrWMUvvHuYO4RRbviuuWR5DqyTbTk/icsrdbT0HfRYk7+ZAGvALtKGnuDXDohHaxFFu/7KNo26hIfzU/+BCy16w7w1bDw== by https://journals.lww.com/continuum from Downloaded Downloaded Address correspondence to Dr Sindhu Ramchandren, University of Michigan, from Charcot-Marie-Tooth Department of Neurology, https://journals.lww.com/continuum 2301 Commonwealth Blvd #1023, Ann Arbor, MI 48105, Disease and [email protected]. Relationship Disclosure: Dr Ramchandren has served Other Genetic on advisory boards for Biogen and Sarepta Therapeutics, by mAXWo3ZnzwrcFjDdvMDuzVysskaX4mZb8eYMgWVSPGPJOZ9l+mqFwgfuplwVY+jMyQlPQmIFeWtrhxj7jpeO+505hdQh14PDzV4LwkY42MCrzQCKIlw0d1O4YvrWMUvvHuYO4RRbviuuWR5DqyTbTk/icsrdbT0HfRYk7+ZAGvALtKGnuDXDohHaxFFu/7KNo26hIfzU/+BCy16w7w1bDw== Inc, and has received research/grant support from Polyneuropathies the Muscular Dystrophy Association (Foundation Sindhu Ramchandren, MD, MS Clinic Grant) and the National Institutes of Health (K23 NS072279). Unlabeled Use of ABSTRACT Products/Investigational Purpose of Review: Genetic polyneuropathies are rare and clinically heterogeneous. Use Disclosure: This article provides an overview of the clinical features, neurologic and electrodiagnostic Dr Ramchandren reports no disclosure. findings, and management strategies for Charcot-Marie-Tooth disease and other * 2017 American Academy genetic polyneuropathies as well as an algorithm for genetic testing. of Neurology. -

Understanding Foot Drop Diagnosis and Treatment WHAT IS FOOT DROP?
Understanding Foot Drop Diagnosis and Treatment WHAT IS FOOT DROP? First and foremost, Foot Drop inability to lift and control the is not a disease, but rather forefoot. It typically affects a symptom of an underlying only one foot but can also neurological, muscular or ana- affect both feet and it can be tomical condition. The term temporary or permanent. “Foot Drop”, or sometimes “Drop Foot”, describes the WHAT ARE THE SYMPTOMS? Typical signs and symptoms of • Dragging the forefoot Foot Drop may include: on the floor as you walk • Slapping the foot to the floor with each step • Frequent or increased incidence of falling or stumbling • Not able to voluntarily point toes upwards and/or move • Difficulty lifting toes or forefoot ankle from side to side • Vaulting toe-walking on sound • Pain, weakness or numbness in side, to clear swing through of the foot or toes affected side WHY IS THIS HAPPENING? Foot Drop is caused by weakness or paralysis of the muscles below the knee that lift the foot. The underlying causes are varied and symptoms may overlap. Causes may include: • Conditions that affect the spinal cord or brain, such as Cerebral Palsy, Multiple Sclerosis or Stroke may cause Foot Drop. • It can also result from injury to the nerves in the lower back, leg or after a trauma to the lower leg. Nerve damage may occur from a surgical procedure such as hip or knee replacement. Damage or injury to the nerves can also occur as a result from Spinal Stenosis. • Diseases such as Muscle Dystrophy, Charcot-Marie-Tooth (CMT) or Myosistis which can cause progressive muscle weakness which can contribute to Foot Drop. -

Foot Drop Caused by a Focal Brain Injury - Two Case Report
CASE REPORT J Kor Neurotraumatol Soc 1(1):118-121, 2005 Foot Drop Caused by A Focal Brain Injury - Two Case Report - Min-Su Kang, M.D., Jin-Young Youm, M.D., Seung-Won Choi, M.D., Sun-Hwan Kim, M.D., Hyeon-Song Koh, M.D., Shi-Hun Song, M.D., and Youn Kim, M.D. Department of Neurosurgery, College of Medicine, Chungnam National University, Daejeon, Korea Foot drop is caused by peripheral and spinal motor neuron lesions and muscular dystrophy. Foot drop secondary to brain lesions is rarely seen in practice. We present two cases with foot drop caused by focal brain injury. A 49-year-old male patient was admitted with right foot drop for 4m falling down injury. Neurologic examination revealed normal except for weakness at dorsiflexion of the right ankle and big toe. L-spine MRI, L-spine CT and both legs EMG showed normal findings. A 69-year-old male patient was referred with left foot drop and headache after bicycle accident. Neurological examinations showed normal except for weakness in dorsiflexion of the left ankle and big toe without sensory loss. L-spine MRI, L-spine CT and both legs EMG showed normal findings. In first case, there are important focal brain injury lesions in premotor area and SMA. In second case, premotor area, SMA and primary motor area may be damaged. In two cases, hemorrhagic cortical contusions in parasagittal area were the causes of the foot drop. And the foot drop was the initial clinical presentation in both cases. Clinicians, if they detect upper motor type neurologic deficits such as positive Babinski' sign, hyper-reflexia or clonus in a patient with a foot drop, should take into account the possibility of central lesion as reason for the foot drop. -

Correction of Dropped Foot Using Functional Electrical Stimulation (FES)
Functional Electrical Stimulation (FES) Clinical Service at the National Clinical FES Centre Salisbury District Hospital & OML Outreach Clinics Correction of Dropped Foot and other gait problems Dropped foot is the inability to lift the foot as the leg swings forward when walking. It is caused by weakness in the muscles that lift the foot and/or excessive activity (spasticity) in the antagonist muscles. Dropped foot increases the risk of falls, reduces mobility and participation. Functional Electrical Stimulation (FES) is the production of functional movement in paralysed muscles by the application of small pulses of electrical current to the nerves that supply them. The Odstock Dropped Foot Stimulator (ODFS) stimulates the common peroneal nerve using self adhesive skin electrodes mounted on the lower leg. Stimulation is timed to the walking cycle by using a pressure switch placed in the shoe under the heel. Stimulation begins when the heel is lifted from the ground and ends just after heel strike. Stimulation causes the foot to lift and stabilises the ankle when it is returned to the ground. The ODFS is primarily used as a long term orthosis. However, therapeutic training benefit has been demonstrated in people who have a dropped foot due to stroke, spinal cord injury, Parkinson’s and some people with MS. The main effects of the ODFS are: Increased safety due to reduced tripping and increased stability in stance. Increased walking speed and range. Reduced effort of walking. Greater confidence and independence. The ODFS is a practical device with adherence to treatment at one year of 86%. FES can be used to assist in any neurological condition resultant from an upper motor- neuron lesion. -

PERIPHERAL NEUROPATHY Ralph F
PERIPHERAL NEUROPATHY Ralph F. Józefowicz, MD Peripheral neuropathy is a general term for any disorder affecting the peripheral nerves. Since peripheral neuropathy can be caused by numerous factors, an investigation into the cause of the neuropathy should be undertaken as soon as the diagnosis of neuropathy is made. CLINICAL FEATURES Symptoms Since the peripheral nervous system consists of motor, sensory and autonomic nerves, symptoms can fall into all three of these categories. • Sensory symptoms include distal dysesthesias, pain and numbness. A characteristic pattern of numbness is one in which the distal portions of the nerves are first affected, the so-called "stocking-glove" pattern. This pattern occurs because nerve fibers are affected according to length of axon, without regard to root or nerve trunk distribution. • Motor symptoms include weakness, which once again is distal, and typically involves extensor groups rather than flexor groups of muscles. • Autonomic dysfunction is common and includes orthostasis, impotence in males and gastroparesis. Signs Signs of peripheral neuropathy also include sensory, motor and autonomic components. • Sensory disturbance is manifest as distal loss of pin, temperature and vibratory perception as well as proprioception. Initial signs are frequently confined to the toes and feet. A positive Romberg sign is frequently present due to proprioceptive loss in the lower extremities. • Motor signs include distal weakness, primarily in extensor groups, and most prominent in the lower extremities initially. Distal muscles are often atrophic, and one should carefully assess the bulk of the extensor digitorum brevis muscles in the feet and of the intrinsic muscles of the hands. Muscle tone is reduced and often is flaccid.