GBS/CIDP Foundation International
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-
Unilateral Foot Drop: an Unusual Presentation of a More Common
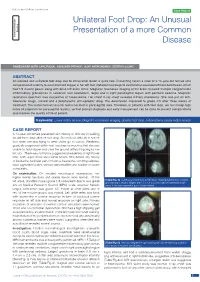
DOI: 10.7860/JCDR/2017/26249.10738 Case Report Unilateral Foot Drop: An Unusual Section Presentation of a more Common Internal Medicine Disease RAMESHWAR NATH CHAURASIA1, ABHISHEK PathaK2, VIJAY nath MISHRA3, DEEPIKA JOSHI4 ABSTRACT An isolated and unilateral foot drop due to intracranial lesion is quite rare. Presenting herein a case of a 14-year-old female who complained of inability to wear and hold slipper in her left foot. Detailed neurological examination revealed left foot dorsiflexion which had 1/5 muscle power along with brisk left ankle reflex. Magnetic resonance imaging of the brain revealed multiple conglomerate inflammatory granulomas in cerebrum and cerebellum, larger one in right parasagittal region with perifocal oedema. Magnetic resonance spectrum was suggestive of tuberculoma. Her chest X-ray chest revealed milliary shadowing. She was put on anti- tubercular drugs, steroid and a prophylactic anti-epileptic drug. The dorsiflexion improved to grade 4/5 after three weeks of treatment. The motor homunculus for foot is located in parasagittal area. Therefore, in patients with foot drop, we must keep high index of suspicion for parasagittal lesions, so that prompt diagnosis and early management can be done to prevent complications and improve the quality of life of patient. Keywords: Lower motor neuron, Magnetic resonance imaging, Spastic foot drop, Tuberculoma, Upper motor neuron CASE REPORT A 14-year-old female presented with history of difficulty in walking for last three days after left foot drop. She noticed difficulty in her left foot when she was trying to wear shoes go to school. Weakness gradually progressed within next two days so much so that she was unable to hold slipper and clear the ground without tripping by her left foot. -
Physical Therapy & FSHD
Physical Therapy & FSHD Facioscapulohumeral Muscular Dystrophy A Guide for Patients & Physical Therapists Authors: Wendy M. King, P.T., Assistant Professor, Neurology & Shree Pandya, P.T., M.S., Assistant Professor, Neurology & Physical Medicine and Rehabilitation A publication of the FSH Society, Inc. www.fshsociety.org Table of Contents Introduction ...............................................................................4 Facioscapulohumeral Dystrophy (FSHD) .....................5 Manifestations of Impairments Related to FSHD ......5 Exercise and FSHD ...................................................................7 Hydrotherapy (Water Therapy) and FSHD ..................9 Pain and FSHD ...........................................................................9 Surgical Management of Scapular Problems ............11 Who Are Physical Therapists &What Can You Expect When You See Them? .................................12 To Physical Therapists .......................................................14 Treatment of Pain .................................................................15 Summary ...................................................................................16 References ................................................................................17 About the FSH Society .........................................................18 Contact Information .............................................................19 ‐3‐ Introduction he purpose of this guide is to assist physical T therapists and patients to develop -

Foot Drop Schema Script
CPS Foot Drop Schema Script Hi everyone - my name is Maniraj. I’m excited to narrate this Clinical Problem Solvers schema on foot drop. Foot drop is really a story about a weakness or paralysis in the muscles that dorsiflex the foot. A patient with foot drop will drag their toes while walking. To avoid tripping over their toes while walking, a patient will lift their foot higher off the ground. Since there is no dorsiflexion for a heel strike when bringing their foot down, the patient “overshoots” and slaps their foot on the ground. This is called a steppage gait. What muscles are we talking about? The main dorsiflexor muscles are the tibialis anterior and the extensors of the toes (extensor hallucis longus and extensor digitorum longus). All of these muscles are innervated by the deep peroneal nerve, which is a branch of the common peroneal nerve. The peroneal nerve itself is a terminal branch of the sciatic nerve; the other branch of the sciatic is the tibial nerve. To help anchor the nerve functions we’ll be talking about, I think it’d be beneficial to first review acronyms that can be used to memorize them. The peroneal nerve functions to evert and dorsiflex at the ankle, which can be remembered by the acronym PED. The tibial nerve functions to invert and plantarflex at the ankle, so that becomes TIP. Since the sciatic nerve is really just the bundle of peroneal & tibial nerves, you can remember the sciatic nerve functions as PED + TIP. The sciatic nerve also supplies the hamstrings, which flex the leg at the knee. -

Prescription of Foot and Ankle Orthoses for Children with Charcot–Marie–Tooth Disease: a Review of the Evidence
Narrative Review Prescription of foot and ankle orthoses for children with Charcot–Marie–Tooth disease: a review of the evidence Grant Scheffers1, Claire Hiller1, Kathryn Refshauge1, Joshua Burns1,2 1Faculty of Health Sciences, The University of Sydney, Australia, 2Institute for Neuroscience and Muscle Research, The Children’s Hospital at Westmead, Australia Background: Charcot–Marie–Tooth disease (CMT) is the most common inherited peripheral neuropathy and is associated with debilitating lower limb impairments and activity limitations. These impairments and activity limitations are potentially amendable to the prescription of orthoses, yet there is no universal, literature-based consensus to inform the decision making process of whether or not orthoses are indicated for a particular child with CMT, and if so, what type of device. Objectives: The aims of this paper were to: (1) review the lower limb impairments and activity limitations of children with CMT; (2) review the indications of commonly prescribed foot and ankle orthoses; and (3) formulate a clinical algorithm for the optimal prescription of foot and ankle orthoses for children with CMT. Major findings: We conducted a comprehensive search of the major databases and reference lists of relevant articles and books. In general, in-shoe orthoses are indicated for children with CMT and pes cavus and foot pain and/or mild balance impairments, whilst ankle-foot orthoses are indicated for children with CMT and pes cavus, foot drop, global foot and ankle muscle weakness and/or ankle equinus, and moderate-severe balance impairments and/or difficulty walking. Conclusions: A clinical algorithm is proposed to guide the prescription of foot and ankle orthoses for children with CMT. -

Diagnosis and Treatment of Facioscapulohumeral Muscular Dystrophy: 2015 Guidelines Steven Karceski Neurology 2015;85;E41-E43 DOI 10.1212/WNL.0000000000001865
PATIENT PAGE Section Editors Diagnosis and treatment of DavidC.Spencer,MD Steven Karceski, MD facioscapulohumeral muscular dystrophy 2015 guidelines Steven Karceski, MD WHAT DID THE AUTHORS STUDY? Dr. Tawil led a in people with FSHD. However, a person with committee of doctors who specialize in diagnosing FSHD could develop heart problems unrelated to and treating facioscapulohumeral muscular dystrophy FSHD. If a person with FSHD developed heart prob- (FSHD). Together, they reviewed published articles lems, he or she would need to see a doctor for an eval- and research in FSHD and similar muscular dystro- uation and treatment. phies. They assembled detailed recommendations Although rare, patients with a low number of about the diagnosis and treatment of people with copies of D4Z4 may develop problems with their FSHD.1 vision. They develop Coats disease, which can be de- tected by an ophthalmologist using special equip- HOW IS FSHD DIAGNOSED? The initial step to the ment called indirect ophthalmoscopy. In short, a diagnosis of FSHD is taking a careful medical history. person who has a low number of copies should be This starts in the doctor’s office. The doctor will ask screened and evaluated for this possibility by a many questions about the person’s weakness: how it trained eye specialist. started, where it is most noticeable, how quickly it is Pain is common in people with FSHD. The pain worsening, and whether there is a family history of occurs in the muscles and bones. It often responds to the same kind of problem. If there is a family history several medications and physical therapy. -

Eating-Disorders-Mar-Handout.Pdf
More specifically…. How/Is it possible to move (back) towards Intuitive/Conscious Eating once diagnosed/treated for an eating disorder??? Introduction Anastasia Nevin MS RD RYT Registered Dietitian/Nutritionist and Yoga Teacher in NYC Owner of Anastasia Health LLC, a full-time Manhattan based nutrition and yoga private practice treating men and women struggling with eating disorder, disordered eating and body image issues Phoenix Rising Yoga Therapy training, Restorative Yoga and Ayurveda, integrating movement, breath, mindfulness, and body awareness through an integrative healing Psychology degree from Stanford University, Nutrition MS RD from Columbia University Worked as Lead Nutritionist/Yoga Therapist at Monte Nido’s EDTNY, helped found NYC program IOP Nutritionist/Yoga Therapist at Renfrew Center NYC www.anastasia-health.com Myths about Food and Recovery “Just eat the food” mentality Eating Disorder is just a way of seeking attention All people with eating disorders are extremely thin Eating disorders are about vanity Eating disorders are a result of poor parenting A person with an eating disorder can choose to stop whenever they want Challenges to Eating for the Eating Disorder Patient Food for the ED patient is the “enemy” Fear of weight gain***!! Gastrointestinal Pain/Delayed Gastric Emptying Increased Distress/Anxiety Hypermetabolism Poor Body Image Increased urge to use ED behaviors to compensate (restricting, purging, laxatives, exercise) Eating Disorder Statistics Eating Disorders are a daily struggle -

Effects of Hypermetabolism on Ventilation and Chemosensitivity
Effects of Hypermetabolism on Ventilation and Chemosensitivity Clifford W. Zwillich, … , Steven A. Sahn, John V. Weil J Clin Invest. 1977;60(4):900-906. https://doi.org/10.1172/JCI108844. Research Article Muscular exercise is associated with hypermetabolism and increased hypoxic ventilatory response (HVR). In order to dissociate mechanical and metabolic factors, the effect of hypermetabolism on hypoxic ventilatory response was evaluated at rest. Carbohydrate and protein feeding increases metabolic rate, and their effects on chemosensitivity, ventilation, and blood pH were evaluated in six normal subjects 2 h and 3 h after calorically equal test meals (1,000 cal). After carbohydrate, base-line oxygen consumption (Vȯ 2) increased from 237±11.3 ml/min (SEM) to 302±19.4 (P < 0.001) and 303±18.5 (P < 0.001) at 2 h and 3 h, respectively. Hypoxic ventilatory response, measured as shape parameter A, increased from a control of 144±11.8 to 330±61.0 (P < 0.01) at 2 h and 286±57.0 (P < 0.05) at 3 h. These changes were associated with a mild metabolic acidosis as pH decreased from a control of 7.402±0.004 to 7.371±0.009 (P < 0.005) at 2 h and 7.377±0.008 (P < 0.005) at 3 h. After protein, Vȯ 2 increased from 241±6.7 to 265±6.2 (P < 0.02) and 270±5.4 (P < 0.001), an overall increase less than that which occurred after carbohydrate (P < 0.01). Hypoxic ventilatory response increased from 105±14.5 to 198±24.3 P( < 0.02) at 2 h and 219±17.3 (P < 0.01) at 3 h, which was not different from the increase with carbohydrate. -

Enteral Nutrition in Patients with Respiratory Disease
Eur Respir J, 1996, 9, 364–370 Copyright ERS Journals Ltd 1996 DOI: 10.1183/09031936.96.09020364 European Respiratory Journal Printed in UK - all rights reserved ISSN 0903 - 1936 SERIES 'CLINICAL PHYSIOLOGY IN RESPIRATORY INTENSIVE CARE' Edited by A. Rossi and C. Roussos Enteral nutrition in patients with respiratory disease S.K. Pingleton Enteral nutrition in patients with respiratory disease. S.K. Pingleton. ©ERS Journals Division of Pulmonary Diseases and Critical Ltd 1996. Care Medicine, University of Kansas Medical ABSTRACT: Nutritional assessment and management is an important therapeutic Center, Kansas City, Kansas, USA. modality in patients with respiratory disease. Malnutrition adversely affects res- Correspondence: S.K. Pingleton, Division piratory function. Nutritional therapy for the spontaneously breathing patient of Pulmonary Diseases and Critical Care should include an appropriate diet plus the consideration of nutritional supplements. Medicine, University of Kansas Medical Complete nutritional support should be undertaken with enteral nutrition in criti- Center, 39th and Rainbow Blvd, Kansas cally ill patients with respiratory failure. Nutritional complications occur. Overfeed- City, Kansas 66160, USA ing can lead to nutritionally associated hypercapnia. Keywords: Enteral nutrition, malnutrition, Eur Respir J., 1996, 9, 364–370. respiratory disease Received: April 6 1995 Accepted for publication November 7, 1995 Nutrition is an important aspect of patient care in any failure (ARF) have a 60% incidence of malnutrition [3]. patient with respiratory disease. Malnutrition adversely Disease severity can be assessed by the degree of pulmo- effects lung function by diminishing respiratory muscle nary function and gas exchange abnormalities. Malnutri- strength, altering ventilatory capacity, and impairing tion occurs in 50% of patients with chronic hypoxaemia immune function. -

Amyloid Goiter in Familial Mediterranean Fever: Description of 42 Cases from a French Cohort and from Literature Review
Journal of Clinical Medicine Article Amyloid Goiter in Familial Mediterranean Fever: Description of 42 Cases from a French Cohort and from Literature Review Hélène Vergneault 1 , Alexandre Terré 1, David Buob 2,†, Camille Buffet 3 , Anael Dumont 4, Samuel Ardois 5, Léa Savey 1, Agathe Pardon 6,‡, Pierre-Antoine Michel 7, Jean-Jacques Boffa 7,†, Gilles Grateau 1,† and Sophie Georgin-Lavialle 1,*,† 1 Internal Medicine Department and National Reference Center for Autoinflammatory Diseases and Inflammatory Amyloidosis (CEREMAIA), APHP, Tenon Hospital, Sorbonne University, 4 rue de la Chine, 75020 Paris, France; [email protected] (H.V.); [email protected] (A.T.); [email protected] (L.S.); [email protected] (G.G.) 2 Department of Pathology, APHP, Tenon Hospital, Sorbonne University, 4 rue de la Chine, 75020 Paris, France; [email protected] 3 Thyroid Pathologies and Endocrine Tumor Department, APHP, Pitié-Salpêtrière Hospital, Sorbonne University, 47-83 Boulevard de l’Hôpital, 75013 Paris, France; [email protected] 4 Department of Internal Medicine, Caen University Hospital, Avenue de la Côte de Nacre, 14000 Caen, France; [email protected] 5 Department of Internal Medecine, Rennes Medical University, 2 rue Henri le Guilloux, 35000 Rennes, France; [email protected] 6 Dialysis Center, CH Sud Francilien, 40 Avenue Serge Dassault, 91100 Corbeil-Essonnes, France; [email protected] 7 Citation: Vergneault, H.; Terré, A.; Department of Nephrology, APHP, Tenon Hospital, 4 rue de la Chine, 75020 Paris, France; [email protected] (P.-A.M.); [email protected] (J.-J.B.) Buob, D.; Buffet, C.; Dumont, A.; * Correspondence: [email protected]; Tel.: +33-156016077 Ardois, S.; Savey, L.; Pardon, A.; † Groupe de Recherche Clinique amylose AA Sorbonne Université- GRAASU. -

Dissociated Leg Muscle Atrophy in Amyotrophic Lateral
www.nature.com/scientificreports OPEN Dissociated leg muscle atrophy in amyotrophic lateral sclerosis/ motor neuron disease: the ‘split‑leg’ sign Young Gi Min1,4, Seok‑Jin Choi2,4, Yoon‑Ho Hong3, Sung‑Min Kim1, Je‑Young Shin1 & Jung‑Joon Sung1* Disproportionate muscle atrophy is a distinct phenomenon in amyotrophic lateral sclerosis (ALS); however, preferentially afected leg muscles remain unknown. We aimed to identify this split‑leg phenomenon in ALS and determine its pathophysiology. Patients with ALS (n = 143), progressive muscular atrophy (PMA, n = 36), and age‑matched healthy controls (HC, n = 53) were retrospectively identifed from our motor neuron disease registry. We analyzed their disease duration, onset region, ALS Functional Rating Scale‑Revised Scores, and results of neurological examination. Compound muscle action potential (CMAP) of the extensor digitorum brevis (EDB), abductor hallucis (AH), and tibialis anterior (TA) were reviewed. Defned by CMAPEDB/CMAPAH (SIEDB) and CMAPTA/CMAPAH (SITA), respectively, the values of split‑leg indices (SI) were compared between these groups. SIEDB was signifcantly reduced in ALS (p < 0.0001) and PMA (p < 0.0001) compared to the healthy controls (HCs). SITA reduction was more prominent in PMA (p < 0.05 vs. ALS, p < 0.01 vs. HC), but was not signifcant in ALS compared to the HCs. SI was found to be signifcantly decreased with clinical lower motor neuron signs (SIEDB), while was rather increased with clinical upper motor neuron signs (SITA). Compared to the AH, TA and EDB are more severely afected in ALS and PMA patients. Our fndings help to elucidate the pathophysiology of split‑leg phenomenon. -

Charcot-Marie-Tooth Disease and Other Genetic Polyneuropathies
Review Article 04/25/2018 on mAXWo3ZnzwrcFjDdvMDuzVysskaX4mZb8eYMgWVSPGPJOZ9l+mqFwgfuplwVY+jMyQlPQmIFeWtrhxj7jpeO+505hdQh14PDzV4LwkY42MCrzQCKIlw0d1O4YvrWMUvvHuYO4RRbviuuWR5DqyTbTk/icsrdbT0HfRYk7+ZAGvALtKGnuDXDohHaxFFu/7KNo26hIfzU/+BCy16w7w1bDw== by https://journals.lww.com/continuum from Downloaded Downloaded Address correspondence to Dr Sindhu Ramchandren, University of Michigan, from Charcot-Marie-Tooth Department of Neurology, https://journals.lww.com/continuum 2301 Commonwealth Blvd #1023, Ann Arbor, MI 48105, Disease and [email protected]. Relationship Disclosure: Dr Ramchandren has served Other Genetic on advisory boards for Biogen and Sarepta Therapeutics, by mAXWo3ZnzwrcFjDdvMDuzVysskaX4mZb8eYMgWVSPGPJOZ9l+mqFwgfuplwVY+jMyQlPQmIFeWtrhxj7jpeO+505hdQh14PDzV4LwkY42MCrzQCKIlw0d1O4YvrWMUvvHuYO4RRbviuuWR5DqyTbTk/icsrdbT0HfRYk7+ZAGvALtKGnuDXDohHaxFFu/7KNo26hIfzU/+BCy16w7w1bDw== Inc, and has received research/grant support from Polyneuropathies the Muscular Dystrophy Association (Foundation Sindhu Ramchandren, MD, MS Clinic Grant) and the National Institutes of Health (K23 NS072279). Unlabeled Use of ABSTRACT Products/Investigational Purpose of Review: Genetic polyneuropathies are rare and clinically heterogeneous. Use Disclosure: This article provides an overview of the clinical features, neurologic and electrodiagnostic Dr Ramchandren reports no disclosure. findings, and management strategies for Charcot-Marie-Tooth disease and other * 2017 American Academy genetic polyneuropathies as well as an algorithm for genetic testing. of Neurology. -

Deep Brain Stimulation As a Treatment Approach for Anorexia
Published online: 2019-05-31 THIEME Review Article | Artigo de Revisão 175 Deep Brain Stimulation as a Treatment Approach for Anorexia Nervosa: a Systematic Literature Review Estimulação cerebral profunda como uma abordagem de tratamento para anorexia nervosa: Uma revisão sistemática de literatura Ledismar José da Silva1 Tâmara Husein Naciff1 Maria Flávia Vaz de Oliveira1 1 Department of Medicine, Pontifícia Universidade Católica de Goiás, Address for correspondence Ledismar José da Silva, Departmento Goiânia, GO, Brazil ode Medicina, Pontifícia Universidade Católica do Rio de Janeiro, Rua 235, 76 - Setor Leste Universitário, Goiânia, GO, 74175-120, Brazil Arq Bras Neurocir 2019;38:175–182. (e-mail: [email protected]). Abstract Anorexia nervosa is a psychiatric disorder characterized by distortions of body size, weight, and shape perception, as well as by food restriction and/or binge and purging behaviors. It mostly affects young women and causes severe negative impacts on their physical, psychological, and social health. Recent studies have analyzed deep brain stimulation (DBS), a neurosurgical procedure that involves electrode implantation in strategical brain Keywords areas, to obtain remission of the symptoms of anorexia nervosa. The results showed that ► anorexia nervosa the stimulation of areas associated to the neurocircuitry of anorexia nervosa, such as ► eating disorder nucleus accumbens, anterior cingulate cortex, ventral striatum, and bed nucleus of the stria ► deep brain terminalis, provokes beneficial responses in terms of body mass index, quality of life, social stimulation functioning, and psychiatric comorbidities. Nevertheless, broader investigations are ► neuromodulation needed to endorse the clinical usage of DBS in the management of anorexia nervosa. Resumo A anorexia nervosa é uma desordem psiquiátrica caracterizada pela distorção da percepção de tamanho, peso e formas corporais, bem como por restrição alimentar e/ou comporta- mentos excessivos e purgativos.