Opioid Toxicity and Overdose
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-
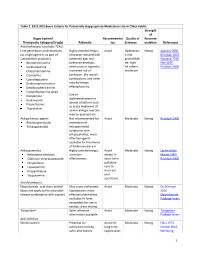
Table 2. 2012 AGS Beers Criteria for Potentially
Table 2. 2012 AGS Beers Criteria for Potentially Inappropriate Medication Use in Older Adults Strength of Organ System/ Recommendat Quality of Recomm Therapeutic Category/Drug(s) Rationale ion Evidence endation References Anticholinergics (excludes TCAs) First-generation antihistamines Highly anticholinergic; Avoid Hydroxyzin Strong Agostini 2001 (as single agent or as part of clearance reduced with e and Boustani 2007 combination products) advanced age, and promethazi Guaiana 2010 Brompheniramine tolerance develops ne: high; Han 2001 Carbinoxamine when used as hypnotic; All others: Rudolph 2008 Chlorpheniramine increased risk of moderate Clemastine confusion, dry mouth, Cyproheptadine constipation, and other Dexbrompheniramine anticholinergic Dexchlorpheniramine effects/toxicity. Diphenhydramine (oral) Doxylamine Use of diphenhydramine in Hydroxyzine special situations such Promethazine as acute treatment of Triprolidine severe allergic reaction may be appropriate. Antiparkinson agents Not recommended for Avoid Moderate Strong Rudolph 2008 Benztropine (oral) prevention of Trihexyphenidyl extrapyramidal symptoms with antipsychotics; more effective agents available for treatment of Parkinson disease. Antispasmodics Highly anticholinergic, Avoid Moderate Strong Lechevallier- Belladonna alkaloids uncertain except in Michel 2005 Clidinium-chlordiazepoxide effectiveness. short-term Rudolph 2008 Dicyclomine palliative Hyoscyamine care to Propantheline decrease Scopolamine oral secretions. Antithrombotics Dipyridamole, oral short-acting* May -

Antihypertensive Agents Using ALZET Osmotic Pumps
ALZET® Bibliography References on the Administration of Antihypertensive Agents Using ALZET Osmotic Pumps 1. Atenolol Q7652: W. B. Zhao, et al. Stimulation of beta-adrenoceptors up-regulates cardiac expression of galectin-3 and BIM through the Hippo signalling pathway. British Journal of Pharmacology 2019;176(14):2465-2481 Agents: Isoproterenol; propranolol; carvedilol; atenolol; ICI-118551 Vehicle: saline; ascorbic acid, buffered; Route: SC; Species: Mice; Pump: 2001; Duration: 1 day; 2 days; 7 days; ALZET Comments: Dose ((ISO 0.6, 6, 20 mg/kg/d), (Prop 2 mg/kg/d), (Carv 2 mg/kg/d), (AT 2 mg/kg/d), (ICI 1 mg/kg/d)); saline with 0.4 mM ascorbic acid used; Controls were non-transgenic and received mp w/ vehicle; animal info (12-16 weeks, Male, (C57BL/6J, beta2-TG, Mst1-TG, or dnMst1-TG)); ICI-118551 is a beta2-antagonist with the structure (2R,3S)-1-[(7-methyl-2,3-dihydro-1H-inden-4-yl)oxy]-3-(propan-2-ylamino)butan-2-ol; cardiovascular; Minipumps were removed to allow for washout of ISO overnight prior to imaging; Q7241: M. N. Nguyen, et al. Mechanisms responsible for increased circulating levels of galectin-3 in cardiomyopathy and heart failure. Sci Rep 2018;8(1):8213 Agents: Isoproterenol, Atenolol, ICI-118551 Vehicle: Saline, ascorbic acid; Route: SC; Species: Mice; Pump: Not Stated; Duration: 48 Hours; ALZET Comments: Dose: ISO (2, 6 or 30 mg/kg/day; atenolol (2 mg/kg/day), ICI-118551 (1 mg/kg/day); 0.4 mM ascorbic used; animal info (12 14 week-old C57Bl/6 mice); cardiovascular; Q6161: C. -

And Antagonists Between the Pithed Rabbit and Rat J.M
Br. J. Pharmac. (1987), 91, 457-466 Difference in the potency ofa2-adrenoceptor agonists and antagonists between the pithed rabbit and rat J.M. Bulloch, 'J.R. Docherty, 2N.A. Flavahan, J.C. McGrath & C.E. McKean Institute ofPhysiology, University ofGlasgow, Glasgow G12 8QQ, Scotland 1 The subtypes ofa-adrenoceptors which mediate pressor responses to sympathomimetic agonists or to nerve stimulation in pithed rabbits have been classified according to the effects of 'selective' antagonists and a comparison has been made, for the xt2-subtype, with corresponding responses in the rat. 2 In the rabbit the dose-response curve for phenylephrine was shifted to the right in parallel by prazosin (1 mg kg-') and was unaffected by rauwolscine (1 mg kg '). The dose-response curve for noradrenaline was shifted to the right by prazosin (I mg kg -') and was shifted to a smaller extent by rauwolscine (1 mg kg -') or imiloxan (1Omg kg-'). After rauwolscine, prazosin produced a rightward shift larger than when given alone. After prazosin, rauwolscine produced a rightward shift larger than when given alone. 3 The responses to pressor nerve stimulation at low frequencies (< 1 Hz) could be reduced by prazosin, rauwolscine or imiloxan but those at a higher frequency could be reduced only by prazosin. 4 These results indicate that the responses to noradrenaline or to nerve stimulation are mediated by both a,- and a2-adrenoceptors. Low doses or frequencies have a proportionately greater component which is M2 5 Responses to noradrenaline after prazosin (1 mg kg -'), were sufficiently sensitive to rauwolscine to be considered as predominantly a2. -

Current and Experimental Therapeutics for the Treatment of Opioid Addiction
105 CURRENT AND EXPERIMENTAL THERAPEUTICS FOR THE TREATMENT OF OPIOID ADDICTION PAUL J. FUDALA GEORGE E. WOODY Currently, numerous effective pharmacologic and behav- ing treatment have been addicted to heroin or other opioids ioral therapies are available for the treatment of opioid ad- for 2 to 3 years, some for 30 years or more. Thus, treatment diction, and these two types of therapies often are combined usually involves changes in patients’ lifestyles. Although to optimize patient management. Newer therapeutic op- generally ineffective in producing sustained remission unless tions may take various forms. For example, methadone combined with long-term pharmacologic, psychosocial, or maintenance is an established treatment modality, whereas behavioral therapies, detoxification alone continues to be the use of buprenorphine and naloxone in an office-based widely used and studied. It is sometimes the only option setting represents a new variation on that theme. Clonidine available for patients who do not meet United States Food has been used extensively to ameliorate opioid withdrawal and Drug Administration (FDA) criteria for, do not desire, signs, whereas lofexidine is a structural analogue that ap- or do not have access to agonist medications such as metha- pears to have less hypotensive and sedating effects. The done or methadyl acetate (L-␣-acetylmethadol or LAAM). depot dosage form of naltrexone, currently under develop- The detoxification process may include use of opioid ment, may increase compliance with a medication that has agonists (e.g., methadone), partial agonists (e.g., buprenor- been an effective opioid antagonist but that has been un- phine), antagonists (e.g., naloxone, naltrexone), or nonopi- derused secondary to patient nonacceptance. -

Add-On Effect of Bedtime Dosing of the Α1-Adrenergic Receptor
1097 Hypertens Res Vol.30 (2007) No.11 p.1097-1105 Original Article Add-On Effect of Bedtime Dosing of the α1 -Adrenergic Receptor Antagonist Doxazosin on Morning Hypertension and Left Ventricular Hypertrophy in Patients Undergoing Long-Term Amlodipine Monotherapy Toshio IKEDA1), Tomoko GOMI1), Yuko SHIBUYA1), Shingo SHINOZAKI1), Yoshifumi SUZUKI1), and Nami MATSUDA1) High morning blood pressure is related to target organ damage and future cardiovascular events. Chrono- biologic therapies focusing on the early morning period may be an important strategy for antihypertensive therapy. The aim of this study was to clarify the add-on effects of bedtime dosing of the α1 -adrenergic recep- tor antagonist doxazosin on morning blood pressure in patients with essential hypertension who were under long-acting calcium channel blocker amlodipine monotherapy. The add-on effects of doxazosin at the max- imum dose of 6 mg at bedtime on home blood pressure and left ventricular geometry for 1 year were inves- tigated in 49 subjects (37 men and 12 women, aged 57.5±9.1 years) with morning hypertension who had been treated with amlodipine alone for more than 1 year. Doxazosin induced a significant decrease in morn- ing blood pressure (145.6±5.6/91.5±5.4 to 132.4±3.7/83.6±5.6 mmHg, p≤0.001/<0.001) without a change of evening blood pressure (128.9±5.1/79.8±5.1 to 127.7±6.0/78.8±6.2 mmHg, p=0.056/0.051). Left ventricular mass index (LVMI; 124.8±19.8 to 95.6±15.7 g/m2, p<0.001), relative wall thickness (0.457±0.061 to 0.405±0.047, p<0.001) and homeostasis model assessment of the insulin resistance index (HOMA-IR; 2.62±1.43 to 1.33±0.75, p<0.001) were decreased after doxazosin therapy. -

Initial Medication Selection for Treatment of Hypertension in an Open-Panel HMO
J Am Board Fam Pract: first published as 10.3122/jabfm.8.1.1 on 1 January 1995. Downloaded from Initial Medication Selection For Treatment Of Hypertension In An Open-Panel HMO Micky jerome, PharmD, MBA, George C. Xakellis, MD, Greg Angstman, MD, and Wayne Patchin, MBA Background: During the past 25 years recommendations for treating hypertension have evolved from a stepped-care approach to monotherapy or sequential monotherapy as experience has been gained and new antihypertensive agents have been introduced. In an effort to develop a disease management strategy for hypertension, we investigated the prescribing patterns of initial medication therapy for newly treated hypertensive patients. Methods: We examined paid claims data of an open-panel HMO located in the midwest. Charts from 377 patients with newly treated hypertension from a group of 12,242 hypertenSive patients in a health insurance population of 85,066 persons were studied. The type of medication regimen received by patients newly treated for hypertension during an 18-month period was categorized into monotherapy, sequential monotherapy, stepped care, and initial treatment with multiple agents. With monotherapy, the class of medication was also reported. Associations between use of angiotensin-converting enzyme (ACE) inhibitors, calcium channel blockers, or (3-blockers and presence of comorbid conditions were reported. Results: Fifty-five percent of patients received monotherapy, 22 percent received stepped care, and 18 percent received sequential monotherapy. Of those 208 patients receiving monotherapy, 30 percent were prescribed a calcium channel blocker, 22 percent an ACE inhibitor, and 14 percent a f3-blocker. No customization of treatment for comorbid conditions was noted. -

Long Acting, Reversible Veterinary Sedative and Analgesic And
University of Kentucky UKnowledge Veterinary Science Faculty Patents Veterinary Science 7-11-2006 Long Acting, Reversible Veterinary Sedative and Analgesic and Method of Use Thomas Tobin University of Kentucky, [email protected] Right click to open a feedback form in a new tab to let us know how this document benefits oy u. Follow this and additional works at: https://uknowledge.uky.edu/gluck_patents Part of the Veterinary Medicine Commons Recommended Citation Tobin, Thomas, "Long Acting, Reversible Veterinary Sedative and Analgesic and Method of Use" (2006). Veterinary Science Faculty Patents. 14. https://uknowledge.uky.edu/gluck_patents/14 This Patent is brought to you for free and open access by the Veterinary Science at UKnowledge. It has been accepted for inclusion in Veterinary Science Faculty Patents by an authorized administrator of UKnowledge. For more information, please contact [email protected]. US007074834B2 (12) United States Patent (10) Patent N0.: US 7,074,834 B2 Tobin (45) Date of Patent: Jul. 11, 2006 (54) LONG ACTING, REVERSIBLE VETERINARY 4,742,054 A 5/1988 Naftchi SEDATIVE AND ANALGESIC AND METHOD 4,950,648 A 8/1990 Raddatz et a1. OF USE 5,635,204 A * 6/1997 GevirtZ et a1. ............ .. 424/449 5,942,241 A 8/1999 Chasin et a1. (75) Inventor: Thomas Tobin, Lexington, KY (US) 5,958,933 A 9/1999 Naftchi (73) Assignee: University of Kentucky Foundation, OTHER PUBLICATIONS Lexington, KY (US) MEDLINE AN 20000025586, Veveris et al, Brit. J. Pharmacol, 128 (5), 1089-97, Nov. 1999, abstract.* ( * ) Notice: Subject to any disclaimer, the term of this Veterinary Pharmacology and Therapeutics, Adams, pp. -

Drugs Commonly Used to Treat High Blood Pressure
Drugs Commonly Used to Treat High Blood Pressure High blood pressure also called hypertension, is when your heart is working too hard to push blood though the body and causes pressure against the walls of your arteries. When not treated properly, hypertension can increase your risk for a heart attack, stroke, kidney failure and eye damage. If taken exactly as prescribed by a doctor, medications are an effective way to keep your blood pressure at a safe level and can help you avoid serious and costly health issues. The chart below lists some of the most commonly prescribed medications used to treat high blood pressure. This chart only provides a sample list of drug options (not all drugs available) and may change. Generic Drugs Brand-name Drugs acebutolol hydrochlorothiazide timolol Aceon acetazolamide hydroflumethiazide torsemide Atacand/Atacand HCT* amiloride/amiloride-HCTZ indapamide trandolapril Avalide amlodipine isradipine triamterene/triamterene-HCTZ Avapro amlodipine-benazepril labetalol/labetalol HCL-HCTZ verapamil/verapamil ER Azor atenolol lisinopril/lisinopril-HCTZ Benicar/Benicar HCT atenolol-chlorthalidone methazolamide Bystolic benazepril/benazepril-HCTZ methylclothiazide Cardene SR bendroflumethiazide methyldopa Cardizem LA betaxolol metolazone Catapres-TTS 1/2/3 bisoprolol/bisoprolol-HCTZ metoprolol-HCTZ Coreg CR bumetanide metoprolol/metoprolol ER Covera HS captopril/captopril-HCTZ minoxidil Cozaar carvedilol moexipril/moexipril-HCTZ Diovan/Diovan HCT* chlorothiazide nadolol/nadolol bendroflumethiazide Dynacirc/Dynacirc -

1988 Joint National Committee Guidelines for Managing Hypertension: How Are They Different?
CONTRIBUTION • 1988 Joint National Committee guidelines for managing hypertension: how are they different? RAY W. GIFFORD, JR., MD • The new Joint National Committee guidelines on managing hypertension retain the stepped care con- cept but add flexibility. The 1988 report recommends that, in addition to diuretics and beta blockers, cal- cium-channel blockers and ACE inhibitors be considered for initial monotherapy. Compared to previous JNC reports, lower starting doses of most antihypertensive drugs, especially diuretics, are recommended. For the first time, the guidelines discuss the cost of antihypertensive therapy. Specific nonpharmacologic therapy and its role in relation to drug therapy are discussed in greater detail than previous reports. • INDEX TERM: HYPERTENSION • CLEVECLIN] MED 1989; 56:41-47 INCE its inception in 1973, the National High The 1988 report (JNC IV),5 which was published in Blood Pressure Education Program of the May (Hypertension Month), introduced some new is- National Heart, Lung, and Blood Institute, sues and updated some others. Key differences between Sthrough its Coordinating Committee, has pub- this and the previous report are outlined here. lished state-of-the-art guidelines on detection, evalua- tion, and treatment of high blood pressure. These con- STEPPED CARE sensus documents are written by a committee of authorities appointed by the director of the National The stepped care approach to managing hypertension Heart, Lung, and Blood Institute. The first report, which was introduced in the Data Base for Effective Antihy- was titled the Data Base for Effective Antihypertensive pertensive Therapy,1 in 1973, when the only available Therapy, was published only as a document of the De- choices among antihypertensive drugs were ganglion partment of Health, Education and Welfare.1 Sub- blocking agents, guanethidine, hydralazine, methyl- sequent communications have been issued as reports of dopa, reserpine, and thiazide diuretics. -

Combination Therapy
Combination Antihypertensive Therapy: When to use it Diabetes George L. Bakris, MD, F.A.S.N., F.A.S.H. Professor of Medicine Director, ASH Comprehensive Hypertension Center The University of Chicago Medicine Development of Antihypertensive Therapies ? More Effective but As effective and As effective and even effective for poorly tolerated better tolerated better tolerated SBP 1940s 1950 1957 1960s 1970s 1980s 1990s 2001- 2009 ARBs Direct Direct ACE inhibitors Renin vasodilators inhibitors α-blockers Peripheral Thiazides ETa sympatholytics diuretics Blockers Central ααα 2 Calcium Ganglion agonists blockers antagonists- VPIs Calcium DHPs Others Veratrum antagonists- alkaloids non DHPs βββ-blockers Evolution of Fixed Dose Combination Antihypertensive Therapies 1960s 1970s 1980s 1990s 2000- present Combination CCBs+ ARBs Diuretics RAS Blockers ARB + Aldactazide, with CCBs chlorthalidone Dyazide, Maxzide, DRIs +ARBs Guanabenz SerApAs RAS Blockers (Lotrel) DRIs+ CCBs (reserpine, with diuretics hydralazine, Beta blocker +diuretics TRIPLE Combos HCTZ) (CCB+RAS Blocker + diuretic) Rationale for Fixed-Dose Combination Therapy: Background • Traditional antihypertensive therapy yields goal BP in <60% of treated hypertensive patients1-3 • Switching from one monotherapy to another is effective in only about 50% of patients1 • Most patients will require at least two drugs to attain goal BP (<140/90 mm Hg, or <130/80 mm Hg for patients with diabetes or chronic renal disease)4-6 BP = blood pressure 1. Materson BJ et al. J Hum Hypertens. 1995;9(10):791-796. 2. Messerli FH. J Hum Hypertens. 1992;6 Suppl. 2:S19-S21. 3. Ram CV. J Clin Hypertens (Greenwich). 2004;6(10):569-577. 4. Chobanian AV, et al. JAMA. -

Comparison of Agonistic and Antagonistic Actions of Guanabenz and Guanfacin on A, and A2-Adrenoceptors in Isolated Smooth Muscles
Comparison of Agonistic and Antagonistic Actions of Guanabenz and Guanfacin on a, and a2-Adrenoceptors in Isolated Smooth Muscles Kouichi TAKEUCHI, Miki KOGURE and Takao HASHIMOTO Departmentof Pharmacology,Meiji College of Pharmacy, 1-35-23, Nozawa,Setagaya-ku, Tokyo 154, Japan Accepted November22, 1986 Abstract-The effects of guanabenz, guanfacine and clonidine on a-adrenoceptors were investigated in isolated rat vas deferens and rabbit aortic strip. All 3 drugs at low concentrations (10-9-10-8 M) caused inhibition of twitch responses of the rat vas deferens induced by nerve stimulation. These effects were competitively antagonized by yohimbine. Guanfacine and clonidine at relatively high concen trations (10-°-10-4 M) produced contractions of the rat vas deferens which were antagonized by prazosin. These contractile responses were not much affected by denervation. Prazosin-sensitive contractions by guanfacine and clonidine were also observed in the rabbit aortic strip, which were not affected by reserpine pre treatment. In both tissues, the intrinsic activity of guanfacine was almost identical to that of norepinephrine, whereas that of clonidine was less than one half. Guanabenz and clonidine showed a competitive antagonistic effect against nor epinephrine and phenylephrine in both the rat vas deferens and rabbit aorta, the antagonisms being similar in potency. The results indicate that all 3 drugs are potent agonists on the presynaptic a2-adrenoceptor. In contrast, on the postsynaptic ai -adrenoceptor, guanfacine and guanabenz showed only agonistic and antagonistic actions, respectively, whereas clonidine exhibited partial agonistic characteristics. Guanabenz and guanfacine are newly adrenoceptors in peripheral tissues, the introduced antihypertensive drugs possessing effects of guanabenz, guanfacine and a guanidine residue in their structural formula clonidine were comparatively investigated in (1-5). -

Guanabenz Elisa Kit Instructions Product #109219 & 109216 Forensic Use Only
Neogen Corporation 944 Nandino Blvd., Lexington KY 40511 USA 800/477-8201 USA/Canada | 859/254-1221 Fax: 859/255-5532 | E-mail: [email protected] | Web: www.neogen.com/Toxicology GUANABENZ ELISA KIT INSTRUCTIONS PRODUCT #109219 & 109216 FORENSIC USE ONLY INTENDED USE: For the determination of trace quantities of Guanabenz and/or other metabolites in human urine, blood, oral fluid. DESCRIPTION Neogen Corporation’s Guanabenz ELISA (Enzyme-Linked ImmunoSorbent Assay) test kit is a qualitative one-step kit designed for use as a screening device for the detection of drugs and/or their metabolites. The kit was designed for screening purposes and is intended for forensic use only. It is recommended that all suspect samples be confirmed by a quantitative method such as gas chromatography/mass spectrometry (GC/MS). ASSAY PRINCIPLES Neogen Corporation’s test kit operates on the basis of competition between the drug or its metabolite in the sample and the drug-enzyme conjugate for a limited number of antibody binding sites. First, the sample or control is added to the microplate. Next, the diluted drug-enzyme conjugate is added and the mixture is incubated at room temperature. During this incubation, the drug in the sample or the drug-enzyme conjugate binds to antibody immobilized in the microplate wells. After incubation, the plate is washed 3 times to remove any unbound sample or drug-enzyme conjugate. The presence of bound drug-enzyme conjugate is recognized by the addition of K-Blue® Substrate (TMB). After a 30 minute substrate incubation, the reaction is halted with the addition of Red Stop Solution.