Coeliac Disease with Histological Features of Peptic Duodenitis: Value
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Dyspepsia (Indigestion)
Indigestion (dydpepsia). Indigestion information - Patient | Patient Page 1 of 5 View this article online at https://patient.info/health/dyspepsia-indigestion Dyspepsia (Indigestion) Dyspepsia (indigestion) is a term which describes pain and sometimes other symptoms which come from your upper gut (the stomach, oesophagus or duodenum). There are various causes (described below). Treatment depends on the likely cause. Understanding digestion Food passes down the gullet (oesophagus) into the stomach. The stomach makes acid which is not essential but helps to digest food. Food then passes gradually into the first part of the small intestine (the duodenum). In the duodenum and the rest of the small intestine, food mixes with chemicals called enzymes. The enzymes come from the pancreas and from cells lining the intestine. The enzymes break down (digest) the food. Digested food is then absorbed into the body from the small intestine. What is dyspepsia? Dyspepsia is a term which includes a group of symptoms that come from a problem in your upper gut. The gut (gastrointestinal tract) is the tube that starts at the mouth and ends at the anus. The upper gut includes the oesophagus, stomach and duodenum. Various conditions cause dyspepsia. The main symptom is usually pain or discomfort in the upper tummy (abdomen). In addition, other symptoms that may develop include: • Bloating. • Belching. • Quickly feeling full after eating. • Feeling sick (nausea). • Being sick (vomiting). Symptoms are often related to eating. Doctors used to include heartburn (a burning sensation felt in the lower chest area) and bitter-tasting liquid coming up into the back of the throat (sometimes called 'waterbrash') as symptoms of dyspepsia. -

Abnormal Small Bowel Permeability and Duodenitis in Recurrent Abdominal Pain
Archives ofDisease in Childhood 1990; 65: 1311-1314 1311 Abnormal small bowel permeability and duodenitis Arch Dis Child: first published as 10.1136/adc.65.12.1311 on 1 December 1990. Downloaded from in recurrent abdominal pain S B van der Meer, P P Forget, J W Arends Abstract assess the value of 5"Cr-EDTA permeability Thirty nine children with recurrent abdominal tests of intestinal inflammation. As the absorp- pain aged between 5.5 and 12 years, underwent tion of 51Cr-EDTA takes place predominantly endoscopic duodenal biopsy to find out if in the small bowel,'2 duodenal biopsies from 39 there were any duodenal inflammatory patients with recurrent abdominal pain were changes, and if there was a relationship examined for the presence of inflammatory between duodenal inflammation and intestinal changes. permeability to 5tCr-EDTA. Duodenal in- flammation was graded by the duodenitis scale of Whitehead et al (grade 0, 1, 2, and 3). Patients and methods In 13 out of 39 patients (33%) definite signs of During a prospective study 106 children with inflammation were found (grade 2 and 3). recurrent abdominal pain were investigated Intestinal permeability to 5tCr-EDTA in according to a standard protocol. Patients were patients with duodenitis (grade 1, 2, and 3) diagnosed as having recurrent abdominal pain if was significantly higher (4-42 (1-73)%) than in they were aged between 5 5 and 12 years; had patients with normal (grade 0) duodenal had recurrent abdominal pain for at least six biopsy appearances (3.3 (0-9)%). A significant months; had had attacks of pain varying in association was found between duodenal in- severity, duration, and frequency; and if their flammation and abnormal intestinal per- attacks were sometimes accompanied by pale- meability. -

~L.Il~I~1 ORGANISATION MONDIALE ORGANIZATION DE LA SANTE ~,JII /'1 'IJ,Rj ~,JII-:.CJI REGIONAL OFFICE for THE
WORLD HEALTH ~l.Il~I~1 ORGANISATION MONDIALE ORGANIZATION DE LA SANTE ~,JII /'1 'IJ,rJ ~,JII-:.CJI REGIONAL OFFICE FOR THE . BUREAU REGIONAL DE LA EASTERN MEDITBRRANEAN MEDITERRANEE ORIENTALE REGIONAL CCMVIITrEE FOR THE EM/RC14/Tech.Disc./3 EASTERN MEDITERRANEAN 25 August 1964 Fourteenth Session Agenda item 12 TECHNICAL DISCUSSIONS INFANTILE DIARRHOEA CONTRIBUTIONS FROM VARIOUS EXPERTS IN THE EASTERN MEDITERRANEAN REGION (In original language o~ presentation) EM/RC14/Tech.Disc./3 TABLE OF CONTENTS INFANTILE DIARRHOEA IN EGYPl', UAR, by A. Shafik Abbasy, M.D. 1 I Assessment of the Magnitude of Diarrhoeal Disease 1 II Study of Factors Influencing Morbidity and Mortality 3 III Etiological Studies 7 IV Conclusion 13 V Recommendations 13 References 17 INFANTILE DIARRHOEA IN EGYPl', UAR, by Dr. Girgis Abd-EI-Messih 21 I Introduction 21 II Statistical Data in Egypt 22 III Socio-Economic and Environmental Sanitary Factors in Relation to Infantile Diarrhoea 23 IV Comparison between Rates in Egypt and in some other Countries 24 V The Problem of Infantile Diarrhoea in Egypt 25 References 27 Tables 1 to 8 28 MANAGEMENT OF THE DIARRHOEAL DISEASES IN IRAN, by Dr. Hassan Ahari 35 References 42 INFAl·lrILE DIARRHOEA - Summary of Routine Care and Conclusions 43 observed at the Paediatric Ward, Pahlavi University Hospital, Teheran, by Mohammad Gharib, M.D. THE PROBLEM OF INFANTILE DIARRHOEA IN PAKISTAN, by Dr. Hamid Ali Khan 47 I Case History 48 II Degree of Dehydration 49 III Laboratory Investigation 50 IV Principles of Treatment followed 51 V Results and Analysis 53 VI Treatment and Results 56 VII Further Plans for the Study 57 L 'ETAT ACTUEL DES DIARRHEES INFANTlIES EN IRAN, par le Dr. -

Clinical Biliary Tract and Pancreatic Disease
Clinical Upper Gastrointestinal Disorders in Urgent Care, Part 2: Biliary Tract and Pancreatic Disease Urgent message: Upper abdominal pain is a common presentation in urgent care practice. Narrowing the differential diagnosis is sometimes difficult. Understanding the pathophysiology of each disease is the key to making the correct diagnosis and providing the proper treatment. TRACEY Q. DAVIDOFF, MD art 1 of this series focused on disorders of the stom- Pach—gastritis and peptic ulcer disease—on the left side of the upper abdomen. This article focuses on the right side and center of the upper abdomen: biliary tract dis- ease and pancreatitis (Figure 1). Because these diseases are regularly encountered in the urgent care center, the urgent care provider must have a thorough understand- ing of them. Biliary Tract Disease The gallbladder’s main function is to concentrate bile by the absorption of water and sodium. Fasting retains and concentrates bile, and it is secreted into the duodenum by eating. Impaired gallbladder contraction is seen in pregnancy, obesity, rapid weight loss, diabetes mellitus, and patients receiving total parenteral nutrition (TPN). About 10% to 15% of residents of developed nations will form gallstones in their lifetime.1 In the United States, approximately 6% of men and 9% of women 2 have gallstones. Stones form when there is an imbal- ©Phototake.com ance in the chemical constituents of bile, resulting in precipitation of one or more of the components. It is unclear why this occurs in some patients and not others, Tracey Q. Davidoff, MD, is an urgent care physician at Accelcare Medical Urgent Care in Rochester, New York, is on the Board of Directors of the although risk factors do exist. -

ICD 9-10 Common Codes Gastrocenterology 1115
TM ICD-9-CM and ICD-10-CM Common Codes for Gastroenterology ICD-9 ICD-10 ICD-9 ICD-10 Diagnoses Diagnoses Code Code Code Code Infectious gastroenteritis and colitis, Ulcerative (chronic) pancolitis without 009.1 A09 556.5 K51.00 complications H. Pylori as the cause of disease Other ulcerative colitis without 041.86 B96.81 556.8 K51.80 necessary complications Chronic viral hepatitis b without Vascular disorder of intestine, 070.32 B18.1 557.9 K55.9 delta-agent 070.54 Chronic viral hepatitis c B18.2 558.9 K52.89 Malignant neoplasm of colon, gastroenteritis and colitis 153.9 C18.9 560.31 Gallstone ileus K56.3 211.3 Polyp of colon K63.5 Diverticulosis large intestine w/o 562.1 K57.30 Hemangioma of intra-abdominal perforation or abscess 228.04 D18.03 structures Diverticulitis large intestine w/o 562.11 K57.32 Neoplasm of uncertain behavior of perforation or abscess 235.3 D37.6 liver and biliary passages 564.00 K59.00 278.00 E66.9 Irritable bowel syndrome without 564.1 K58.9 280.9 D50.9 diarrhea 285.9 D64.9 564.5 Functional diarrhea K59.1 455.6 K64.9 565 K60.2 455.8 Other hemorrhoids K64.8 569.3 Hemorrhage of anus and rectum K62.5 530.11 K21.0 569.42 K62.89 without esophagitis rectum 530.3 Esophageal obstruction K22.2 569.89 Enteroptosis K63.4 K63.89 530.81 K21.9 w/o esophagitis 571 Alcoholic fatty liver K70.0 530.85 Barrett's esophagus without dysplasia K22.70 571.1 Alcoholic hepatitis without ascites K70.10 Acute gastric ulcer without Chronic active hepatitis, not 531.3 K25.3 571.49 K73.2 hemorrhage or perforation Other chronic hepatitis, -
Clinical Remission and Normalization of Laboratory Studies in a Patient
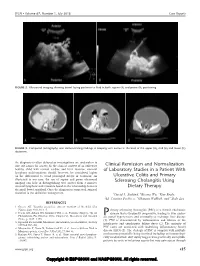
JPGN Volume 67, Number 1, July 2018 Case Reports FIGURE 2. Ultrasound imaging showing bowel laying posterior to fluid in both supine (A) and prone (B) positioning. FIGURE 3. Computed tomography scan demonstrating findings in keeping with ascites at the level of the upper (A), mid (B) and lower (C) abdomen. the diagnosis is often delayed as investigations are undertaken to rule out causes for ascites. In the clinical context of an otherwise Clinical Remission and Normalization healthy child with normal cardiac and liver function, omental of Laboratory Studies in a Patient With lymphatic malformations should, however, be considered higher on the differential to avoid prolonged delays in treatment. As Ulcerative Colitis and Primary illustrated in our case, the use of supine and prone ultrasound imaging can help in distinguishing true ascites from a massive Sclerosing Cholangitis Using omental lymphatic malformation based on the relationship between Dietary Therapy the small bowel and fluid. Once the diagnosis is suspected, surgical resection is the definitive management. ÃDavid L. Suskind, yBicong Wu, ÃKim Braly, zM. Cristina Pacheco, ÃGhassan Wahbeh, and ÃDale Lee REFERENCES 1. Greene AK. Vascular anomalies: current overview of the field. Clin Plastic Surg 2011;38:1–5. rimary sclerosing cholangitis (PSC) is a chronic cholestatic 2. Coran AG, Adzick NS, Krummel TM, et al. Pediatric Surgery. 7th ed. disease that is frequently progressive, leading to liver cirrho- Philadelphia, PA: Elsevier; 2012. Chapter 91, Mesenteric and Omental sis,P portal hypertension, and eventually to end-stage liver disease Cysts, p. 1165–1170. (1). PSC is characterized by inflammation and fibrosis of the 3. -

Efficacy of Duodenal Bulb Biopsy for Diagnosis of Celiac Disease: a Systematic Review and Meta-Analysis
Original article Efficacy of duodenal bulb biopsy for diagnosis of celiac disease: a systematic review and meta-analysis Authors Thomas R. McCarty1,CoreyR.O’Brien1, Anas Gremida2, Christina Ling2,TarunRustagi2 Institutions nalysis to evaluate the diagnostic utility of endoscopic duo- 1 Department of Internal Medicine, Yale University School denal bulb biopsy for celiac disease. of Medicine, New Haven, Connecticut, United States Patients and methods Searches of PubMed, EMBASE, 2 Division of Gastroenterology and Hepatology, University Web of Science, and Cochrane Library databases were per- of New Mexico, Albuquerque, New Mexico, United formed from 2000 through December 2017. Review of States titles/abstracts, full review of potentially relevant studies, and data abstraction was performed. Measured outcomes submitted 7.5.2018 of adult and pediatric patients included location of biopsy, accepted after revision 23.7.2018 mean number of biopsies performed, and diagnosis of ce- liac disease as defined by the modified Marsh-Oberhuber Bibliography classification. DOI https://doi.org/10.1055/a-0732-5060 | Results A total of 17 studies (n=4050) were included. Sev- Endoscopy International Open 2018; 06: E1369–E1378 en studies evaluated adults and 11 studies assessed pedia- © Georg Thieme Verlag KG Stuttgart · New York tric populations. Mean age of adults and pediatric patients ISSN 2364-3722 was46.70±2.69and6.33±1.26years,respectively.Over- all, sampling from the duodenal bulb demonstrated a 5% Corresponding author (95% CI 3– 9; P <0.001) increase in the diagnostic yield of Tarun Rustagi, MD, Division of Gastroenterology and celiac disease. When stratified by pediatric and adult popu- Hepatology, University of New Mexico, MSC10 5550, 1 lations, duodenal bulb biopsy demonstrated a 4% (95% CI: University of New Mexico, Albuquerque NM 87131 1to9;P < 0.001) and 8% (95% CI: 6 to 10; P <0.001) in- Fax: +1-505-272-9751 crease in the diagnostic yield of celiac disease. -

European Consensus on the Histopathology of Inflammatory Bowel Disease☆ F
Journal of Crohn's and Colitis (2013) 7, 827–851 Available online at www.sciencedirect.com ScienceDirect CONSENSUS/GUIDELINES European consensus on the histopathology of inflammatory bowel disease☆ F. Magro a,⁎,1, C. Langner b,1, A. Driessen c, A. Ensari d, K. Geboes e, G.J. Mantzaris f, V. Villanacci g, G. Becheanu h, P. Borralho Nunes i, G. Cathomas j, W. Fries k, A. Jouret-Mourin l, C. Mescoli m, G. de Petris n, C.A. Rubio o, N.A. Shepherd p, M. Vieth q, R. Eliakim r on behalf of the European Society of Pathology (ESP) and the European Crohn's and Colitis Organisation (ECCO)2 a Department of Pharmacology & Therapeutics, Institute for Molecular and Cell Biology, Faculty of Medicine University of Porto, Department of Gastroenterology, Hospital de Sao Joao, Porto, Portugal b Institute of Pathology, Medical University of Graz, Austria c Department of Pathology, University Hospital Antwerp, Belgium d Department of Pathology, Ankara University Medical School, Turkey e Department of Pathology, UZ Leuven, Belgium f 1st Department of Gastroenterology, Evangelismos Hospital, Athens, Greece g Pathology, Spedali Civili, Brescia, Italy h Carol Davila University of Medicine and Pharmacy, Department of Pathology, Bucharest, Romania i Instituto de Anatomia Patologica, Escola Superior de Tecnologia da Saúde de Lisboa & Faculdade de Medicina da Universidade de Lisboa, Portugal j Institute for Pathology, Kanonsspital Baselland, Liestal, Switzerland k Dept. of Clinical and Experimental Medicine, Clinical Unit for Chronic Bowel Disorders, University of -

Often Necessarily Exposed to the Causes of Disease, and Frequently Unwilling
Art. IX. Remarks on the Dysentery and Hepatitis of India. By E. A. Pabkes, m.b., late Assistant Surgeon H. M. 84th Regiment.?London, 1846. 8vo, pp. 271. Of the diseases incident to Europeans in tropical climates, there is perhaps none of more importance than dysentery, whether we consider the amount of mortality arising from it, or the permanently impaired health produced by alteration of structure in those who have laboured under it. In the army this is even more marked than in civil life, for the soldier, often necessarily exposed to the causes of disease, and frequently unwilling to submit to the necessary restraint when convalescent, suffers repeated relapses until the disease terminates either in death or in organic altera- tions of such a character as to render him permanently unfit for military service. Dysentery has consequently attracted much of the attention of the medical officers of the army, and many excellent works have been written upon it. There are still, however, many disputed points in regard to its pathology and treatment, especially in the frequent case of complica- tion with other diseases; and much patient investigation and accurate observation will be requisite ere these can be settled on a satisfactory basis. The volume before us is a valuable contribution to this end, and is most creditable to the industry and talents of the author. It contains the result of his observations while serving in the 84th regiment in India, and professes less to be a systematic work on the diseases treated of, than an endeavour to elucidate various points connected with them about which differences of opinion prevail, and to draw attention to the composite nature of all chronic abdominal diseases. -

Crohn's Disease of the Esophagus, Duodenum, and Stomach
Published online: 2019-06-17 231 Crohn’s Disease of the Esophagus, Duodenum, and Stomach David M. Schwartzberg, MD1 Stephen Brandstetter, MD1 Alexis L. Grucela, MD, FACS, FASCRS2 1 Department of Colorectal Surgery, Digestive Disease Institute, Address for correspondence Alexis L. Grucela, MD, FACS, FASCRS, Cleveland Clinic Foundation, Cleveland, Ohio Division of Colon and Rectal Surgery, New York University Langone 2 Division of Colon and Rectal Surgery, New York University Langone Medical Center, 530 1st Avenue, Suite 7V, New York, NY 10016 Medical Center, New York, New York (e-mail: [email protected]). Clin Colon Rectal Surg 2019;32:231–242. Abstract Upper gastrointestinal Crohn’s is an under-reported, under-recognized phenotype of Crohn’s disease. Routine screening in the pediatric population has shown a higher prevalence compared with adults; however, most adult patients remain asymptomatic with respect to upper gastrointestinal Crohn’s disease. For the patients who are symptomatic, medical treatment is the first line of management, except for cases of Keywords obstruction, perforation, or bleeding. Though most patients respond to medical ► Upper therapy, mainly steroids, with the addition of immunomodulators and more recently Gastrointestinal biologics agents, surgical intervention is usually required only for obstructing gastro- Crohn’s Disease duodenal disease secondary to strictures. Strictureplasty and bypass are safe opera- ► gastroduodenal tions with comparable morbidity, although bypass has higher rates of dumping Crohn’s disease syndrome and marginal ulceration in the long term. Rare cases of gastroduodenal ► esophageal Crohn’s fistulous disease from active distal disease may involve the stomach or duodenum, and disease esophageal Crohn’s disease can fistulize to surrounding structures in the mediastinum ► strictureplasty which may require the highly morbid esophagectomy. -

Inflammatory Bowel Disease Presenting with Concurrent COVID-19 Multisystem Inflammatory Syndrome Katherine F
Prepublication Release Inflammatory Bowel Disease Presenting With Concurrent COVID-19 Multisystem Inflammatory Syndrome Katherine F. Sweeny, MD, Yanjia J. Zhang, MD, PhD, Bonnie Crume, MD, Colin A. Martz, MD, PhD, Melissa M. Blessing, DO, Stacy A. Kahn, MD DOI: 10.1542/peds.2020-027763 Journal: Pediatrics Article Type: Case Report Citation: Sweeny KF, Zhang YJ, Crume B, Martz CA, Blessing MM, Kahn SA. Inflammatory bowel disease presenting with concurrent COVID-19 multisystem inflammatory syndrome. Pediatrics. 2021; doi: 10.1542/peds.2020-027763 This is a prepublication version of an article that has undergone peer review and been accepted for publication but is not the final version of record. This paper may be cited using the DOI and date of access. This paper may contain information that has errors in facts, figures, and statements, and will be corrected in the final published version. The journal is providing an early version of this article to expedite access to this information. The American Academy of Pediatrics, the editors, and authors are not responsible for inaccurate information and data described in this version. Downloaded from©202 www.aappublications.org/news1 American Academy by of guest Pediatrics on September 25, 2021 Prepublication Release Inflammatory Bowel Disease Presenting With Concurrent COVID-19 Multisystem Inflammatory Syndrome Katherine F. Sweeny, MD1*, Yanjia J. Zhang, MD, PhD1*, Bonnie Crume, MD2, Colin A. Martz, MD, PhD2, Melissa M. Blessing, DO3, Stacy A. Kahn, MD1 *Contributed equally as co-first authors. Affiliations: 1. Division of Gastroenterology, Hepatology and Nutrition, 2. Department of Medicine, 3. Department of Pathology, Boston Children’s Hospital, Boston, MA 02115, USA Address Correspondence to: Stacy A Kahn, M.D., Inflammatory Bowel Disease Center, Division of Gastroenterology, Hepatology and Nutrition, Boston Children’s Hospital, 300 Longwood Ave, Boston, MA 02115 Conflict of Interests: The authors have no conflicts of interest relevant to this article to disclose. -

Concomitant Herpes Simplex Virus Colitis and Hepatitis in a Man with Ulcerative Colitis Case Report and Review of the Literature Varun K
Concomitant herpes simplex virus colitis and hepatitis in a man with ulcerative colitis Case report and review of the literature Varun K. Phadke, Emory University Rachel Friedman-Moraco, Emory University Brian Quigley, Emory University Alton Farris III, Emory University John Norvell, Emory University Journal Title: Medicine Volume: Volume 95, Number 42 Publisher: Lippincott, Williams & Wilkins: Medicine | 2016-10-01, Pages e5082-e5082 Type of Work: Article | Final Publisher PDF Publisher DOI: 10.1097/MD.0000000000005082 Permanent URL: https://pid.emory.edu/ark:/25593/rtg24 Final published version: http://dx.doi.org/10.1097/MD.0000000000005082 Copyright information: © 2016 the Author(s). Published by Wolters Kluwer Health, Inc. All rights reserved. This is an Open Access work distributed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License (http://creativecommons.org/licenses/by-nc-nd/4.0/). Accessed October 1, 2021 4:08 PM EDT ® Clinical Case Report Medicine OPEN Concomitant herpes simplex virus colitis and hepatitis in a man with ulcerative colitis Case report and review of the literature ∗ Varun K. Phadke, MDa, , Rachel J. Friedman-Moraco, MDa, Brian C. Quigley, MDb, Alton B. Farris, MDb, J. P. Norvell, MDc,d Abstract Background: Herpesvirus infections often complicate the clinical course of patients with inflammatory bowel disease; however, invasive disease due to herpes simplex virus is distinctly uncommon. Methods: We present a case of herpes simplex virus colitis and hepatitis, review all the previously published cases of herpes simplex virus colitis, and discuss common clinical features and outcomes. We also discuss the epidemiology, clinical manifestations, diagnosis, and management of herpes simplex virus infections, focusing specifically on patients with inflammatory bowel disease.