Gastritis in Patients with Coeliac Disease
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Dyspepsia (Indigestion)
Indigestion (dydpepsia). Indigestion information - Patient | Patient Page 1 of 5 View this article online at https://patient.info/health/dyspepsia-indigestion Dyspepsia (Indigestion) Dyspepsia (indigestion) is a term which describes pain and sometimes other symptoms which come from your upper gut (the stomach, oesophagus or duodenum). There are various causes (described below). Treatment depends on the likely cause. Understanding digestion Food passes down the gullet (oesophagus) into the stomach. The stomach makes acid which is not essential but helps to digest food. Food then passes gradually into the first part of the small intestine (the duodenum). In the duodenum and the rest of the small intestine, food mixes with chemicals called enzymes. The enzymes come from the pancreas and from cells lining the intestine. The enzymes break down (digest) the food. Digested food is then absorbed into the body from the small intestine. What is dyspepsia? Dyspepsia is a term which includes a group of symptoms that come from a problem in your upper gut. The gut (gastrointestinal tract) is the tube that starts at the mouth and ends at the anus. The upper gut includes the oesophagus, stomach and duodenum. Various conditions cause dyspepsia. The main symptom is usually pain or discomfort in the upper tummy (abdomen). In addition, other symptoms that may develop include: • Bloating. • Belching. • Quickly feeling full after eating. • Feeling sick (nausea). • Being sick (vomiting). Symptoms are often related to eating. Doctors used to include heartburn (a burning sensation felt in the lower chest area) and bitter-tasting liquid coming up into the back of the throat (sometimes called 'waterbrash') as symptoms of dyspepsia. -

Abdominal Pain - Gastroesophageal Reflux Disease
ACS/ASE Medical Student Core Curriculum Abdominal Pain - Gastroesophageal Reflux Disease ABDOMINAL PAIN - GASTROESOPHAGEAL REFLUX DISEASE Epidemiology and Pathophysiology Gastroesophageal reflux disease (GERD) is one of the most commonly encountered benign foregut disorders. Approximately 20-40% of adults in the United States experience chronic GERD symptoms, and these rates are rising rapidly. GERD is the most common gastrointestinal-related disorder that is managed in outpatient primary care clinics. GERD is defined as a condition which develops when stomach contents reflux into the esophagus causing bothersome symptoms and/or complications. Mechanical failure of the antireflux mechanism is considered the cause of GERD. Mechanical failure can be secondary to functional defects of the lower esophageal sphincter or anatomic defects that result from a hiatal or paraesophageal hernia. These defects can include widening of the diaphragmatic hiatus, disturbance of the angle of His, loss of the gastroesophageal flap valve, displacement of lower esophageal sphincter into the chest, and/or failure of the phrenoesophageal membrane. Symptoms, however, can be accentuated by a variety of factors including dietary habits, eating behaviors, obesity, pregnancy, medications, delayed gastric emptying, altered esophageal mucosal resistance, and/or impaired esophageal clearance. Signs and Symptoms Typical GERD symptoms include heartburn, regurgitation, dysphagia, excessive eructation, and epigastric pain. Patients can also present with extra-esophageal symptoms including cough, hoarse voice, sore throat, and/or globus. GERD can present with a wide spectrum of disease severity ranging from mild, intermittent symptoms to severe, daily symptoms with associated esophageal and/or airway damage. For example, severe GERD can contribute to shortness of breath, worsening asthma, and/or recurrent aspiration pneumonia. -

Abnormal Small Bowel Permeability and Duodenitis in Recurrent Abdominal Pain
Archives ofDisease in Childhood 1990; 65: 1311-1314 1311 Abnormal small bowel permeability and duodenitis Arch Dis Child: first published as 10.1136/adc.65.12.1311 on 1 December 1990. Downloaded from in recurrent abdominal pain S B van der Meer, P P Forget, J W Arends Abstract assess the value of 5"Cr-EDTA permeability Thirty nine children with recurrent abdominal tests of intestinal inflammation. As the absorp- pain aged between 5.5 and 12 years, underwent tion of 51Cr-EDTA takes place predominantly endoscopic duodenal biopsy to find out if in the small bowel,'2 duodenal biopsies from 39 there were any duodenal inflammatory patients with recurrent abdominal pain were changes, and if there was a relationship examined for the presence of inflammatory between duodenal inflammation and intestinal changes. permeability to 5tCr-EDTA. Duodenal in- flammation was graded by the duodenitis scale of Whitehead et al (grade 0, 1, 2, and 3). Patients and methods In 13 out of 39 patients (33%) definite signs of During a prospective study 106 children with inflammation were found (grade 2 and 3). recurrent abdominal pain were investigated Intestinal permeability to 5tCr-EDTA in according to a standard protocol. Patients were patients with duodenitis (grade 1, 2, and 3) diagnosed as having recurrent abdominal pain if was significantly higher (4-42 (1-73)%) than in they were aged between 5 5 and 12 years; had patients with normal (grade 0) duodenal had recurrent abdominal pain for at least six biopsy appearances (3.3 (0-9)%). A significant months; had had attacks of pain varying in association was found between duodenal in- severity, duration, and frequency; and if their flammation and abnormal intestinal per- attacks were sometimes accompanied by pale- meability. -

~L.Il~I~1 ORGANISATION MONDIALE ORGANIZATION DE LA SANTE ~,JII /'1 'IJ,Rj ~,JII-:.CJI REGIONAL OFFICE for THE
WORLD HEALTH ~l.Il~I~1 ORGANISATION MONDIALE ORGANIZATION DE LA SANTE ~,JII /'1 'IJ,rJ ~,JII-:.CJI REGIONAL OFFICE FOR THE . BUREAU REGIONAL DE LA EASTERN MEDITBRRANEAN MEDITERRANEE ORIENTALE REGIONAL CCMVIITrEE FOR THE EM/RC14/Tech.Disc./3 EASTERN MEDITERRANEAN 25 August 1964 Fourteenth Session Agenda item 12 TECHNICAL DISCUSSIONS INFANTILE DIARRHOEA CONTRIBUTIONS FROM VARIOUS EXPERTS IN THE EASTERN MEDITERRANEAN REGION (In original language o~ presentation) EM/RC14/Tech.Disc./3 TABLE OF CONTENTS INFANTILE DIARRHOEA IN EGYPl', UAR, by A. Shafik Abbasy, M.D. 1 I Assessment of the Magnitude of Diarrhoeal Disease 1 II Study of Factors Influencing Morbidity and Mortality 3 III Etiological Studies 7 IV Conclusion 13 V Recommendations 13 References 17 INFANTILE DIARRHOEA IN EGYPl', UAR, by Dr. Girgis Abd-EI-Messih 21 I Introduction 21 II Statistical Data in Egypt 22 III Socio-Economic and Environmental Sanitary Factors in Relation to Infantile Diarrhoea 23 IV Comparison between Rates in Egypt and in some other Countries 24 V The Problem of Infantile Diarrhoea in Egypt 25 References 27 Tables 1 to 8 28 MANAGEMENT OF THE DIARRHOEAL DISEASES IN IRAN, by Dr. Hassan Ahari 35 References 42 INFAl·lrILE DIARRHOEA - Summary of Routine Care and Conclusions 43 observed at the Paediatric Ward, Pahlavi University Hospital, Teheran, by Mohammad Gharib, M.D. THE PROBLEM OF INFANTILE DIARRHOEA IN PAKISTAN, by Dr. Hamid Ali Khan 47 I Case History 48 II Degree of Dehydration 49 III Laboratory Investigation 50 IV Principles of Treatment followed 51 V Results and Analysis 53 VI Treatment and Results 56 VII Further Plans for the Study 57 L 'ETAT ACTUEL DES DIARRHEES INFANTlIES EN IRAN, par le Dr. -

Gastritis - Symptoms and Causes - Mayo Clinic Visited 11/22/2019
Gastritis - Symptoms and causes - Mayo Clinic Visited 11/22/2019 Request an Appointment Find a Doctor MENU Find a Job Give Now Log in to Patient Account English Patient Care & Health Information Diseases & Conditions Request an Gastritis Appointment Symptoms & causes Diagnosis & treatment Doctors & departments Overview Print Advertisement Gastritis is a general term for a group Mayo Clinic does not endorse companies or of conditions with one thing in common: products. Advertising revenue supports our not- inflammation of the lining of the for-profit mission. stomach. The inflammation of gastritis Advertising & Sponsorship is most often the result of infection with Policy Opportunities Ad Choices the same bacterium that causes most stomach ulcers. Regular use of certain Stomach and pain relievers and drinking too much pyloric valve Mayo Clinic Marketplace alcohol also can contribute to gastritis. Check out these best-sellers and special offers on books and newsletters from Mayo Clinic. Gastritis may occur suddenly (acute gastritis), or appear slowly over time (chronic gastritis). In some cases, gastritis NEW – Guide to Fibromyalgia can lead to ulcers and an increased risk of stomach cancer. Instant access – Mayo Clinic Health Letter For most people, however, gastritis isn't serious and improves quickly with treatment. Diabetes? This diet works … Stop osteoporosis in its tracks The Mayo Clinic Diet Online Products & Services Book: Mayo Clinic on Digestive Health https://www.mayoclinic.org/diseases-conditions/gastritis/symptoms-causes/syc-20355807[11/22/2019 4:16:25 PM] Gastritis - Symptoms and causes - Mayo Clinic Visited 11/22/2019 Symptoms The signs and symptoms of gastritis include: Gnawing or burning ache or pain (indigestion) in your upper abdomen that may become either worse or better with eating Nausea Vomiting A feeling of fullness in your upper abdomen after eating Gastritis doesn't always cause signs and symptoms. -

Association of Helicobacter Pylori Infection and Chronic Atrophic
www.impactjournals.com/oncotarget/ Oncotarget, Vol. 7, No. 13 Association of helicobacter pylori infection and chronic atrophic gastritis with risk of colonic, pancreatic and gastric cancer: A ten-year follow-up of the ESTHER cohort study Xin-Zu Chen1,2,*, Ben Schöttker2,*, Felipe Andres Castro2, Hongda Chen2, Yan Zhang2, Bernd Holleczek2,3, Hermann Brenner2,4 1Department of Gastrointestinal Surgery, West China Hospital, Sichuan University, Chengdu, China 2Division of Clinical Epidemiology and Aging Research, German Cancer Research Center (DKFZ), Heidelberg, Germany 3Saarland Cancer Registry, Saarbrücken, Germany 4German Cancer Consortium (DKTK), Heidelberg, Germany *These authors contributed equally to this work Correspondence to: Hermann Brenner, e-mail: [email protected] Keywords: helicobacter pylori, chronic atrophic gastritis, colon cancer, pancreatic cancer, gastric cancer Received: November 21, 2015 Accepted: February 09, 2016 Published: March 06, 2016 ABSTRACT Objectives: To assess the association of H. pylori and chronic atrophic gastritis (AG) with colonic, pancreatic and gastric cancer in a population-based prospective cohort. Methods: Serum antibodies against H. pylori in general and specific to cytotoxin- associated gene A (CagA), as well as serum pepsinogen I and II were analyzed in 9,506 men and women, aged 50–75 years in a cohort study from Saarland, Germany. Incident cases of colonic, pancreatic and gastric cancer were ascertained by record linkage with data from the Saarland Cancer Registry. Results: During an average follow-up of 10.6 years, 108 colonic, 46 pancreatic and 27 gastric incident cancers were recorded. There was no association between H. pylori infection and colonic cancer (HR = 1.07; 95% CI 0.73–1.56) or pancreatic cancer (HR = 1.32; 0.73–2.39), regardless of either CagA seropositivity or AG status. -

Gastroesophageal Reflux Disease (GERD)
Guidelines for Clinical Care Quality Department Ambulatory GERD Gastroesophageal Reflux Disease (GERD) Guideline Team Team Leader Patient population: Adults Joel J Heidelbaugh, MD Objective: To implement a cost-effective and evidence-based strategy for the diagnosis and Family Medicine treatment of gastroesophageal reflux disease (GERD). Team Members Key Points: R Van Harrison, PhD Diagnosis Learning Health Sciences Mark A McQuillan, MD History. If classic symptoms of heartburn and acid regurgitation dominate a patient’s history, then General Medicine they can help establish the diagnosis of GERD with sufficiently high specificity, although sensitivity Timothy T Nostrant, MD remains low compared to 24-hour pH monitoring. The presence of atypical symptoms (Table 1), Gastroenterology although common, cannot sufficiently support the clinical diagnosis of GERD [B*]. Testing. No gold standard exists for the diagnosis of GERD [A*]. Although 24-hour pH monitoring Initial Release is accepted as the standard with a sensitivity of 85% and specificity of 95%, false positives and false March 2002 negatives still exist [II B*]. Endoscopy lacks sensitivity in determining pathologic reflux but can Most Recent Major Update identify complications (eg, strictures, erosive esophagitis, Barrett’s esophagus) [I A]. Barium May 2012 radiography has limited usefulness in the diagnosis of GERD and is not recommended [III B*]. Content Reviewed Therapeutic trial. An empiric trial of anti-secretory therapy can identify patients with GERD who March 2018 lack alarm or warning symptoms (Table 2) [I A*] and may be helpful in the evaluation of those with atypical manifestations of GERD, specifically non-cardiac chest pain [II B*]. Treatment Ambulatory Clinical Lifestyle modifications. -

Clinical Biliary Tract and Pancreatic Disease
Clinical Upper Gastrointestinal Disorders in Urgent Care, Part 2: Biliary Tract and Pancreatic Disease Urgent message: Upper abdominal pain is a common presentation in urgent care practice. Narrowing the differential diagnosis is sometimes difficult. Understanding the pathophysiology of each disease is the key to making the correct diagnosis and providing the proper treatment. TRACEY Q. DAVIDOFF, MD art 1 of this series focused on disorders of the stom- Pach—gastritis and peptic ulcer disease—on the left side of the upper abdomen. This article focuses on the right side and center of the upper abdomen: biliary tract dis- ease and pancreatitis (Figure 1). Because these diseases are regularly encountered in the urgent care center, the urgent care provider must have a thorough understand- ing of them. Biliary Tract Disease The gallbladder’s main function is to concentrate bile by the absorption of water and sodium. Fasting retains and concentrates bile, and it is secreted into the duodenum by eating. Impaired gallbladder contraction is seen in pregnancy, obesity, rapid weight loss, diabetes mellitus, and patients receiving total parenteral nutrition (TPN). About 10% to 15% of residents of developed nations will form gallstones in their lifetime.1 In the United States, approximately 6% of men and 9% of women 2 have gallstones. Stones form when there is an imbal- ©Phototake.com ance in the chemical constituents of bile, resulting in precipitation of one or more of the components. It is unclear why this occurs in some patients and not others, Tracey Q. Davidoff, MD, is an urgent care physician at Accelcare Medical Urgent Care in Rochester, New York, is on the Board of Directors of the although risk factors do exist. -

In Patients with Crohn's Disease Gut: First Published As 10.1136/Gut.38.3.379 on 1 March 1996
Gut 1996; 38: 379-383 379 High frequency of helicobacter negative gastritis in patients with Crohn's disease Gut: first published as 10.1136/gut.38.3.379 on 1 March 1996. Downloaded from L Halme, P Karkkainen, H Rautelin, T U Kosunen, P Sipponen Abstract In a previous study we described upper gastro- The frequency of gastric Crohn's disease intestinal lesions characteristic of CD in 17% has been considered low. This study was of patients with ileocolonic manifestations of undertaken to determine the prevalence of the disease.10 Furthermore, 40% of these chronic gastritis and Helicobacter pylori patients had chronic, non-specific gastritis. infection in patients with Crohn's disease. This study aimed to determine the prevalence Oesophagogastroduodenoscopy was per- of chronic gastritis and that of H pylori infec- formed on 62 consecutive patients suffer- tion in patients with CD who had undergone ing from ileocolonic Crohn's disease. oesophagogastroduodenoscopy (OGDS) at the Biopsy specimens from the antrum and Fourth Department of Surgery, Helsinki corpus were processed for both histological University Hospital between 1989 and 1994. and bacteriological examinations. Hpylori antibodies of IgG and IgA classes were measured in serum samples by enzyme Patients and methods immunoassay. Six patients (9.70/o) were During a five year period from September 1989 infected with H pylorn, as shown by histo- to August 1994, OGDS was performed on 62 logy, and in five of them the infection consecutive patients with CD to establish the was also verified by serology. Twenty one distribution of their disease. During the study patients (32%) had chronic H pyloni period, the OGDS was repeated (one to seven negative gastritis (negative by both times) - on three patients because of anaemia histology and serology) and one of them and on five patients because of upper gastroin- also had atrophy in the antrum and corpus. -

ICD 9-10 Common Codes Gastrocenterology 1115
TM ICD-9-CM and ICD-10-CM Common Codes for Gastroenterology ICD-9 ICD-10 ICD-9 ICD-10 Diagnoses Diagnoses Code Code Code Code Infectious gastroenteritis and colitis, Ulcerative (chronic) pancolitis without 009.1 A09 556.5 K51.00 complications H. Pylori as the cause of disease Other ulcerative colitis without 041.86 B96.81 556.8 K51.80 necessary complications Chronic viral hepatitis b without Vascular disorder of intestine, 070.32 B18.1 557.9 K55.9 delta-agent 070.54 Chronic viral hepatitis c B18.2 558.9 K52.89 Malignant neoplasm of colon, gastroenteritis and colitis 153.9 C18.9 560.31 Gallstone ileus K56.3 211.3 Polyp of colon K63.5 Diverticulosis large intestine w/o 562.1 K57.30 Hemangioma of intra-abdominal perforation or abscess 228.04 D18.03 structures Diverticulitis large intestine w/o 562.11 K57.32 Neoplasm of uncertain behavior of perforation or abscess 235.3 D37.6 liver and biliary passages 564.00 K59.00 278.00 E66.9 Irritable bowel syndrome without 564.1 K58.9 280.9 D50.9 diarrhea 285.9 D64.9 564.5 Functional diarrhea K59.1 455.6 K64.9 565 K60.2 455.8 Other hemorrhoids K64.8 569.3 Hemorrhage of anus and rectum K62.5 530.11 K21.0 569.42 K62.89 without esophagitis rectum 530.3 Esophageal obstruction K22.2 569.89 Enteroptosis K63.4 K63.89 530.81 K21.9 w/o esophagitis 571 Alcoholic fatty liver K70.0 530.85 Barrett's esophagus without dysplasia K22.70 571.1 Alcoholic hepatitis without ascites K70.10 Acute gastric ulcer without Chronic active hepatitis, not 531.3 K25.3 571.49 K73.2 hemorrhage or perforation Other chronic hepatitis, -
Clinical Remission and Normalization of Laboratory Studies in a Patient
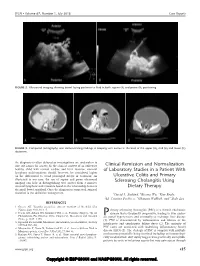
JPGN Volume 67, Number 1, July 2018 Case Reports FIGURE 2. Ultrasound imaging showing bowel laying posterior to fluid in both supine (A) and prone (B) positioning. FIGURE 3. Computed tomography scan demonstrating findings in keeping with ascites at the level of the upper (A), mid (B) and lower (C) abdomen. the diagnosis is often delayed as investigations are undertaken to rule out causes for ascites. In the clinical context of an otherwise Clinical Remission and Normalization healthy child with normal cardiac and liver function, omental of Laboratory Studies in a Patient With lymphatic malformations should, however, be considered higher on the differential to avoid prolonged delays in treatment. As Ulcerative Colitis and Primary illustrated in our case, the use of supine and prone ultrasound imaging can help in distinguishing true ascites from a massive Sclerosing Cholangitis Using omental lymphatic malformation based on the relationship between Dietary Therapy the small bowel and fluid. Once the diagnosis is suspected, surgical resection is the definitive management. ÃDavid L. Suskind, yBicong Wu, ÃKim Braly, zM. Cristina Pacheco, ÃGhassan Wahbeh, and ÃDale Lee REFERENCES 1. Greene AK. Vascular anomalies: current overview of the field. Clin Plastic Surg 2011;38:1–5. rimary sclerosing cholangitis (PSC) is a chronic cholestatic 2. Coran AG, Adzick NS, Krummel TM, et al. Pediatric Surgery. 7th ed. disease that is frequently progressive, leading to liver cirrho- Philadelphia, PA: Elsevier; 2012. Chapter 91, Mesenteric and Omental sis,P portal hypertension, and eventually to end-stage liver disease Cysts, p. 1165–1170. (1). PSC is characterized by inflammation and fibrosis of the 3. -

Autoimmune Diseases in Autoimmune Atrophic Gastritis
Acta Biomed 2018; Vol. 89, Supplement 8: 100-103 DOI: 10.23750/abm.v89i8-S.7919 © Mattioli 1885 Review Autoimmune diseases in autoimmune atrophic gastritis Kryssia Isabel Rodriguez-Castro1, Marilisa Franceschi1, Chiara Miraglia1, Michele Russo1, Antonio Nouvenne1, Gioacchino Leandro3, Tiziana Meschi1, Gian Luigi de’ Angelis1, Francesco Di Mario1 1 Endoscopy Unit, Department of Surgery, ULSS7-Pedemontana, Santorso Hospital, Santorso (VI), Italy; 2 Department of Me- dicine and Surgery, University of Parma, Parma, Italy; 3 National Institute of Gastroenterology “S. De Bellis” Research Hospital, Castellana Grotte, Italy Summary. Autoimmune diseases, characterized by an alteration of the immune system which results in a loss of tolerance to self antigens often coexist in the same patient. Autoimmune atrophic gastritis, characterized by the development of antibodies agains parietal cells and against intrinsic factor, leads to mucosal destruction that affects primarily the corpus and fundus of the stomach. Autoimmune atrophic gastritis is frequently found in association with thyroid disease, including Hashimoto’s thyroiditis, and with type 1 diabetes mellitus, Other autoimmune conditions that have been described in association with autoimmune atrophic gastritis are Ad- dison’s disease, chronic spontaneous urticaria, myasthenia gravis, vitiligo, and perioral cutaneous autoimmune conditions, especially erosive oral lichen planus. Interestingly, however, celiac disease, another frequent auto- immune condition, seems to play a protective role for