Massachusetts Breastfeeding Resource Guide
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Unresolved, Atraumatic Breast Hematoma: Post-Irradiation Or Secondary Breast Angiosarcoma
Breast Disease 33 (2011/2012) 139142 139 DOI 10.3233/BD-2012-0331 IOS Press Case Report Unresolved, atraumatic breast hematoma: Post-irradiation or secondary breast angiosarcoma Glenn Hanna, Samuel J. Lin, Michael D. Wertheimer and Ranjna Sharma Department of Surgery, Beth Israel Deaconess Medical Center, Harvard Medical School, Boston, MA, USA Department of Plastic and Reconstructive Surgery, Beth Israel Deaconess Medical Center, Harvard Medical School, Boston, MA, USA Abstract. Post-irradiation or secondary angiosarcoma of the breast was rst described in the 1980s in patients treated with breast conserving therapy for cancer. The primary management of radiation-induced breast angiosarcoma has focused on surgical resection with an emphasis on achieving negative tumor margins. While surgery remains a key component of treatment, novel therapeutic approaches have surfaced. Despite such advances in treatment, prognosis remains poor. Keywords: Breast cancer, breast conservation therapy, secondary angiosarcoma 1. Clinical scenario amination showed the left breast to be larger than the right, with a 10 15cm areaofa clinicalhematomalo- A 64-year-old post-menopausal Caucasian female cated in the superior and inferior outer quadrants. The presented to our institution with a seven month history overlying skin was hemorrhagic, necrotic and had in- of an unresolved left breast hematoma. Of note, she durated features with areas of active bleeding. Initially, had a history of left breast inltrating ductal carcinoma no discrete underlying mass was identied on physical that was Her-2/Neu negative with estrogen and proges- examination. Areas of peau de orange surrounded the terone receptor positivity seven years prior. She had lesion. She had no palpable lymphadenopathy. -

Chapter Nineteen Breastfeeding Education and Support
Chapter Nineteen Breastfeeding Education and Support Chapter Nineteen – Breastfeeding Education and Support Contents Chapter Nineteen Breastfeeding Education and Support .................................................................... 19-1 Overview .............................................................................................................................................. 19-6 Introduction ..................................................................................................................................... 19-6 In This Chapter ................................................................................................................................. 19-6 Section A Breastfeeding Promotion ..................................................................................................... 19-7 Staffing ............................................................................................................................................. 19-7 Funding ............................................................................................................................................ 19-7 WIC Breastfeeding Committee ........................................................................................................ 19-7 Clinic Environment ........................................................................................................................... 19-7 Breastfeeding Messages and Resources ......................................................................................... -

The Thoracic Radiologist's Guide to the Breast
The Thoracic Radiologist’s Guide to the Breast Gurpriya Gupta MD, Stacy Ries, DO, Jillian Krauss MD, Sayf Al-Katib MD, and Michael Farah MD 1: Beaumont Health System, Royal Oak MI Learning Objectives T o recognize normal CT appearance of breast tissue as CT may often provide the first images of the breast ⦿ To identify CT cross-sectional imaging appearance of benign and malignant breast processes in females and males ⦿ To become familiar with expected cross-sectional imaging appearance of the post-operative breast and recognize post-operative complications ⦿ To discuss the potential advantages of CT evaluation of the breast and encourage accurate description of findings for more valuable reporting ⦿ DisclosureDisclosures The authors of this educational exhibit have no significant financial disclosures to make. Introduction • Increased utilization of CT imaging has led to increased detection of incidental breast lesions • CT may be the first evaluation of the breast • Breast findings may easily be missed or not appropriately managed • 2003 study evaluating MDCT perform on 149 women with 173 breast lesions (Inoue et al) • Features predictive of malignancy: irregular margins, irregular shape, and rim enhancement • 2010 study with 78 incidental breast lesions on CT (Moyle et al) • Best morphological predictors of malignancy: spiculation and irregularity • Calcification patterns were found to be “diagnostically unhelpful” • Limited literature regarding imaging features for benign breast findings on CT. • Therefore, in the absence of long-term -

R2P2 Resident Radpath .Pptx
Clues You Can Use: Core Breast Breast Imaging Division March 2018 BI-RADS® Assessment Categories o Assessments are divided into incomplete Category 0 and final assessment categories Categories 1-6 o Overall assessment based on the most worrisome finding or the need for immediate additional evaluation o Screening mammograms may be assigned Category 0,1,2 BI-RADS® Assessment Categories o BI-RADS® Category 0: INCOMPLETE - NEED ADDITIONAL IMAGING EVALUATION AND/OR PRIOR MAMMOGRAMS FOR COMPARISON o BI-RADS® Category 1: NEGATIVE o BI-RADS® Category 2: BENIGN o BI-RADS® Category 3: PROBABLY BENIGN o BI-RADS® Category 4: SUSPICIOUS o BI-RADS® Category 5: HIGHLY SUGGESTIVE OF MALIGNANCY o BI-RADS® Category 6: KNOWN BIOPSY-PROVEN MALIGNANCY Management Recommendations o Management recommendations on a per Assessment basis o Wording emphasizes recall, routine mammography screening, tissue diagnosis, surgical excision o Management recommended wording for tissue diagnosis is: “Biopsy should be performed in the absence of clinical contraindications.” o Management recommended wording for BI-RADS® 6 is : “Surgical excision when clinically appropriate.” o Category 0: INCOMPLETE - NEED ADDITIONAL IMAGING EVALUATION AND/OR PRIOR MAMMOGRAMS FOR COMPARISON Recall for additional imaging and/or comparison with prior examinations o Category 1: NEGATIVE Routine mammography screening o Category 2: BENIGN Routine mammography screening o Category 3: PROBABLY BENIGN Short interval 6 month follow-up OR continued surveillance o Category 4: SUSPICIOUS ABNORMALITY Biopsy -

Amy Spangler MN, RN, IBCLC
...Location Information… Conference: RAISING AWARENESS: CURRENT ISSUES IN This program is approved for 6.0 Owensboro Health Regional Hospital 1201 Pleasant Valley Road LACTATION CPEUs by the Commission on Owensboro, KY 42303 Dietetic Registration (CDR). 270-417-2000 Western Kentucky Café meeting rooms A,B,C,D Parking Lot A, Hospital entrance A, Follow signs Breastfeeding Coalition This program is approved for st to the Café mtg. rooms on 1 floor. 15th Annual Conference 4.75 L-CERPS and 1.25 R– CERPS OwensboroHealth.org by IBCLE, approval # C1551175. This program has been awarded Lodging: 7.2 Contact Hours (50 minutes Hampton Inn & Suites Downtown/Waterfront 401 W. 2nd Street per contact hour) approved by the Owensboro, KY 42301 Kentucky Board of Nursing KBN 270-685-2005 Provider # 5-0033-1-15-011. http://hamptoninn.hilton.com/en/hp/groups/ personalized/O/OWBDWHX-WKB-20150806/ index.jhtml Featuring: Deadline for block rate is July 6. Amy Spangler About the Speaker: MN, RN, IBCLC Amy Spangler earned her baccalaureate degree in nursing from Ohio State University and her master’s degree in maternal and child health from the University of Florida. She is an International Board Certified Lactation Consultant, a former president of the International Owensboro Health Lactation Consultant Association, and a former Regional Hospital chair of the United States Breastfeeding 1201 Pleasant Valley Road Committee. Amy is a member of the adjunct Owensboro, KY 42303 faculty at Emory University, College of Nursing and 270-417-2000 currently serves as President of baby gooroo. 855-417-8555 She is the author of BREASTFEEDING, A Parent’s We love babies, and we especially love Guide, BREASTFEEDING, Your guide to a healthy, happy babies. -

Breastfeeding Resources I N T H E Finger Lakes R E G I O N
Breastfeeding Resources I n t h e Finger Lakes R e g i o n Community Breastfeeding Support Resources: SPCC WIC: Breastfeeding Peer Counselor Program and Breast Pump Program. Breastfeeding Coordinator -1 888-942-6886 ext. 305 Cornell Cooperative Extension (CCE) in Wayne County. Maureen Weidman, IBCLC, RLC, Breastfeeding Classes & Breastfeeding Support 1-315-331-8415 Cornell Cooperative Extension (CCE) in Seneca County. Devra Rivkin, CLC, 1-315-539-9252 or © 1-315-651-6106 La Leche League (LLL): Mother to Mother Breastfeeding Support Groups Rochester Area:(211) 1-585-275-5151 Finger Lakes Area: 1-315-548-7980 Ontario County Public Health Maternal Child Health Nurse and CLC 1-800-299-2995 Child and Family Resources: Teresa Kennedy, CLC– 585-919-2476 ext.2506 or Natalie Ball, CLC– 315-781-1491 Breast Pumps are now covered by insurance providers due to Internet Breastfeeding Resources: the Affordable Care Act. Most providers require a prescription from your Health Care Provider. For more information, contact New York State Department of Health Breastfeeding Website a local or national durable medical supplier listed below. www.breastfeedingpartners.org Health Systems Services: 1-585-905-0583 La Leche League International’s Website 699 South Main Street, Canandaigua NY 14424 www.llli.org Southside Medical Supply: 1-585-271-7141 1815 South Clinton Ave, suite 405, Rochester Baby GooRoo Website, by Amy Spangler, RN IBCLC Nu-Life Medical Supplies: 1-585-672-5105 www.babygooroo.com 7300 Pittsford-Palmyra Rd, Fairport Westside Medical Supply : 1-585-227-8750 765 Elmgrove Rd., Rochester, NY 14624 sdrive\breastfeeding 2015\breastfeedingreasourcelist This institution is an equal opportunity provider. -

Human Milk Insights Sept 2019
September 2019 The Human Milk Insights newsletter presents the latest breastfeeding topics and clinical practice solutions, addresses coding issues challenging the lactation community, features a lactation service, and announces upcoming webinars and conferences. CONTRIBUTORS FEATURED STORIES THIS MONTH Katie McGee, RN, BSN, IBCLC Education Consultant NEWS YOU CAN USE Westchester, IL ▪ Human Milk and Legislation Maria Lennon, MSN, CNM, IBCLC ▪ Human Milk and Economics Nurse-Midwife, Perinatal Education ▪ Human Milk and Medications Consultant ▪ Human Milk Protocol Sedona, AZ. ▪ Human Milk and Organizations Irene M. Zoppi RN, MSN, IBCLC ▪ Human Milk and NICU Clinical Education Specialist ▪ Human Milk and Infant Health Medela, LLC. ▪ Human Milk and Maternal Health McHenry, IL. HUMAN MILK EDUCATION ▪ Human Milk Monthly Webinar Series ▪ Neonatal Perspectives ▪ Talking Points Flashcards ▪ Welcome CLINICAL PEARLS IN LACTATION ▪ A Serious Topic: A Mother’s Mental Health TOOLS YOU CAN USE ▪ Resources for Perinatal Mental Health SPOTLIGHT ON PRACTICE ▪ Amy K. Spangler, MN, RN, IBCLC, FILCA NEWS YOU CAN USE The Academy of Breastfeeding Medicine HUMAN MILK AND LEGISLATION released a new protocol for breastfeeding infants with cleft lip, cleft palate, or cleft lip Law requiring accommodations for and palate. breastfeeding families https://www.bfmed.org/protocols On July 25, 2019, the Fairness of Breastfeeding Mothers Act of 2019 was signed into law (Public Law No. 116-30). HUMAN MILK AND ORGANIZATIONS This Act requires that certain public buildings that contain a public restroom also USBC provide a lactation room available for use by The USBC – Affiliated Continuity of Care a member of the public. Constellation has launched a survey titled http://www.usbreastfeeding.org/fairness-act “Continuity of Care in Breastfeeding Support – Summer 2019 Survey.” The survey is aimed to develop a framework of what HUMAN MILK AND ECONOMICS continuity of care in breastfeeding support means, as well as identifying barriers and Breastfeeding Savings Calculator opportunities for improvement. -

Maintain Milk Supply
Connecticut WIC Program: Consistent Breastfeeding Education Messages: Building & Maintaining a Milk Supply Why is this important? Extending the duration of breastfeeding extends the impact of breastfeeding benefits for mom and infant. Offering guidance and support prior to delivery, within the first weeks postpartum and beyond helps women increase their duration of breastfeeding by building and maintaining a sufficient milk supply WIC’s Goal: Assist mothers in learning the skills to build and maintain a milk supply. Increase duration of breastfeeding for WIC participants. Learning Objectives: After participating in a group session or individual counseling the participant will: 1. Identify their breastfeeding goals Assess: • Willingness to breastfeed, breastfeeding goals • Social support: spouse/partner, family, friends • Medical support: WIC, Healthcare provider (ideally w/CLC or IBCLC on staff) • Community support: local BF support group, LLL 2. Understand the importance of the early postpartum period in building and maintaining a milk supply 3. Identify key steps they can take to get breastfeeding off to a good start 4. Know how to tell if their infant is getting enough breast milk 5. Learn where to go for additional support in the community to build and maintain an adequate milk supply to meet their breastfeeding goals Key Educational Messages: Prenatal BF support Affirmation: It’s good you’ve thought about how you’re planning to feed your baby. Many other moms feel overwhelmed with all the information they receive. • Put baby to breast within the first hour after delivery/ Encourage mom to practice rooming-in • Educate about colostrum and differences in onset of milk supply (DM, cesarean delivery, etc) Birth to 6 weeks postpartum Affirmation: Wow! You are doing a great job! OR Yes, a lot of mom experience that, it’s normal to feel that way. -

Pennsylvania Breastfeeding Referral Guide
PENNSYLVANIA BREASTFEEDING REFERRAL GUIDE Revised June 2020 Table of Contents Introduction .......................................................................................................................................... 5 Definitions ............................................................................................................................................ 6 Information for All Counties.................................................................................................................. 7 ADAMS................................................................................................................................................ 8 ALLEGHENY ....................................................................................................................................... 9 ARMSTRONG ................................................................................................................................... 11 BEAVER ............................................................................................................................................ 12 BEDFORD ......................................................................................................................................... 13 BERKS .............................................................................................................................................. 14 BLAIR ............................................................................................................................................... -

Methods and Material
THE MAMMOGRAPHIC AND SONOGRAPHIC FEATURES OF MALE BREAST DISEASES AT KING HUSSEIN MEDICAL CENTRE Amal A. Smadi, MD, JBR* ABSTRACT Objectives: To describe the mammographic and sonographic features of male breast diseases, and to correlate the radiological, cytological and histopathological diagnoses. Methods: This is a retrospective descriptive study that was conducted at King Hussein Medical Centre, Amman, Jordan between January 1st 2004 and December 31st 2007. The mammograms and breast ultrasounds of 88 symptomatic male patients were reviewed and analyzed. A total of 24 patients with unilateral breast masses underwent fine-needle aspiration, eight of them with suspected malignant lesions underwent further true cut biopsy and surgery. The radiological, cytological and histopathological diagnoses were correlated. Results: Sixty one (70%) patients had gynaecomastia, 15 (17%) had fatty breasts (pseudo-gynaecomastia), eight (9%) had primary breast carcinoma, two (2%) had lipomas, one (1%) had abscess, and one (1%) had hematoma. The characteristic radiological features were confirmed by fine-needle aspiration cytology in 16 patients and by both cytology and histopathology studies in eight cases. Conclusion: Radiological findings provide characteristic diagnostic appearances for certain important male breast diseases. The radiological features can be accurately correlated with pathological diagnosis. Key words: Male Breast, Mammography, Sonography JRMS March 2010; 17(1): 57-61 Introduction in diagnosis can result from ignorance of the Breast disorders in males can be distressing and existence of breast cancer in males, and this may patients often feel embarrassed and anxious.(1) In adversely affect prognosis. In evaluating the our community a male patient with breast clinically abnormal male breast, mammography and ultrasound are essential, and should be performed enlargement or mass will be very reluctant to seek (2) medical advice as this might be considered a social along with the physical clinical examination. -
Keep It Simple, Third Edition/Amy Spangler Section
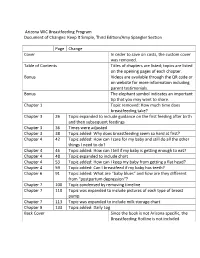
Arizona WIC Breastfeeding Program Document of Changes: Keep It Simple, Third Edition/Amy Spangler Section Page Change Cover In order to save on costs, the custom cover was removed. Table of Contents Titles of chapters are listed; topics are listed on the opening pages of each chapter. Bonus Videos are available through the QR code or on website for more information including parent testimonials. Bonus The elephant symbol indicates an important tip that you may want to share. Chapter 1 Topic removed: How much time does breastfeeding take? Chapter 3 26 Topic expanded to include guidance on the first feeding after birth and then subsequent feedings Chapter 3 36 Times were adjusted Chapter 3 38 Topic added: Why does breastfeeding seem so hard at first? Chapter 4 42 Topic added: How can I care for my baby and still do all the other things I need to do? Chapter 4 46 Topic added: How can I tell if my baby is getting enough to eat? Chapter 4 48 Topic expanded to include chart Chapter 4 53 Topic added: How can I keep my baby from getting a flat head? Chapter 4 59 Topic added: Can I breastfeed if my baby has teeth? Chapter 6 91 Topic added: What are “baby blues” and how are they different from “postpartum depression”? Chapter 7 100 Topic condensed by removing timeline Chapter 7 110 Topic was expanded to include pictures of each type of breast pump. Chapter 7 113 Topic was expanded to include milk storage chart. Chapter 9 133 Topic added: Daily Log Back Cover Since the book is not Arizona specific, the Breastfeeding Hotline is not included. -

The CDC Guide to Breastfeeding Interventions
U.S. Department of Health and Human Services Katherine R. Shealy, MPH, IBCLC, RLC Ruowei Li, MD, PhD Sandra Benton-Davis, RD, LD Laurence M. Grummer-Strawn, PhD U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES Centers for Disease Control and Prevention National Center for Chronic Disease Prevention and Health Promotion Division of Nutrition and Physical Activity Acknowledgments We gratefully acknowledge and thank all contributors and reviewers of The CDC Guide to Breastfeeding Interventions. The efforts of Jane Heinig, PhD, IBCLC, RLC, Deborah Galuska, PhD, Diana Toomer, Barbara Latham, RD, LD, Carol MacGowan, MPH, RD, LD, Robin Hamre, MPH, RD, and members of the CDC Obesity Team helped make this document possible. Publication Support was provided by Palladian Partners, Inc., under Contract No. 200-980-0415 for the National Center for Chronic Disease Prevention and Health Promotion, Centers for Disease Control and Prevention, U.S. Department of Health and Human Services. Photographs contained in this guide were purchased solely for educational purposes and may not be reproduced for commercial use. Recommended Citation Shealy KR, Li R, Benton-Davis S, Grummer-Strawn LM. The CDC Guide to Breastfeeding Interventions. Atlanta: U.S. Department of Health and Human Services, Centers for Disease Control and Prevention, 2005. For more information or to download this document or sections of this document, please visit http://www.cdc.gov/breastfeeding To request additional copies of this document, please email your request to [email protected] or write to us at the following address and request The CDC Guide to Breastfeeding Interventions: Maternal and Child Nutrition Branch, Division of Nutrition and Physical Activity National Center for Chronic Disease Prevention and Health Promotion Centers for Disease Control and Prevention 4770 Buford Highway, NE Mailstop K–25 Atlanta, Georgia 30341-3717 Contents Introduction Introduction .