Red Blood Cell Antigen Genotyping
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Human and Mouse CD Marker Handbook Human and Mouse CD Marker Key Markers - Human Key Markers - Mouse
Welcome to More Choice CD Marker Handbook For more information, please visit: Human bdbiosciences.com/eu/go/humancdmarkers Mouse bdbiosciences.com/eu/go/mousecdmarkers Human and Mouse CD Marker Handbook Human and Mouse CD Marker Key Markers - Human Key Markers - Mouse CD3 CD3 CD (cluster of differentiation) molecules are cell surface markers T Cell CD4 CD4 useful for the identification and characterization of leukocytes. The CD CD8 CD8 nomenclature was developed and is maintained through the HLDA (Human Leukocyte Differentiation Antigens) workshop started in 1982. CD45R/B220 CD19 CD19 The goal is to provide standardization of monoclonal antibodies to B Cell CD20 CD22 (B cell activation marker) human antigens across laboratories. To characterize or “workshop” the antibodies, multiple laboratories carry out blind analyses of antibodies. These results independently validate antibody specificity. CD11c CD11c Dendritic Cell CD123 CD123 While the CD nomenclature has been developed for use with human antigens, it is applied to corresponding mouse antigens as well as antigens from other species. However, the mouse and other species NK Cell CD56 CD335 (NKp46) antibodies are not tested by HLDA. Human CD markers were reviewed by the HLDA. New CD markers Stem Cell/ CD34 CD34 were established at the HLDA9 meeting held in Barcelona in 2010. For Precursor hematopoetic stem cell only hematopoetic stem cell only additional information and CD markers please visit www.hcdm.org. Macrophage/ CD14 CD11b/ Mac-1 Monocyte CD33 Ly-71 (F4/80) CD66b Granulocyte CD66b Gr-1/Ly6G Ly6C CD41 CD41 CD61 (Integrin b3) CD61 Platelet CD9 CD62 CD62P (activated platelets) CD235a CD235a Erythrocyte Ter-119 CD146 MECA-32 CD106 CD146 Endothelial Cell CD31 CD62E (activated endothelial cells) Epithelial Cell CD236 CD326 (EPCAM1) For Research Use Only. -

Viewed Under 23 (B) Or 203 (C) fi M M Male Cko Mice, and Largely Unaffected Magni Cation; Scale Bars, 500 M (B) and 50 M (C)
BRIEF COMMUNICATION www.jasn.org Renal Fanconi Syndrome and Hypophosphatemic Rickets in the Absence of Xenotropic and Polytropic Retroviral Receptor in the Nephron Camille Ansermet,* Matthias B. Moor,* Gabriel Centeno,* Muriel Auberson,* † † ‡ Dorothy Zhang Hu, Roland Baron, Svetlana Nikolaeva,* Barbara Haenzi,* | Natalya Katanaeva,* Ivan Gautschi,* Vladimir Katanaev,*§ Samuel Rotman, Robert Koesters,¶ †† Laurent Schild,* Sylvain Pradervand,** Olivier Bonny,* and Dmitri Firsov* BRIEF COMMUNICATION *Department of Pharmacology and Toxicology and **Genomic Technologies Facility, University of Lausanne, Lausanne, Switzerland; †Department of Oral Medicine, Infection, and Immunity, Harvard School of Dental Medicine, Boston, Massachusetts; ‡Institute of Evolutionary Physiology and Biochemistry, St. Petersburg, Russia; §School of Biomedicine, Far Eastern Federal University, Vladivostok, Russia; |Services of Pathology and ††Nephrology, Department of Medicine, University Hospital of Lausanne, Lausanne, Switzerland; and ¶Université Pierre et Marie Curie, Paris, France ABSTRACT Tight control of extracellular and intracellular inorganic phosphate (Pi) levels is crit- leaves.4 Most recently, Legati et al. have ical to most biochemical and physiologic processes. Urinary Pi is freely filtered at the shown an association between genetic kidney glomerulus and is reabsorbed in the renal tubule by the action of the apical polymorphisms in Xpr1 and primary fa- sodium-dependent phosphate transporters, NaPi-IIa/NaPi-IIc/Pit2. However, the milial brain calcification disorder.5 How- molecular identity of the protein(s) participating in the basolateral Pi efflux remains ever, the role of XPR1 in the maintenance unknown. Evidence has suggested that xenotropic and polytropic retroviral recep- of Pi homeostasis remains unknown. Here, tor 1 (XPR1) might be involved in this process. Here, we show that conditional in- we addressed this issue in mice deficient for activation of Xpr1 in the renal tubule in mice resulted in impaired renal Pi Xpr1 in the nephron. -

Mcleod Neuroacanthocytosis Syndrome
NCBI Bookshelf. A service of the National Library of Medicine, National Institutes of Health. Pagon RA, Adam MP, Ardinger HH, et al., editors. GeneReviews® [Internet]. Seattle (WA): University of Washington, Seattle; 1993- 2017. McLeod Neuroacanthocytosis Syndrome Hans H Jung, MD Department of Neurology University Hospital Zurich Zurich, Switzerland [email protected] Adrian Danek, MD Neurologische Klinik Ludwig-Maximilians-Universität München, Germany ed.uml@kenad Ruth H Walker, MD, MBBS, PhD Department of Neurology Veterans Affairs Medical Center Bronx, New York [email protected] Beat M Frey, MD Blood Transfusion Service Swiss Red Cross Schlieren/Zürich, Switzerland [email protected] Christoph Gassner, PhD Blood Transfusion Service Swiss Red Cross Schlieren/Zürich, Switzerland [email protected] Initial Posting: December 3, 2004; Last Update: May 17, 2012. Summary Clinical characteristics. McLeod neuroacanthocytosis syndrome (designated as MLS throughout this review) is a multisystem disorder with central nervous system (CNS), neuromuscular, and hematologic manifestations in males. CNS manifestations are a neurodegenerative basal ganglia disease including (1) movement disorders, (2) cognitive alterations, and (3) psychiatric symptoms. Neuromuscular manifestations include a (mostly subclinical) sensorimotor axonopathy and muscle weakness or atrophy of different degrees. Hematologically, MLS is defined as a specific blood group phenotype (named after the first proband, Hugh McLeod) that results from absent expression of the Kx erythrocyte antigen and weakened expression of Kell blood group antigens. The hematologic manifestations are red blood cell acanthocytosis and compensated hemolysis. Allo-antibodies in the Kell and Kx blood group system can cause strong reactions to transfusions of incompatible blood and severe anemia in newborns of Kell-negative mothers. -

4-6 Weeks Old Female C57BL/6 Mice Obtained from Jackson Labs Were Used for Cell Isolation
Methods Mice: 4-6 weeks old female C57BL/6 mice obtained from Jackson labs were used for cell isolation. Female Foxp3-IRES-GFP reporter mice (1), backcrossed to B6/C57 background for 10 generations, were used for the isolation of naïve CD4 and naïve CD8 cells for the RNAseq experiments. The mice were housed in pathogen-free animal facility in the La Jolla Institute for Allergy and Immunology and were used according to protocols approved by the Institutional Animal Care and use Committee. Preparation of cells: Subsets of thymocytes were isolated by cell sorting as previously described (2), after cell surface staining using CD4 (GK1.5), CD8 (53-6.7), CD3ε (145- 2C11), CD24 (M1/69) (all from Biolegend). DP cells: CD4+CD8 int/hi; CD4 SP cells: CD4CD3 hi, CD24 int/lo; CD8 SP cells: CD8 int/hi CD4 CD3 hi, CD24 int/lo (Fig S2). Peripheral subsets were isolated after pooling spleen and lymph nodes. T cells were enriched by negative isolation using Dynabeads (Dynabeads untouched mouse T cells, 11413D, Invitrogen). After surface staining for CD4 (GK1.5), CD8 (53-6.7), CD62L (MEL-14), CD25 (PC61) and CD44 (IM7), naïve CD4+CD62L hiCD25-CD44lo and naïve CD8+CD62L hiCD25-CD44lo were obtained by sorting (BD FACS Aria). Additionally, for the RNAseq experiments, CD4 and CD8 naïve cells were isolated by sorting T cells from the Foxp3- IRES-GFP mice: CD4+CD62LhiCD25–CD44lo GFP(FOXP3)– and CD8+CD62LhiCD25– CD44lo GFP(FOXP3)– (antibodies were from Biolegend). In some cases, naïve CD4 cells were cultured in vitro under Th1 or Th2 polarizing conditions (3, 4). -

Fcγr Binding and ADCC Activity of Human Igg Allotypes
fimmu-11-00740 May 4, 2020 Time: 17:25 # 1 ORIGINAL RESEARCH published: 06 May 2020 doi: 10.3389/fimmu.2020.00740 FcgR Binding and ADCC Activity of Human IgG Allotypes Steven W. de Taeye1,2*†, Arthur E. H. Bentlage2, Mirjam M. Mebius3, Joyce I. Meesters3, Suzanne Lissenberg-Thunnissen2, David Falck4, Thomas Sénard4, Nima Salehi1, Manfred Wuhrer4, Janine Schuurman3, Aran F. Labrijn3, Theo Rispens1‡ and Gestur Vidarsson2‡ 1 Sanquin Research and Landsteiner Laboratory, Department of Immunopathology, Amsterdam UMC, University of Amsterdam, Amsterdam, Netherlands, 2 Sanquin Research and Landsteiner Laboratory, Department of Experimental Edited by: Immunohematology, Amsterdam UMC, University of Amsterdam, Amsterdam, Netherlands, 3 Genmab, Utrecht, Eric O. Long, Netherlands, 4 Center for Proteomics and Metabolomics, Leiden University Medical Center, Leiden, Netherlands National Institute of Allergy and Infectious Diseases (NIAID), United States Antibody dependent cellular cytotoxicity (ADCC) is an Fc-dependent effector function Reviewed by: of IgG important for anti-viral immunity and anti-tumor therapies. NK-cell mediated Amy W. Chung, ADCC is mainly triggered by IgG-subclasses IgG1 and IgG3 through the IgG-Fc- The University of Melbourne, Australia receptor (FcgR) IIIa. Polymorphisms in the immunoglobulin gamma heavy chain gene Geoffrey Thomas Hart, University of Minnesota Twin Cities, likely form a layer of variation in the strength of the ADCC-response, but this has United States never been studied in detail. We produced all 27 known IgG allotypes and assessed *Correspondence: FcgRIIIa binding and ADCC activity. While all IgG1, IgG2, and IgG4 allotypes behaved Steven W. de Taeye [email protected]; similarly within subclass, large allotype-specific variation was found for IgG3. -
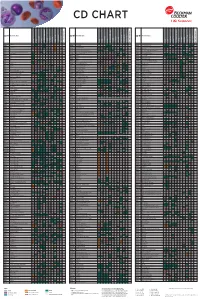
Flow Reagents Single Color Antibodies CD Chart
CD CHART CD N° Alternative Name CD N° Alternative Name CD N° Alternative Name Beckman Coulter Clone Beckman Coulter Clone Beckman Coulter Clone T Cells B Cells Granulocytes NK Cells Macrophages/Monocytes Platelets Erythrocytes Stem Cells Dendritic Cells Endothelial Cells Epithelial Cells T Cells B Cells Granulocytes NK Cells Macrophages/Monocytes Platelets Erythrocytes Stem Cells Dendritic Cells Endothelial Cells Epithelial Cells T Cells B Cells Granulocytes NK Cells Macrophages/Monocytes Platelets Erythrocytes Stem Cells Dendritic Cells Endothelial Cells Epithelial Cells CD1a T6, R4, HTA1 Act p n n p n n S l CD99 MIC2 gene product, E2 p p p CD223 LAG-3 (Lymphocyte activation gene 3) Act n Act p n CD1b R1 Act p n n p n n S CD99R restricted CD99 p p CD224 GGT (γ-glutamyl transferase) p p p p p p CD1c R7, M241 Act S n n p n n S l CD100 SEMA4D (semaphorin 4D) p Low p p p n n CD225 Leu13, interferon induced transmembrane protein 1 (IFITM1). p p p p p CD1d R3 Act S n n Low n n S Intest CD101 V7, P126 Act n p n p n n p CD226 DNAM-1, PTA-1 Act n Act Act Act n p n CD1e R2 n n n n S CD102 ICAM-2 (intercellular adhesion molecule-2) p p n p Folli p CD227 MUC1, mucin 1, episialin, PUM, PEM, EMA, DF3, H23 Act p CD2 T11; Tp50; sheep red blood cell (SRBC) receptor; LFA-2 p S n p n n l CD103 HML-1 (human mucosal lymphocytes antigen 1), integrin aE chain S n n n n n n n l CD228 Melanotransferrin (MT), p97 p p CD3 T3, CD3 complex p n n n n n n n n n l CD104 integrin b4 chain; TSP-1180 n n n n n n n p p CD229 Ly9, T-lymphocyte surface antigen p p n p n -

Blood Bank I D
The Osler Institute Blood Bank I D. Joe Chaffin, MD Bonfils Blood Center, Denver, CO The Fun Just Never Ends… A. Blood Bank I • Blood Groups B. Blood Bank II • Blood Donation and Autologous Blood • Pretransfusion Testing C. Blood Bank III • Component Therapy D. Blood Bank IV • Transfusion Complications * Noninfectious (Transfusion Reactions) * Infectious (Transfusion-transmitted Diseases) E. Blood Bank V (not discussed today but available at www.bbguy.org) • Hematopoietic Progenitor Cell Transplantation F. Blood Bank Practical • Management of specific clinical situations • Calculations, Antibody ID and no-pressure sample questions Blood Bank I Blood Groups I. Basic Antigen-Antibody Testing A. Basic Red Cell-Antibody Interactions 1. Agglutination a. Clumping of red cells due to antibody coating b. Main reaction we look for in Blood Banking c. Two stages: 1) Coating of cells (“sensitization”) a) Affected by antibody specificity, electrostatic RBC charge, temperature, amounts of antigen and antibody b) Low Ionic Strength Saline (LISS) decreases repulsive charges between RBCs; tends to enhance cold antibodies and autoantibodies c) Polyethylene glycol (PEG) excludes H2O, tends to enhance warm antibodies and autoantibodies. 2) Formation of bridges a) Lattice structure formed by antibodies and RBCs b) IgG isn’t good at this; one antibody arm must attach to one cell and other arm to the other cell. c) IgM is better because of its pentameric structure. P}Chaffin (12/28/11) Blood Bank I page 1 Pathology Review Course 2. Hemolysis a. Direct lysis of a red cell due to antibody coating b. Uncommon, but equal to agglutination. 1) Requires complement fixation 2) IgM antibodies do this better than IgG. -

Immuno 2014 No. 1
Journal of Blood Group Serology and Molecular Genetics VOLUME 30, N UMBER 1, 2014 Immunohematology Journal of Blood Group Serology and Molecular Genetics Volume 30, Number 1, 2014 CONTENTS R EPORT 1 Indirect antiglobulin test-crossmatch using low-ionic-strength saline–albumin enhancement medium and reduced incubation time: effectiveness in the detection of most clinically significant antibodies and impact on blood utilization C.L. Dinardo, S.L. Bonifácio, and A. Mendrone, Jr. R EV I EW 6 Raph blood group system M. Hayes R EPORT 11 I-int phenotype among three individuals of a Parsi community from Mumbai, India S.R. Joshi C A SE R EPORT 14 Evans syndrome in a pediatric liver transplant recipient with an autoantibody with apparent specificity for the KEL4 (Kpb) antigen S.A. Koepsell, K. Burright-Hittner, and J.D. Landmark R EV I EW 18 JMH blood group system: a review S.T. Johnson R EPORT 24 Demonstration of IgG subclass (IgG1 and IgG3) in patients with positive direct antiglobulin tests A. Singh, A. Solanki, and R. Chaudhary I N M EMOR ia M 28 George Garratty, 1935–2014 Patricia A. Arndt and Regina M. Leger 30 A NNOUNCEMENTS 34 A DVERT I SEMENTS 39 I NSTRUCT I ONS FOR A UTHORS E D I TOR - I N -C H I EF E D I TOR ia L B OA RD Sandra Nance, MS, MT(ASCP)SBB Philadelphia, Pennsylvania Patricia Arndt, MT(ASCP)SBB Paul M. Ness, MD Pomona, California Baltimore, Maryland M A N AG I NG E D I TOR James P. -

Gene List HTG Edgeseq Immuno-Oncology Assay
Gene List HTG EdgeSeq Immuno-Oncology Assay Adhesion ADGRE5 CLEC4A CLEC7A IBSP ICAM4 ITGA5 ITGB1 L1CAM MBL2 SELE ALCAM CLEC4C DST ICAM1 ITGA1 ITGA6 ITGB2 LGALS1 MUC1 SVIL CDH1 CLEC5A EPCAM ICAM2 ITGA2 ITGAL ITGB3 LGALS3 NCAM1 THBS1 CDH5 CLEC6A FN1 ICAM3 ITGA4 ITGAM ITGB4 LGALS9 PVR THY1 Apoptosis APAF1 BCL2 BID CARD11 CASP10 CASP8 FADD NOD1 SSX1 TP53 TRAF3 BCL10 BCL2L1 BIRC5 CASP1 CASP3 DDX58 NLRP3 NOD2 TIMP1 TRAF2 TRAF6 B-Cell Function BLNK BTLA CD22 CD79A FAS FCER2 IKBKG PAX5 SLAMF1 SLAMF7 SPN BTK CD19 CD24 EBF4 FASLG IKBKB MS4A1 RAG1 SLAMF6 SPI1 Cell Cycle ABL1 ATF1 ATM BATF CCND1 CDK1 CDKN1B NCL RELA SSX1 TBX21 TP53 ABL2 ATF2 AXL BAX CCND3 CDKN1A EGR1 REL RELB TBK1 TIMP1 TTK Cell Signaling ADORA2A DUSP4 HES1 IGF2R LYN MAPK1 MUC1 NOTCH1 RIPK2 SMAD3 STAT5B AKT3 DUSP6 HES5 IKZF1 MAF MAPK11 MYC PIK3CD RNF4 SOCS1 STAT6 BCL6 ELK1 HEY1 IKZF2 MAP2K1 MAPK14 NFATC1 PIK3CG RORC SOCS3 SYK CEBPB EP300 HEY2 IKZF3 MAP2K2 MAPK3 NFATC3 POU2F2 RUNX1 SPINK5 TAL1 CIITA ETS1 HEYL JAK1 MAP2K4 MAPK8 NFATC4 PRKCD RUNX3 STAT1 TCF7 CREB1 FLT3 HMGB1 JAK2 MAP2K7 MAPKAPK2 NFKB1 PRKCE S100B STAT2 TYK2 CREB5 FOS HRAS JAK3 MAP3K1 MEF2C NFKB2 PTEN SEMA4D STAT3 CREBBP GATA3 IGF1R KIT MAP3K5 MTDH NFKBIA PYCARD SMAD2 STAT4 Chemokine CCL1 CCL16 CCL20 CCL25 CCL4 CCR2 CCR7 CX3CL1 CXCL12 CXCL3 CXCR1 CXCR6 CCL11 CCL17 CCL21 CCL26 CCL5 CCR3 CCR9 CX3CR1 CXCL13 CXCL5 CXCR2 MST1R CCL13 CCL18 CCL22 CCL27 CCL7 CCR4 CCRL2 CXCL1 CXCL14 CXCL6 CXCR3 PPBP CCL14 CCL19 CCL23 CCL28 CCL8 CCR5 CKLF CXCL10 CXCL16 CXCL8 CXCR4 XCL2 CCL15 CCL2 CCL24 CCL3 CCR1 CCR6 CMKLR1 CXCL11 CXCL2 CXCL9 CXCR5 -

Introduction to the Rh Blood Group.Pdf
Introduction to the Rhesus Blood Group Justin R. Rhees, M.S., MLS(ASCP)CM, SBBCM University of Utah Department of Pathology Medical Laboratory Science Program Objectives 1. Describe the major Rhesus (Rh) blood group antigens in terms of biochemical structure and inheritance. 2. Describe the characteristics of Rh antibodies. 3. Translate the five major Rh antigens, genotypes, and haplotypes from Fisher-Race to Wiener nomenclature. 4. State the purpose of Fisher-Race, Wiener, Rosenfield, and ISBT nomenclatures. Background . How did this blood group get its name? . 1937 Mrs. Seno; Bellevue hospital . Unknown antibody, unrelated to ABO . Philip Levine tested her serum against 54 ABO-compatible blood samples: only 13 were compatible. Rhesus (Rh) blood group 1930s several cases of Hemolytic of the Fetus and Newborn (HDFN) published. Hemolytic transfusion reactions (HTR) were observed in ABO- compatible transfusions. In search of more blood groups, Landsteiner and Wiener immunized rabbits with the Rhesus macaque blood of the Rhesus monkeys. Rhesus (Rh) blood group 1940 Landsteiner and Wiener reported an antibody that reacted with about 85% of human red cell samples. It was supposed that anti-Rh was the specificity causing the “intragroup” incompatibilities observed. 1941 Levine found in over 90% of erythroblastosis fetalis cases, the mother was Rh-negative and the father was Rh-positive. Rhesus macaque Rhesus (Rh) blood group Human anti-Rh and animal anti- Rh are not the same. However, “Rh” was embedded into blood group antigen terminology. The -

Rabbit Anti-Phospho-CD18-SL10462R-FITC
SunLong Biotech Co.,LTD Tel: 0086-571- 56623320 Fax:0086-571- 56623318 E-mail:[email protected] www.sunlongbiotech.com Rabbit Anti-Phospho-CD18 SL10462R-FITC Product Name: Anti-Phospho-CD18 (Thr758)/FITC Chinese Name: FITC标记的磷酸化整合素β2/Integrin β2抗体 CD18 (Phospho Thr758); CD18 (Phospho-Thr758); CD18 (Phospho T758); p-CD18 (T758); p-CD18 (Thr758); Integrin beta 2; 95 subunit beta; CD 18; CD18; Cell surface adhesion glycoprotein LFA 1/CR3/P150,959 beta subunit precursor); Cell surface adhesion glycoproteins LFA 1/CR3/p150,95 subunit beta; Cell surface adhesion glycoproteins LFA-1/CR3/p150; Complement receptor C3 beta subunit; Complement Alias: receptor C3 subunit beta; Integrin beta chain beta 2; Integrin beta-2; Integrin, beta 2 (complement component 3 receptor 3 and 4 subunit); ITB2_HUMAN; ITGB2; LAD; LCAMB; Leukocyte associated antigens CD18/11A, CD18/11B, CD18/11C; Leukocyte cell adhesion molecule CD18; LFA 1; LFA1; Lymphocyte function associated antigen 1; MAC 1; MAC1; MF17; MFI7; OTTHUMP00000115278; OTTHUMP00000115279; OTTHUMP00000115280; OTTHUMP00000115281; OTTHUMP00000115282. Organism Species: Rabbit Clonality: Polyclonal React Species: Human,Mouse,Rat,Chicken,Dog,Pig,Cow,Horse,Rabbit,Sheep,Guinea Pig, Flow-Cyt=1:50-200ICC=1:50-200IF=1:50-200www.sunlongbiotech.com Applications: not yet tested in other applications. optimal dilutions/concentrations should be determined by the end user. Molecular weight: 82kDa Form: Lyophilized or Liquid Concentration: 1mg/ml KLH conjugated synthesised phosphopeptide derived from human CD18 around the immunogen: phosphorylation site of Thr758 Lsotype: IgG Purification: affinity purified by Protein A Storage Buffer: 0.01M TBS(pH7.4) with 1% BSA, 0.03% Proclin300 and 50% Glycerol. Store at -20 °C for one year. -

3407 M16141436 19 3.Pdf
Immunohematology JOURNAL OF BLOOD GROUP SEROLOGY AND EDUCATION V OLUME 19, NUMBER 3, 2003 Immunohematology JOURNAL OF BLOOD GROUP SEROLOGY AND EDUCATION V OLUME 19, NUMBER 3, 2003 CONTENTS 73 DNA analysis for donor screening of Dombrock blood group antigens J.R. STORRY, C.M.WESTHOFF,D.CHARLES-PIERRE,M.RIOS,K.HUE-ROYE,S.VEGE,S.NANCE, AND M.E. REID 77 Studies on the Dombrock blood group system in non-human primates C. MOGOS,A.SCHAWALDER,G.R. HALVERSON, AND M.E. REID 83 Murine monoclonal antibodies can be used to type RBCs with a positive DAT G.R. HALVERSON,P.HOWARD,H.MALYSKA,E.TOSSAS, AND M.E. REID 86 Rh antigen and phenotype frequencies and probable genotypes for the four main ethnic groups in Port Harcourt, Nigeria Z.A. JEREMIAH AND F.I. BUSERI 89 Antibodies detected in samples from 21,730 pregnant women S. JOVANOVIC-SRZENTIC,M.DJOKIC,N.TIJANIC,R.DJORDJEVIC,N.RIZVAN,D.PLECAS, AND D. FILIMONOVIC 93 BOOK REVIEWS S. GERALD SANDLER,MD THERESA NESTER,MD 95 COMMUNICATIONS Letter to the Editors Letter From the Editors Irregular RBC antibodies in the Ortho Dedication sera of Brazilian pregnant women 97 IN MEMORIAM BERTIL CEDEGREN,MD 98 99 ANNOUNCEMENTS ADVERTISEMENTS 103 INSTRUCTIONS FOR AUTHORS EDITOR-IN-CHIEF MANAGING EDITOR Delores Mallory, MT(ASCP)SBB Mary H. McGinniss,AB, (ASCP)SBB Rockville, Maryland Bethesda, Maryland TECHNICAL EDITOR SENIOR MEDICAL EDITOR Christine Lomas-Francis, MSc Scott Murphy, MD New York, New York Philadelphia, Pennsylvania ASSOCIATE MEDICAL EDITORS S. Gerald Sandler, MD Geralyn Meny, MD Ralph Vassallo, MD Washington, District of Columbia Philadelphia, Pennsylvania Philadelphia, Pennsylvania EDITORIAL BOARD Patricia Arndt, MT(ASCP)SBB W.