Inclusion of Additional Reference Reagents in the Existing Collection of WHO International Reference Reagents for Blood Group Genotyping
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Human and Mouse CD Marker Handbook Human and Mouse CD Marker Key Markers - Human Key Markers - Mouse
Welcome to More Choice CD Marker Handbook For more information, please visit: Human bdbiosciences.com/eu/go/humancdmarkers Mouse bdbiosciences.com/eu/go/mousecdmarkers Human and Mouse CD Marker Handbook Human and Mouse CD Marker Key Markers - Human Key Markers - Mouse CD3 CD3 CD (cluster of differentiation) molecules are cell surface markers T Cell CD4 CD4 useful for the identification and characterization of leukocytes. The CD CD8 CD8 nomenclature was developed and is maintained through the HLDA (Human Leukocyte Differentiation Antigens) workshop started in 1982. CD45R/B220 CD19 CD19 The goal is to provide standardization of monoclonal antibodies to B Cell CD20 CD22 (B cell activation marker) human antigens across laboratories. To characterize or “workshop” the antibodies, multiple laboratories carry out blind analyses of antibodies. These results independently validate antibody specificity. CD11c CD11c Dendritic Cell CD123 CD123 While the CD nomenclature has been developed for use with human antigens, it is applied to corresponding mouse antigens as well as antigens from other species. However, the mouse and other species NK Cell CD56 CD335 (NKp46) antibodies are not tested by HLDA. Human CD markers were reviewed by the HLDA. New CD markers Stem Cell/ CD34 CD34 were established at the HLDA9 meeting held in Barcelona in 2010. For Precursor hematopoetic stem cell only hematopoetic stem cell only additional information and CD markers please visit www.hcdm.org. Macrophage/ CD14 CD11b/ Mac-1 Monocyte CD33 Ly-71 (F4/80) CD66b Granulocyte CD66b Gr-1/Ly6G Ly6C CD41 CD41 CD61 (Integrin b3) CD61 Platelet CD9 CD62 CD62P (activated platelets) CD235a CD235a Erythrocyte Ter-119 CD146 MECA-32 CD106 CD146 Endothelial Cell CD31 CD62E (activated endothelial cells) Epithelial Cell CD236 CD326 (EPCAM1) For Research Use Only. -

Viewed Under 23 (B) Or 203 (C) fi M M Male Cko Mice, and Largely Unaffected Magni Cation; Scale Bars, 500 M (B) and 50 M (C)
BRIEF COMMUNICATION www.jasn.org Renal Fanconi Syndrome and Hypophosphatemic Rickets in the Absence of Xenotropic and Polytropic Retroviral Receptor in the Nephron Camille Ansermet,* Matthias B. Moor,* Gabriel Centeno,* Muriel Auberson,* † † ‡ Dorothy Zhang Hu, Roland Baron, Svetlana Nikolaeva,* Barbara Haenzi,* | Natalya Katanaeva,* Ivan Gautschi,* Vladimir Katanaev,*§ Samuel Rotman, Robert Koesters,¶ †† Laurent Schild,* Sylvain Pradervand,** Olivier Bonny,* and Dmitri Firsov* BRIEF COMMUNICATION *Department of Pharmacology and Toxicology and **Genomic Technologies Facility, University of Lausanne, Lausanne, Switzerland; †Department of Oral Medicine, Infection, and Immunity, Harvard School of Dental Medicine, Boston, Massachusetts; ‡Institute of Evolutionary Physiology and Biochemistry, St. Petersburg, Russia; §School of Biomedicine, Far Eastern Federal University, Vladivostok, Russia; |Services of Pathology and ††Nephrology, Department of Medicine, University Hospital of Lausanne, Lausanne, Switzerland; and ¶Université Pierre et Marie Curie, Paris, France ABSTRACT Tight control of extracellular and intracellular inorganic phosphate (Pi) levels is crit- leaves.4 Most recently, Legati et al. have ical to most biochemical and physiologic processes. Urinary Pi is freely filtered at the shown an association between genetic kidney glomerulus and is reabsorbed in the renal tubule by the action of the apical polymorphisms in Xpr1 and primary fa- sodium-dependent phosphate transporters, NaPi-IIa/NaPi-IIc/Pit2. However, the milial brain calcification disorder.5 How- molecular identity of the protein(s) participating in the basolateral Pi efflux remains ever, the role of XPR1 in the maintenance unknown. Evidence has suggested that xenotropic and polytropic retroviral recep- of Pi homeostasis remains unknown. Here, tor 1 (XPR1) might be involved in this process. Here, we show that conditional in- we addressed this issue in mice deficient for activation of Xpr1 in the renal tubule in mice resulted in impaired renal Pi Xpr1 in the nephron. -

Mcleod Neuroacanthocytosis Syndrome
NCBI Bookshelf. A service of the National Library of Medicine, National Institutes of Health. Pagon RA, Adam MP, Ardinger HH, et al., editors. GeneReviews® [Internet]. Seattle (WA): University of Washington, Seattle; 1993- 2017. McLeod Neuroacanthocytosis Syndrome Hans H Jung, MD Department of Neurology University Hospital Zurich Zurich, Switzerland [email protected] Adrian Danek, MD Neurologische Klinik Ludwig-Maximilians-Universität München, Germany ed.uml@kenad Ruth H Walker, MD, MBBS, PhD Department of Neurology Veterans Affairs Medical Center Bronx, New York [email protected] Beat M Frey, MD Blood Transfusion Service Swiss Red Cross Schlieren/Zürich, Switzerland [email protected] Christoph Gassner, PhD Blood Transfusion Service Swiss Red Cross Schlieren/Zürich, Switzerland [email protected] Initial Posting: December 3, 2004; Last Update: May 17, 2012. Summary Clinical characteristics. McLeod neuroacanthocytosis syndrome (designated as MLS throughout this review) is a multisystem disorder with central nervous system (CNS), neuromuscular, and hematologic manifestations in males. CNS manifestations are a neurodegenerative basal ganglia disease including (1) movement disorders, (2) cognitive alterations, and (3) psychiatric symptoms. Neuromuscular manifestations include a (mostly subclinical) sensorimotor axonopathy and muscle weakness or atrophy of different degrees. Hematologically, MLS is defined as a specific blood group phenotype (named after the first proband, Hugh McLeod) that results from absent expression of the Kx erythrocyte antigen and weakened expression of Kell blood group antigens. The hematologic manifestations are red blood cell acanthocytosis and compensated hemolysis. Allo-antibodies in the Kell and Kx blood group system can cause strong reactions to transfusions of incompatible blood and severe anemia in newborns of Kell-negative mothers. -

4-6 Weeks Old Female C57BL/6 Mice Obtained from Jackson Labs Were Used for Cell Isolation
Methods Mice: 4-6 weeks old female C57BL/6 mice obtained from Jackson labs were used for cell isolation. Female Foxp3-IRES-GFP reporter mice (1), backcrossed to B6/C57 background for 10 generations, were used for the isolation of naïve CD4 and naïve CD8 cells for the RNAseq experiments. The mice were housed in pathogen-free animal facility in the La Jolla Institute for Allergy and Immunology and were used according to protocols approved by the Institutional Animal Care and use Committee. Preparation of cells: Subsets of thymocytes were isolated by cell sorting as previously described (2), after cell surface staining using CD4 (GK1.5), CD8 (53-6.7), CD3ε (145- 2C11), CD24 (M1/69) (all from Biolegend). DP cells: CD4+CD8 int/hi; CD4 SP cells: CD4CD3 hi, CD24 int/lo; CD8 SP cells: CD8 int/hi CD4 CD3 hi, CD24 int/lo (Fig S2). Peripheral subsets were isolated after pooling spleen and lymph nodes. T cells were enriched by negative isolation using Dynabeads (Dynabeads untouched mouse T cells, 11413D, Invitrogen). After surface staining for CD4 (GK1.5), CD8 (53-6.7), CD62L (MEL-14), CD25 (PC61) and CD44 (IM7), naïve CD4+CD62L hiCD25-CD44lo and naïve CD8+CD62L hiCD25-CD44lo were obtained by sorting (BD FACS Aria). Additionally, for the RNAseq experiments, CD4 and CD8 naïve cells were isolated by sorting T cells from the Foxp3- IRES-GFP mice: CD4+CD62LhiCD25–CD44lo GFP(FOXP3)– and CD8+CD62LhiCD25– CD44lo GFP(FOXP3)– (antibodies were from Biolegend). In some cases, naïve CD4 cells were cultured in vitro under Th1 or Th2 polarizing conditions (3, 4). -
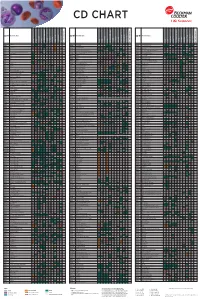
Flow Reagents Single Color Antibodies CD Chart
CD CHART CD N° Alternative Name CD N° Alternative Name CD N° Alternative Name Beckman Coulter Clone Beckman Coulter Clone Beckman Coulter Clone T Cells B Cells Granulocytes NK Cells Macrophages/Monocytes Platelets Erythrocytes Stem Cells Dendritic Cells Endothelial Cells Epithelial Cells T Cells B Cells Granulocytes NK Cells Macrophages/Monocytes Platelets Erythrocytes Stem Cells Dendritic Cells Endothelial Cells Epithelial Cells T Cells B Cells Granulocytes NK Cells Macrophages/Monocytes Platelets Erythrocytes Stem Cells Dendritic Cells Endothelial Cells Epithelial Cells CD1a T6, R4, HTA1 Act p n n p n n S l CD99 MIC2 gene product, E2 p p p CD223 LAG-3 (Lymphocyte activation gene 3) Act n Act p n CD1b R1 Act p n n p n n S CD99R restricted CD99 p p CD224 GGT (γ-glutamyl transferase) p p p p p p CD1c R7, M241 Act S n n p n n S l CD100 SEMA4D (semaphorin 4D) p Low p p p n n CD225 Leu13, interferon induced transmembrane protein 1 (IFITM1). p p p p p CD1d R3 Act S n n Low n n S Intest CD101 V7, P126 Act n p n p n n p CD226 DNAM-1, PTA-1 Act n Act Act Act n p n CD1e R2 n n n n S CD102 ICAM-2 (intercellular adhesion molecule-2) p p n p Folli p CD227 MUC1, mucin 1, episialin, PUM, PEM, EMA, DF3, H23 Act p CD2 T11; Tp50; sheep red blood cell (SRBC) receptor; LFA-2 p S n p n n l CD103 HML-1 (human mucosal lymphocytes antigen 1), integrin aE chain S n n n n n n n l CD228 Melanotransferrin (MT), p97 p p CD3 T3, CD3 complex p n n n n n n n n n l CD104 integrin b4 chain; TSP-1180 n n n n n n n p p CD229 Ly9, T-lymphocyte surface antigen p p n p n -

Immuno 2014 No. 1
Journal of Blood Group Serology and Molecular Genetics VOLUME 30, N UMBER 1, 2014 Immunohematology Journal of Blood Group Serology and Molecular Genetics Volume 30, Number 1, 2014 CONTENTS R EPORT 1 Indirect antiglobulin test-crossmatch using low-ionic-strength saline–albumin enhancement medium and reduced incubation time: effectiveness in the detection of most clinically significant antibodies and impact on blood utilization C.L. Dinardo, S.L. Bonifácio, and A. Mendrone, Jr. R EV I EW 6 Raph blood group system M. Hayes R EPORT 11 I-int phenotype among three individuals of a Parsi community from Mumbai, India S.R. Joshi C A SE R EPORT 14 Evans syndrome in a pediatric liver transplant recipient with an autoantibody with apparent specificity for the KEL4 (Kpb) antigen S.A. Koepsell, K. Burright-Hittner, and J.D. Landmark R EV I EW 18 JMH blood group system: a review S.T. Johnson R EPORT 24 Demonstration of IgG subclass (IgG1 and IgG3) in patients with positive direct antiglobulin tests A. Singh, A. Solanki, and R. Chaudhary I N M EMOR ia M 28 George Garratty, 1935–2014 Patricia A. Arndt and Regina M. Leger 30 A NNOUNCEMENTS 34 A DVERT I SEMENTS 39 I NSTRUCT I ONS FOR A UTHORS E D I TOR - I N -C H I EF E D I TOR ia L B OA RD Sandra Nance, MS, MT(ASCP)SBB Philadelphia, Pennsylvania Patricia Arndt, MT(ASCP)SBB Paul M. Ness, MD Pomona, California Baltimore, Maryland M A N AG I NG E D I TOR James P. -

3407 M16141436 19 3.Pdf
Immunohematology JOURNAL OF BLOOD GROUP SEROLOGY AND EDUCATION V OLUME 19, NUMBER 3, 2003 Immunohematology JOURNAL OF BLOOD GROUP SEROLOGY AND EDUCATION V OLUME 19, NUMBER 3, 2003 CONTENTS 73 DNA analysis for donor screening of Dombrock blood group antigens J.R. STORRY, C.M.WESTHOFF,D.CHARLES-PIERRE,M.RIOS,K.HUE-ROYE,S.VEGE,S.NANCE, AND M.E. REID 77 Studies on the Dombrock blood group system in non-human primates C. MOGOS,A.SCHAWALDER,G.R. HALVERSON, AND M.E. REID 83 Murine monoclonal antibodies can be used to type RBCs with a positive DAT G.R. HALVERSON,P.HOWARD,H.MALYSKA,E.TOSSAS, AND M.E. REID 86 Rh antigen and phenotype frequencies and probable genotypes for the four main ethnic groups in Port Harcourt, Nigeria Z.A. JEREMIAH AND F.I. BUSERI 89 Antibodies detected in samples from 21,730 pregnant women S. JOVANOVIC-SRZENTIC,M.DJOKIC,N.TIJANIC,R.DJORDJEVIC,N.RIZVAN,D.PLECAS, AND D. FILIMONOVIC 93 BOOK REVIEWS S. GERALD SANDLER,MD THERESA NESTER,MD 95 COMMUNICATIONS Letter to the Editors Letter From the Editors Irregular RBC antibodies in the Ortho Dedication sera of Brazilian pregnant women 97 IN MEMORIAM BERTIL CEDEGREN,MD 98 99 ANNOUNCEMENTS ADVERTISEMENTS 103 INSTRUCTIONS FOR AUTHORS EDITOR-IN-CHIEF MANAGING EDITOR Delores Mallory, MT(ASCP)SBB Mary H. McGinniss,AB, (ASCP)SBB Rockville, Maryland Bethesda, Maryland TECHNICAL EDITOR SENIOR MEDICAL EDITOR Christine Lomas-Francis, MSc Scott Murphy, MD New York, New York Philadelphia, Pennsylvania ASSOCIATE MEDICAL EDITORS S. Gerald Sandler, MD Geralyn Meny, MD Ralph Vassallo, MD Washington, District of Columbia Philadelphia, Pennsylvania Philadelphia, Pennsylvania EDITORIAL BOARD Patricia Arndt, MT(ASCP)SBB W. -

Supp Table 6.Pdf
Supplementary Table 6. Processes associated to the 2037 SCL candidate target genes ID Symbol Entrez Gene Name Process NM_178114 AMIGO2 adhesion molecule with Ig-like domain 2 adhesion NM_033474 ARVCF armadillo repeat gene deletes in velocardiofacial syndrome adhesion NM_027060 BTBD9 BTB (POZ) domain containing 9 adhesion NM_001039149 CD226 CD226 molecule adhesion NM_010581 CD47 CD47 molecule adhesion NM_023370 CDH23 cadherin-like 23 adhesion NM_207298 CERCAM cerebral endothelial cell adhesion molecule adhesion NM_021719 CLDN15 claudin 15 adhesion NM_009902 CLDN3 claudin 3 adhesion NM_008779 CNTN3 contactin 3 (plasmacytoma associated) adhesion NM_015734 COL5A1 collagen, type V, alpha 1 adhesion NM_007803 CTTN cortactin adhesion NM_009142 CX3CL1 chemokine (C-X3-C motif) ligand 1 adhesion NM_031174 DSCAM Down syndrome cell adhesion molecule adhesion NM_145158 EMILIN2 elastin microfibril interfacer 2 adhesion NM_001081286 FAT1 FAT tumor suppressor homolog 1 (Drosophila) adhesion NM_001080814 FAT3 FAT tumor suppressor homolog 3 (Drosophila) adhesion NM_153795 FERMT3 fermitin family homolog 3 (Drosophila) adhesion NM_010494 ICAM2 intercellular adhesion molecule 2 adhesion NM_023892 ICAM4 (includes EG:3386) intercellular adhesion molecule 4 (Landsteiner-Wiener blood group)adhesion NM_001001979 MEGF10 multiple EGF-like-domains 10 adhesion NM_172522 MEGF11 multiple EGF-like-domains 11 adhesion NM_010739 MUC13 mucin 13, cell surface associated adhesion NM_013610 NINJ1 ninjurin 1 adhesion NM_016718 NINJ2 ninjurin 2 adhesion NM_172932 NLGN3 neuroligin -

ABO, Rh and Kell) and Ncovid-19 Susceptibility – a Retrospective Observational Study
Relationship between blood group phenotypes (ABO, Rh and Kell) and nCOVID-19 susceptibility – A retrospective observational study. Sudhir Bhandari SMS Medical College and Hospitals, Jaipur, Rajasthan, India Ajeet Singh Shaktawat SMS Medical College and Hospitals, Jaipur, Rajasthan, India Amit Tak ( [email protected] ) SMS Medical College and Hospitals, Jaipur, Rajasthan, India https://orcid.org/0000-0003-2509-2311 Bhoopendra Patel Government Medical College, Barmer, Rajasthan, India Jyotsna Shukla SMS Medical College and Hospitals, Jaipur, Rajasthan, India Sanjay Singhal SMS Medical College and Hospitals, Jaipur, Rajasthan, India Kapil Gupta SMS Medical College and Hospitals, Jaipur, Rajasthan, India Jitendra Gupta SMS Medical College and Hospitals, Jaipur, Rajasthan, India Shivankan Kakkar SMS Medical College and Hospitals, Jaipur, Rajasthan, India Amitabh Dube SMS Medical College and Hospitals, Jaipur, Rajasthan, India Sunita Dia Medstar Washington Hospital Center, Washington DC 20010, USA. Mahendra Dia North Carolina State University, Raleigh, NC 27695-7609, USA. Todd C Wehner North Carolina State University, Raleigh, NC 27695-7609, USA. Research Article Keywords: ABO blood grouping, coronavirus disease, COVID-19, multinomial test Page 1/13 Posted Date: July 10th, 2020 DOI: https://doi.org/10.21203/rs.3.rs-39611/v1 License: This work is licensed under a Creative Commons Attribution 4.0 International License. Read Full License Page 2/13 Abstract Since the outbreak of coronavirus disease-19 research has been continued to explore multiple facets of the disease. The objective of the present study is to evaluate the relationship between blood group phenotypes and COVID-19 susceptibility. In this hospital based, retrospective observational study 132 COVID-19 patients were enrolled from SMS Medical College and attached Hospitals, Jaipur, India after the proper approval from the institutional ethics committee. -

Red Blood Cell Antigen Genotyping
Red Blood Cell Antigen Genotyping Testing is useful in determining allelic variants predicting red blood cell (RBC) antigen phenotypes for patients with recent history of transfusion or with conflicting serological antibody results due to partial, variant, or weak expression antigens. Also Tests to Consider useful as an aid in management of hemolytic disease of the fetus and newborn (HDFN). Typical Testing Strategy Disease Overview Phenotype Testing Evaluates specific RBC antigen presence by serology Prevalence and/or Incidence Results can aid in selecting antigen negative RBC units Erythrocyte alloimmunization occurs in up to 58% of sickle cell patients, up to 35% in other transfusion-dependent patients, and in approximately 0.8% of all pregnant Antigen Testing, RBC Phenotype women. Extended 0013020 Method: Hemagglutination Serological testing includes K, Fya, Fyb, Jka, Symptoms Jkb, S, s (k, cellano, testing performed if indicated) to assess maternal or paternal RBC Transfusion reactions or HDFN can occur due to alloimmunization: phenotype status. Antigen Testing, Rh Phenotype 0013019 Intravascular hemolysis: hemoglobinuria, jaundice, shock Extravascular hemolysis: fever and chills Method: Hemagglutination HDFN: fetal hemolytic anemia, hepatosplenomegaly, jaundice, erythroblastosis, Antigen testing for D, C, E, c, and e to assess neurological damage, hydrops fetalis maternal, paternal, or newborn Rh phenotype status Clinical presentation is variable and dependent upon the specific antibody and recipient factors Genotype Testing May help -

Mirepoix LLC on Behalf of Caris Life Sciences, June 22, 2020 No Revisions to These Recommendations
0211U Oncology (pan-tumor), DNA and RNA by next generation sequencing, utilizing formalin-fixed paraffin-embedded tissue, interpretative report for single nucleotide variants, copy number alterations, tumor mutational burden, and microsatellite instability, with therapy association Submitted by Joel de Jesus, Mirepoix LLC on behalf of Caris Life Sciences, June 22, 2020 No revisions to these recommendations 0211U: MI Cancer Seek™ - NGS analysis C. Public Comment Rationale • Recommendation to crosswalk 0211U MI Cancer Seek is a combined whole transcriptome AND whole exome to 0019U (NLA=$3675.00) + 0036U sequencing test that is equivalent to (NLA=$4780.00) performing both: • 0019U: Oncology, RNA, gene expression • 1x multiplier for each by whole transcriptome sequencing, formalin-fixed paraffin-embedded tissue • Recommendation of an NLA equal to or fresh frozen tissue, predictive $8455 for 0211U algorithm reported as potential targets for therapeutic agents • 0036U: Exome (ie, somatic mutations), paired formalin-fixed paraffin-embedded tumor tissue and normal specimen, sequence analyses Submitted by Joel de Jesus, Mirepoix LLC on behalf of Caris Life Sciences, June 22, 2020 No revisions to these recommendations 0211U: MI Cancer Seek™ - NGS analysis C. 0019U* 0211U 0036U** Assay type Whole Whole Whole Whole Transcriptome Transcriptome Exome Exome Sequencing Sequencing Sequencing Sequencing Platform NGS NGS (Illumina) NGS (Illumina) RNASeq RNASeq & DNASeq DNASeq Samples tested FFPE & frozen tumor tissue FFPE tumor tissue FFPE tumor tissue -

Copyrighted Material
P1: SFK/UKS P2: SFK/UKS QC: SFK/UKS T1: SFK Color: 1C ind BLBK321-Paidas September 7, 2010 15:9 Trim: 244mm X 172mm Index Note: Italicized f and t refer to figures and tables, respectably. Abciximab, 207 anti-A, 29 ABO blood group, 28–9 anti-B, 29 ABO hemolytic disease, 29 anti-c, 28 acetaminophen, 45 anticoagulant therapy, 111–43 acidosis, 197 antiplatelet agents, 141 acquired thrombophilia, 68–74. See also low molecular weight heparin, 127–30, inherited thrombophilia 140–41 diagnosis of, 68, 72t for mechanical heart valve incidence of, 68 thromboprophylaxis, 138–43 obstetrical complications, 73 unfractionated heparin, 127, 140–41 pathogenecity, 71 for venous thromboembolism, 111–18 pathophysiology of, 71 for venous thromboembolism in pregnancy, activated partial thromboplastin time (aPTT), 118–36 127, 173 vitamin K antagonists, 139–40 activated protein C (APC), 6, 74–9, 191 anti-D immunoglobulin, 33 activated recombinant factor VII (rFVIIa), 165 antenatal, 33 activation markers, 7 dose regime, 35 acute fatty liver of pregnancy (AFLP), 187 indications for RhD-negative mothers, 35 acute leukemia, 20 antifibrinolytic drugs, 202 ADAMST13 deficiency, 44 anti-Kell, 28 adenosine diphosphate (ADP), 60, 61–2 f antiphospholipid antibody syndrome (APAS), adherent placenta, 169–70 68–74 alpha-delta storage pool deficiency, 165 clinical consequences, 72–3 Alport syndrome, 60 diagnosis of, 68, 72t amegakaryocytic thrombocytopenia, 60 incidence of, 68 amniotic fluid embolism (AFE), 184–5 obstetrical complications, 73 anaphylaxis, 211 pathogenicity, 71 anemia,