Study of Brachial Plexus with Regards to Its Formation, Branching Pattern and Variations and Possible Clinical Implications of Those Variations
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Bilateral Presence of a Variant Subscapularis Muscle
CASE REPORT Bilateral presence of a variant subscapularis muscle Krause DA and Youdas JW Krause DA, Youdas JW. Bilateral presence of a variant subscapularis the lateral subscapularis inserting into the proximal humerus with the tendon of muscle. Int J Anat Var. 2017;10(4):79-80. the subscapularis. The axillary and lower subscapular nerves coursed between the observed muscle and the subscapularis. The presence of the muscle has potential ABSTRACT to entrap the axillary nerve and the lower subscapular nerve. We describe the presence of an accessory subscapularis muscle observed bilaterally Key Words: Accessory subscapularis; Axillary nerve; Lower subscapular nerve; in a human anatomy laboratory. The muscle originated from the mid-region of Entrapment INTRODUCTION everal anatomic variations in axillary musculature have been reported (1- S4). One of the more common variations is the axillary arch muscle, also known as Langer’s muscle, the axillopectoral muscle, and the pectordorsal muscle (3,4). This muscle typically arises from the lateral aspect of the latissimus dorsi inserting deep to the pectoralis major on the humerus. Several variations of the axillary arch muscle are described with a reported incidence of 6-9% (4-6). Less frequent and distinctly different than the axillary arch muscle, is a variant muscle associated with the subscapularis. This has been termed the subscapulo-humeral muscle, subscapularis minor, subscapularis-teres-latissimus muscle, and the accessory subcapularis muscle (1,2,7). Reported incidence ranges from 0.45 to 2.6% (2,7). CASE REPORT A variant muscle associated with the subscapularis bilaterally was observed on a Caucasian female embalmed cadaver during routine dissection in a human anatomy class for first year physical therapy students. -
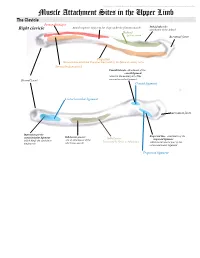
Muscle Attachment Sites in the Upper Limb
This document was created by Alex Yartsev ([email protected]); if I have used your data or images and forgot to reference you, please email me. Muscle Attachment Sites in the Upper Limb The Clavicle Pectoralis major Smooth superior surface of the shaft, under the platysma muscle Deltoid tubercle: Right clavicle attachment of the deltoid Deltoid Axillary nerve Acromial facet Trapezius Sternocleidomastoid and Trapezius innervated by the Spinal Accessory nerve Sternocleidomastoid Conoid tubercle, attachment of the conoid ligament which is the medial part of the Sternal facet coracoclavicular ligament Conoid ligament Costoclavicular ligament Acromial facet Impression for the Trapezoid line, attachment of the costoclavicular ligament Subclavian groove: Subclavius trapezoid ligament which binds the clavicle to site of attachment of the Innervated by Nerve to Subclavius which is the lateral part of the the first rib subclavius muscle coracoclavicular ligament Trapezoid ligament This document was created by Alex Yartsev ([email protected]); if I have used your data or images and forgot to reference you, please email me. The Scapula Trapezius Right scapula: posterior Levator scapulae Supraspinatus Deltoid Deltoid and Teres Minor are innervated by the Axillary nerve Rhomboid minor Levator Scapulae, Rhomboid minor and Rhomboid Major are innervated by the Dorsal Scapular Nerve Supraspinatus and Infraspinatus innervated by the Suprascapular nerve Infraspinatus Long head of triceps Rhomboid major Teres Minor Teres Major Teres Major -

Examination of the Shoulder Bruce S
Examination of the Shoulder Bruce S. Wolock, MD Towson Orthopaedic Associates 3 Joints, 1 Articulation 1. Sternoclavicular 2. Acromioclavicular 3. Glenohumeral 4. Scapulothoracic AC Separation Bony Landmarks 1. Suprasternal notch 2. Sternoclavicular joint 3. Coracoid 4. Acromioclavicular joint 5. Acromion 6. Greater tuberosity of the humerus 7. Bicipital groove 8. Scapular spine 9. Scapular borders-vertebral and lateral Sternoclavicular Dislocation Soft Tissues 1. Rotator Cuff 2. Subacromial bursa 3. Axilla 4. Muscles: a. Sternocleidomastoid b. Pectoralis major c. Biceps d. Deltoid Congenital Absence of Pectoralis Major Pectoralis Major Rupture Soft Tissues (con’t) e. Trapezius f. Rhomboid major and minor g. Latissimus dorsi h. Serratus anterior Range of Motion: Active and Passive 1. Abduction - 90 degrees 2. Adduction - 45 degrees 3. Extension - 45 degrees 4. Flexion - 180 degrees 5. Internal rotation – 90 degrees 6. External rotation – 45 degrees Muscle Testing 1. Flexion a. Primary - Anterior deltoid (axillary nerve, C5) - Coracobrachialis (musculocutaneous nerve, C5/6 b. Secondary - Pectoralis major - Biceps Biceps Rupture- Longhead Muscle Testing 2. Extension a. Primary - Latissimus dorsi (thoracodorsal nerve, C6/8) - Teres major (lower subscapular nerve, C5/6) - Posterior deltoid (axillary nerve, C5/6) b. Secondary - Teres minor - Triceps Abduction Primary a. Middle deltoid (axillary nerve, C5/6) b. Supraspinatus (suprascapular nerve, C5/6) Secondary a. Anterior and posterior deltoid b. Serratus anterior Deltoid Ruputure Axillary Nerve Palsy Adduction Primary a. Pectoralis major (medial and lateral pectoral nerves, C5-T1 b. Latissimus dorsi (thoracodorsal nerve, C6/8) Secondary a. Teres major b. Anterior deltoid External Rotation Primary a. Infraspinatus (suprascapular nerve, C5/6) b. Teres minor (axillary nerve, C5) Secondary a. -

Brachial Plexus Posterior Cord Variability: a Case Report and Review
CASE REPORT Brachial plexus posterior cord variability: a case report and review Edward O, Arachchi A, Christopher B Edward O, Arachchi A, Christopher B. Brachial plexus posterior cord anatomical variability. This case report details the anatomical variants discovered variability: a case report and review. Int J Anat Var. 2017;10(3):49-50. in the posterior cord of the brachial plexus in a routine cadaveric dissection at the University of Melbourne, Australia. Similar findings in the literature are reviewed ABSTRACT and the clinical significance of these findings is discussed. The formation and distribution of the brachial plexus is a source of great Key Words: Brachial plexus; Posterior cord; Axillary nerve; Anatomical variation INTRODUCTION he brachial plexus is the neural network that supplies motor and sensory Tinnervation to the upper limb. It is typically composed of anterior rami from C5 to T1 spinal segments, which subsequently unite to form superior, middle and inferior trunks. These trunks divide and reunite to form cords 1 surrounding the axillary artery, which terminate in branches of the plexus. The posterior cord is classically described as a union of the posterior divisions from the superior, middle and inferior trunks of the brachial plexus, with fibres from all five spinal segments. The upper subscapular, thoracodorsal and lower subscapular nerves propagate from the cord prior to the axillary and radial nerves forming terminal branches. Variability in the brachial plexus is frequently reported in the literature. It is C5 nerve root Suprascapular nerve important for clinicians to be aware of possible variations when considering Posterior division of C5-C6 injuries or disease of the upper limb. -

BRACHIAL PLEXUS ANATOMY, INJURIES and MANAGEMENT • Brachial Plexus Is Network of Nerves That Supply Sensation and Motor Function to Upper Extremity
BRACHIAL PLEXUS ANATOMY, INJURIES AND MANAGEMENT • Brachial plexus is network of nerves that supply sensation and motor function to upper extremity • Formed by ventral primary rami of lowest four cervical and upper most thoracic nerve ( c5-T1) Anatomy • Roots - c5 – t1 • Trunks – Upper ,middle and lower • Division- Anterior and posterior • Cords – Medial, posterior and lateral • Branches commons.wikimedia.org/wiki/File:Brachial_plexus.jpg Branches • Roots - phrenic nerve – C3,4,5 – diaphragm Long thoracic n - c5,6,7 – serratus anterior dorsal scapular n – c5 - rhomboidus , levator scapulae • Trunk - suprascapular n – c5- supraspinatus infraspinatus Branches of cord • Lateral cord lateral pectoral nerve • Medial cord medial cutaneous nerve of arm medial cutaneous nerve of forearm medial pectoral nerve • posterior cord upper and lower subscapular nerve thoraco-dorsal nerve (c6-8) • Lateral cord – musculocutaneous nerve (c5,6,7) and contribute to medial nerve • Posterior cord – axillary(c5-6) and radial nerve (c5-t1) • Medial cord – median nerve contribution and ulnar nerve (c8-T1) Roots Sensory Motor Deficits Reflex C5 Lateral border upper Deltoid Biceps arm to elbow Supraspinatus Infraspinatus Rhomboids C6 Lateral forearm Biceps supinator Thumb, index Brachioradialis Brachialis C7 Middle finger, Triceps triceps Front & back of hand Wrist flexors & Extensors Lat.dorsi,Pec major C8 Little finger Finger flexor & finger Heel of hand to above extensor wrist Flexor Carpi ulnaris T1 In the axilla All small hand none muscles Variations • Pre-fixed ( 28-62%) post-fixed ( 16-73%) http://www.msdlatinamerica.com/ebooks/HandSurgery/sid744608.html Injuries of brachial plexus • Most common cause of injury – RTA (70%) • Obstetrics • Iatrogenic – positioning , surgical trauma . • Miscellaneous - radiation , tumors ,neuritis . -

Electrodiagnosis of Brachial Plexopathies and Proximal Upper Extremity Neuropathies
Electrodiagnosis of Brachial Plexopathies and Proximal Upper Extremity Neuropathies Zachary Simmons, MD* KEYWORDS Brachial plexus Brachial plexopathy Axillary nerve Musculocutaneous nerve Suprascapular nerve Nerve conduction studies Electromyography KEY POINTS The brachial plexus provides all motor and sensory innervation of the upper extremity. The plexus is usually derived from the C5 through T1 anterior primary rami, which divide in various ways to form the upper, middle, and lower trunks; the lateral, posterior, and medial cords; and multiple terminal branches. Traction is the most common cause of brachial plexopathy, although compression, lacer- ations, ischemia, neoplasms, radiation, thoracic outlet syndrome, and neuralgic amyotro- phy may all produce brachial plexus lesions. Upper extremity mononeuropathies affecting the musculocutaneous, axillary, and supra- scapular motor nerves and the medial and lateral antebrachial cutaneous sensory nerves often occur in the context of more widespread brachial plexus damage, often from trauma or neuralgic amyotrophy but may occur in isolation. Extensive electrodiagnostic testing often is needed to properly localize lesions of the brachial plexus, frequently requiring testing of sensory nerves, which are not commonly used in the assessment of other types of lesions. INTRODUCTION Few anatomic structures are as daunting to medical students, residents, and prac- ticing physicians as the brachial plexus. Yet, detailed understanding of brachial plexus anatomy is central to electrodiagnosis because of the plexus’ role in supplying all motor and sensory innervation of the upper extremity and shoulder girdle. There also are several proximal upper extremity nerves, derived from the brachial plexus, Conflicts of Interest: None. Neuromuscular Program and ALS Center, Penn State Hershey Medical Center, Penn State College of Medicine, PA, USA * Department of Neurology, Penn State Hershey Medical Center, EC 037 30 Hope Drive, PO Box 859, Hershey, PA 17033. -

Variant Branches of Brachial Plexus - a Case Report
eISSN 1308-4038 International Journal of Anatomical Variations (2012) 5: 5–7 Case Report Variant branches of brachial plexus - a case report Published online April 8th, 2012 © http://www.ijav.org Prashant Nashiket CHAWARE Abstract Jaideo Manohar UGHADE During routine dissection of brachial plexus we observed two upper subscapular nerves. These two upper subscapular nerves, lower subscapular nerve and axillary nerve arose from posterior Sudhir Vishnupant PANDIT division of upper trunk. Posterior cord gave thoracodorsal nerve and continued as radial Gajanan Laxmanrao MASKE nerve. We also found that anterior division of middle trunk divided into two branches; anterior division-a and anterior division-b. Anterior division-a joined anterior division of upper trunk to Department of Anatomy, Shri Vasantrao Naik Government form the lateral cord. Anterior division-b joined medial root-1 of median nerve to form medial root-2 of median nerve. This medial root-2 joined with lateral root of median nerve to form Medical College, Yavatmal, Maharashtra, INDIA. median nerve. The anterior division-b carrying fibers from C7 primary ramus, contributed fibers to form medial root-2 of median nerve and then joined with the ulnar nerve. Presence of C7 root Dr. Prashant Nashiket Chaware in ulnar nerve was clearly seen in our case, which is seldom visualized in routine dissection. © Assistant Professor Int J Anat Var (IJAV). 2012; 5: 5–7. Department of Anatomy Shri Vasantrao Naik Government Medical College Yavatmal, Maharashtra 445001, INDIA. +91 7232 242456 ext. 157 [email protected] Received September 8th, 2011; accepted March 10th, 2012 Key words [posterior cord] [median nerve] [ulnar nerve] [nerve variations] Introduction trunk was much thinner than the others (Figure 1). -

Section 1 Upper Limb Anatomy 1) with Regard to the Pectoral Girdle
Section 1 Upper Limb Anatomy 1) With regard to the pectoral girdle: a) contains three joints, the sternoclavicular, the acromioclavicular and the glenohumeral b) serratus anterior, the rhomboids and subclavius attach the scapula to the axial skeleton c) pectoralis major and deltoid are the only muscular attachments between the clavicle and the upper limb d) teres major provides attachment between the axial skeleton and the girdle 2) Choose the odd muscle out as regards insertion/origin: a) supraspinatus b) subscapularis c) biceps d) teres minor e) deltoid 3) Which muscle does not insert in or next to the intertubecular groove of the upper humerus? a) pectoralis major b) pectoralis minor c) latissimus dorsi d) teres major 4) Identify the incorrect pairing for testing muscles: a) latissimus dorsi – abduct to 60° and adduct against resistance b) trapezius – shrug shoulders against resistance c) rhomboids – place hands on hips and draw elbows back and scapulae together d) serratus anterior – push with arms outstretched against a wall 5) Identify the incorrect innervation: a) subclavius – own nerve from the brachial plexus b) serratus anterior – long thoracic nerve c) clavicular head of pectoralis major – medial pectoral nerve d) latissimus dorsi – dorsal scapular nerve e) trapezius – accessory nerve 6) Which muscle does not extend from the posterior surface of the scapula to the greater tubercle of the humerus? a) teres major b) infraspinatus c) supraspinatus d) teres minor 7) With regard to action, which muscle is the odd one out? a) teres -

Unilateral Intercordal Neural Communication Coexistent with Variant Branching Pattern of Posterior Cord of Brachial Plexus
CAse reporT Unilateral intercordal neUral commUnication coexistent with variant branching pattern of posterior cord of brachial plexUs Renu Baliyan, Vandana Mehta, Jyoti Arora, Ashish Kr. Nayyar, R. K. Suri, Gaytri Rath Department of Anatomy, Vardhman Mahavir Medical College, New Delhi, India Summary: Variant branching pattern of the cords of brachial plexus coupled with erroneous communications has been an area of concern for surgeons opting to explore this region. Anaesthetic blocks and surgical approaches are the highlights of these interventions, where a keen familiarization of the anatomy of this region is mandatory. The present case description reports a unilateral variant branching pattern of the posterior cord coexistent with a neural communication between lateral and medial cords in an adult male cadaver. This intercordal neural communication between lateral and medial cords was oriented obliquely and measured 2.2 cm in length. Furthermore, the posterior cord revealed a variant branching pattern. It branched into three upper subscapular nerves and a common trunk for the thoracodorsal and lower subscapular nerves. The lowest of the three upper subscapular nerves gave a communicating twig to the thoracodorsal nerve. Inspite of uncount- able reports on variations of brachial plexus, descriptions regarding anomalous branching patterns hold enormous clinical significance for the radiologists, anesthetists and surgeons, besides being of academic interest for the anatomists. Key words: Posterior cord; Medial cord; Lateral cord; Neural communication introduction along with an intercordal neural communication between medial and lateral cords of brachial plexus. The hallmark of the axillary region is the brachial plexus, which is a plexiform arrangement of the anterior primary case report rami of the lowest 4 cervical and first thoracic spinal nerves. -

Study of Variations in the Origin and Distance of Origin of Axillary Nerve Ijcrr of the Posterior Cord of Brachial Plexus
Original Article STUDY OF VARIATIONS IN THE ORIGIN AND DISTANCE OF ORIGIN OF AXILLARY NERVE IJCRR OF THE POSTERIOR CORD OF BRACHIAL PLEXUS Santosh M. Bhosale, Nagaraj S. Mallashetty Assistant Professor, Department of Anatomy, S.S.I.M.S & R.C, Davangere-577004, Karnataka, India. ABSTRACT Background: Variations in the origin of axillary nerve from the posterior cord of brachial plexus and its distance of origin from mid clavicular point are important during surgical approaches to the axilla and upper arm, administration of anesthetic blocks, interpreting effects of nervous compressions and in repair of plexus injuries. The patterns of branching show population differ- ences. Data from the South indian population is scarce. Objective: To describe the variations in the origin of the axillary nerve from the posterior cord of brachial plexus and its distance of origin from mid- clavicular point in the South Indian population. Materials and methods: Forty brachial plexuses from twenty formalin fixed cadavers were explored by gross dissection. Origin and order of branching of axillary nerve and its distance of origin from mid- clavicualr point was recorded. Representative pho- tographs were then taken using a digital camera (Sony Cybershot R, W200, 7.2 Megapixels). Results: In forty specimens studied, 87.5% of axillary nerve originated from the posterior cord of brachial plexus and in 12.5% of specimens axillary nerve took origin from common trunk along with thoracodorsal or lower subscapular nerve or both. In 32.5% of the specimens axillary nerve had origin from posterior cord of brachial plexus at a distance of 4.6-5.0cm from mid-clavicular point. -

The Brachial Plexus the Brachial Plexus
The brachial plexus The brachial plexus Formation Supraclavicular portion Trunks Divisions Infraclavicular portion Cords Branches The brachial plexus The brachial plexus is a network of nerves that supply the upper limb The brachial plexus extends from the neck into the axilla Formation It is formed by five roots from the anterior (ventral) primary rami of C5,6,7,8, and T1 Formation the roots of the brachial plexus should not be confused with The ventral dorsal & the ventral and dorsal rami form ventral roots of the roots of a spinal n. roots which unite to the brachial plexus form the spinal nerves Supraclavicular portion Scalenus medius The roots lie in the neck between scalenus anterior and scalenus medius Scalenus anterior muscles Supraclavicular portion C5 & C6 unite to form the upper trunk Supraclavicular portion C8 & T1 unite to form the lower trunk Supraclavicular portion C7 continues as the middle trunk Trunks of the brachial plexus The trunks lie in the posterior triangle of the neck and can be felt in the angle between the clavicle and sternocleidomastoid muscle clavicle Trunks of the brachial plexus The inferior trunk lies on the first rib posterior to the subclavian artery Inferior trunk Divisions of the brachial plexus Behind the clavicle, each trunk divides into anterior and posterior divisions Trunks of the brachial plexus the anterior divisions supply anterior (flexor) parts while the posterior divisions supply posterior (extensor) parts of the upper limb Infraclavicular portion The three posterior divisions unite to form the posterior Posterior cord cord Infraclavicular portion the anterior divisions of the upper and lateral cord middle trunks unite to form the lateral cord Infraclavicular portion the anterior division of the lower trunk continues as the medial cord medial cord Cords of the brachial plexus The cords are arranged around the second part of the axillary artery as indicated by their names. -

Scalene Entrapment Syndrome M CD by James 0
1:1 m m I I m Scalene entrapment syndrome m CD by James 0. Royder, DO, FAA() m ver the years, a continuing diagnostic and thera- When the Tinel's Sign and the Phalen's Test are both peutic dilemma is presented by the large number negative, one can usually rule out a mononeuropathy of 0 0 of patients who present with cervical the ulnar or radial nerve, such as Carpal Tunnel, Guyon radiculopathy without positive neurological findings and Tunnel or Tardy Ulnar Palsy syndromes. When the a negative MRI. Muscle spasms, rigidity, restriction of Scalene-cramp Test' evokes a pattern of referred pain range of motion are the presenting objective findings, down the upper extremity, it suggests entrapment of the while neck pain, headaches, light headedness. along with brachial plexus by the scalene muscles. In performing this pain and "tingling" in the shoulder, arm and hand are the test, the patient rotates the head toward the painful ex- initial subjective complaints. tremity and then pulls his chin down into the supraclav- The patient's history will usually reveal some type of icular fossa..this causes the scalene muscles on that side traumatic event preceding the onset of these symptoms. to contract and will exaggerate the referred pain if the In some cases, the symptoms develop insidiously over a scalenes are involved. period of time. A series of continuous, repetitive traumas The Scalene-relief Test' is a quick way to check to see can produce the same damage. Initially, we must rule out if the scalene muscles are involved.