Nutrition Department This Booklet Has Been Developed by the Nutrition and Gastroenterology Department’S at Alfred Health, Melbourne
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Adult Tube Feeding
Guide to ADULT TUBE FEEDING Parents’ Practical Guide to Pediatric Tube Feeding | XX Contents Introduction 3 Finding Community Support 4 Understanding the Tube Feeding System 6 Monitoring Your Response to Tube Feeding 8 Taking Charge of Your Doctor Visits 18 Tube Feeding Monitoring Checklist 20 Medication Record 28 Notes 30 Glossary 32 Guide to Adult Tube Feeding | 1 Introduction We know that tube feeding brings major changes to your life. But you don’t have to face them alone. We hope you find this guide a useful, practical resource that can help you tube feed successfully at home. You’ll find step-by-step instructions on handling issues you face every day, from coping with infections to preparing for a doctor’s appointment. The guide includes worksheets (P. 20-31) that make it simple to record important information about your progress. We’ve also added a helpful glossary (P. 32-34) that you can refer to if you come across any unfamiliar terms. While technical and medical support form the foundation of tube-feeding success, we believe that emotional support is just as important. Hopefully, you’ll find resources in this guide that make your journey easier. Guide to Adult Tube Feeding | 3 Finding Community Support With support and guidance, you can take control of the tube-feeding process and adjust successfully to this new lifestyle change. Visit the link below to find educational resources, support groups and the opportunity to connect with others in your situation. The Oley Foundation The Oley Foundation is a nonprofit organization for people who depend on home enteral (tube) feeding or parenteral (intravenous) feeding. -

JEJUNOSTOMY Feeding Tube PASSPORT (JEJ)
Hull University Teaching Hospitals NHS Trust JEJUNOSTOMY Feeding Tube PASSPORT (JEJ) Tube INFORMATION ABOUT MY JEJUNOSTOMY FEEDING TUBE Affix Addressograph Has a tube How inserted? Site of bowel insertion: e.g. Jejunum, Terminal Ileum (Circle) Date inserted: Skin Suture Removal Date Yes / No Weekly Balloon change (If required) Abdominal measurement (If required) cm Type of feed: Continuous/mls per hour mls Flush with of sterile water pre & post feed & medication. 30mls Additional flushes can be given as indicated by your dietitian. Long term plan If during the first 7 days following your tube insertion, you notice any leak of fluid around the tube, pain on feeding, flushing or if there is fresh bleeding, STOP the feed immediately and contact Ward 14 Castle Hill Hospital - see contact numbers on page 16 2 CONTENTS Page Going home with a jejunostomy tube 4 What is a feeding jejunostomy tube 4 How long will I need it? 5 Surgically placed jejunostomy tube with stitches 5 & 6 Jejunostomy tube with balloon 6 General care / stoma care 7 Flushing 8 Pump feeding/Key Points 9 My Feed regime 10 & 11 Tube blockage 12 Tube fallen out 12 Mouth care 13 Medicine 13 Feed storage and disposal 13 Training prior to going home 14 Going home 14 Equipment for discharge 15 When discharged from hospital 15 Contact numbers between 9am-5pm 16 Emergency contact details after 5pm 16 This booklet contains useful information and advice for patients leaving hospital with a Jejunostomy feeding tube. How it works and how to maintain it. It also lists specific interventions of what to do should you encounter any problems. -

Tube Feeding Protocol: Supporting an Individual with a Feeding Tube
Tube Feeding Protocol: Supporting an Individual with a Feeding Tube Introduction Some people may be unable to take foods or fluids by mouth due to dysphagia. Others may require supplementation because they are unable to take sufficient foods or fluids by mouth, and formula delivered through a feeding tube may provide them with much needed additional nutrients. It is helpful if guidelines (A Tube Feeding Protocol) are in place prior to the need for this intervention. Below are some suggested guidelines for supporting an Individual with a feeding tube. Information to be documented by the physician The reason (medical diagnosis) requiring feeding tube insertion Type of feeding tube inserted Types of feeding tubes The Nasogastric Tube (NG tube): Passed into either nostril, down the esophagus and into the stomach. This is used for short term feedings. The Gastrostomy tube (G - tube or PEG): Surgically placed through the abdominal wall into the stomach. The tube will be located below the rib cage and to the left. The Jejunostomy tube (J - tube or PEJ): Surgically implanted in the upper portion of the jejunum (Part of the small intestine.) The tube will be located lower in the abdomen and more toward the center than the G – tube. Feedings through a J – tube must always be by pump. The Gastrostomy-Jejunostomy (GJ - tube): Surgically placed in the stomach, like the G – tube, but the tubing is longer, the end is in the jejunum, and there are two ports. Feeding technique Feeding techniques Bolus: A set amount of formula is given over a short period of time via syringe. -
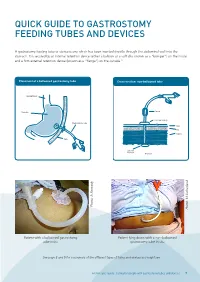
Quick Guide to Gastrostomy Feeding Tubes and Devices
QUICK GUIDE TO GASTROSTOMY FEEDING TUBES AND DEVICES A gastrostomy feeding tube or device is one which has been inserted directly through the abdominal wall into the stomach. It is secured by an internal retention device (either a balloon or a soft disc known as a “bumper”) on the inside and a firm external retention device (known as a “flange”) on the outside.11 Placement of a ballooned gastrostomy tube Cross-section: non-ballooned tube Oesophagus Stomach Clamp External Flange Gastrostomy tube Skin Fat Muscle Skin Internal Bumper Stomach Photo: APhoto: Kennedy Photo: MPhoto: Sutherland Patient with a ballooned gastrostomy Patient lying down with a non-ballooned tube insitu gastrostomy tube in situ See page 8 and 9 for a summary of the different types of tubes and devices you might see. A Clinician’s Guide: Caring for people with gastrostomy tubes and devices 7 Common features of gastrostomy feeding tubes and devices include, but are not limited to: Refer to manufacturer’s guidelines for advice on brand specific tube and device features Ballooned Gastrostomy Tube Ballooned Gastrostomy Tube With side port Without side port Feeding Port Feeding Port (Enteral Dispenser (Enteral Dispenser and Feed Bag and Feed Bag connect here) connect here) ml/cc Balloon Port Balloon Port ml/cc Side Port (X ml/cc) (X ml/cc) French (size) [For example:16/18/20] French (size) [For example:16/18/20] FR FR cm markings cm markings External External Flange Flange Balloon Balloon Non-ballooned Gastrostomy Tube Non-ballooned Gastrostomy Tube with collapsible internal -

Mic Gastrostomy Feeding Tubes Care Booklet.Pdf
GASTROSTOMY CARE GUIDE GASTROSTOMY CARE GUIDE Universal INDICATIONS FOR Adapter TUBE FEEDING Medication PATIENT INFORMATION Complete nutrition supports Port development, growth, and heal- ing. If the ability to eat or Replaceable Date of tube insertion swallow is lost, or the patient is unable to tolerate food, enteral Feeding feeding can sustain life, nour- Patient name Phone ish, and even increase body Adapter weight. Tube feeding is also Physician Phone used to supplement a deficient food and fluid intake. The feed- Type 0100 0110 0150 0160 (circle one) Fr Size ing procedure can be managed safely and economically at Manufacturer's lot number (printed on package) home, away from the hospital setting. A surgical gastrostomy Mark above the SECUR-LOK® Ring in cm provides access to the stomach if long term nutritional support (this means the mark after the initial placement) is necessary. Balloon volume if 0100, or 0110 type G Tube Pure medical grade silicone (the volume should be between 7 and 10 cc) construction makes MIC Feeding Tubes durable, yet soft and comfortable to wear. They SECUR-LOK® Formula are also translucent, allowing Ring visualization of the inside of Brand name the tube above the skin line. All MIC Enteral Feeding Tubes Method of delivery are latex free. Volume, rate and time the feeding should take MIC PEG Total amount of daily water PEG stands for Percutan- eous (through the skin) Additional ingredients Endoscopic (use of a flexible lighted tube to visualize tube Irrigate the tube with water before and after feeding and medication placement) Gastrostomy administration. (surgical opening into the stomach). -

2Nd Quarter 2001 Medicare Part a Bulletin
In This Issue... From the Intermediary Medical Director Medical Review Progressive Corrective Action ......................................................................... 3 General Information Medical Review Process Revision to Medical Record Requests ................................................ 5 General Coverage New CLIA Waived Tests ............................................................................................................. 8 Outpatient Hospital Services Correction to the Outpatient Services Fee Schedule ................................................................. 9 Skilled Nursing Facility Services Fee Schedule and Consolidated Billing for Skilled Nursing Facility (SNF) Services ............. 12 Fraud and Abuse Justice Recovers Record $1.5 Billion in Fraud Payments - Highest Ever for One Year Period ........................................................................................... 20 Bulletin Medical Policies Use of the American Medical Association’s (AMA’s) Current Procedural Terminology (CPT) Codes on Contractors’ Web Sites ................................................................................. 21 Outpatient Prospective Payment System January 2001 Update: Coding Information for Hospital Outpatient Prospective Payment System (OPPS) ......................................................................................................................... 93 he Medicare A Bulletin Providers Will Be Asked to Register Tshould be shared with all to Receive Medicare Bulletins and health care -

Expert Mark H
Ask the expert Mark H. DeLegge, Enteral nutrition MD, FASGE 1. Q: How do you code for percutaneous endoscopic jejunostomy (PEJ)? A: For direct (D) PEJ, I use code 44372, with a Relative Value Unit (RVU) of 6.72. Ask the expert features questions submitted 2. Q: In the severely ill patient, is there any role for amino acid supplementation? by members, with A: Arginine and glutamine are two very important amino acids for the critically ill patient, who is often in the intensive care unit (ICU) on a ventilator. Arginine is a conditionally essential amino acid, meaning answers provided by that in critical situations, it should be supplemented. Multiple studies have determined that arginine is an ASGE physician experts. immuno-enhancing supplement that has been shown to improve rates of morbidity and mortality and days ASGE’s Publications on a ventilator in an ICU in some very ill patients. There have been concerns about the use of arginine in septic patients, because arginine is metabolized to nitrous oxide – a vasodilator. However, these concerns Committee identifies are unfounded. authors and topics for Glutamine is an immune-stimulating amino acid that is also trophic for the small bowel mucosa. Although oral the column. In this or enteral administration of glutamine has not been shown to improve clinical outcomes in critically ill patients, issue, Mark H. DeLegge, intravenous administration of glutamine has been shown to be beneficial. Intravenous glutamine is currently available internationally but not in the United States. Therefore, oral arginine supplementation or use of an MD, FASGE, responds arginine-fortified enteral formula should be considered in critically ill patients. -

MIC & ENTRAL G-Tube Patient Booklet
MIC* & ENTRAL* Gastrostomy Tubes MIC* Gastrostomy tube MIC* Bolus Gastrostomy tube ENTRAL* Gastrostomy tube PATIENT BOOKLET MIC* G-TUBE, MIC* BOLUS G-TUBE, ENTRAL* G-TUBE PATIENT BOOKLET CONTENTS YOUR AVANOS* GASTROSTOMY TUBE INFORMATION 3 INTRODUCTION 4 WHAT IS YOUR TUBE FOR? 5 ABOUT YOUR G-TUBE 5 INITIAL PLACEMENT FIRST 72 HOURS CARE 7 DAILY CARE 7 WHEN THE STOMA IS HEALED 7 WEEKLY ROUTINE 8 BEFORE FEEDING BEGINS 9 ADMINISTRATION OF TUBE FEEDS 10 ADMINISTRATION OF MEDICATION 10 FLUSHING YOUR TUBE 10 REPLACEMENT AND ACCIDENTAL REMOVAL 11 PROBLEM SOLVING 12 CHILDREN’S SPECIAL CONCERNS 13 TERMS YOU’LL NEED TO KNOW 13 SOME G-TUBE PEG DO’S AND DON’TS 14 2 YOUR AVANOS* GASTROSTOMY TUBE INFORMATION PATIENT NAME OR ID __________________________________________________________________ NURSE ______________________________________________________________________________ DIETITIAN ____________________________________________________________________________ GENERAL PRACTITIONER _______________________________________________________________ * GASTROSTOMY TYPE MIC G-TUBE O FR SIZE: _____________ * MIC BOLUS G-TUBE O * ENTRAL G-TUBE O DATE OF INSERTION ___________________________________________________________________ CM MARKING AT SKIN LEVEL _____________________ CM BALLOON FILL VOLUME ________________________________________________________________ REPLACEMENT DATE ___________________________________________________________________ NAME AND TYPE OF TUBE FEED __________________________________________________________ AMOUNT OF FEED ______________________________ -

Your Guide to Home Tube Feeding
w .com Provided by YOUR GUIDE TO Home Tube Feeding visit mytubefeeding.com Your Healthcare Resources The resource people listed below will help you with questions about your home tube feeding program. Physician .................................................................................... Nurse .......................................................................................... Address ....................................................................................... Address ....................................................................................... Phone .......................................................................................... Phone .......................................................................................... 2 Email ............................................................................................ Email ............................................................................................ Registered Dietitian .............................................................. Supply Source .......................................................................... Address ....................................................................................... Address ....................................................................................... Phone .......................................................................................... Phone .......................................................................................... Email ........................................................................................... -

Alteration in Periodontal Pathogens and Periodontal Status in Patients with Nasogastric Tube Feeding- a Clinical and Microbiological Study
Original Research Article http://doi.org/10.18231/j.ijpi.2020.005 Alteration in periodontal pathogens and periodontal status in patients with nasogastric tube feeding- A clinical and microbiological study Jaisika Rajpal1*, Aakash Arora2, Prerna Arora3, Ruchika Prasad4 1,3,4Senior Consultant, 2Reader, 1Private Practitioner, Ghaziabad, Uttar Pradesh, 2Dept. of Oral and Maxillofacial Surgery, 2Shree Bankey Bihari Dental College and Research Centre, Ghaziabad, Uttar Pradesh, 3Private Practitioner, Lucknow, Uttar Pradesh, 4Private Practitioner, Delhi, India *Corresponding Author: Jaisika Rajpal Email: [email protected] Abstract Introduction: The oral indigenous microbiota exists in a state of balance with the host, but the long-term use of tube feeding alters the intraoral conditions in general and periodontal microbiota in particular. The aim of this study was to examine the impact of nasogastric tube feeding on the periodontal microbiota and to explore the periodontal status in patients with nasogastric tube feeding. Method-In this study, the plaque microbiota of subjects fed enterally was compared comprehensively with that of subjects fed orally to characterize the oral indigenous microbiota of tube-fed patients. Thirty patients with nasogastric tube feeding (test group) and thirty patients fed orally (control group) were recruited for the study. Periodontal health status was assessed by plaque index and gingival bleeding by using William’s periodontal probe. Microbiological evaluation was done by quantitative cultures of dental plaque 7 days after nasogastric tube insertion. In controls, cultures of plaque and buccal mucosa were done after 7 days of hospitalization. Results: A high prevalence of potentially pathogenic isolations was found in tuboenterally fed patients in Group I as compared to Group II along with increased bleeding sites and plaque index. -

Tube Feeding: a Guide Fordirect Support Workers
Tube Feeding: A guide for direct support workers Updated September 2007 Acknowledgements: Tube Feeding: A guide for direct support workers caring for people with a disability in supported accommodation who require tube feeding, was developed by the Disability Services Division of the Department of Human Services. Main contributors to the guide are: Sue Gebert Dietitian, Disability Services. Sue Milner Statewide Advisor, Nutrition and Dietetics, Disability Services. Thank you to the following people in Eastern Metropolitan Region involved in the initial development of the guide: Julie Carpenter, Looi Chong, Lisian Choo, Hilary Gillen, Rosa Harlond, and Monica White. Thank you to the following dietitians involved in the development of the guide: Chadia Bastin, Megan Murray, and Kerryn O’Brien. Published by Disability Services Division Victorian Government Department of Human Services Melbourne Victoria Australia March 2005 Updated September 2007 © Copyright State of Victoria, Department of Human Services, 2005. This publication is copyright. No part may be reproduced by any process except in accordance with the provisions of the Copyright Act 1968. ISBN 0731162161 Also published on www.dhs.vic.gov.au Authorised by the Victorian Government, 50 Lonsdale Street, Melbourne. Tube Feeding: A Guide for Direct Support Workers 1 Contents 1. Introduction 3 2. Glossary 4 3. Checklist for establishing tube feeding in supported accommodation 5 4. When is tube feeding necessary? 6 5. What is tube feeding? 6 6. Process of deciding when tube feeding is needed 6 7. Types of tubes 7 8. Putting in the tube 7 9. Methods of giving tube feeds 8 10. Where do you get formula and equipment for tube feeds? 8 11. -

What Is an Enteral Feeding Tube?
Your Feeding Tubes Feeding Your What Is an Enteral Feeding Tube? Enteral refers to within the digestive system or intestine. Enteral feeding tubes allow liquid food to enter your stomach or intestine through a tube. The soft, flexible tube enters a surgically created opening in the abdominal wall called an ostomy. An enterostomy tube in the stomach is called a gastrostomy. A tube in the small intestine is called a jejunostomy. The site on the abdomen where the tube is inserted is called a stoma. The location of the stoma depends on your specific operation and the shape of your abdomen. Most stomas: f Lie flat against your body f Are round in shape f Are red and moist (similar to the inside of your mouth) f Have no feeling Gastrostomy feeding tube Stoma tract Surgical Patient Education 112830_BODY.indd 1 8/21/15 9:25 AM 3 Who Needs an Enteral Feeding Tube? Cancer, trauma, nervous system and digestive system disorders, and congenital birth defects can cause difficulty in feeding. Some people also have difficulty swallowing, which increases the chance that they will breathe in food (aspirate). People who have difficulties feeding can benefit from a feeding tube. Your doctor will explain to you the specific reasons why you or your family member need a feeding tube. For some, a feeding tube is a new way of life, but for others, the tube is temporary and used until the problem can be treated or repaired. Low-profile feeding tube American College of Surgeons • Division of Education 112830_BODY.indd 2 8/21/15 9:25 AM 2 Your Feeding Tubes Feeding Your Understanding Your Digestive System When food enters your oral cavity (mouth), the lips and tongue move it toward the back of the throat.