Tube Feeding Troubleshooting Guide
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Adult Tube Feeding
Guide to ADULT TUBE FEEDING Parents’ Practical Guide to Pediatric Tube Feeding | XX Contents Introduction 3 Finding Community Support 4 Understanding the Tube Feeding System 6 Monitoring Your Response to Tube Feeding 8 Taking Charge of Your Doctor Visits 18 Tube Feeding Monitoring Checklist 20 Medication Record 28 Notes 30 Glossary 32 Guide to Adult Tube Feeding | 1 Introduction We know that tube feeding brings major changes to your life. But you don’t have to face them alone. We hope you find this guide a useful, practical resource that can help you tube feed successfully at home. You’ll find step-by-step instructions on handling issues you face every day, from coping with infections to preparing for a doctor’s appointment. The guide includes worksheets (P. 20-31) that make it simple to record important information about your progress. We’ve also added a helpful glossary (P. 32-34) that you can refer to if you come across any unfamiliar terms. While technical and medical support form the foundation of tube-feeding success, we believe that emotional support is just as important. Hopefully, you’ll find resources in this guide that make your journey easier. Guide to Adult Tube Feeding | 3 Finding Community Support With support and guidance, you can take control of the tube-feeding process and adjust successfully to this new lifestyle change. Visit the link below to find educational resources, support groups and the opportunity to connect with others in your situation. The Oley Foundation The Oley Foundation is a nonprofit organization for people who depend on home enteral (tube) feeding or parenteral (intravenous) feeding. -

General Signs and Symptoms of Abdominal Diseases
General signs and symptoms of abdominal diseases Dr. Förhécz Zsolt Semmelweis University 3rd Department of Internal Medicine Faculty of Medicine, 3rd Year 2018/2019 1st Semester • For descriptive purposes, the abdomen is divided by imaginary lines crossing at the umbilicus, forming the right upper, right lower, left upper, and left lower quadrants. • Another system divides the abdomen into nine sections. Terms for three of them are commonly used: epigastric, umbilical, and hypogastric, or suprapubic Common or Concerning Symptoms • Indigestion or anorexia • Nausea, vomiting, or hematemesis • Abdominal pain • Dysphagia and/or odynophagia • Change in bowel function • Constipation or diarrhea • Jaundice “How is your appetite?” • Anorexia, nausea, vomiting in many gastrointestinal disorders; and – also in pregnancy, – diabetic ketoacidosis, – adrenal insufficiency, – hypercalcemia, – uremia, – liver disease, – emotional states, – adverse drug reactions – Induced but without nausea in anorexia/ bulimia. • Anorexia is a loss or lack of appetite. • Some patients may not actually vomit but raise esophageal or gastric contents in the absence of nausea or retching, called regurgitation. – in esophageal narrowing from stricture or cancer; also with incompetent gastroesophageal sphincter • Ask about any vomitus or regurgitated material and inspect it yourself if possible!!!! – What color is it? – What does the vomitus smell like? – How much has there been? – Ask specifically if it contains any blood and try to determine how much? • Fecal odor – in small bowel obstruction – or gastrocolic fistula • Gastric juice is clear or mucoid. Small amounts of yellowish or greenish bile are common and have no special significance. • Brownish or blackish vomitus with a “coffee- grounds” appearance suggests blood altered by gastric acid. -

Nutrition Department This Booklet Has Been Developed by the Nutrition and Gastroenterology Department’S at Alfred Health, Melbourne
Nutrition Department This booklet has been developed by the Nutrition and Gastroenterology Department’s at Alfred Health, Melbourne. Inside you will find information on tube feeding at home CONTENTS 1. Your tube & feeding regime Tube details page 1 Feeding regime page 1 2. Important contact phone numbers page 1 3. Introduction What is tube feeding? page 2 Who receives tube feeding? page 2 4. The feeding tube Nasogastric tube page 3 Nasojejunal tube page 3 Gastrostomy tubes page 3—7 Jejunostomy tubes page 8 Trans-gastric jejunostomy tubes page 8 5. The formula Formula selection & feeding plan page 9 - 10 Formula storage & preparation page 10 6. Feeding methods Continuous OR Intermittent feeding using a pump page 11 - 12 Continuous OR Intermittent feeding using gravity drip page 13 - 14 Bolus feeding page 15 - 16 Oral feeding page 16 7. Medication Administration of medication page 17 8. Care during tube feeding Gastrostomy feeding tube care: Care immediately post tube insertion page 18 Daily tube & stoma care page 19 Jejunostomy, trans-gastric jejunostomy & PEG—J page 20 Nasogastric tube care page 20 Care of the tube feeding equipment page 21 Mouth care page 21 9. Possible problems & solutions Blocked Tube page 22 Constipation page 22 - 23 Diarrhoea page 23 - 24 Irritation, skin redness &/or oozing page 24 Leaking around tube page 24 Nausea & vomiting page 25 Reflux page 25 Tube dislodged or falls out page 25 Tube deteriorated or damaged page 25 What to do if your feeding tube has fallen out page 26 10. The Alfred Home Enteral Nutrition (HEN) program Requirements of the HEN Program page 27 The PEG/HEN Clinic page 28 Ordering formula & equipment pager 28 11. -

Diagnostic Approach to Chronic Constipation in Adults NAMIRAH JAMSHED, MD; ZONE-EN LEE, MD; and KEVIN W
Diagnostic Approach to Chronic Constipation in Adults NAMIRAH JAMSHED, MD; ZONE-EN LEE, MD; and KEVIN W. OLDEN, MD Washington Hospital Center, Washington, District of Columbia Constipation is traditionally defined as three or fewer bowel movements per week. Risk factors for constipation include female sex, older age, inactivity, low caloric intake, low-fiber diet, low income, low educational level, and taking a large number of medications. Chronic constipa- tion is classified as functional (primary) or secondary. Functional constipation can be divided into normal transit, slow transit, or outlet constipation. Possible causes of secondary chronic constipation include medication use, as well as medical conditions, such as hypothyroidism or irritable bowel syndrome. Frail older patients may present with nonspecific symptoms of constipation, such as delirium, anorexia, and functional decline. The evaluation of constipa- tion includes a history and physical examination to rule out alarm signs and symptoms. These include evidence of bleeding, unintended weight loss, iron deficiency anemia, acute onset constipation in older patients, and rectal prolapse. Patients with one or more alarm signs or symptoms require prompt evaluation. Referral to a subspecialist for additional evaluation and diagnostic testing may be warranted. (Am Fam Physician. 2011;84(3):299-306. Copyright © 2011 American Academy of Family Physicians.) ▲ Patient information: onstipation is one of the most of 1,028 young adults, 52 percent defined A patient education common chronic gastrointes- constipation as straining, 44 percent as hard handout on constipation is 1,2 available at http://family tinal disorders in adults. In a stools, 32 percent as infrequent stools, and doctor.org/037.xml. -

JEJUNOSTOMY Feeding Tube PASSPORT (JEJ)
Hull University Teaching Hospitals NHS Trust JEJUNOSTOMY Feeding Tube PASSPORT (JEJ) Tube INFORMATION ABOUT MY JEJUNOSTOMY FEEDING TUBE Affix Addressograph Has a tube How inserted? Site of bowel insertion: e.g. Jejunum, Terminal Ileum (Circle) Date inserted: Skin Suture Removal Date Yes / No Weekly Balloon change (If required) Abdominal measurement (If required) cm Type of feed: Continuous/mls per hour mls Flush with of sterile water pre & post feed & medication. 30mls Additional flushes can be given as indicated by your dietitian. Long term plan If during the first 7 days following your tube insertion, you notice any leak of fluid around the tube, pain on feeding, flushing or if there is fresh bleeding, STOP the feed immediately and contact Ward 14 Castle Hill Hospital - see contact numbers on page 16 2 CONTENTS Page Going home with a jejunostomy tube 4 What is a feeding jejunostomy tube 4 How long will I need it? 5 Surgically placed jejunostomy tube with stitches 5 & 6 Jejunostomy tube with balloon 6 General care / stoma care 7 Flushing 8 Pump feeding/Key Points 9 My Feed regime 10 & 11 Tube blockage 12 Tube fallen out 12 Mouth care 13 Medicine 13 Feed storage and disposal 13 Training prior to going home 14 Going home 14 Equipment for discharge 15 When discharged from hospital 15 Contact numbers between 9am-5pm 16 Emergency contact details after 5pm 16 This booklet contains useful information and advice for patients leaving hospital with a Jejunostomy feeding tube. How it works and how to maintain it. It also lists specific interventions of what to do should you encounter any problems. -

Tube Feeding Protocol: Supporting an Individual with a Feeding Tube
Tube Feeding Protocol: Supporting an Individual with a Feeding Tube Introduction Some people may be unable to take foods or fluids by mouth due to dysphagia. Others may require supplementation because they are unable to take sufficient foods or fluids by mouth, and formula delivered through a feeding tube may provide them with much needed additional nutrients. It is helpful if guidelines (A Tube Feeding Protocol) are in place prior to the need for this intervention. Below are some suggested guidelines for supporting an Individual with a feeding tube. Information to be documented by the physician The reason (medical diagnosis) requiring feeding tube insertion Type of feeding tube inserted Types of feeding tubes The Nasogastric Tube (NG tube): Passed into either nostril, down the esophagus and into the stomach. This is used for short term feedings. The Gastrostomy tube (G - tube or PEG): Surgically placed through the abdominal wall into the stomach. The tube will be located below the rib cage and to the left. The Jejunostomy tube (J - tube or PEJ): Surgically implanted in the upper portion of the jejunum (Part of the small intestine.) The tube will be located lower in the abdomen and more toward the center than the G – tube. Feedings through a J – tube must always be by pump. The Gastrostomy-Jejunostomy (GJ - tube): Surgically placed in the stomach, like the G – tube, but the tubing is longer, the end is in the jejunum, and there are two ports. Feeding technique Feeding techniques Bolus: A set amount of formula is given over a short period of time via syringe. -
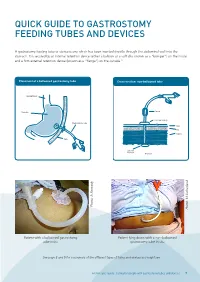
Quick Guide to Gastrostomy Feeding Tubes and Devices
QUICK GUIDE TO GASTROSTOMY FEEDING TUBES AND DEVICES A gastrostomy feeding tube or device is one which has been inserted directly through the abdominal wall into the stomach. It is secured by an internal retention device (either a balloon or a soft disc known as a “bumper”) on the inside and a firm external retention device (known as a “flange”) on the outside.11 Placement of a ballooned gastrostomy tube Cross-section: non-ballooned tube Oesophagus Stomach Clamp External Flange Gastrostomy tube Skin Fat Muscle Skin Internal Bumper Stomach Photo: APhoto: Kennedy Photo: MPhoto: Sutherland Patient with a ballooned gastrostomy Patient lying down with a non-ballooned tube insitu gastrostomy tube in situ See page 8 and 9 for a summary of the different types of tubes and devices you might see. A Clinician’s Guide: Caring for people with gastrostomy tubes and devices 7 Common features of gastrostomy feeding tubes and devices include, but are not limited to: Refer to manufacturer’s guidelines for advice on brand specific tube and device features Ballooned Gastrostomy Tube Ballooned Gastrostomy Tube With side port Without side port Feeding Port Feeding Port (Enteral Dispenser (Enteral Dispenser and Feed Bag and Feed Bag connect here) connect here) ml/cc Balloon Port Balloon Port ml/cc Side Port (X ml/cc) (X ml/cc) French (size) [For example:16/18/20] French (size) [For example:16/18/20] FR FR cm markings cm markings External External Flange Flange Balloon Balloon Non-ballooned Gastrostomy Tube Non-ballooned Gastrostomy Tube with collapsible internal -

Mic Gastrostomy Feeding Tubes Care Booklet.Pdf
GASTROSTOMY CARE GUIDE GASTROSTOMY CARE GUIDE Universal INDICATIONS FOR Adapter TUBE FEEDING Medication PATIENT INFORMATION Complete nutrition supports Port development, growth, and heal- ing. If the ability to eat or Replaceable Date of tube insertion swallow is lost, or the patient is unable to tolerate food, enteral Feeding feeding can sustain life, nour- Patient name Phone ish, and even increase body Adapter weight. Tube feeding is also Physician Phone used to supplement a deficient food and fluid intake. The feed- Type 0100 0110 0150 0160 (circle one) Fr Size ing procedure can be managed safely and economically at Manufacturer's lot number (printed on package) home, away from the hospital setting. A surgical gastrostomy Mark above the SECUR-LOK® Ring in cm provides access to the stomach if long term nutritional support (this means the mark after the initial placement) is necessary. Balloon volume if 0100, or 0110 type G Tube Pure medical grade silicone (the volume should be between 7 and 10 cc) construction makes MIC Feeding Tubes durable, yet soft and comfortable to wear. They SECUR-LOK® Formula are also translucent, allowing Ring visualization of the inside of Brand name the tube above the skin line. All MIC Enteral Feeding Tubes Method of delivery are latex free. Volume, rate and time the feeding should take MIC PEG Total amount of daily water PEG stands for Percutan- eous (through the skin) Additional ingredients Endoscopic (use of a flexible lighted tube to visualize tube Irrigate the tube with water before and after feeding and medication placement) Gastrostomy administration. (surgical opening into the stomach). -

Today's Topic: Bloating
Issue 1; August 2017 Dr. Rajiv Sharma attended medical school at Daya- nand Medical College, Punjab, India. He received his Undernourished, intelligence Internal Medicine training from Loma Linda Univer- sity, Loma Linda, California and received his Gastro- becomes like the bloated belly enterology Fellowship training from University of Rochester, Rochester, New York. Dr. Sharma trained of a starving child: swollen, under the mentorship of Dr. Richard G. Farmer, who is world renowned for his work on Inflammatory Bowel Disease. filled with nothing the body Rajiv Sharma, MD Dr. Sharma’s special interests include GERD, NERD, can use.” Inflammatory Bowel Disease (Crohn’s & Ulcerative Colitis), IBS, Acute and Chronic Pancreatitis, Gastro- intestinal Malignancies and Familial Cancer Syn- - Andrea Dworkin dromes. In an effort to share his extensive knowledge with the public, Dr. Sharma re- leased his first book, Pursuit of Gut Happiness: A Guide for Using Probiotics to Inside this issue Achieve Optimal Health, in 2014. In Dr. Sharma’s free time, he enjoys medical writing, watching movies, exercis- Differential Diagnosis 2 ing and spending time with his family. He believes in “whole person care” and the effect of mind, body and spirit on “wellness”. He has a special interest in nu- trition, exercise and healthy eating. He prides himself on being a “fact doctor” as Signs of a More Serious 2 he backs his opinions and works with solid scientific research while aiming to deliver a simple and clear message. Problem Lab Workup 2 Non-Pathological Bloating 2 Today’s Topic: Bloating Bloating may seem an odd topic to choose for our first newsletter. -

2Nd Quarter 2001 Medicare Part a Bulletin
In This Issue... From the Intermediary Medical Director Medical Review Progressive Corrective Action ......................................................................... 3 General Information Medical Review Process Revision to Medical Record Requests ................................................ 5 General Coverage New CLIA Waived Tests ............................................................................................................. 8 Outpatient Hospital Services Correction to the Outpatient Services Fee Schedule ................................................................. 9 Skilled Nursing Facility Services Fee Schedule and Consolidated Billing for Skilled Nursing Facility (SNF) Services ............. 12 Fraud and Abuse Justice Recovers Record $1.5 Billion in Fraud Payments - Highest Ever for One Year Period ........................................................................................... 20 Bulletin Medical Policies Use of the American Medical Association’s (AMA’s) Current Procedural Terminology (CPT) Codes on Contractors’ Web Sites ................................................................................. 21 Outpatient Prospective Payment System January 2001 Update: Coding Information for Hospital Outpatient Prospective Payment System (OPPS) ......................................................................................................................... 93 he Medicare A Bulletin Providers Will Be Asked to Register Tshould be shared with all to Receive Medicare Bulletins and health care -

Travelers' Diarrhea
Travelers’ Diarrhea What is it and who gets it? Travelers’ diarrhea (TD) is the most common illness affecting travelers. Each year between 20%-50% of international travelers, an estimated 10 million persons, develop diarrhea. The onset of TD usually occurs within the first week of travel but may occur at any time while traveling and even after returning home. The primary source of infection is ingestion of fecally contaminated food or water. You can get TD whenever you travel from countries with a high level of hygiene to countries that have a low level of hygiene. Poor sanitation, the presence of stool in the environment, and the absence of safe restaurant practices lead to widespread risk of diarrhea from eating a wide variety of foods in restaurants, and elsewhere. Your destination is the most important determinant of risk. Developing countries in Latin America, Africa, the Middle East, and Asia are considered high risk. Most countries in Southern Europe and a few Caribbean islands are deemed intermediate risk. Low risk areas include the United States, Canada, Northern Europe, Australia, New Zealand, and several of the Caribbean islands. Anyone can get TD, but persons at particular high-risk include young adults , immunosuppressed persons, persons with inflammatory-bowel disease or diabetes, and persons taking H-2 blockers or antacids. Attack rates are similar for men and women. TD is caused by bacteria, protozoa or viruses that are ingested by eating contaminated food or beverages. For short-term travelers in most areas, bacteria are the cause of the majority of diarrhea episodes. What are common symptoms of travelers’ diarrhea? Most TD cases begin abruptly. -

Expert Mark H
Ask the expert Mark H. DeLegge, Enteral nutrition MD, FASGE 1. Q: How do you code for percutaneous endoscopic jejunostomy (PEJ)? A: For direct (D) PEJ, I use code 44372, with a Relative Value Unit (RVU) of 6.72. Ask the expert features questions submitted 2. Q: In the severely ill patient, is there any role for amino acid supplementation? by members, with A: Arginine and glutamine are two very important amino acids for the critically ill patient, who is often in the intensive care unit (ICU) on a ventilator. Arginine is a conditionally essential amino acid, meaning answers provided by that in critical situations, it should be supplemented. Multiple studies have determined that arginine is an ASGE physician experts. immuno-enhancing supplement that has been shown to improve rates of morbidity and mortality and days ASGE’s Publications on a ventilator in an ICU in some very ill patients. There have been concerns about the use of arginine in septic patients, because arginine is metabolized to nitrous oxide – a vasodilator. However, these concerns Committee identifies are unfounded. authors and topics for Glutamine is an immune-stimulating amino acid that is also trophic for the small bowel mucosa. Although oral the column. In this or enteral administration of glutamine has not been shown to improve clinical outcomes in critically ill patients, issue, Mark H. DeLegge, intravenous administration of glutamine has been shown to be beneficial. Intravenous glutamine is currently available internationally but not in the United States. Therefore, oral arginine supplementation or use of an MD, FASGE, responds arginine-fortified enteral formula should be considered in critically ill patients.