Tube Feeding Protocol: Supporting an Individual with a Feeding Tube
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Routine Use of Feeding Jejunostomy in Pancreaticoduodenectomuy: A
Preprints (www.preprints.org) | NOT PEER-REVIEWED | Posted: 95 JuneSeptember 2020 2020 doi:10.20944/preprints202006.0114.v1 doi:10.20944/preprints202006.0114.v2 Routine use of Feeding Jejunostomy in Pancreaticoduodenectomuy: A Metaanalysis. DR.Bhavin Vasavada Consultant HepatoPancreaticobiliary and Liver Transplant Surgeon, Shalby Hospitals, Ahmedabad. Email: [email protected] Dr.Hardik Patel Consultant HepatoPancreaticobiliary and Liver Transplant Surgeon, Shalby Hospitals, Ahmedabad. Conflict of Interests: none. Funding disclosure: none. Abbreviations: Post operative pancreatic fistula (POPF), total parentral nutrition (TPN), Surgical site infections. (SSI) Keywords: Pancreaticoduodenectomy; feeding jejunostomy; morbidity; mortality Abstract: Aims and objectives: The primary aim of our study was to evaluate morbidity and mortality following feeding jejunostomy in pancreaticoduodenectomy compared to the control group. We © 2020 by the author(s). Distributed under a Creative Commons CC BY license. Preprints (www.preprints.org) | NOT PEER-REVIEWED | Posted: 95 JuneSeptember 2020 2020 doi:10.20944/preprints202006.0114.v1 doi:10.20944/preprints202006.0114.v2 also evaluated individual complications like delayed gastric emptying, post operative pancreatic fistula, superficial and deep surgical site infection. We also looked for time to start oral nutrition and requirement of total parentral nutrition. Material and Methods: The study was conducted according to the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) statement and MOOSE guidelines. [9,10]. We searched pubmed, cochrane library, embase, google scholar with keywords like “feeding jejunostomy in pancreaticodudenectomy”, “entral nutrition in pancreaticoduodenectomy, “total parentral nutrition in pancreaticoduodenectomy’, “morbidity and mortality following pancreaticoduodenectomy”. Two independent authors extracted the data (B.V and H.P). The meta-analysis was conducted using Open meta-analysis software. -

Adult Tube Feeding
Guide to ADULT TUBE FEEDING Parents’ Practical Guide to Pediatric Tube Feeding | XX Contents Introduction 3 Finding Community Support 4 Understanding the Tube Feeding System 6 Monitoring Your Response to Tube Feeding 8 Taking Charge of Your Doctor Visits 18 Tube Feeding Monitoring Checklist 20 Medication Record 28 Notes 30 Glossary 32 Guide to Adult Tube Feeding | 1 Introduction We know that tube feeding brings major changes to your life. But you don’t have to face them alone. We hope you find this guide a useful, practical resource that can help you tube feed successfully at home. You’ll find step-by-step instructions on handling issues you face every day, from coping with infections to preparing for a doctor’s appointment. The guide includes worksheets (P. 20-31) that make it simple to record important information about your progress. We’ve also added a helpful glossary (P. 32-34) that you can refer to if you come across any unfamiliar terms. While technical and medical support form the foundation of tube-feeding success, we believe that emotional support is just as important. Hopefully, you’ll find resources in this guide that make your journey easier. Guide to Adult Tube Feeding | 3 Finding Community Support With support and guidance, you can take control of the tube-feeding process and adjust successfully to this new lifestyle change. Visit the link below to find educational resources, support groups and the opportunity to connect with others in your situation. The Oley Foundation The Oley Foundation is a nonprofit organization for people who depend on home enteral (tube) feeding or parenteral (intravenous) feeding. -

Laparoscopic Truncal Vagotomy and Gatrojejunostomy for Pyloric Stenosis
ORIGINAL ARTICLE pISSN 2234-778X •eISSN 2234-5248 J Minim Invasive Surg 2015;18(2):48-52 Journal of Minimally Invasive Surgery Laparoscopic Truncal Vagotomy and Gatrojejunostomy for Pyloric Stenosis Jung-Wook Suh, M.D.1, Ye Seob Jee, M.D., Ph.D.1,2 Department of Surgery, 1Dankook University Hospital, 2Dankook University School of Medicine, Cheonan, Korea Purpose: Peptic ulcer disease (PUD) remains one of the most prevalent gastrointestinal diseases and Received January 27, 2015 an important target for surgical treatment. Laparoscopy applies to most surgical procedures; however Revised 1st March 9, 2015 its use in elective peptic ulcer surgery, particularly in cases of pyloric stenosis, has not been popular. 2nd March 28, 2015 The aim of this study was to describe the role of laparoscopic surgery and an easily performed Accepted April 20, 2015 procedure for pyloric stenosis. We accordingly performed laparoscopic truncal vagotomy with gastrojejunostomy in 10 consecutive patients with pyloric stenosis. Corresponding author Ye Seob Jee Methods: Data were collected prospectively from all patients who underwent laparoscopic truncal Department of Surgery, Dankook vagotomy with gastrojejunostomy from August 2009 to May 2014 and reviewed retrospectively. University Hospital, Dankook Results: A total of 10 patients underwent laparoscopic trucal vagotomy with gastrojejunostomy for University School of Medicine, 119, peptic ulcer obstruction from August 2009 to May 2014 in ○○ university hospital. The mean age was Dandae-ro, Dongnam-gu, Cheonan 62.6 (±16.4) years old and mean BMI was 19.3 (±2.5) kg/m2. There were no conversions to open 330-714, Korea surgery and no occurrence of intra-operative complications. -

Nutrition Department This Booklet Has Been Developed by the Nutrition and Gastroenterology Department’S at Alfred Health, Melbourne
Nutrition Department This booklet has been developed by the Nutrition and Gastroenterology Department’s at Alfred Health, Melbourne. Inside you will find information on tube feeding at home CONTENTS 1. Your tube & feeding regime Tube details page 1 Feeding regime page 1 2. Important contact phone numbers page 1 3. Introduction What is tube feeding? page 2 Who receives tube feeding? page 2 4. The feeding tube Nasogastric tube page 3 Nasojejunal tube page 3 Gastrostomy tubes page 3—7 Jejunostomy tubes page 8 Trans-gastric jejunostomy tubes page 8 5. The formula Formula selection & feeding plan page 9 - 10 Formula storage & preparation page 10 6. Feeding methods Continuous OR Intermittent feeding using a pump page 11 - 12 Continuous OR Intermittent feeding using gravity drip page 13 - 14 Bolus feeding page 15 - 16 Oral feeding page 16 7. Medication Administration of medication page 17 8. Care during tube feeding Gastrostomy feeding tube care: Care immediately post tube insertion page 18 Daily tube & stoma care page 19 Jejunostomy, trans-gastric jejunostomy & PEG—J page 20 Nasogastric tube care page 20 Care of the tube feeding equipment page 21 Mouth care page 21 9. Possible problems & solutions Blocked Tube page 22 Constipation page 22 - 23 Diarrhoea page 23 - 24 Irritation, skin redness &/or oozing page 24 Leaking around tube page 24 Nausea & vomiting page 25 Reflux page 25 Tube dislodged or falls out page 25 Tube deteriorated or damaged page 25 What to do if your feeding tube has fallen out page 26 10. The Alfred Home Enteral Nutrition (HEN) program Requirements of the HEN Program page 27 The PEG/HEN Clinic page 28 Ordering formula & equipment pager 28 11. -

JEJUNOSTOMY Feeding Tube PASSPORT (JEJ)
Hull University Teaching Hospitals NHS Trust JEJUNOSTOMY Feeding Tube PASSPORT (JEJ) Tube INFORMATION ABOUT MY JEJUNOSTOMY FEEDING TUBE Affix Addressograph Has a tube How inserted? Site of bowel insertion: e.g. Jejunum, Terminal Ileum (Circle) Date inserted: Skin Suture Removal Date Yes / No Weekly Balloon change (If required) Abdominal measurement (If required) cm Type of feed: Continuous/mls per hour mls Flush with of sterile water pre & post feed & medication. 30mls Additional flushes can be given as indicated by your dietitian. Long term plan If during the first 7 days following your tube insertion, you notice any leak of fluid around the tube, pain on feeding, flushing or if there is fresh bleeding, STOP the feed immediately and contact Ward 14 Castle Hill Hospital - see contact numbers on page 16 2 CONTENTS Page Going home with a jejunostomy tube 4 What is a feeding jejunostomy tube 4 How long will I need it? 5 Surgically placed jejunostomy tube with stitches 5 & 6 Jejunostomy tube with balloon 6 General care / stoma care 7 Flushing 8 Pump feeding/Key Points 9 My Feed regime 10 & 11 Tube blockage 12 Tube fallen out 12 Mouth care 13 Medicine 13 Feed storage and disposal 13 Training prior to going home 14 Going home 14 Equipment for discharge 15 When discharged from hospital 15 Contact numbers between 9am-5pm 16 Emergency contact details after 5pm 16 This booklet contains useful information and advice for patients leaving hospital with a Jejunostomy feeding tube. How it works and how to maintain it. It also lists specific interventions of what to do should you encounter any problems. -
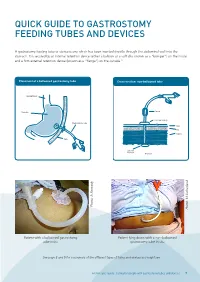
Quick Guide to Gastrostomy Feeding Tubes and Devices
QUICK GUIDE TO GASTROSTOMY FEEDING TUBES AND DEVICES A gastrostomy feeding tube or device is one which has been inserted directly through the abdominal wall into the stomach. It is secured by an internal retention device (either a balloon or a soft disc known as a “bumper”) on the inside and a firm external retention device (known as a “flange”) on the outside.11 Placement of a ballooned gastrostomy tube Cross-section: non-ballooned tube Oesophagus Stomach Clamp External Flange Gastrostomy tube Skin Fat Muscle Skin Internal Bumper Stomach Photo: APhoto: Kennedy Photo: MPhoto: Sutherland Patient with a ballooned gastrostomy Patient lying down with a non-ballooned tube insitu gastrostomy tube in situ See page 8 and 9 for a summary of the different types of tubes and devices you might see. A Clinician’s Guide: Caring for people with gastrostomy tubes and devices 7 Common features of gastrostomy feeding tubes and devices include, but are not limited to: Refer to manufacturer’s guidelines for advice on brand specific tube and device features Ballooned Gastrostomy Tube Ballooned Gastrostomy Tube With side port Without side port Feeding Port Feeding Port (Enteral Dispenser (Enteral Dispenser and Feed Bag and Feed Bag connect here) connect here) ml/cc Balloon Port Balloon Port ml/cc Side Port (X ml/cc) (X ml/cc) French (size) [For example:16/18/20] French (size) [For example:16/18/20] FR FR cm markings cm markings External External Flange Flange Balloon Balloon Non-ballooned Gastrostomy Tube Non-ballooned Gastrostomy Tube with collapsible internal -

Mic Gastrostomy Feeding Tubes Care Booklet.Pdf
GASTROSTOMY CARE GUIDE GASTROSTOMY CARE GUIDE Universal INDICATIONS FOR Adapter TUBE FEEDING Medication PATIENT INFORMATION Complete nutrition supports Port development, growth, and heal- ing. If the ability to eat or Replaceable Date of tube insertion swallow is lost, or the patient is unable to tolerate food, enteral Feeding feeding can sustain life, nour- Patient name Phone ish, and even increase body Adapter weight. Tube feeding is also Physician Phone used to supplement a deficient food and fluid intake. The feed- Type 0100 0110 0150 0160 (circle one) Fr Size ing procedure can be managed safely and economically at Manufacturer's lot number (printed on package) home, away from the hospital setting. A surgical gastrostomy Mark above the SECUR-LOK® Ring in cm provides access to the stomach if long term nutritional support (this means the mark after the initial placement) is necessary. Balloon volume if 0100, or 0110 type G Tube Pure medical grade silicone (the volume should be between 7 and 10 cc) construction makes MIC Feeding Tubes durable, yet soft and comfortable to wear. They SECUR-LOK® Formula are also translucent, allowing Ring visualization of the inside of Brand name the tube above the skin line. All MIC Enteral Feeding Tubes Method of delivery are latex free. Volume, rate and time the feeding should take MIC PEG Total amount of daily water PEG stands for Percutan- eous (through the skin) Additional ingredients Endoscopic (use of a flexible lighted tube to visualize tube Irrigate the tube with water before and after feeding and medication placement) Gastrostomy administration. (surgical opening into the stomach). -

2Nd Quarter 2001 Medicare Part a Bulletin
In This Issue... From the Intermediary Medical Director Medical Review Progressive Corrective Action ......................................................................... 3 General Information Medical Review Process Revision to Medical Record Requests ................................................ 5 General Coverage New CLIA Waived Tests ............................................................................................................. 8 Outpatient Hospital Services Correction to the Outpatient Services Fee Schedule ................................................................. 9 Skilled Nursing Facility Services Fee Schedule and Consolidated Billing for Skilled Nursing Facility (SNF) Services ............. 12 Fraud and Abuse Justice Recovers Record $1.5 Billion in Fraud Payments - Highest Ever for One Year Period ........................................................................................... 20 Bulletin Medical Policies Use of the American Medical Association’s (AMA’s) Current Procedural Terminology (CPT) Codes on Contractors’ Web Sites ................................................................................. 21 Outpatient Prospective Payment System January 2001 Update: Coding Information for Hospital Outpatient Prospective Payment System (OPPS) ......................................................................................................................... 93 he Medicare A Bulletin Providers Will Be Asked to Register Tshould be shared with all to Receive Medicare Bulletins and health care -

Laparoscopic Witzel Jejunostomy
[Downloaded free from http://www.journalofmas.com on Wednesday, February 12, 2020, IP: 93.55.127.222] How I do It Laparoscopic Witzel jejunostomy Marco Lotti1, Michela Giulii Capponi2, Denise Ferrari2, Giulia Carrara1, Luca Campanati2, Alessandro Lucianetti2 1Advanced Surgical Oncology Unit, Department of General Surgery 1, Papa Giovanni XXIII Hospital, Bergamo, Italy, 2Department of General Surgery 1, Papa Giovanni XXIII Hospital, Bergamo, Italy Abstract The placement of a feeding jejunostomy can be indicated in malnourished patients with gastric and oesophagogastric junction cancer to allow for enteral nutritional support. In these patients, the jejunostomy tube can be suitably placed at the time of staging laparoscopy. Several techniques of laparoscopic jejunostomy (LJ) have been described, yet the Witzel approach remains neglected, due to the perceived difficulty of suturing the bowel around the tube and securing them to the abdominal wall. Here, we describe a novel technique for LJ, using a single barbed suture for securing the bowel and tunnelling the jejunostomy catheter according to the Witzel approach. Keywords: Enteral nutrition, oesophagogastric junction cancer, gastric cancer, jejunostomy, laparoscopic jejunostomy Address for correspondence: Dr. Marco Lot, Advanced Surgical Oncology Unit, Ospedale Papa Giovanni XXIII, Piazza OMS, 1, 24127 Bergamo, Italy. E‑mail: [email protected] Received: 17.10.2019, Accepted: 11.11.2019, Published: 11.02.2020 INTRODUCTION use of peel-away introducers, sealing the entry site with barbed -

Short Bowel, Short Answer?
478 Nightingale 8 Van Doorn L, Figueiredo C, Sanna R, et al. Clinical relevance of the cagA, 10 Yamaoka Y, Kodama T, Kashima K, et al. Variants of the 3' region of the vacA and iceA status of Helicobacter pylori. Gastroenterology 1998;115:58–66. cagA gene in Helicobacter pylori isolates from patients with diVerent H. 9 Rudi J, Kolb C, Maiwald M, et al. Diversity of Helicobacter pylori vacA and pylori-associated diseases. J Clin Microbiol 1998;36:2258–63. cagA genes and relationship to VacA and CagA protein expression, 11 Blaser MJ. Helicobacters are indigenous to the human stomach: duodenal cytotoxin production and associated diseases. J Clin Microbiol 1998;36: ulceration is due to changes in gastric microecology in the modern era. Gut 944–8. 1998;43:721–7. See article on page 559 Short bowel, short answer? from their stoma.14 This is because of loss of normal daily intestinal secretions (about 4 litres/24 hours), rapid gastric emptying and rapid small bowel transit.15 If a patient has less than 100 cm jejunum remaining and a stoma he/she is The paper by Jeppsen et al (see page 559) shows that likely, as a minimum, to need long term parenteral saline.14 glucagon-like peptide-2 (GLP-2) concentrations are low in This requirement does not reduce with time.3 Patients patients lacking an ileum and colon. This is not an with a retained colon do not have these problems and, unexpected finding as the L cells that produce GLP-2 are owing to functional adaptation, nutrient absorption situated in the ileum and colon. -

Expert Mark H
Ask the expert Mark H. DeLegge, Enteral nutrition MD, FASGE 1. Q: How do you code for percutaneous endoscopic jejunostomy (PEJ)? A: For direct (D) PEJ, I use code 44372, with a Relative Value Unit (RVU) of 6.72. Ask the expert features questions submitted 2. Q: In the severely ill patient, is there any role for amino acid supplementation? by members, with A: Arginine and glutamine are two very important amino acids for the critically ill patient, who is often in the intensive care unit (ICU) on a ventilator. Arginine is a conditionally essential amino acid, meaning answers provided by that in critical situations, it should be supplemented. Multiple studies have determined that arginine is an ASGE physician experts. immuno-enhancing supplement that has been shown to improve rates of morbidity and mortality and days ASGE’s Publications on a ventilator in an ICU in some very ill patients. There have been concerns about the use of arginine in septic patients, because arginine is metabolized to nitrous oxide – a vasodilator. However, these concerns Committee identifies are unfounded. authors and topics for Glutamine is an immune-stimulating amino acid that is also trophic for the small bowel mucosa. Although oral the column. In this or enteral administration of glutamine has not been shown to improve clinical outcomes in critically ill patients, issue, Mark H. DeLegge, intravenous administration of glutamine has been shown to be beneficial. Intravenous glutamine is currently available internationally but not in the United States. Therefore, oral arginine supplementation or use of an MD, FASGE, responds arginine-fortified enteral formula should be considered in critically ill patients. -

MIC & ENTRAL G-Tube Patient Booklet
MIC* & ENTRAL* Gastrostomy Tubes MIC* Gastrostomy tube MIC* Bolus Gastrostomy tube ENTRAL* Gastrostomy tube PATIENT BOOKLET MIC* G-TUBE, MIC* BOLUS G-TUBE, ENTRAL* G-TUBE PATIENT BOOKLET CONTENTS YOUR AVANOS* GASTROSTOMY TUBE INFORMATION 3 INTRODUCTION 4 WHAT IS YOUR TUBE FOR? 5 ABOUT YOUR G-TUBE 5 INITIAL PLACEMENT FIRST 72 HOURS CARE 7 DAILY CARE 7 WHEN THE STOMA IS HEALED 7 WEEKLY ROUTINE 8 BEFORE FEEDING BEGINS 9 ADMINISTRATION OF TUBE FEEDS 10 ADMINISTRATION OF MEDICATION 10 FLUSHING YOUR TUBE 10 REPLACEMENT AND ACCIDENTAL REMOVAL 11 PROBLEM SOLVING 12 CHILDREN’S SPECIAL CONCERNS 13 TERMS YOU’LL NEED TO KNOW 13 SOME G-TUBE PEG DO’S AND DON’TS 14 2 YOUR AVANOS* GASTROSTOMY TUBE INFORMATION PATIENT NAME OR ID __________________________________________________________________ NURSE ______________________________________________________________________________ DIETITIAN ____________________________________________________________________________ GENERAL PRACTITIONER _______________________________________________________________ * GASTROSTOMY TYPE MIC G-TUBE O FR SIZE: _____________ * MIC BOLUS G-TUBE O * ENTRAL G-TUBE O DATE OF INSERTION ___________________________________________________________________ CM MARKING AT SKIN LEVEL _____________________ CM BALLOON FILL VOLUME ________________________________________________________________ REPLACEMENT DATE ___________________________________________________________________ NAME AND TYPE OF TUBE FEED __________________________________________________________ AMOUNT OF FEED ______________________________